to the editor: Bedrails are widely used in the care of patients staying in hospitals and nursing homes. It is not known whether bedrails decrease the patient's risk of falling or whether they increase the patient's chance of injury from falling over or through them.1 It is known that entrapment in bedrails can lead to death, but such deaths have been difficult to study. Sketches of lethal bedrail entrapments have been based on brief written reports.
We are not aware of published photographs that could help physicians, bed manufacturers and policymakers understand how these deaths occur or how to prevent them. Decedents are often moved before their deaths can be photographed. We report here two cases of death by bedrail entrapment. In the first case, a video camera mounted on the ceiling with a digital clock inset inadvertently taped the death of the patient. In the second case, the death was documented by a coroner's photograph. Line drawings accompanying these case reports depict the scenario of these deaths, based on the videotape and the coroner's photograph.
In Case 1, an obtunded patient with a traumatic head injury died of asphyxiation. Videotape frames show two phases of movement: the patient leaving the bed and the patient becoming entrapped in the bedrail. Figure 1a shows the patient's left leg moving off the bed and into the space between the upper and lower bedrails. Figure 1b shows the patient's torso sliding into the slot between the upper and lower bedrails. The tape shows that once the patient's legs were in the slot, the raised head of the bed allowed the patient to slide into the slot. After the patient's pelvis moved off the bed, his weight pulled him into the space between the upper bedrail and the mattress frame.
FIGURE 1A.

The patient's leg is moving off the bed into the space between the upper and lower bedrails.
FIGURE 1B.

The patient is sliding into the space between the upper and lower bedrails.
Figure 1c shows the final position of the patient, in which the patient is suspended with his thorax lodged and compressed in a 6-inch gap between the upper bedrail and the mattress frame. Ten minutes elapsed between the time that the nurse last centered the patient on the bed and the time that the patient became positioned as shown in Figure 1a. Two more minutes passed from the time the patient was in the position in Figure 1a to the time that he was in the position shown in Figure 1c. The patient was found asphyxiated 14 minutes after reaching the position in Figure 1c, and resuscitation efforts failed.
FIGURE 1C.
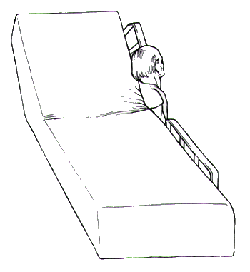
The patient is suspended with the thorax lodged and compressed in a 6-inch gap between the upper bedrail and the mattress frame.
Case 2 involved a confused, agitated, small elderly person who died afer sliding between the mattress and the bedrail. Figure 2 shows the patient's torso compressed in the space between the bedrail and the mattress, with the buttocks hanging above the floor. With the mattress pressed against the opposite bedrail, the space was only 4 inches wide.
FIGURE 2.
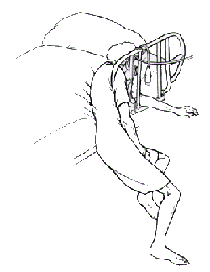
The patient is found asphyxiated. Her torso is compressed between the bedrail and the mattress.
The patient in Case 2 had fallen from her bed on several previous occasions. On two occasions shortly before her death, the patient was found trapped by the bedrail. The patient had been monitored with a string-type position alarm that sounds when a patient moves out of position and pulls a cord out of an alarm box. The alarm did not sound during her death because the string was not pulled out of the alarm box. The alarm failed during a previous bedrail entrapment when the alarm box was pulled from the headboard and dragged across the mattress. The patient did not use the nurse call signal (seen hanging over the bedrail) before this or previous falls.
These cases illuminate how bedrail deaths occur. The U.S. Food and Drug Administration, along with studies of bedrail and restraint deaths, emphasizes that confused, agitated people who behave impulsively are at an especially high risk of entrapment.2–4 The patient in Case 1 was semiconscious; the patient in Case 2 was confused. Both were impulsive and actively mobile. Both had experienced “rehearsal incidents” with nonlethal bedrail entrapments shortly before their deaths. These are very common occurrences before deaths that are related to physical restraints3 and should prompt swift, fundamental modification of the bed environment for the patient's safety.
These events show that the ability to prevent such deaths, given the present design of beds, is limited. Restraints may cause asphyxiation by themselves and do not prevent lethal entrapment in bedrails.3–5 Lethal entrapment can occur with a single half-bedrail, split bedrails or a full-length rail. The string alarm in Case 2 did not alert medical staff to the entrapment. It is very difficult to gauge the safety of bed proportions. The space between the bedrails and the bed frame in these cases was 6 and 4 inches. Regular monitoring will not prevent these deaths as evidenced by the rapidity of events in Case 2. Neither bed had a weight-position sensor; perhaps rapid response to such alarms may prevent some deaths.
Overall, prevention of these types of deaths will require much more judicious use of bedrails, swift and effective changes for patients at high risk of entrapment, and fundamental changes in the design of the bed environment.

