
Am Fam Physician. 1998;58(3):749-756
See related patient information handout on preventing heat illness, written by the authors of this article.
Heat-related illnesses cause 240 deaths annually. Although common in athletes, heat-related illnesses also affect the elderly, persons with predisposing medical conditions and those taking a variety of medications. Symptoms range from mild weakness, dizziness and fatigue in cases of heat edema, to syncope, exhaustion and multisystem complications, including coma and death, in cases of heat stroke. Milder heat-related symptoms can be treated with hydration, rest and removal from the hot environment. Heat stroke, a life-threatening problem, must be treated emergently. Prompt recognition is critical since rapid cooling is the cornerstone of treatment and must not be delayed. Fluid resuscitation with dextrose and normal or half-normal saline is also important. These therapies should be instituted while the patient is being stabilized. Heat illness may be prevented by recognizing which individuals are at risk, using appropriate hydration and paying attention to acclimatization and environmental conditions. Preventive care should include drinking plenty of fluids before, during and after activities, gradually increasing the time spent working in the heat and avoiding exertion during the hottest part of the day.
Although heat-related illnesses are treatable and preventable,1–3 at least 240 persons die of heat-related illnesses in the United States each year.1 In 1980, 1,700 persons died during a prolonged heat wave.1 Heat stroke is ranked third behind head and neck trauma and cardiac disorders as a cause of death among U.S. high school athletes.2 In 1995, five high school students died of heat-related illnesses.3 The mortality from heat-related illness is probably under-reported because deaths related to cardiovascular, cerebrovascular and respiratory disorders occur during heat waves.
Etiology, Risk Factors and Pathophysiology
Heat-related illnesses are more common in the summer but can also occur in moderate conditions, depending on environmental factors. Heat production is affected by multiple environmental factors including temperature, humidity, sun exposure, wind and clothing. The body's thermoregulatory system is responsible for allowing the body to heat and cool itself as necessary. This system can be overwhelmed during periods of heat stress if the sum of the environmental heat load and the metabolic heat load exceeds the body's capacity for heat dissipation.4
Dehydration of more than 3 percent of body weight is an important risk factor in heat-related illnesses.5 In addition, if lost fluids are not restored, the risk of heat-related illness is higher. These losses can be exacerbated by utilization of replacement fluids that are diuretic (i.e., beverages containing caffeine or alcohol). Thirst cannot be relied on as a measure of fluid loss, since athletes may not become thirsty until they are 5 percent dehydrated.6
| Physical conditions |
| Fever |
| Dehydration |
| Medications (see Table 2) |
| Prolonged exertion |
| Chronic illnesses |
| Cardiac conditions |
| Cystic fibrosis |
| Uncontrolled diabetes |
| Uncontrolled hypertension |
| Eating disorders |
| Malignant hyperthermia |
| Peripheral vascular disease |
| Extensive skin disease or damage, or both |
| Autonomic nervous system disorders |
| Psychiatric conditions |
| Hyperthyroidism |
| Older age |
| Decreased vasodilatory response |
| Decreased maximum heart rate, resulting in decreased maximum cardiac output |
| Decreased thirst response |
| Decreased fitness level |
| Decreased mobility resulting in increased difficulty of easily obtaining fluids |
| Increased body mass |
| More heat generated for same level of activity |
| Less efficient heat dissipation |
| Fewer heat-activated sweat glands in skin overlying adipose tissue |
| Decreased cardiac output per unit of body weight |
| Younger age |
| Decreased ability to sweat |
| Decreased cardiac output at a given metabolic rate |
| Greater core temperature required to initiate sweating |
| Slower acclimatization |
| More heat produced for the same level of activity |
| Additional factors |
| Lack of access to air conditioning |
| Residing in upper floors in tall buildings |
| Sleep deprivation (decreases skin blood flow and rate of sweating) |
| Previous heat stroke |
| Use of equipment or heavy clothing (football player's pads, firefighter's protective gear, etc.) |
| Recent move from a temperate to a hot climate |
| Urban setting |
| Alpha agonists |
| Amphetamines |
| Anticholinergic medications |
| Antihistamines |
| Anti-parkinsonian agents |
| Beta-adrenergic blockers |
| Calcium channel blockers |
| Cocaine |
| Diuretics |
| Ethanol |
| Heroin |
| Inhaled anesthetics |
| Laxatives |
| LSD |
| Monoamine oxidase inhibitors |
| PCP |
| Phenothiazines |
| Sympathomimetic medications |
| Thyroid agonists |
| Tricyclic antidepressants |
It is important to recognize that the collapse of an athlete during exercise does not necessarily indicate heat-related illness. While a heat-related illness must be considered in the differential diagnosis, a variety of other etiologies must also be considered.12
The heat load increases greatly during exercise. Twenty times more energy is produced at maximal activity, 75 percent of which is converted to heat rather than to work.9 Heat dissipation occurs by central and peripheral mechanisms, through radiation, conduction, convection and evaporation.
Increases in core temperature stimulate vasodilation and sweating. Vasodilation contributes to heat loss by convection. However, vasodilation may decrease blood pressure if cardiac output cannot increase enough to normalize blood pressure. Peripheral vascular resistance will increase, improving blood pressure but worsening attempts at heat loss. Sweating causes heat loss by evaporation.4 A small amount of the heat produced by muscle tissue is transferred passively by conduction to the tissue of the overlying skin. Some heat may be dissipated by convection via superficial veins en route to the heart.
Central mechanisms of heat dissipation, however, play a far more important role than peripheral means. Most heat is transported by blood from working muscles to the vena cava and then to the heart. Blood has a high heat capacity and can transport large amounts of heat with only a moderate increase in temperature. Heat is then dissipated by increased blood flow to the skin.6,9
Radiation and conduction dissipate most of the heat when ambient temperatures are less than 20°C (68°F). Evaporation becomes more important in ambient temperatures greater than 20°C (68°F). During strenuous exercise, 85 percent of heat loss occurs by evaporation. A 70-kg (154-lb) athlete will lose 1 to 2 L (2.1 to 4.2 pt) of sweat per hour during exercise. As ambient temperature and humidity increase, heat dissipation is less efficient. Elevated humidity decreases the evaporation of sweat. High ambient temperatures can cause heat gain through radiation.9
Types of Heat-Related Illness
Heat Edema
Heat edema, the mildest form of heat-related illness, occurs when swelling develops in dependent areas of unacclimatized persons during hot summer months. This disorder is caused by transient peripheral vasodilation from the heat and orthostatic pooling during prolonged sitting or standing. Heat edema may improve with periodic exercise or elevation of the legs.2
Heat Cramps
Heat cramps are painful spasms of skeletal muscles of the arms, legs or abdomen.3 Predisposing factors include lack of acclimatization, a negative sodium balance and use of diuretic medications. Heat cramps may be a warning sign of impending heat exhaustion.9 Treatment consists of oral or parenteral sodium replacement. Most athletes and adolescents will obtain enough sodium through natural cravings for salty foods (e.g., pretzels, chips). An oral rehydration solution can be made using one teaspoon of table salt per one quart of water.9
Heat Syncope
Heat syncope presents as an orthostatic syncopal episode or dizziness that usually occurs with prolonged standing or sudden rising from a sitting or lying position.3 Predisposing factors include exercise without a cool-down period, dehydration and lack of acclimatization.9 Heat syncope can result from inadequate cardiac output and postural hypotension.12 Recovery is immediate once the patient falls to the ground. Treatment consists of placing the patient in a supine position and replacing any water deficit. In severe cases, the patient's consciousness may be altered. Heat syncope can be avoided by having the patient sit or lie down when premonitory symptoms of lightheadedness and weakness are experienced.
Heat Exhaustion
Heat exhaustion occurs when a person experiences excess sweating in a hot humid environment, causing volume depletion. Core body temperature may rise above 38.0°C (100.4°F) but lower than 40.5°C (104.9°F). Symptoms include profuse sweating, malaise, headache, dizziness, anorexia, nausea, vomiting, vertigo, chills, muscle or general weakness, tachycardia and hypotension, visual disturbances and cutaneous flushing. Major neurologic impairment is absent.2,13,14
Symptomatic patients should be moved to a cool area to rest.2,9,13 Oral rehydration (approximately 1 L [2.1 pt] per hour for several hours) is preferred in patients who are coherent and without gastrointestinal symptoms. Elevation of the legs can reduce postural hypotension. Recovery should be rapid and the patient should feel better in two to three hours. If recovery is not progressing, the patient may need additional intervention such as more intensive cooling or intravenous rehydration.12,13 Dextrose in half-normal or normal saline is the most commonly used intravenous rehydration solution in patients with heat exhaustion.
Heat Stroke
Heat stroke is characterized by a core body temperature of at least 40.5°C (104.9°F) and acute mental status changes. Heat stroke occurs when heat production exceeds heat dissipation. The mortality rate in patients with heat stroke may be as high as 10 percent.1 The resultant hyperthermia causes damage to tissues in multiple organ systems.13 Endotoxins and cytokines may play a significant role in the progression and severity of hyperthermia.14 Predisposing factors include the risk factors for heat exhaustion as well as genetic predisposition. Heat stroke may be divided into two types, exertional and classic heat stroke2 (Table 35,8,15 ). The more severe and prolonged the episode, the worse the predicted outcome, especially when effective cooling measures are delayed. Heat stroke is a true medical emergency. The diagnosis is made when a markedly elevated temperature and changes in mental status follow heat exposure. The differential diagnosis includes hyperthyroid storm, pheochromocytoma, central nervous system injury, infection, anti-cholinergic poisoning, drug ingestion and neuroleptic malignant syndrome.
| Characteristic | Classic heat stroke | Exertional heat stroke |
|---|---|---|
| General health | Predisposing health factors | Healthy person |
| Age | Older | Younger |
| Occurrence | Often occurs during high temperatures | Occurs sporadically |
| Sweating | Absent | Present |
| Activity | Sedentary | Strenuous |
| Disseminated intravascular coagulation | Uncommon | Common |
| Acute renal failure | Uncommon | Common |
| Lactic acidosis | Uncommon | Common |
| Hyperuricemia | Moderate | Severe |
| Hypokalemia | Rare | Common |
| Rhabdomyolysis | Rare | Common |
Evaluation of Heat Stroke
History
It is important to obtain a history of the symptoms and the preceding circumstances.6 A description of the neurologic changes may be obtained from family, friends or bystanders. Premonitory symptoms such as weakness and dizziness often may go unrecognized,16 and patients frequently present acutely with collapse.3 It is critical to review the patient's medical history, medication history and history of illicit drug use, as well as treatment administered before and during initial medical intervention.
Physical Examination
Patients may be tachycardic, tachypneic, hypotensive or normotensive at initial evaluation.6 Core body temperature should be obtained with a rectal, esophageal or bladder probe.2 Tympanic, oral or axillary temperatures are not accurate for the measurement of core temperature. Temperature may be lower if cooling has been started en route to the emergency department.5 The thermometer used must be able to register above 41.0°C (105.8°F).
The skin may be hot and dry, especially in cases of classic heat stroke. The neurologic examination may reveal irritability, confusion and ataxia. Seizures may or may not be present initially but may occur during cooling. Coma may be the most common presentation, and decorticate posturing may be present. Severe volume depletion and peripheral vasoconstriction will be present. Hypotension decreases perfusion as heat stroke progresses. The onset of coagulopathy, which may progress to disseminated intravascular coagulation (DIC), may be signaled by ecchymosis, hematemesis, hematuria and epistaxis. The laboratory work-up is summarized in Table 4.2,6,16
| Test | Findings related to heat stroke |
|---|---|
| Chest x-ray | Pulmonary edema, pulmonary congestion, adult respiratory distress syndrome |
| EKG | Conduction abnormalities, nonspecific ST-T wave changes, arrhythmias, myocardial infarction |
| ABG | Respiratory alkalosis, oxygenation status |
| Cardiac isoenzymes | Myocardial injury |
| CBC | Leukocytosis, elevated hematocrit |
| Fibrinogin, fibrin split products | Coagulopathy, disseminated intravascular coagulation |
| LDH, AST, ALT, CK, potassium, BUN | Elevated in renal or hepatic injury |
| Lactate | Commonly elevated in exertional heat stroke, predicts poor prognosis in classic heat stroke |
| Calcium, phosphorus, glucose | Decreased |
| Urinalysis | Myoglobin casts, red blood cells |
Treatment Considerations in Heat Stroke
External Cooling
Rapid cooling to bring the patient's core temperature to 38.8°C (101.8°F) is a critical factor in improving prognosis. There is controversy regarding which cooling techniques are most effective. Evaporative and immersion methods of cooling, or a combination of these methods, have been demonstrated to be useful.2,6,13,17,18
Evaporative methods require removal of restrictive or unnecessary clothing, spraying the patient with water or wrapping the patient in wet towels or sheets, and increasing air flow over the patient. This method can be readily available in the field and does not interfere with other aspects of resuscitation. Vasoconstriction and shivering are less frequently associated with evaporative methods than with immersion methods.2,6,17
Immersion methods are effective but may be difficult to arrange and may delay cooling. They involve the use of ice baths, a cooling blanket, ice packs to the axillae, groin and neck, and cool or cold water immersion. The resultant hypothermic vasoconstriction of cutaneous blood vessels may increase blood pressure in hypotensive patients. It can, however, diminish peripheral circulation and retard heat loss. Shivering can also occur, generating body heat and impeding cooling efforts. Diazepam (Valium) and neuroleptic agents such as chlorpromazine (Thorazine) can inhibit shivering.2,6,18 Immersion limits access to the patient for resuscitation in the event of cardiac arrest and precludes the use of electrocardiographic (EKG) monitoring, causes vagal stimulation and may cause bradycardia.2
Internal Cooling
Internal methods for cooling patients may be used for treatment of hyperthermia when external methods have not been effective. Cold water irrigation to the stomach or rectum, peritoneal lavage and cardiopulmonary bypass should only be used in addition to external cooling methods.2
Other Management Considerations
Respiratory and cardiac status must be evaluated and closely monitored. Oxygen supplementation and intubation should be provided if respiratory assistance is indicated. Intravenous access should be obtained for the administration of fluids (usually dextrose plus normal or half-normal saline) and medication. A fluid challenge should be provided if the patient is hypotensive. Urine output should be monitored.2,6
Complications and Prognosis of Heat Stroke
| Central nervous system | |
| Cerebral edema | |
| Seizures | |
| Coma | |
| Liver injury | |
| Renal failure | |
| Cardiac disorders | |
| Arrhythmias | |
| Congestive heart failure | |
| Hypotension | |
| Pulmonary disorders | |
| Pulmonary edema | |
| Adult respiratory distress syndrome | |
| Coagulopathy | |
| Disseminated intravascular coagulation (a common cause of death) | |
Hepatic damage is very common and is thought to be related to DIC. Renal failure can occur and is due to severe rhabdomyolysis. Serum and urine myoglobin levels may be normal initially; therefore, it is important to follow these levels serially. Renal failure is a result of deposits of myoglobin within the renal tubules.19
| Delay in cooling |
| Coma that lasts longer than two hours |
| Elevation in CK, LDH, ALP levels |
| Elevation in AST level, especially if >1,000 U per L (16.67 μkat per L) in first 24 hours |
| Hypotension |
| Prolongation of prothrombin time |
Prevention of Heat-Related Illness
Prevention remains the cornerstone of therapy.21 As the number of people participating in athletic activities increases and as the intensity and duration of events increase, an increase in heat-related illnesses may be expected.11 Environmental conditions contribute to heat injury, but an awareness of other predisposing factors can assist in decreasing the number of adverse events. This would include observance of atmospheric conditions, use of proper clothing, timing of workouts and attention to the hydration status of the participants. Persons who may be at risk should be identified in order to prevent heat-related illness (Tables 1 and 2).
Environment
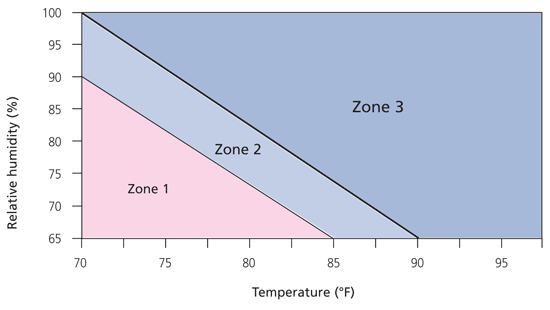
The vast majority of heat-related problems are a direct result of the environmental conditions in which the athlete has been exercising. Accurate assessment of these conditions coupled with a working knowledge of heat stress charts may be extremely beneficial in evaluating the risk of heat injury as a result of environmental conditions. Wet bulb globe temperatures are helpful, and information on obtaining such temperatures is often found in sports medicine texts.9 The actual risk of heat injury related to environmental conditions can be predicted using the heat stress danger chart in Figure 1.
Acclimatization
The process of becoming accustomed to exercise in the heat is known as acclimatization. Essentially, the body learns to work more efficiently in hot weather with less generation of its own internal heat. This acclimatization process is an essential part of preventing heat-related illnesses.11
Repeated episodes of exercise in the heat facilitate the acclimatization process.13 Adults require four to seven sessions of one to four hours each in the heat. Children require slightly longer.9,10 Such acclimatization is best done during the heat of the day and is facilitated by continual replacement of wet clothing with dry garments.
This improvement in the body's efficiency is accomplished by the training effect (improved level of physical condition, which allows for increased exercise capacity in the heat, improved heat dissipation and changes in metabolism). The more efficient heat dissipation mechanism is largely due to an increase in sweat production for a given increase in core temperature. This process will occur more rapidly in a conditioned athlete.10
Hydration
Adequate fluid status is important for the prevention of heat illness. Fluids must be consumed before the urge for them rises, since a substantial amount of dehydration can occur before stimulation of the thirst mechanism occurs. Pre- and post-heat exposure weights should be checked, and for each pound of weight lost, the athlete should consume 448 g (16 oz) of fluid.
In an effort to obtain and maintain an adequate fluid balance, prehydration is important and must be continuously emphasized. Prehydration provides a fluid “cushion” and delays the onset of dehydration. Dehydration is generally not a problem in exertion lasting less than 20 to 60 minutes.
Proper hydration involves ingestion of up to 448 g (16 oz) of fluid before the exercise. The athlete should then continue to drink 224 g (8 oz) of fluid every 20 minutes during the activity, with a goal of not experiencing thirst during training and voiding light yellow urine at least four times daily. The fluid can be something as simple as water or may be a flavored drink. Flavored drinks can contain sugar, which should not be very high in concentration. Examples of acceptable, widely available products include Gatorade Frost Thirst Quencher (14 g of sugar per 240 mL [about 8 oz]) and Allsport Body Quencher (19 g of sugar per 240 mL [about 8 oz]). By way of comparison, a standard 240-mL (8-oz) serving of soda contains 26 to 31 g of sugar.