Establishing a diagnosis of osteomyelitis of the foot in patients with diabetes is often problematic because of the difficulty in determining whether the infection involves the bone or only the soft tissue. In addition, diabetes is a common cause of noninfectious bone disease, such as neuropathic osteoarthropathy, which can have the radiographic appearance of osteomyelitis. Lipsky reviewed the diagnostic and management approach to foot infections in patients with diabetes.
The first step in establishing the diagnosis is a careful clinical examination. Patients with soft tissue infection or skin ulceration over a bony prominence are at risk for osteomyelitis. The risk is significantly increased if the wound has been present for more than two weeks.
Several other clinical findings have been shown to be predictive of osteomyelitis. One study showed that an ulcer area of more than 2 cm2 has a sensitivity of 56 percent and a specificity of 92 percent for the diagnosis of osteomyelitis. If the depth of the ulcer is more than 3 mm, the likelihood of bony infection is much greater. A positive “probe-to-bone” test (making contact with bone when the ulcer is probed) has been reported to have a sensitivity of 66 percent, a specificity of 85 percent and a positive predictive value of 89 percent in the diagnosis of osteomyelitis.
One study showed that an erythrocyte sedimentation rate (ESR) greater than 70 mm per hour was present in 100 percent of patients with osteomyelitis. However, the same study showed that the ESR had a sensitivity of only 28 percent. The white blood cell count has not been found to be useful in diagnosing osteomyelitis.
The author notes that bony changes that are due to infection are not evident on plain films until 10 to 20 days after the onset of infection, when 40 to 70 percent of bone has been resorbed. Previous studies have shown that plain radiographs are about 60 percent sensitive and 66 percent specific for the diagnosis of osteomyelitis.
Bone scanning with technetium-99m can demonstrate abnormal uptake two weeks before changes are seen on plain films. The sensitivity of 99mTc bone scans in identifying osteomyelitis has been found to be about 86 percent, but the specificity has been noted to be poor, at only 45 percent. The explanation is that any preexisting osseous condition that causes bone turnover will result in a positive bone scan.
Indium-111–labeled leukocyte scanning is quite specific for infection, showing a 78 percent specificity in previous studies. Limitations of this study include leukocyte scanning's poor resolution in differentiating bony infection from adjacent soft tissue infection and the fact that it requires the withdrawal and reinfusion of blood.
Magnetic resonance imaging (MRI) provides excellent tissue contrast, making it an extremely sensitive test for osteomyelitis. A 99 percent sensitivity rate has been demonstrated in previous studies. However, false-positive results may occur in the presence of osteoarthropathy. Poor cortex resolution may result in false-negative results in patients with isolated cortical infection and no bone marrow involvement. Overall, several recent studies have shown MRI to be the best diagnostic imaging study for osteomyelitis. MRI has also been reported to be useful for monitoring the response to antimicrobial treatment. The primary limitation of MRI is cost.
The definitive diagnostic study for osteomyelitis is a bone biopsy. This procedure is reported to be 95 percent sensitive and 99 percent specific for identifying osteomyelitis. Bone specimens can be obtained percutaneously, but surgery may be necessary. The advantage of performing a bone biopsy is that it provides specific identification of the organism and its antimicrobial sensitivities. Disadvantages include cost (approximately $800) and patient discomfort.
The author refers to a recent decision and cost-effectiveness analysis of diabetic foot infections by other investigators which revealed that noninvasive testing adds significant expense to the evaluation of patients with diabetic foot ulcers but does little to change the patient's outcome. He notes that these investigators advocated surgical debridement followed by a 10-week course of antibiotic therapy based on the results of soft tissue culture. He disagrees with the conclusions of these investigators and advocates the thoughtful use of noninvasive diagnostic studies (see algorithm).
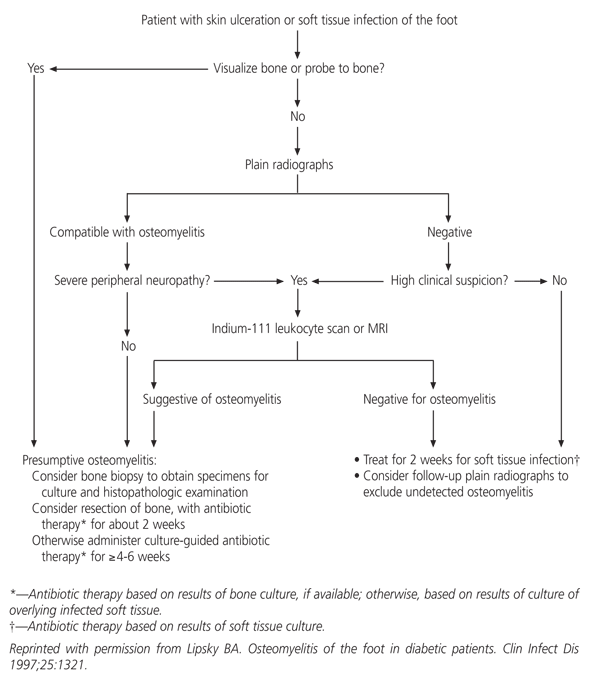
Suggested approach to the diagnostic evaluation and treatment of cutaneous ulceration or soft tissue infection of the foot in patients with diabetes. (MRI = magnetic resonance imaging)

