Family physicians often must evaluate patients with testicular pain or masses. The incidental finding of a scrotal mass may also require evaluation. Patients may seek evaluation of a scrotal mass as an incidental finding. An accurate history combined with a complete examination of the male external genitalia will help indicate a preliminary diagnosis and proper treatment. Family physicians must keep in mind the emergency or “must not miss” diagnoses associated with testicular masses, including testicular torsion, epididymitis, acute orchitis, strangulated hernia and testicular cancer. Referral to a urologist should be made immediately if one of these diagnoses is suspected. Benign causes of scrotal masses, including hydrocele, varicocele and spermatocele, may be diagnosed and managed easily in the primary care office.
Patients with a testicular mass may present with a painless lump or scrotal pain, which can range from severe pain to a dull ache that worsens with exercise. The pain may be localized or may radiate along the spermatic cord into the lower abdomen. Examination may reveal a mass in the testicle or in an adjacent structure. It is important for family physicians to have a thorough understanding of various benign and pathologic processes in order to render timely, effective treatment. It is imperative, therefore, to understand the structure of the normal male genitalia and the scrotal contents.
Examination of the Male Genitalia
Penis
The penis (Figure 1) should be inspected for ulcers and palpated for plaques or induration. Cultures for gonorrhea and Chlamydia should be performed to evaluate any urethral discharge.
FIGURE 1.
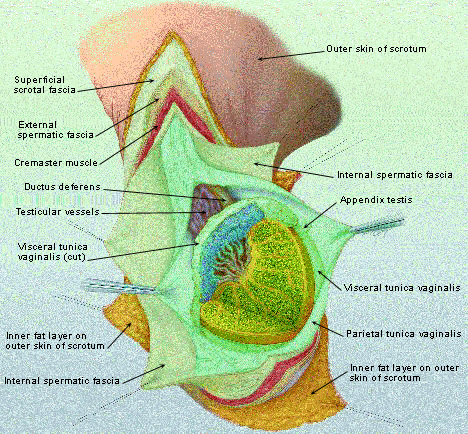
Normal anatomy of the male genitalia.
Testes
The testes should be palpated for masses, equal volume, tenderness or cryptorchidism. A testicle less than 3.5 cm long is considered small. All masses and swellings should be transilluminated. Light will not transmit through a solid tumor, while a hydrocele will glow a soft red color. Chronic testicular lesions, including orchitis and testicular torsion, can cause unilateral or bilateral testicular atrophy. If a testicle cannot be palpated in the scrotum, the inguinal canals and lower abdomen should be examined. A nonpalpable testicle may be physiologically retracted transiently, or it may be truly cryptorchid. The cremasteric reflex on both sides must be checked. This can be done by lightly stroking the medial thigh, with a normal reflex of transient cephalad retraction of the ipsilateral testicle.
Epididymis, Spermatic Cord and Vas Deferens
Palpation should be performed to evaluate for induration and to localize pain to the testicle or adjacent structures. The epididymis is posterior to the testicle. The patient should perform the Valsalva maneuver while standing so he can be evaluated for a mass of dilated testicular veins in the spermatic cord forming a varicocele above and behind the testis.
Inguinal Canals
The inguinal canals should be explored for hernias or cord tenderness. Funiculitis, an inflammation of cord structures, may cause inguinal or scrotal pain, but the testis is normal. Evaluation for cord lipomas or hydroceles should also be performed.
‘Must Not Miss’ Diagnoses
Testicular Torsion
Mechanism. In cases of testicular torsion, an anatomic deformity allows the spermatic cord to twist, resulting in occlusion of testicular blood flow. This anomaly is known as the “bell-clapper” deformity, in which the tunica vaginalis completely surrounds the testis. The deformity leads to inadequate posterior fixation of the testis to the epididymis and scrotal wall. An autopsy series1 found the incidence of bell-clapper deformity to be 12 percent among asymptomatic men. The free-floating testis is more likely to twist on its cord and strangulate its blood supply through intra-vaginal torsion. Initiating factors for torsion can include trauma or vigorous exercise, but symptoms may also occur during sleep. Many patients will recall a previous history of minor similar pain that resolved spontaneously. Such a history favors the diagnosis of torsion.
Extravaginal torsion, which is far less common than intravaginal torsion, occurs exclusively in neonates. In this disorder, incomplete attachment of the gubernaculum and testicular tunics to dartos fascia causes the cord to twist above the level of the testis and tunica vaginalis. This twisting also obliterates the blood supply to the testis.2 An associated anatomic defect is usually not present on the contralateral side.3
Clinical Presentation. Intravaginal testicular torsion occurs most often in young men but can also affect middle-aged men. Patients with testicular torsion often present with sudden, severe, unilateral scrotal pain that is often associated with nausea and vomiting.4 Scrotal edema and erythema are typically present, and lower abdominal pain may also occur. Physical examination reveals a tender, firm affected testis that may appear retracted upward as a result of twisting of the spermatic cord.
The torsed testis is often swollen and edematous, and it is difficult to distinguish normal anatomy. Normal positioning of the epididymis cannot rule out torsion, since the testis may have rotated 360 or 720 degrees.2 However, a testis that has torsed 360 or 720 degrees usually is found higher in the scrotum than its mate. The cremasteric reflex is usually absent in testicular torsion5 and, therefore, the presence of the cremasteric reflex implies epididymitis rather than torsion. Elevation of the scrotum without relief of pain (Prehn's sign) is also said to indicate torsion, but this finding is unreliable. Urinalysis is normal in 90 percent of patients with testicular torsion,6 whereas patients with epididymitis will likely have pyuria.
Management. If the history and physical examination support the diagnosis of torsion, immediate referral to a urologist is mandatory. Rapid detorsion and scrotal exploration should not be delayed. The uninvolved side should also have fixation performed to correct the anatomic defect. When the diagnosis is uncertain, patients should be considered to have testicular torsion until it is proved otherwise. In these patients, testicular blood flow should be evaluated with radionuclide scanning or Doppler ultrasound to help confirm the diagnosis. When torsion is diagnosed, bilateral orchiopexy should be performed, since the bell-clapper deformity often occurs bilaterally.
Prognosis. If blood flow is restored within six hours of torsion, 80 to 100 percent of testes can be saved. In areas where surgical services are limited, detorsion can be attempted by lifting the scrotum or rotating the testicle on its pedicle. If successful, the patient will experience immediate relief, but surgical exploration and orchiopexy are still necessary. Salvage rates drop to 20 percent if detorsion surgery is performed after more than 24 hours of scrotal pain.7 Spermatogenesis may be impaired following unilateral torsion, but this may be the result of a preexisting bilateral congenital defect. In one study8 of biopsies taken during orchiopexy, 55 percent were abnormal.
Torsion of the Testicular Appendage
The appendix testis, a remnant of the müllerian duct, is also susceptible to torsion. The clinical picture is similar to that of testicular torsion with the sudden onset of severe scrotal pain and, thus, it must be differentiated from spermatic cord torsion. A tiny tender mass may be palpable at the upper pole of the testis, and a “blue dot” sign may be visible on the skin of the scrotum early in the course of the disorder. Later, inflammation may occur and produce a hydrocele, which may make physical examination difficult. The time course from onset to resolution of this condition is usually about two weeks. Referral to a urologist is recommended if the patient presents too late for an accurate physical examination and precise diagnosis, although surgery is not usually indicated. Conservative measures such as scrotal support and nonsteroidal anti-inflammatory drugs (NSAIDs) will usually suffice.
Epididymitis
Clinical Presentation. Epididymitis is the most common cause of painful swelling of the testis in postpubertal males.9 A typical history for epididymitis is the gradual development of scrotal pain, with fever, urethral discharge and urinary symptoms. On physical examination, the epididymis is sensitive and may be enlarged and indurated. The presence of edema may cause difficulty in distinguishing the epididymis from the testicle. The scrotum may also be erythematous. The cremasteric reflex is usually present, and elevation of the scrotum may provide relief of pain. Pyuria is common, and the absence of pyuria makes the diagnosis of epididymitis unlikely.10 Epididymitis may also be present in children, but the presenting signs may not be as dramatic as they are in older males. It should be remembered that the chronic inflammation of tuberculosis also may produce a tender enlargement of the epididymis (Figure 2).
FIGURE 2.
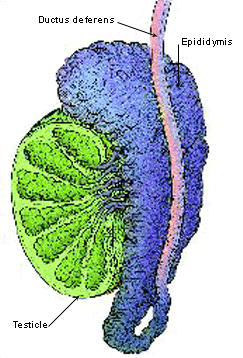
Epididymitis.
Management. The etiology of epididymitis is often an ascending infection, secondary to reflux up the vas from the prostatic urethra, with resulting infection of the epididymis. In prepubertal boys and in men over the age of 35, bacterial urinary tract infection is a frequent cause of epididymitis, while in postpubertal patients under 35 years of age, Neisseria gonorrhoeae and Chlamydia trachomatis are common causes.2 For this reason, urethral Gram's stain and culture should be obtained in order to direct treatment, and the patient's sexual partners should be treated if a sexually transmitted organism is identified.
Treatment should include agents active against Chlamydia and N. gonorrhoeae; ceftriaxone (Rocephin), 250 mg intramuscularly in a single dose, plus oral doxycycline (Vibramycin), 100 mg twice daily for seven days, is an acceptable regimen. The patient with a suspected urinary tract infection can be treated with ciprofloxacin (Cipro), 500 mg orally twice daily for 10 to 14 days. Nonspecific treatments include bed rest, scrotal elevation, local ice therapy and oral NSAIDs.
Complete evaluation of the genitourinary tract should be performed to identify underlying abnormalities in patients with epididymitis caused by a bacterial urinary tract infection. In one study, 39 percent of children with epididymitis were found to have structural or functional urinary tract abnormalities.11 However, underlying urinary tract abnormalities are uncommon in men with uncomplicated sexually transmitted epididymitis, and a complete urologic evaluation is therefore not indicated in these patients.
Prognosis. The inflammation and pain of epididymitis resolve over two to four weeks when properly treated. Chronic epididymitis usually represents the irreversible end stage of a severe case of acute epididymitis that has been followed by frequent mild attacks. Fibroplasia leads to scarring of the epididymis that may cause a lump in the scrotum. Except for recurring pain and the threat of infertility, chronic epididymitis is not a serious health problem.12
Acute Orchitis
Clinical Presentation. Acute orchitis presents with the sudden onset of testicular pain and high fever. Nausea and vomiting are also common. The testis is enlarged, indurated and tender on palpation. Proteinuria or hematuria may be present.
Although many infectious agents can produce a primary infection in the testis, pyogenic bacteria and viruses are the causative agents in most cases.2 Although uncommon in prepubertal males, mumps orchitis occurs in 20 to 35 percent of cases of mumps parotitis, and the onset is usually three to four days after the development of parotitis.12 Mumps orchitis is bilateral in 15 percent of cases.13 Tuberculosis and syphilis may also cause orchitis, and an autoimmune response to spermatozoa may cause a granulomatous orchitis in older men.
Management. Treatment of orchitis includes bed rest, scrotal support, local ice therapy and analgesics. Specific antibacterial agents should be administered if a bacterial source is suspected. Orchiectomy occasionally may be necessary to differentiate granulomatous orchitis from testicular cancer.
Prognosis. Spermatogenesis may be damaged by mumps orchitis. Although older studies reported sterility in 25 to 30 percent of cases, it is rare today. Since bilateral involvement occurs in only 15 percent of cases, infertility rates as low as 4 percent have been reported.14 Infertile testes will commonly become atrophic, but androgenic function usually is maintained.
Inguinal Hernia
An inguinal hernia commonly presents as a scrotal mass. An incarcerated hernia cannot be reduced back into the abdominal cavity, while a strangulated hernia has a compromised blood supply. Strangulation should be suspected when a tender mass consistent with a diagnosis of hernia is palpated in the scrotum. Rapid surgical evaluation is indicated.
Testicular Cancer
Clinical Presentation. A testicular tumor usually presents as a painless mass found by the patient or physician on routine examination. The patient may complain of a dull ache or a sense of scrotal heaviness. Any hematoma or hydrocele that results from minor scrotal trauma should raise suspicion of underlying testicular cancer. Uncommonly, some men have acute pain secondary to bleeding into the testis from extravasation of tumor vessels, causing an expanding mass effect against the inelastic tunica albuginea. Testicular cancer represents only 1 percent of all cancer in males, but it is one of the most commonly occurring cancers in young men, with an average patient age of 32 years. This tumor affects a spectrum of ages, and it is appropriate to advise teenage boys about it. A significantly increased incidence of testicular cancer is found in patients with cryptorchidism,15 developing in both the nondescended and the contralateral descended testes.
When examining patients with a testicular mass, evaluation for gynecomastia should also be performed. Leydig's cells produce testosterone, and 30 percent of patients with Leydig's cell tumors present with gynecomastia. The etiology for gynecomastia in germ cell tumors is unclear.16 Rarely, tumors of the testis present with manifestations of systemic disease, such as hemoptysis from pulmonary metastases, a supraclavicular mass from lymph node metastases, or an abdominal mass from retroperitoneal lymphatic spread or primary tumor arising from an undescended intra-abdominal testis.
The scrotum should be transilluminated, since a reactive hydrocele may accompany testicular cancer. Scrotal ultrasonography will help define suspected lesions; testicular ultrasound has proved to be highly reliable in differentiating between intratesticular and extratesticular lesions.17 Other diagnostic procedures include tumor marker screening: serum alpha fetoprotein (AFP) and human chorionic gonadotropin (HCG), along with lactate dehydrogenase (LDH). An abdominal computed tomographic (CT) scan should be performed for staging, as well as a chest film and a CT scan of the lungs for evaluation of metastatic disease.15
Pathogenesis. Ninety-seven percent of testicular tumors are germinal in origin, with seminoma being the most common, followed by embryonal cell carcinoma, teratoma and choriocarcinoma.15 Testicular tumors spread via lymphatic drainage, which follows predictable and preferential pathways.18 Seminomas typically spread along the lymph system in a stepwise fashion. Some nonseminomatous germ cell tumors (NSGCT) can also spread hematogenously and present with pulmonary manifestations. Other tumors of nongerminal origin include Leydig's cell tumors, Sertoli's cell tumors and gonadoblas-toma. Serum AFP is excreted to varying degrees by NSGCT but not by pure seminoma. An elevated AFP level implies NSGCT or mixed tumor. About one half of NSGCT and mixed tumors will secrete beta HCG, as will about 10 percent of pure seminomas. LDH is elevated in approximately 60 percent of patients with NSGCT. While it is not specific, LDH can be an indicator of tumor burden and can be used to follow patients with cancer of the testis. In any patient with suspected testicular cancer, AFP, beta HCG and LDH levels should be obtained before starting therapy.19 These markers can help with diagnosis and management. Significant levels of HCG or AFP should not be detectable in patients without cancer.
Management. Radical orchiectomy with high ligation of the spermatic cord via an inguinal approach is appropriate for surgery on testicular masses. A surgical approach through the scrotum can lead to scrotal recurrence or inguinal lymph node metastases. Histologic diagnosis from the orchiectomy and clinical staging dictates further therapy. Advanced spread of disease may require debulking via chemotherapy. Seminomas are very radiosensitive and therefore most early-stage seminomas are treated with orchiectomy and radiation therapy. Advanced stage seminomas and nonseminomatous tumors can be treated with several chemotherapeutic regimens in addition to orchiectomy and lymph node dissection. If levels have previously been found to be elevated, serum AFP and HCG levels can be followed to detect recurrence of disease.
Prognosis. Five-year survival rates exceed 90 percent in many series. The tremendous improvement in cure rates is due in large part to the introduction of cisplatin (Platinol) chemotherapy. Further research is necessary to decrease toxicity of therapy while maintaining efficacy. Relapses usually occur within 18 months of initiation of chemotherapy.15
Benign Causes of Testicular Masses
Hydrocele
Mechanism. A hydrocele is a collection of peritoneal fluid between the parietal and visceral layers of the tunica vaginalis surrounding the testicle. In infants, hydroceles are due to incomplete obliteration of the processus vaginalis. This communicating hydrocele allows the peritoneal fluid to pass between the peritoneal cavity and the layers of the tunica vaginalis. This defect usually closes spontaneously within the first year of life and requires no specific therapy. A noncommunicating hydrocele presenting in an adult may represent an imbalance in the secretory and absorptive capacities of the layers of the tunica vaginalis, such as from injury or infection causing an inflammatory reaction. It may also accompany testicular neoplasm or torsion (Figure 3).
FIGURE 3.
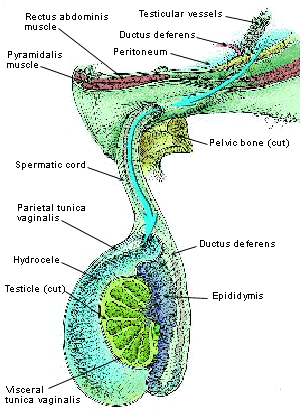
Hydrocele.
Clinical Presentation. A hydrocele appears as a painless scrotal swelling that can be transilluminated. The swelling may be small and soft before the patient arises in the morning but worsen throughout the day, becoming large and tense. Patients may complain of unilateral weight and bulk. Trauma to the scrotum may cause hemorrhage into the hydrocele sac. A new hydrocele or one that hemorrhages after minor trauma may signal testicular cancer.
Management. A hydrocele that occurs during infancy may spontaneously resolve with the closure of the processus vaginalis and, therefore, surgical treatment should be withheld until after the first year of life. Treatment may be necessary for a very large or enlarging hydrocele or for an associated indirect hernia.20 Aspiration of the fluid of a communicating hydrocele is generally unsuccessful because of the patent connection with the peritoneum. In adult males, aspiration of the fluid may be necessary to carefully palpate the testis. A scrotal ultrasound should be considered if the diagnosis is in question, since a reactive hydrocele may occur with a testicular neoplasm. Adults do not require therapy for hydrocele unless complications are present, such as discomfort from the bulky mass or a tense hydrocele that may diminish circulation and lead to atrophy. Trauma to the scrotum may cause hemorrhage into the hydrocele sac.
Varicocele
A varicocele (Figure 4) is an abnormal tortuosity and dilation of the pampiniform venous plexus and internal spermatic vein. A varicocele is present in up to 20 percent of all males and is often asymptomatic. It is the most common surgically correctable cause of male infertility, occurring in approximately 30 percent of infertile men.21 The causes of infertility in such patients are unknown, although many theories focus on the elevated testicular temperature that is due to the increased blood flow, with a resultant decrease in spermatogenesis and sperm motility. A majority of infertile males with varicocele will note improved semen parameters after surgical repair.
FIGURE 4.
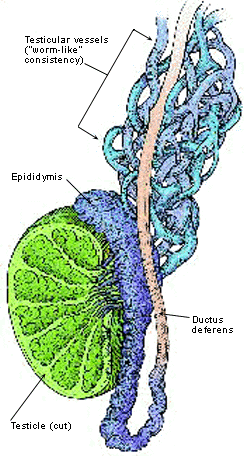
Varicocele.
Clinical Presentation. Most varicoceles occur on the left side, largely because of the differences in the venous drainage patterns of the right and left testicular veins. The left testicular vein drains into the renal vein and the right testicular vein drains directly into the vena cava. Patients may report a mass lying posterior to and above the testis. Dilation of veins is commonly decreased when the patient is supine, and dilation and tortuosity are increased when the patient is upright. Patients should be examined in both positions and should perform the Valsalva maneuver while standing to accentuate dilation. The classic description is that of a “bag of worms” superior to the testicle.
Management. Not all varicoceles are associated with infertility, and not all require correction. The presence of an abnormal semen analysis in patients with a clinically detectable varicocele is an indication for treatment if the patient is infertile. Some varicoceles are symptomatic, causing a dull ache or a heavy sensation, and this is also an indication for treatment. Treatment of varicoceles is directed at occlusion of the dilated testicular veins, either through surgical ligation or injected sclerotherapy. The sudden occurrence of a left-sided varicocele in an older man should prompt evaluation for a possible renal tumor with resultant occlusion of the spermatic vein. A right-sided varicocele would warrant consideration of possible vena cava obstruction.
Spermatocele
A spermatocele (Figure 5) usually presents as a painless cystic mass separate from the testis. Typically, a spermatocele is located superior and posterior to the testis, is freely movable and transilluminates easily. Aspiration of the contents usually reveals dead sperm. No treatment is necessary unless the mass is bothersome.
FIGURE 5.
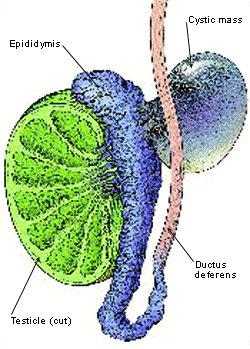
Spermatocele.

