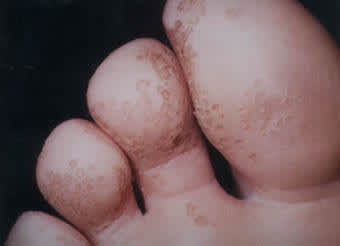
For several months, a 17-year-old male athlete noticed that his feet had an itchy, burning sensation at the heels and toes. His foot odor had become so malodorous (somewhat akin to rotting fish) that he would not remove his shoes except immediately before washing his feet. Washing made the odor somewhat milder, but only for a short time. The patient had tried an over-the-counter “athlete's foot” powder without results. He had no other health problems and was not taking any medication. The accompanying figure shows the toes of his right foot.
Question
Which one of the following is the most likely diagnosis given the history and physical appearance of the foot above?
A. Tinea pedis.
B. Superficial candidiasis.
C. Dyshidrotic eczema.
D. Allergic contact dermatitis related to athletic shoe rubber.
E. Pitted keratolysis.
Discussion
The answer is E: Pitted keratolysis is an aptly named disorder that usually affects younger patients, especially athletes or those who spend prolonged periods in occlusive footwear.1,2 Bacterial species in the Corynebacterium and/or Micrococcus families invade the stratum corneum (the superficial “dead” part of the skin) and excrete exoenzymes (keratinase), which digest the keratin, creating the characteristic pits shown in the figure and producing a foul odor. These bacteria produce porphyrins that reveal bright coral-pink fluorescence in the pits under Wood's light, which confirms the diagnosis. A false-negative result may occur if the patient has recently washed the feet. For this reason, a late-afternoon examination of the feet may be the most revealing. While systemic antibiotics such as clindamycin (Cleocin) or erythromycin (a 10-day course at dosages appropriate for age and weight) will satisfactorily treat the condition, most cases respond to therapy for one to two weeks with twice-daily applications of topical clindamycin or erythromycin gels and lotions. Gels seem to be somewhat more effective than lotions but may be significantly more irritating if the inflammation and pitting are particularly severe. Shoes may harbor the smell forever and will need to be replaced.
Candidiasis rarely occurs in the immunocompetent person. Other fungal infections may have bullous presentations that can leave denuded areas, although usually not pits. These infections are best diagnosed with a potassium hydroxide scraping and may be treated with any topical or systemic antifungal agents. Dyshidrotic eczema (also called dyshidrosis or pompholyx) is an intensely pruritic condition that affects the hands more often than the feet and presents with tapioca-like “bubbles” in the skin. While bubbles may appear on the palms and soles, and may be rubbed and scratched enough to leave small pits, the sides of the digits are more characteristically affected. Many cases of dyshidrotic eczema are the result of an occult allergen causing an allergic contact dermatitis.
“Shoe dermatitis” is most likely related to the rubber and elastic compounds in shoes, the elastic glues used to bind shoe components and the foam inserts used in shoe footbeds. A battery of patch tests or patch tests to parts of the suspect shoe itself may reveal that the patient is sensitive to one or more compounds found in modern footwear.3 Mid- to high-potency topical steroids may benefit patients with chronic cases as long as the offending type of footwear is avoided and a diagnosis of tinea pedis is excluded. A course of systemic steroids of no less than two weeks' duration is required for treatment of severe, acute eczematous outbreaks.

