to the editor: Anterior traumatic shoulder dislocations carry a risk for rotator cuff tears.2–4,6 Many of these tears are of the supraspinatus tendon, and quick diagnosis can give the patient options that make for a greater degree of function. If a tear is undetected, the tendons retract and the muscle atrophies to the point that repair of the rotator cuff would be tenuous.
A 75-year-old man was seen eight weeks after a fall which had resulted in an anterior dislocation of his right shoulder (Figure 1). This was easily reduced in the emergency department.
FIGURE 1.
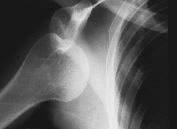
Radiograph of an anterior subcoracoid dislocation. Note the relationship of the humeral head and the glenoid. Although there are no bony avulsions, the physician must be aware of the possibility of rotator cuff injuries.
Subsequent follow-up visits demonstrated a persistent component of night pain and limited function. Physical examination revealed an inability to actively forward elevate or abduct. Strength on external rotation was compromised as well.
Treatment included a six-week course of physical therapy, without much improvement. Analgesics and anti-inflammatory medications were ineffective. The patient underwent magnetic resonance imaging (MRI) of the shoulder, which demonstrated a tear of the supraspinatus tendon with retraction of the tendon (Figure 2).
FIGURE 2.
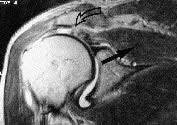
Magnetic resonance imaging showing a tear of the rotator cuff. The open arrow shows retraction of the supraspinatus tendon toward the glenoid rim. The solid arrow shows the supraspinatus muscle belly. Atrophy of the muscle will show a decrease in signal along with fatty infiltrates.
It was explained to the patient that he could choose to have surgery in an attempt to repair the rotator cuff or choose to accept his disability, knowing that repair at a later date would be difficult. The patient elected to have surgery, during which the retracted tendon was mobilized and repaired.
The patient was placed in a stepped rehabilitation program and has regained essentially normal motion and strength. He is able to perform activities of daily life and has minimal discomfort in the shoulder.
Index dislocations of the shoulder seldom occur after the age of 40; when they do, they should engender heightened suspicion of rotator cuff tears.2–4,6 In this example, the initial trauma resulted in an index subcoracoid dislocation, readily reducible and without associated fracture. Occasionally a small avulsion fracture of the greater tuberosity in and of itself serves as a marker for rotator cuff tendon avulsion. In most cases, however, physical examination and clinical suspicion must be the physician's guides.
The typical course for a patient recovering from an uneventful index anterior dislocation is moderate pain that decreases by the end of the second week, during which motion and strength gradually return. In contrast, this patient had noted a high level of persistent pain, diminished motion and, most important, decreased strength on forward elevation and external rotation. The weakness on external rotation implied an injury not only to the supraspinatus, but also to the more posterior infraspinatus. This is an important physical finding and one which should alert the physician to the possibility of a rotator cuff injury.1,2,5
A number of diagnostic tools are available for the patient who presents two to four weeks after dislocation. Radiographs, though helpful in identifying avulsion of the greater tuberosity, do not show rotator cuff tear. Arthrography and ultrasonography will show the presence of a tear (but not its size), the number of tendons involved, the degree of retraction or changes within the muscle bodies, such as fatty infiltration. MRI, on the other hand, will provide all the information needed to properly assess a tear. This is important in patients with prior shoulder problems. The treatment of these patients is based on a careful assessment of their needs, activity levels and the size of the tear. In most cases, an acute rotator cuff tendon tear is best repaired within the first four weeks to minimize the amount of retraction, fibrosis and atrophy. In rare cases, when the patient is older, is medically compromised or leads a functionally undemanding life, noninvasive care is offered. This consists of a gentle rehabilitation program aimed at restoration of function below the horizontal.

