Although the cause or causes of sudden infant death syndrome (SIDS) remain unknown, the incidence of SIDS is on the decline in the United States and other countries. This decline has been accomplished largely through public education campaigns informing parents about several important factors associated with an increased risk of SIDS. These factors are prone and side infant sleeping positions, exposure of infants to cigarette smoke and potentially hazardous sleeping environments. Risk-reduction measures such as placing healthy infants to sleep in the supine position, avoiding passive smoke exposure both before and after birth and optimizing crib safety are beginning to lower the SIDS rate in this country. Through patient education, family physicians can further reduce the incidence of the number one cause of death in infants one week to one year old.
After decades as the number one cause of death in infants between one week and one year of age, sudden infant death syndrome (SIDS) is declining in the United States.1 This change was not brought about by breakthrough discoveries of the cause or causes of SIDS, but by public education about risk factors for SIDS.1 When armed with the latest facts about SIDS risk reduction, the family physician is uniquely positioned to inform parents about the disorder and help them institute risk-reduction measures, thereby having a major impact on the SIDS rate.
SIDS is defined as “The sudden death of an infant under one year of age that remains unexplained after a thorough case investigation, including performance of a complete autopsy; examination of the death scene; and review of the clinical history.”2 SIDS is unique because, by definition its major presenting symptom is unexplained death, the diagnosis is based entirely on what is not found. SIDS is, in other words, a diagnosis of exclusion.
Until very recently, the United States averaged 1.3 to 1.4 SIDS deaths per 1,000 live births.1 Numerous theories and interventions, including home cardiorespiratory monitoring, came and went with little or no impact on the incidence of SIDS. Until recently, most SIDS research aimed to find the cause or causes of SIDS. It was widely assumed that SIDS could be reduced or eliminated if researchers could just find a physiologic abnormality or “predictor” that would allow prospective identification of infants with an increased risk of SIDS. To date, however, no predictors have been identified, and the occurrence of SIDS still cannot be predicted in individual infants.3
New Directions in SIDS Research
In the late 1980s, investigators realized that it was not necessary to understand the basic underlying cause or causes of SIDS in order to do something about it. Mounting evidence suggested that certain factors, such as sleeping in the prone position or exposure to cigarette smoke, were associated with an increased risk of SIDS. In the late 1980s, several groups of investigators set out to determine if the incidence of SIDS could be reduced by changing selected child-care practices such as sleeping position, cigarette-smoke exposure and use of potentially hazardous bedding materials, and by using breast feeding rather than bottle feeding.4–7 The early results of large-scale public health campaigns from countries such as New Zealand were striking: SIDS rates began to decline soon after the initiation of public education drives.4 As more and more similar results emerged from studies in various countries, it became clear that risk-reduction measures could be effective in reducing the incidence of SIDS.
The most current figures for the United States (1994) indicate that the incidence of SIDS has declined approximately 20 to 30 percent since 1992. Much of this decline has been attributed to the 1992 recommendations of the American Academy of Pediatrics (AAP) that healthy infants be placed on their backs for sleep.1,8 In countries where the prone sleeping rate has been reduced to no more than 5 to 10 percent, the reduction in the SIDS rate has approached 70 to 80 percent. Although the final data are not yet available, the SIDS rate for 1995 is projected to be approximately 0.85 SIDS deaths per 1,000 live births.1 If confirmed, this would represent a nearly 40 percent decline from the SIDS rate of the last two decades in the United States (Figure 1).1,9
FIGURE 1.
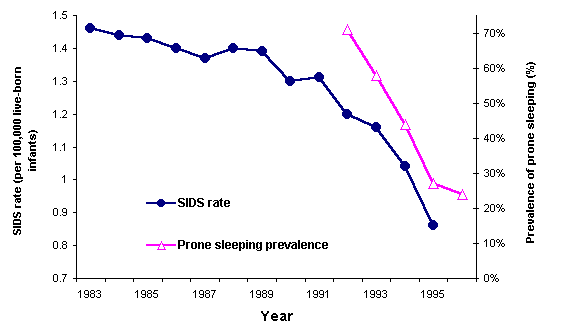
SIDS rate versus prone sleeping rate in the United States, 1983 to 1995 (1995 data are preliminary).
This remarkable decline was brought about by encouraging parents to follow simple risk-reduction measures, based on major modifiable risk factors for SIDS identified by epidemiologic studies. Headway must still be made, however, in the area of pre- and post-natal cigarette-smoke exposure which, if reduced, could contribute to an additional substantial reduction in the incidence of SIDS. Although estimates vary, it is likely that in the United States such risk-reduction measures, if widely practiced, could reduce the rate of SIDS by 50 percent or more.
Risk-Reduction Measures: What to Tell Parents
The major risk-reduction measures supported by available scientific research are (1) having healthy babies sleep in the supine position; (2) not exposing babies to cigarette smoke, either during pregnancy or after birth; (3) making the sleeping environment as safe as possible; and, possibly, (4) breast feeding rather than bottle feeding.
Sleeping Position
Available data indicate that the prone (on the stomach) sleeping position is associated with the highest risk of SIDS; the supine, or back, position, is associated with the lowest risk, and the side-lying position falls in between.9,10 Basically, “back is best” from a SIDS risk-reduction point of view.
The mechanisms by which the prone sleeping position might lead to SIDS are not known. Studies suggest that the prone sleeping position may increase SIDS risk by increasing the probability that the baby rebreathes his or her own expired gas, leading to carbon dioxide build-up and low oxygen levels; by causing upper airway obstruction; by interfering with body heat dissipation, leading to overheating; and by a variety of other proposed mechanisms. Whatever the mechanism, evidence from numerous countries, including the United States, suggests that changing babies from the prone to the supine sleeping position results in a substantial decline in the SIDS rate.
It is important to note that the supine sleeping position is currently recommended for healthy infants by the AAP and the National Institutes of Health.8,9 For infants with medical conditions such as symptomatic gastroesophageal reflux, sleeping position recommendations must take into account the potential risk of sleeping supine, especially for infants with swallowing dysfunction or unilateral vocal cord paralysis, who have an increased risk of aspiration. However, at the present time no scientific evidence shows that vomiting and aspiration pose a threat to healthy infants. Countries that have switched predominantly from the prone to the supine sleeping position for infants have shown no increase in reports of choking on vomitus or of aspiration pneumonia.11
Although vomiting and pneumonia do not appear to be a cause for concern, parents should be aware of other “side effects” of the supine sleeping position. Infant development may be affected, with minor delays in the maturation of motor skills.12 However, there is no evidence that these changes in motor development have permanent or adverse effects. Similarly, when a baby sleeps exclusively in the supine position, some transient changes in head shape may occur, such as flattening of the back of the head, leading to parental concerns or even misdiagnosis of craniosynostosis. At the present time no evidence has been found to show that this flattening is harmful to infants or associated with any permanent effects on head shape.13 Orthopedic specialists recommend simply varying the baby's head position during sleep to minimize the effects on head shape of sleeping in the supine position.
Some parents have gone overboard with the supine-position recommendations and have kept their babies supine even when awake and playing. Physicians should emphasize that the supine-position recommendation applies only to sleep. When awake, the baby can and should spend time in the prone position, which is important for infant development. It is important to remember that the peak incidence of SIDS occurs between two and four months of age, about the same time that many women decide to go back to work. Infants this age still sleep during the day and, when they are at day care facilities, they may be placed prone for sleep and/or placed in nonapproved sleeping environments (sofas, adult beds, etc.), which could be hazardous.
Cigarette Smoke Exposure
Smoking during pregnancy exposes the developing fetus to toxins and other potentially harmful effects of cigarette smoke. Numerous research studies confirm that maternal smoking during pregnancy increases the risk of SIDS.5,6,14–17 In addition, increasing evidence suggests that exposing the baby after birth to cigarette smoke also increases the risk of SIDS.18,19 The increase in SIDS risk appears to be related to the “dose” of passive-smoke exposure—the greater the exposure to smoke both before and after birth, the higher the risk of SIDS.15,18
Although several reasonable theories could potentially explain how cigarette-smoke exposure could increase the risk of SIDS (e.g., toxic effects of nicotine, fetal oxygen delivery lowered by carbon monoxide, irritant effects of smoke on the infant's lungs after birth), the link or links are still being explored and are not yet understood. However, the weight of the epidemiologic evidence linking smoke exposure and SIDS is strong.14 Mothers should not smoke during pregnancy. After birth, the baby should not be exposed to environmental cigarette smoke. Studies suggest that smoking anywhere in the home may increase the risk, so just going into another room to smoke is not sufficient. Current data suggest that no one should smoke in the home or in a car with a baby. However, because smoking is addictive behavior, it is not enough to simply tell people to stop smoking. Smoking cessation counseling before and during pregnancy is an important part of prenatal care, for both the expectant mother and the father, and should be a major component in risk-reduction efforts. This counseling should continue postnatally as needed. Not all states have regulations prohibiting environmental cigarette-smoke exposure in day care centers. Therefore, parents should be reminded to explore the practices of their day care provider and provide specific instructions and guidelines to the provider to be sure that their baby won't be exposed to cigarette smoke.
Potentially Hazardous Sleeping Environments
The sleeping environment also appears to be linked to SIDS in some cases.20 A recent study from the U.S. Consumer Products Safety Commission (CPSC) indicated that as many as 30 percent of deaths diagnosed as SIDS-related in the past may have been related to unsafe sleeping environments or unsafe bedding material.21,22 Studies going back three decades have indicated that soft bedding material may be hazardous for young infants. A recent resurgence of research in this area has confirmed that soft mattresses, pillows and other bedding material can be hazardous and may be associated with infant deaths diagnosed as SIDS.
The CPSC has recently been active with public education efforts concerning “crib safety.” Although the recommendations appear to be common-sense measures for ensuring that the crib environment is as safe as possible, many parents are not aware of or have not thought about some of the potential hazards. Recommendations include making sure that the crib is in good working order with no missing or broken parts; being sure that the mattress meets CPSC standards, is in good condition and is the proper size for the crib; and positioning the crib so that curtain or blind cords do not hang down into or near the crib and pose a possible strangulation hazard.21,22
Other recommendations, such as positioning the baby for sleep on the back, are based on mounting evidence that prone and side sleeping positions are associated with an increased risk of SIDS compared with the back sleeping position. Recommendations against using soft bedding, thick blankets or comforters, pillows, bumpers and soft crib toys are based on increasing evidence that use of these items is also associated with a higher SIDS risk, possibly by increasing the risk of carbon dioxide rebreathing (asphyxiation).
Finally, because of the potential hazards of overheating, it is generally recommended that for sleep, a baby should be lightly dressed and covered with a sheet or thin blanket, and the room temperature should be such that it would be comfortable for an adult in a short-sleeve shirt. Swaddling and tight “tucking in” of infants is not recommended.
It is currently recommended that infants not be placed for sleep on adult beds.23 This raises obvious questions about infant-parent co-sleeping, which is believed by some researchers to be potentially beneficial to both parents and infants.24 Research data on this topic, at the present time, do not provide a clear answer. Some studies have found infant/parent co-sleeping to be associated with a higher risk of SIDS, while others have not.10,25 In addition, several studies showing a correlation between co-sleeping and increased SIDS risk also find that co-sleeping appears to be linked with other risk factors, such as smoke exposure.10,26 Although studies of maternal-infant interactions during sleep indicate several potential benefits of co-sleeping,27 there is no question that adult bedding material can be dangerous for infants, and infant/parent co-sleeping may expose an infant to this risk. Studies are ongoing in an effort to answer questions concerning the risks versus benefits of co-sleeping and whether it can be done in a manner that does not increase the SIDS risk. Until this information is available, it would seem prudent not to expose infants to the well-documented hazards of sleeping on adult bedding materials.
Breast Feeding
After numerous studies on breast feeding and SIDS, results are conflicting, and the relationship is still unclear. Several research studies have found a relationship between breast feeding and a lowered SIDS risk,28 while others have not found such a relationship.10 Still other studies have found a lower rate of SIDS in breast-fed infants, but statistical analysis suggests that it was not the breast feeding per se that was responsible for the apparent relationship.29 Contrary to the common view, no evidence shows that breast feeding per se is “protective” against SIDS. Of course, breast feeding offers many potential physiologic and psychologic benefits to mother and infant and is, in general, preferable to bottle feeding and recommended.
Infant Home Monitoring
Risk-reduction measures are apparently responsible for the recent 20 to 30 percent decline in the incidence of SIDS, while infant home monitoring has had no demonstrable impact in two decades. This result raises obvious questions about the role of infant home monitoring as a SIDS risk-reduction measure. At the present time, infant home monitoring is still recommended for use with any infant believed to be at risk of sudden death, as suggested by the 1987 National Institutes of Health Consensus Development Conference on Infantile Apnea and Home Monitoring.30 This recommendation includes preterm infants still having abnormal apnea or bradycardia when ready for discharge from the nursery, infants with one or more episodes of severe apparent life-threatening event (ALTE) and infants with medical conditions (e.g., central hypoventilation, tracheostomy) or on respiratory support (e.g., supplemental oxygen, home ventilators).
The original NIH consensus conference30 recommended home monitoring for “siblings of two or more SIDS victims.” The weight of current evidence strongly suggests that the risk of SIDS is increased significantly in subsequent siblings, although the impact of home monitoring in this subgroup has not been adequately studied.31 It is now common practice to disregard the “two or more” recommendation and offer home monitoring for any subsequent sibling of a SIDS victim.
Home monitoring in the past had little effect on the incidence of SIDS, most likely because, for the most part, subgroups with the wrong risk factors were being monitored. Studies of signs and symptoms preceding SIDS have shown that over 90 percent of parents of SIDS victims had not observed the infant turn blue or stop breathing before death.32 The great majority of infants dying of SIDS are apparently healthy infants who do not meet the criteria for home monitoring. Therefore, it is not surprising that home monitoring, as it was used in the past, did not have a significant impact on the overall SIDS rate. In addition, for many years there was an excessive focus on central apnea per se, the presence of which is now known not to be a risk factor for SIDS.
This does not mean, however, that monitoring should not be used in selected infants such as siblings of SIDS victims and others believed to be at increased risk of sudden death. A large collaborative study31 of home infant monitoring, sponsored by the NIH National Institute of Child Health and Development, is currently under way. Until further recommendations are forthcoming from the NIH or the AAP, home monitoring is still recommended for the indications outlined above.
The Family That Has Already Lost a Child to SIDS
The family that has already lost a child to SIDS requires special attention. The fact that the infant's death is unexplained nearly always leads to intense self-questioning and self-blaming by parents and other caregivers. It is typical for parents to seek out as much information about SIDS as possible, analyzing every possible theory as to how it may relate to their own child's death. Adding to the guilt and confusion is the common misperception on the part of the general public that risk factors are causes. Therefore, if the baby was sleeping on its stomach or was bottle-fed, or if there was smoking in the household, parents are likely to believe that these things must have “caused” SIDS to occur. It takes a well-informed yet sensitive physician to explain risk factors so that the family is adequately informed about risk reduction efforts that can be made for a subsequent baby, while emphasizing the relatively lower risk of recurrence. In addition to the family physician, numerous local, national and Internet resources are available to families (Table 1).
TABLE 1 SIDS Information and Support Resources for Physicians and Parents
| The SIDS Network | |
| 9 Gonch Farm Rd., Ledyard, CT 06339 | |
| Telephone: 800-560-1454; fax: 860-887-7309 | |
| E-mail: sidsnet@sids-network.org | |
| Internet address: http://sids-network.org | |
| Association of SIDS and Infant Mortality Programs (ASIP) | |
| 630 W. Fayette St., Room 5-684, Baltimore, MD 21201 | |
| Telephone: 410-706-5062; fax: 410-706-0146 | |
| The National Sudden Infant Death Syndrome Resource Center (NSRC) | |
| 2070 Chain Bridge Rd., Suite 450, Vienna, VA 22182 | |
| Telephone: 703-821-8955; fax: 703-821-2098 | |
| Internet address: http://www.circsol.com/SIDS/ | |
| The Canadian Foundation for the Study of Infant Deaths | |
| #308, 586 Eglinton Ave. East, Toronto, Ontario, Canada M4P 1P2 | |
| Telephone: 800-END-SIDS; fax: 416-488-3864 | |
| E-mail: sidscanada@inforamp.net | |
| Internet address: http://www.sidscanada.org | |
| SIDS Center of New Jersey | |
| The Don Imus WFAN Pediatric Center, | |
| Hackensack University Medical Center, 30 Prospect Ave., Hackensack, NJ 07601 | |
| Telephone: 800-996-5002; fax: 201-996-0754 | |
| Sudden Infant Death Syndrome Alliance | |
| 1314 Bedford Ave., Suite 210, Baltimore, MD 21208 | |
| Telephone: 410-653-8226; fax: 410-653-8709 | |
| E-mail: sidshq@charm.net | |
| National Institute of Child Health and Human Development | |
| Back to Sleep, 31 Center Dr., | |
| MSC2425, Room 2A32, Bethesda, MD 20892-2425 | |
| Telephone: 800-505-CRIB | |
| Internet address: http://www.nih.gov/nichd/news/SIDS_HP_2/home1B.html | |
| American Sudden Infant Death Syndrome (SIDS) Institute | |
| 6065 Roswell Road, Suite 876, Atlanta, GA 30328 | |
| Telephone: 800-232-7437; fax: 404-843-0577 | |
| E-mail: prevent@sids.org | |
| Internet address: http://www.sids.org | |

