Ankle injuries are common presenting complaints in both emergency departments and family physicians' offices. Approximately 1 million ankle injuries occur annually in the United States; most of them are sprains resulting from inversion injuries. Treatment options differ according to the grade of injury—grade I and grade II sprains usually respond to rest and immobilization, while grade III sprains require casting or, possibly, surgery. A chronic “ankle” injury should prompt evaluation for other conditions, such as talar dome lesion. Most ankle injuries can be treated adequately in the family physician's office, although some of the more serious injuries should be referred to an orthopedic specialist for further evaluation.
Because of its weight-bearing function and the construction of its articulation, the ankle is the most commonly injured joint among athletes1–3 and a frequent cause of morbidity in the general population. Estimates of the frequency of ankle injuries in the United States vary from 1 to 10 million per year.4,5 Of these injuries, 85 percent are sprains, and 85 percent of sprains are inversion injuries.4,6 The sports most frequently associated with ankle sprains are basketball, football and cross-country running.1,7
Although sprains account for the most significant number of ankle injuries, great morbidity can result from other ankle injuries, such as talar dome lesions, which should always be considered in the differential diagnosis.
Anatomy
The bones involved in ankle articulation are the distal tibia and fibula, including the malleoli and the talus. The tibia and the fibula are bound together by the anterior inferior tibio-fibular ligament, the posterior inferior tibio-fibular ligament and the interosseous membrane, which runs between the two long bones. The talus is a wedge-shaped bone that is wider anteriorly than posteriorly and fits into the mortise formed by the bound tibia and fibula.
This articulation is maintained by many ligamentous attachments, most notably on the lateral side by the anterior talofibular, calcaneo-fibular and posterior talofibular ligaments (Figure 1) and medially by the deltoid complex of ligaments (Figure 2). The ankle is also supported laterally by the tendons of the peroneus longus and the peroneus brevis. Medially, the tendons of the tibialis anterior and posterior, the flexor digitorum longus, the flexor hallucis longus and the extensor hallucis longus (Figure 3) also add integrity to the ankle.
FIGURE 1.
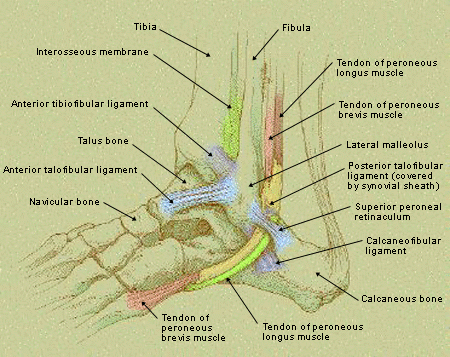
Lateral view of tendons and ligaments responsible for maintaining ankle articulation.
FIGURE 2.
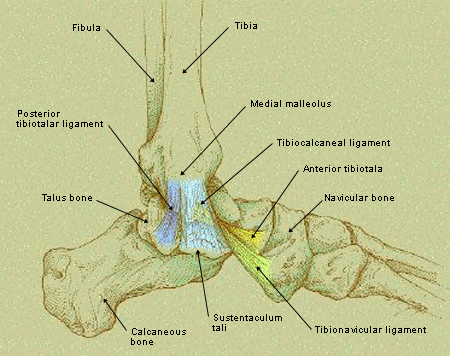
Deltoid ligaments of the ankle.
FIGURE 3.
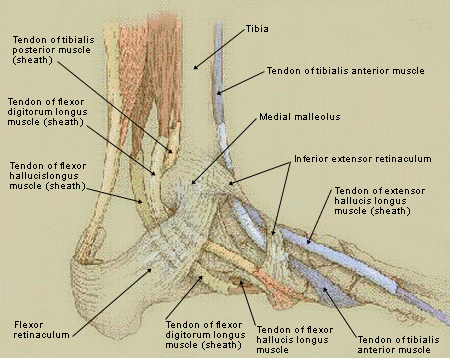
Medial view of ankle tendons.
Movement at the ankle joint itself actually occurs only in the vertical plane (i.e., dorsi-flexion and plantar flexion). Inversion and eversion actually take place at the subtalar or calcaneotalar joint. This joint is considerably stronger than the ankle joint and, as a result, most inversion/eversion injuries occur at the ankle rather than at the subtalar joint.
Acute Sprains
As is true with all injuries, obtaining a good history before performing the physical examination will help the family physician decide which treatment options to pursue. First, discovering the position of the ankle at the time of injury may help determine the degree of disability. For example, in the plantar-flexed position, the narrower, posterior part of the talus forms the ankle articulation and, as such, gives more room for “play” in the joint. Also, in that position, the anterior talofibular is at its greatest tension,8 placing it in position to sustain injury.
Second, determine whether the patient was immediately able to bear weight or whether he or she needed assistance to walk after the injury. Inability to bear weight may signify more serious injury, such as a possible fracture,9 and therefore signals the need for a more thorough diagnostic work-up, such as radiography.
Third, if the patient is a child or adolescent with open growth plates, the chances of a growth plate fracture are higher, and casting may be required. Radiographs are indicated in all children to rule out a Salter-Harris fracture involving the growth plate.
Fourth, if the patient heard a popping or snapping noise at the time of the injury, a partial- or full-tendon rupture may have occurred.
Finally, if this type of injury has occurred before, the ankle is more likely to be reinjured.
Ankle sprains have been characterized as either grade I, grade II or grade III (Table 1). The anterior talofibular is the most commonly injured ligament,10,11 followed by the calcaneofibular10 and, finally, the posterior talofibular.10 Although it can be difficult to determine the grade of the sprain, this determination can be a guide to appropriate treatment.
TABLE 1 Physical Findings in Ankle Sprains by Grade
| Sign/symptom | Grade I | Grade II | Grade III |
|---|---|---|---|
| Tendon | No tear | Partial tear | Complete tear |
| Loss of functional ability | Minimal | Some | Great |
| Pain | Minimal | Moderate | Severe |
| Swelling | Minimal | Moderate | Severe |
| Ecchymosis | Usually not | Frequently | Yes |
| Difficulty bearing weight | No | Usually | Almost always |
A grade I sprain is usually characterized by minimal loss of functional ability, minimal pain, minimal swelling and the ability to bear weight. The integrity of the ligaments remains intact and, typically, radiographs are not necessary. Treatment consists of rest, ice, compression and elevation (RICE). Nonsteroidal anti-inflammatory drugs (NSAIDs) are helpful to control both pain and swelling. Crutches may be useful for patients who do not tolerate the injury well, to prevent reinjury when they attempt to ambulate.
Grade II sprains tend to produce some functional impairment, an increase in subjective pain, moderate swelling and ecchymosis, and more difficulty bearing weight. The ligament, although still intact, has a partial tear. Treatment consists of using the RICE protocol and NSAIDs. Usually, patients with a grade II sprain need a rigid ankle support, such as an air cast or stirrup-type ankle support. Some authors recommend casting.12 Nonweight bearing with crutches is recommended until ambulation is pain free. At that time, rehabilitative exercises should be begun, either with a physical therapist or a prescribed home regimen. Rehabilitation is important since patients who have experienced a previous grade II ankle sprain are not only more prone to reinjury but also tend to have a more lax joint following injury.
Complete rupture of the ligament is indicative of a grade III sprain. The patient has severe functional loss, severe pain, diffuse swelling and bruising, and inability to bear weight on the joint. Treatment of grade III sprains remains controversial. There is much debate in the literature regarding the use of surgical intervention versus casting.13,14 Some experts15 recommend surgery for patients younger than 40 years of age and advocate conservative treatment, followed by surgery if necessary, in patients older than age 40. Others16 believe that if only the anterior talofibular is involved, casting is adequate and that if both the anterior talofibular and the calcaneofibular are torn, surgical intervention is warranted.
Finally, Brostrom,17 who is probably the clinical researcher most widely quoted on ankle injuries, found that surgery resulted in the best outcome for grade III sprains. Brostrom qualified this recommendation by adding that surgery should be the primary treatment for athletes but not for noncompetitive patients. He argued that a secondary repair could always be performed later, if needed.
Determining whether the injury is truly a grade II partial tear or a grade III complete tear may be difficult. In addition to radiography, clinical tests can help differentiate grade I and grade II ankle sprains from grade III sprains. The anterior drawer test is used to assess the integrity of the anterior talofibular. While holding the distal tibia and fibula in place with one hand, the physician should grasp the heel of the affected ankle with the other hand and attempt to move the ankle anteriorly with respect to the rest of the leg. A movement of 4 mm or greater is considered positive for anterior talofibular rupture.18,19 A very good review of the proper technique for performing this test was written nearly 20 years ago.20
The calcaneofibular ligament can be assessed by the talar tilt test. While holding the distal end of the tibia and fibula in one hand, the physician uses the other hand to invert the injured ankle. The calcaneofibular ligament can be presumed to be involved if the tilt is 5 to 10 percent greater on the injured side when compared with the uninjured ankle.4
The routine use of ankle radiographs is debatable. Some physicians believe that all sprained ankles should be x-rayed to rule out fracture, and others believe that stress radiographs can show loss of tendon integrity. In today's world of cost-conscious medicine, however, it may be useful to evaluate ankle injuries according to the Ottawa Ankle Rules (Table 2).9,21 During a five-month period, 750 adult patients were evaluated in two emergency departments after presenting with acute blunt ankle injuries. The goal of this prospective study was to develop clinical “decision rules” to predict fractures, allowing radiography to be used more selectively.21 The investigators conducted a follow-up study by applying the rules during evaluation of 2,342 patients with acute ankle injuries presenting to two emergency departments.9 Use of the Ottawa Ankle Rules decreased use of radiography by 28 percent, and the calculated sensitivity of this test for fracture was at the 95 percent confidence level. In this study, no fractures were missed when the Ottawa Ankle Rules were applied.9
TABLE 2 Ottawa Ankle Rules for Foot and Ankle Radiographic Series in Patients with Acute Ankle Injury
| An ankle radiographic series is required only if patient has pain in malleolar zone and any one of the following findings: | A foot radiographic series is required only if patient has pain in midfoot zone and any one of the following findings: |
| Bone tenderness at the posterior edge or tip of the lateral malleolus | Bone tenderness at the base of the fifth metatarsal |
| Bone tenderness at the posterior edge or tip of the medial malleolus | Bone tenderness at the navicular |
| Inability to bear weight both immediately and in emergency department | Inability to bear weight both immediately and in emergency department |
As a general rule, it may be helpful to treat grade I and grade II sprains in non–athletic-related injuries identically (Table 3). For athletes, more aggressive treatment—such as surgery in grade III sprains and early rehabilitation in other sprains—should be tailored to fit the specific need. It is also beneficial for the physician to have a good working relationship with a respected physical therapist or athletic trainer, to accelerate rehabilitation of these patients in a safe manner. Physical therapists and athletic trainers can also retrain patients who have proprioceptive loss after injury by using a Babst board. The latter consists of a flat board under which half-spheres of various sizes can be attached, forming a kind of teeter-totter. The patient uses the board first to increase range of motion, then follows with balancing exercises to increase proprioception and stabilization that was lost with the injury.
TABLE 3 Treatment of Ankle Sprains
| Grades I and II |
| Rest |
| Ice |
| Compression: elastic wrap, air cast, foam stirrup |
| Elevation |
| Acetaminophen during the first 24 hours; NSAIDs after the first 24 hours |
| Crutches until weight bearing is pain free |
| Casting can be appropriate for grade II sprains |
| Range-of-motion and ankle strengthening exercises when patient is pain free |
| Grade III |
| Casting vs. surgery should be determined on an individual basis |
| Factors to consider in making operative decision: age of patient, level of athletic participation, number of ligaments involved. Surgery is favored in younger patients with a high level of athletic activity, especially when more than one ligament is involved. |
NSAIDs = nonsteroidal anti-inflammatory drugs.
It is important to remind patients that once an ankle sprain has occurred, the joint itself is usually never as strong as it was before the injury. Continued ankle strengthening exercises, either at home, at a gym or at a physical therapy facility, are very beneficial, as is protective support of the ankle when participating in athletic activities. Traditionally, ankle taping has been used by many athletes to help protect themselves from ankle injury. Although taping offers some protection, studies have shown that support breakdown can occur quickly. One study22 showed that 40 percent of tape support was lost after 10 minutes. Therefore, the use of other support devices should be considered. Better protection is provided by a lace-up type of ankle support, which can be obtained at most sporting goods stores. This type of ankle support allows full motion in the vertical plane and still protects against inversion injuries.
Treatment and Follow-Up
Patients with grade I or grade II sprains can be reevaluated in seven to 10 days. As mentioned previously, NSAIDs can be used for pain and swelling, and the RICE protocol should be implemented. Progress is evidenced by improvement in passive and active range of motion, as well as by the ability to bear weight without pain. Early mobilization (24 to 48 hours in grade I sprains) is important and can begin as soon as pain decreases. Use of crutches should be discontinued when ambulation is pain free.
Grade III sprains can be plaster casted for one to three weeks12 or patients can be referred to an orthopedist for surgical evaluation (in the United States, nonoperative intervention is preferred). If pain persists, evaluation for chronic conditions (Table 4) should be carried out, and the cast can then be reapplied and reassessed at one-week intervals.
TABLE 4 Differential Diagnosis of Chronic Ankle Sprain
| Ankle fracture |
| Talar dome lesions (osteochondritis dissecans) |
| Peroneal tendon subluxation |
| Peroneal nerve entrapment |
| Recurrent ankle sprain |
| Talotibial exostosis |
| Lateral impingement |
Exercises using plantar flexion/dorsiflexion, as well as inversion/eversion, can be started, using elastic tubing or light weights draped over the dorsum of the foot. Babst boards, as mentioned previously, can help increase range of motion and restore proprioception.
If pain or instability persists (more than four to six weeks), repeat evaluation with radiographs, computed tomographic scan or bone scan may be helpful in ruling out chronic conditions (Table 4).
Chronic Sprains
It is not uncommon for a patient to complain of recurrent ankle sprains or a sprain that “won't go away.” While the etiology of such discomfort is commonly a weakened ligamentous complex resulting from a previous injury and, likely, little or no rehabilitation, other diagnoses should also be considered, such as a talar dome lesion (osteochondritis dissecans).
A talar dome fracture is characterized by the post-traumatic formation of necrotized bone on the articular surface of the talus. Affected patients often mention chronic ankle pain, swelling and limping, aggravated by activity. Acutely, radiography might not show the lesion formation during the first few weeks, and other imaging studies might be needed. If the problem persists, standard radiography will show a characteristic ulcerated lesion on the talus. If the fragment of bone composing the ulceration is nondisplaced, casting and nonweight bearing can be appropriate treatments. If, however, the osteochondral fragment is displaced, surgery is usually indicated.

