Skin infections are common and may be caused by bacteria, fungi or viruses. Breaks in the skin integrity, particularly those that inoculate pathogens into the dermis, frequently cause or exacerbate skin infections. Bacterial skin infections caused by corynebacteria include erythrasma, trichomycosis axillaris and pitted keratolysis. Staphylococci may cause impetigo, ecthyma and folliculitis. Streptococcal skin infections include impetigo and erysipelas. Human papillomavirus skin infections present as several different types of warts, depending on the surface infected and its relative moisture, and the patterns of pressure. The many dermatomycoses (skin infections caused by fungi or yeasts) include tinea capitis, tinea barbae, tinea cruris, tinea manus, tinea pedis and tinea unguium (onychomycosis). Candidal infections occur in moist areas, such as the vulva, mouth, penis, skinfolds and diaper area. Wounds caused by wood splinters or thorns may result in sporotrichosis. Animal bites may result in complex, serious infections, requiring tetanus and, possibly, rabies prophylaxis in addition to appropriate antibiotic therapy.
The skin has the largest surface area of all of the body organs and is the most exposed organ. Although the skin is remarkably effective in providing protection against the external environment, skin infections are nevertheless a common presentation in most family practices.
Bacterial Skin Infections
Skin infections are often the result of a break in the integrity of the skin. Bacterial skin infections include erythrasma and related diseases, impetigo, ecthyma, folliculitis, erysipelas and cellulitis. While there are certainly other bacterial skin infections, they are either uncommon or result from systemic illness. These types of bacterial skin infections are not discussed in this article.
Erythrasma and Related Conditions
Erythrasma is a superficial skin infection caused by corynebacteria that commonly occurs in intertriginous spaces. While moderate itching and discomfort may be noted, the patient generally presents with only skin-color changes in the infected area. The infected skin is often reddish-brown, may be slightly raised from the surrounding skin and may show the appearance of central clearing. The lesions are largely confluent but may have poorly defined borders. Because of the production of porphyrins by the infecting Corynebacterium, Wood's light demonstrates the lesions as a coral-pink color.
Erythrasma is often confused with a fungal infection, such as tinea cruris, but this confusion is of little consequence since corynebacteria are often eradicated with an imidazole cream (such as Miconazole and others), the agent used to treat tinea infections. The preferred treatment for erythrasma is a course of oral erythromycin, plus vigorous daily cleansing with soap and water.
Other diseases commonly caused by corynebacteria include trichomycosis axillaris and pitted keratolysis. Patients affected by trichomycosis axillaris present with complaints of a disagreeable underarm odor and a history of hyperhidrosis and poor hygiene. Examination reveals the underarm hair to be coated with black, yellow-white or reddish deposits. Daily cleansing with soap and water generally cures the infection, and regular use of antiperspirants aids in prevention. Topical erythromycin is occasionally required to eliminate the infection.
Patients with pitted keratolysis present with complaints of painful burning of the feet and a history of wearing occlusive footwear in warm, damp environments. Examination reveals small, punctate, pitted lesions on calloused areas of the feet and a disagreeable foot odor. Frequent cleansing of the feet and application of topical erythromycin are generally effective in eliminating the infection. Use of antiperspirants also aids in cure and prevents recurrence.
Impetigo
Impetigo is a common infection in children that may also occur in adults. It is generally caused by either Staphylococcus aureus or streptococci. Patients report skin lesions, often with associated adenopathy, but have minimal systemic signs and symptoms. Impetigo may present in two forms: small vesicles with a honey-colored crust or purulent-appearing bullae. Bullous impetigo is less common than small-vesicle impetigo. S. aureus is the organism that commonly causes bullous impetigo. S. aureus is also the most frequently found organism in small-vesicle impetigo, although group A beta-hemolytic streptococcus is also a common pathogen in patients over the age of two.1
Systemic treatment employs beta-lactamase–resistant antibiotics. Topical mupirocin (Bactroban) is effective in 90 percent of cases and is more effective than oral erythromycin.1 To date, topical mupirocin has not been compared with other commonly used oral antibiotics, many of which have efficacy superior to that of erythromycin. Application of mupirocin ointment to the nares twice a day for five days may be efficacious in outbreaks of recurrent methicillin-resistant S. aureus skin infection, if the nares are colonized.2 Erythromycin resistance is now common among strains of S. aureus3 (Figure 1). Rarely, a poststreptococcal illness, such as nephritis, may be a complication when impetigo is caused by certain strains of group A beta-hemolytic streptococci.
FIGURE 1.
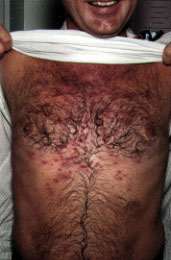
Erythromycin-resistant Staphylococcus aureus infection. This pustular skin lesion, which was infected with S. aureus, failed to respond to the macrolide antibiotic azithromycin (Zithromax) but was cured with cephalexin (Keflex) therapy.
Ecthyma
Ecthyma occurs in debilitated persons, such as patients with poorly controlled diabetes, and is generally caused by the same organisms that cause impetigo. The patient presents with moderately painful lesions with adherent crusts, generally on the legs; the lesions may subsequently become purulent, poorly healing ulcers. These lesions tend to be deeper seated than those of impetigo.
Improved nutritional status and two to three weeks of treatment with a beta-lactamase–resistant antibiotic are usually required to bring about resolution of the lesions.4
Folliculitis and Related Conditions
Patients with folliculitis present with yellowish pustules at the base of hairs, particularly on the scalp, back, legs and arms. Often, the patient lives in a warm, damp climate. Persons with diabetes are particularly susceptible to this infection. Frequent use of soap and water and the use of topical antibiotic agents, such as mupirocin or bacitracin (Neosporin, Polysporin), generally clear the lesions. Occasionally, the addition of a systemic antistaphylococcal agent is required.
Hot-tub folliculitis is a special form of folliculitis caused by Pseudomonas. It occurs when patients bathe in poorly maintained hot tubs. Hot-tub folliculitis is generally a self-limited condition, although the infection can progress to a serious illness in immunocompromised persons. If the lesions do not resolve within five days of discontinuing hot-tub use, therapy with antibiotics such as ciprofloxacin (Cipro) should be considered.4,5
Furuncles, or boils, are more aggressive forms of folliculitis. Patients present with a painful, often fluctuant swelling in a non–weight-bearing area, most commonly areas of friction, the nasal area or the external ear. Treatment often requires drainage of the lesion. Antibiotic therapy should be considered if the furuncle is not yet fluctuant, if there is evidence of surrounding cellulitis or lymphadenitis, or if the lesion is on the face. A carbuncle is a collection of furuncles and typically occurs on the back of the neck in middle-aged and older men. The lesions have many interconnecting sinuses and tend to recur despite drainage and antibiotics. Surgical drainage and resection of the lesions is often necessary.
Hidradenitis suppurativa, which initially may be confused with furunculosis, is pathologically related to furuncles.6 Hidradenitis often affects persons with concurrent acne conglobata, although it may occur in other persons as well. Persons with hidradenitis generally have chronic and recurrent episodes of multiple furuncles in the axillae, mons pubis, scrotum, labial or inguinal areas. Drainage and antibiotics are useful, and hormonal treatment with leuprolide (Lupron) and cyproterone acetate (not available in the United States) has been successful.7 Patients may also benefit from the use of isotretinoin (Accutane), 0.5 to 2.0 mg per kg daily in two divided doses for 16 to 20 weeks.
While medical treatment offers a conservative approach, studies of the use of leuprolide, cyproterone acetate and isotretinoin in the treatment of hidradenitis are few, and these treatments are not approved by the U.S. Food and Drug Administration. Surgical resection of the affected area is often necessary.7
Erysipelas
Erysipelas presents acutely as marked redness, pain and swelling in the affected area. Erysipelas may be increasing in frequency, and infection involving the legs has replaced facial infection as the most common site.8 The lesion has a sharply defined, if somewhat serpiginous, spreading border, and prominent adenopathy is present. The patient may appear systemically ill, with increased temperature and an elevated white blood cell count. The illness is generally believed to be caused by beta-hemolytic streptococci, but recently other organisms have also been implicated.8,9
An oral antibiotic, usually penicillin, is sufficient for treatment. Sepsis may occur in persons with diabetes and in immunocompromised persons, and hospital admission should be considered for such patients, as well as for any patient with significant systemic signs and symptoms.
Cellulitis
Cellulitis may be caused by a variety of organisms, including group A streptococci, S. aureus, Haemophilus influenzae and, in coastal areas, halophilic Vibrio species. Cellulitis is a relatively deep infection, generally resulting from a break in the skin. It involves subcutaneous spaces in addition to the dermis. The patient presents with pain, redness, warmth and systemic symptoms such as fever. The affected area appears red and is warm to the touch, but the erythema does not have a sharply demarcated border. Lymphangitic streaking and lymphadenopathy are commonly present. Lymphatic drainage is damaged by cellulitis, which renders the area predisposed to subsequent infections (Figure 2).
FIGURE 2.
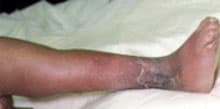
Cellulitis in a patient with congenital and surgical deformities of the leg. Admission to the hospital for administration of intravenous nafcillin (Nafcil) was required to resolve the infection. This case illustrates the problem of predisposition to cellulitis after lymphatic drainage or circulation has been compromised.
Treatment includes immobilization and elevation of the affected area, and antibiotics directed against the suspected organism, which is usually beta-hemolytic streptococci or S. aureus. If the patient has a history of a penetrating injury that occurred in brackish water, coverage for marine Vibrio species should be instituted. A suggested regimen is oral doxycycline, 100 mg twice daily for 10 days, and intravenous ceftazidime (Ceptaz, Fortaz, Tazicef), 2 g every eight hours for five days.
Warts
Viruses commonly cause skin infections. Human papillomavirus (HPV) causes focal areas of epithelial hyperplasia, referred to as warts. Indeed, selected types of HPV are capable of inducing malignant transformation of the epithelium, including that of the cervix. Commonly occurring warts include common warts, plantar warts, juvenile warts and condylomata.
Common warts usually develop on the extremities. The shape of the wart depends on the body surface affected. Facial warts appear filiform, and warts in areas subject to abrasion appear as a flattened mosaic of multiple warts. Plantar warts on the heel and sole are surrounded by hyperkeratotic, callus-like skin. Plantar warts may be quite painful when they occur on weight-bearing surfaces. Multiple plantar warts may combine to become a large “mosaic wart.” Flat warts are small, 1- to 4-mm papules, often occurring on the face and legs of children and adolescents. While inconspicuous at first, they propagate rapidly, often into the hundreds.10
Condylomata occur in intertriginous areas and on mucous membranes, commonly in the genital and rectal areas. This infection may be transmitted sexually. The lesions begin as small papules, which often become whitish with maceration as they grow. Vulvar and anogenital condylomata generally exhibit a cauliflower-like appearance. The lesions may become quite large and, rarely, may cause destruction of surrounding tissues. Condylomata are associated with cervical carcinoma (especially among smokers), and the rate of penile cancer is higher among men with genital warts than among men without such a history.11 Among the 70 known subtypes of HPV, types 16 and 18 are especially associated with the development of carcinoma. As the ability to identify HPV subtypes is refined, subtyping may become useful in stratifying the patient's risk of cancer.12
No standard and routinely effective treatment for warts exists. Most warts, if left without treatment, spontaneously regress over a period of many months to years. Local treatments that should be considered are cryotherapy, application of fluorouracil cream, application of keratolytic agents (salicylic acid), application of podophyllin, sharp curettage, radiofrequency resection and laser ablation. There are certainly other therapies in use, and experienced clinicians recognize that no one of them is uniformly effective.13 Genital HPV infections are particularly difficult to treat because of the location of the lesions. The use of cryotherapy or podophyllin for external lesions or cryotherapy or laser ablation for any genital lesion has found favor with most clinicians.
Fungal and Yeast Infections
Fungi and yeast are capable of causing many different forms of skin infections, broadly referred to as dermatomycoses. Candida albicans and Trichophyton, Epidermophyton, Microsporum and Malassezia species are the most common infecting organisms. Many of the lesions caused by fungi are distinctive, and diagnosis is primarily based on the presenting pattern rather than on culture or other test results. However, laboratory testing may be helpful if systemic agents are used in the treatment of these infections.14
Dermatophytoses
The dermatophytoses are a group of common infections generally caused by Trichophyton species. These infections include tinea capitis, tinea barbae, tinea corporis, tinea cruris, tinea manus, tinea pedis and tinea unguium.
Tinea Capitis. Tinea capitis is a fungal infection of the scalp, generally occurring in infants and children. The lesions have three characteristic appearances: diffuse, fine scaling; patchy alopecia with broken hairs (“black dot” tinea capitis) and inflammatory, boggy, purulent nodules (kerion). Diffuse scaling is associated with Microsporum audouinii and is more common in white boys than in other patient groups. With Microsporum infections, the hair shaft fluoresces under black light, and this test is useful in distinguishing this infection from seborrheic dermatitis.
“Black dot” tinea capitis, which is caused by Trichophyton tonsurans, presents as patchy alopecia and broken hair shafts—the so-called black dots. This infection exhibits no gender predilection but is more common in blacks and Hispanics than in other groups. T. tonsurans does not fluoresce under black light. Kerions may be misdiagnosed as furuncles.15
The treatment of choice for tinea capitis is griseofulvin (Fulvicin, Grifulvin V, Grisactin, etc.), although itraconazole (Sporanox) and terbinafine (Lamisil) are also being studied for this purpose.16,17
Tinea Barbae. Tinea barbae is an infection of the beard that typically occurs in animal handlers. Patients present with pustular folliculitis of the whiskers, which appear as dusty wicks in the centers of the pustules. Tinea barbae is usually self-limited but may be treated with oral griseofulvin or oral azole antifungal agents such as fluconazole (Diflucan), itraconazole or terbinafine.18
Tinea Corporis. Tinea corporis, the familiar ringworm, is characterized by reddish, scaling, nearly circular lesions with central clearing. Treatment with topical imidazoles generally clears the lesions.
Tinea Cruris. Patients with tinea cruris, or “jock itch,” present with a pruritic, discolored rash on the groin, perianal and inner thigh areas. Tinea cruris may be confused with erythrasma, but the confusion is of little significance, since both conditions tend to respond to imidazole creams. In addition to imidazole creams, washing the area with soap and water and wearing loose-fitting cotton undergarments help treat the infection and prevent recurrence.
Tinea Pedis and Tinea Manus. Tinea pedis is the most common fungal skin infection in North America and Europe.14 Tinea manus, an infection of the hands, is rare but similar to the foot infection. Tinea pedis occurs in three patterns: cracking and maceration in the interdigital spaces (interdigital infection); irregular but sharply defined hyperkeratotic lesions (plantar moccasin-type infection); and itchy, vesicular lesions (vesiculobullous infection).19 All three patterns may occur in the same person.20
Treatment involves the use of imidazole creams and keeping the feet dry by frequently changing socks, avoiding occlusive footwear and applying an antiperspirant to the soles of the feet. Occasionally, systemic treatment is warranted in patients with resistant or particularly painful lesions, especially the hyperkeratotic variety.
Tinea Unguium. The patient with tinea unguium, or onychomycosis, has thickened, difficult-to-trim, brittle nails, usually of the great toe (Figure 3). Onychomycosis may be subtyped into four categories, but the distinction does not affect treatment strategies.21 The patient's complaints are usually cosmetic in nature, rather than functional disability. A substantial number of other disorders can cause nail dystrophy, and some authors recommend obtaining a fungal culture before treatment.22 Cultures that are positive for Trichophyton species are predictive of successful treatment with oral agents. Cultures that grow nondermatophytes, such as Scopulariopsis, generally suggest that the infection will not respond to oral agents.
FIGURE 3.
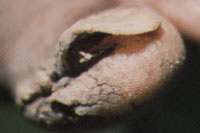
Markedly thickened and deformed nail in a patient with onychomycosis, or tinea unguium. Surrounding skin is also thickened and macerated as a result of occlusive and damp footwear.
Until fairly recently, there was no effective treatment for onychomycosis. However, oral itraconazole, terbinafine and other similar agents can be reasonably expected to cure the condition.23
Oral Candidiasis
Oral candidiasis commonly occurs as thrush in infants and immunocompromised patients. This infection can be divided into a number of different clinical forms, including acute or chronic pseudomembranous oral candidiasis; acute or chronic erythematous; hyperplastic or nodular candidiasis; and medial rhomboid glossitis. Angular cheilitis may accompany oral candidiasis or occur separately.24 In pseudomembranous oral candidiasis, an underlying erythematous base is noted when the creamy white pseudomembrane is removed. Painful, reddened lesions are characteristic in erythematous forms of oral candidiasis. Irregular white plaques that cannot be removed and loss of tongue papillae are features of hyperplastic candidiasis. A diamond-shaped plaque on the dorsum of the tongue is present in medial rhomboid candidiasis.
Angular cheilitis, characterized by cracks and fissures at the corners of the mouth, is more common in elderly patients with poorly fitting dentures. Candidal thrush or angular cheilitis can be treated with topical imidazole creams or troches, although immunosuppressed patients may require systemic therapy.
Candidal Vulvovaginitis
Candidal vulvovaginitis is manifested by vaginal itching and discharge, often accompanied by dysuria and pain on penetration during sexual intercourse. Pelvic examination may reveal a creamy to cheesy, whitish discharge; redness of the vaginal wall and external genitalia may also be present. Candidal spores and hyphae can be visualized on potassium hydroxide preparation and microscopic examination of the discharge.
Topical imidazoles, many now available without prescription, are effective in the treatment of this infection. The use of systemic agents in the routine treatment of vaginal candidiasis is discouraged by some authorities.25 Systemic therapy such as a single 150-mg dose of fluconazole is effective but carries a higher risk of adverse effects than the use of intra-vaginal topical agents.26
Candidal Balanitis
Candidal balanitis occurs primarily in uncircumcised men, particularly men who are obese, have phimosis, are elderly or have diabetes. Poor hygiene and sexual intercourse with a woman who has candidal vulvovaginitis add additional risk. Grayish-white deposits on an inflamed base are noted on the penile prepuce and glans. Thorough cleansing and application of imidazole creams generally eradicate the infection, although systemic treatment may be required, particularly if secondary infection occurs.
Candidal Intertrigo
Candidal intertrigo typically occurs in obese patients with redundant, moist and overlapping skinfolds. Macerated and reddened areas are found under the skinfolds, with surrounding scaling and, often, satellite lesions. Keeping such areas dry and clean, along with use of topical imidazoles, clears the lesions.
Diaper Rash
Candidal diaper rash occurs in infants when poorly absorbent, moisture-trapping diapers are used. Scattered small, reddish lesions with a scaly surrounding “collarette” are present. Use of an imidazole cream and regularly allowing the diaper area to be exposed to air usually clear the rash. Long-term use of imidazole and steroid creams is discouraged and unnecessarily exposes the infant to the risk of adverse topical effects and suppression of the adrenal axis from steroids.
Chronic Paronychia
Chronic paronychia occurs primarily in persons who must keep their hands in rubber gloves or water for long periods of time, such as dentists, dishwashers and bartenders. The nail fold is reddened and may be fluctuant and painful. Treatment with a topical imidazole or systemic ketoconazole or itraconazole is useful.24 Drainage is sometimes needed. Patients should be instructed to thoroughly and frequently dry their hands.
Pityriasis Versicolor
Pityriasis versicolor is also known as tinea versicolor, although the causative agent is Malassezia species and not a dermatophyte. Malassezia species have also been associated with seborrheic dermatitis, atopic dermatitis and folliculitis.24 Persons with this condition are typically adolescents and adults who live in a humid environment. Patients present with light-colored, asymptomatic lesions on the back, chest or buttocks. The lesions may become confluent and scaly as they spread. Scrapings and culture may aid in confirmation of the condition but are generally not necessary.27 Pityriasis versicolor is mildly contagious.
The infection may be treated with selenium-based shampoos, imidazole creams and short courses or single-dose regimens of oral ketoconazole, fluconazole or itraconazole.28
Wound Infections
Wounds break the continuity of the skin and allow organisms to gain access to tissues. Agents that inflict wounds can be grouped by the depth of the wound and by the likelihood that they will serve as carriers for organisms that will cause infection. Wound infections may occur as a result of penetrating trauma from plants, animals, guns, knives or other objects. Various plant products can puncture the skin and result in a wound infection. Because plants are generally made of porous materials, a thorn or other such object can serve as a vehicle for the entry of S. aureus or other organisms into the tissues. Cellulitis commonly occurs after such breaks in the skin.
Sporotrichosis
Sporotrichosis results from traumatic inoculation of rotting wood products. Five variations of sporotrichosis have been described. Lymphocutaneous sporotrichosis manifests as multiple bluish-red areas of swelling along the lymph node chain draining the primary inoculation site. Fixed cutaneous sporotrichosis occurs when prior immunity to the organism keeps the lesion contained as a cluster of wart-like growths at the inoculation site. Sporotrichosis may become disseminated in immunocompromised persons or may be associated with multiple inflamed papulonodules as a result of hematogenous spread. In the mucocutaneous form of disseminated disease, both skin and mucous membranes are involved. Extracutaneous sporotrichosis, another form of disseminated infection, involves bone, the large joints, the eyes, muscle or the kidneys. This last form of infection is rare but particularly dangerous.
Oral potassium iodide is often sufficient treatment for localized disease; however, therapy with amphotericin, flucytosine (Ancobon), itraconazole or ketoconazole should be considered in severe cases. As with any break in the skin, tetanus prophylaxis may be warranted.
Animal Bites
Animal bites, particularly dog, cat or primate bites, may result in serious infection. These bites allow entry of Pasteurella multocida, Eikenella corrodens, Bacteroides species or other organisms into subcutaneous tissue, potentially resulting in rapidly spreading and destructive cellulitis. This complication can be prevented or forestalled with early irrigation and treatment with amoxicillin-clavulanic acid (Augmentin), although cefuroxime (Ceftin), doxycycline and other antibiotics are also useful. Tetanus precautions are essential, and rabies prophylaxis should be considered for wild-animal bites, especially those of raccoons, bats and skunks.
Vibrio Infection
Breaks in the skin caused by fish spines or other penetrating objects in brackish water may result in Vibrio infection. When a patient presents with a history of penetrating injury in brackish water, the wound should be irrigated, and treatment with tetracycline or another antibiotic effective against Vibrio organisms should be instituted.
Necrotizing Fasciitis
Traumatic or surgical wounds may, rarely, lead to necrotizing fasciitis, a significant and life-threatening illness. The infection most commonly develops in episiotomy sites or abdominal incision sites. Persons with diabetes or alcoholism may contract the illness without preceding trauma. Subcutaneous gas production occurs (so-called gas gangrene) when clostridial organisms are present, but multiple organisms are generally found in wound cultures. Tissue breakdown and muscle necrosis may occur rapidly, particularly if clostridial organisms are present. Surgical removal of devitalized tissue is required, as is high-dose parenteral antibiotic therapy.

