Cardiac rehabilitation is an important management strategy in patients with coronary artery disease. Substantial data from both mortality and morbidity studies support the benefits. Recent studies of patients with coronary artery disease have shown that exercise confers greater benefit in those who are also on a fat-controlled diet than in those who are not. In addition, high-intensity exercise has been found to improve left ventricular function in men with coronary artery disease. Individual home exercise programs, both with and without telephone monitoring, are prescribed by physicians and health care professionals for an increasing number of patients. Aggressive modification of coronary risk factors is also incorporated in the overall cardiac rehabilitation program, and the concept of greater total kilocalorie expenditure per week is emphasized.
Cardiac rehabilitation has become an important aspect of management in patients with coronary artery disease, especially after a myocardial infarction, coronary artery bypass surgery or coronary angioplasty. Cardiac rehabilitation is also useful in patients with valvular heart disease and controlled congestive heart failure, as well as in those with certain other cardiovascular diseases.1 In addition, recent data support the benefit of treadmill exercise training in patients with peripheral arterial disease.2,3 Some of the current issues and trends in cardiac rehabilitation are listed in Table 1.
TABLE 1 Current Trends in Cardiac Rehabilitation
| Aggressive coronary risk modification for secondary prevention |
| Primary prevention in families of those with atherosclerotic vascular disease |
| Home telephone electrocardiogram-monitored cardiac rehabilitation exercise |
| Home individualized nonmonitored cardiac rehabilitation exercise |
| Behavior modification and compliance intervention |
| New CPT codes to document rehabilitation activities |
| A greater role in managed and capitated care |
CPT = common procedural terminology.
The benefits of cardiac rehabilitation have been demonstrated in both population studies and mortality and morbidity studies.1 A recent meta-analysis4 concluded that overall mortality, cardiovascular mortality and rates of sudden death were significantly decreased in patients who were active in cardiac rehabilitation with exercise, as compared with control subjects. However, no difference was found in the incidence of subsequent myocardial infarction.
Exercise Strategies
Recent studies in Europe have shown that high-intensity exercise confers greater benefit in patients with coronary artery disease who are also on a fat-controlled diet than in those who are not.5,6 These controlled studies demonstrated regression or lack of progression of coronary lesions in patients who performed high-intensity exercise and were also on a low-fat diet. The changes were maintained during the follow-up period of six years.7 Changes were documented by coronary arteriography both before and after the intervention. The Training Level Comparison Study8 showed that high-intensity (versus low-intensity) exercise results in a higher left ventricular ejection fraction in men with coronary artery disease. These studies have not yet been analyzed with regard to changes in survival.
Other investigators have also reported that exercise training programs have either no harmful effects or possibly beneficial effects on ventricular function and/or “remodeling” in subjects with coronary heart disease.9–12 Therefore, higher intensity exercise may be not only appropriate but also beneficial in patients with either depressed or normal left ventricular function.
Home Programs
Strategies for cardiac rehabilitation have changed over recent years. Currently, less emphasis is being placed on office or hospital visits for electrocardiographic (ECG) monitoring and supervised group programs. Many patients are unable to participate in such programs because of travel considerations, expense or inconvenience. Consequently, more patients are being managed individually through home programs. These programs involve aggressive coronary risk modification with specific emphasis on smoking cessation, lipid control, blood pressure control and physical activity.
Monitored Programs
Home telephone ECG-monitored programs have been evaluated in several studies.13,14 Such monitoring is done by means of a telephone ECG transmitter, in concert with voice transmission, through a standard telephone system. These voice and ECG signals are transmitted, locally or long-distance, to a central monitoring station for interpretation. During these sessions, voice communication may be useful for sharing information, obtaining exercise advice or discussing safety concerns. The ECG signal is used to document heart rate and rhythm. A recent unpublished study compared home-monitored exercise with standard hospital-based programs. The home program was found to be safe and effective in providing rehabilitative exercise.
Unmonitored Programs
Home exercise programs without telephone monitoring are also being used by cardiologists and primary care physicians for patients who have been evaluated with an exercise test. Such individual programs should, however, include periodic face-to-face physician counseling. Patients assigned to these programs are predominantly those at low risk according to American Heart Association (AHA) criteria (Table 2)15 who show no evidence of left ventricular dysfunction, high-grade arrhythmias, unstable angina pectoris or other medical problems that could be of concern in home exercise.
An initial exercise test is important for these patients, and some physicians periodically repeat the test to ensure the safety and efficacy of the program, as well as to confirm that the assigned level of exercise training is appropriate.
TABLE 2 American Heart Association Low-Risk Criteria for Exercise
| New York Heart Association class 1 or 2 |
| Exercise capacity over 6 METs (≥ 21 mL per kg per minute oxygen consumed) |
| No evidence of heart failure |
| Free of angina or ischemia at rest or with exercise |
| Appropriate increase in blood pressure with exercise |
| No sequential ectopic ventricular ectopy (three or more beats in a row) |
| Ability to satisfactorily self-monitor exercise intensity |
MET = metabolic equivalent.
Information from Fletcher GF, Balady G, Froelicher VF, Hartley LH, Haskell WL, Pollock ML. Exercise standards. A statement for healthcare professionals from the American Heart Association Writing Group. Circulation 1995;91:580–615.
Risk Factor Management
Aggressive coronary risk factor modification is now incorporated in the overall cardiac rehabilitation program more frequently than it was in the past. This comprehensive risk modification specifically focuses on smoking cessation, blood lipid management, blood pressure control and weight management. It also includes the use of antiplatelet agents (aspirin), angiotensin converting enzyme (ACE) inhibitors, beta blockers and estrogens. The AHA has provided guidelines for risk modification,16 and the data substantially support the benefits of aggressive risk intervention in patients with many types of vascular disease, including coronary and carotid artery disease, abdominal aortic disease and peripheral arterial disease.
Other risk markers are currently under investigation.17,18 These include elevated levels of insulin, fibrinogen, homocysteine, lipoprotein(a) and lipoprotein receptors. Elevated homocysteine levels, especially in patients with known coronary artery disease, have recently been reported to be strongly predictive of mortality.19 Clinicians should consider measuring plasma homocysteine levels in patients with vascular disease who have a normal lipid profile. Elevated homocysteine levels can be effectively lowered with the use of oral folate supplementation.20
Implementation of Exercise
More recently, the concept of greater total kilocalorie expenditure per week has been evaluated.21 Increased caloric expenditure can be accomplished not only by performing high-intensity exercise but also by exercising more frequently and for longer periods. The number of kilocalories expended per week should be considered in the end result. Clinical studies suggest that the expenditure of a total of 2,200 to 3,500 calories during one week is optimal.21–23 This goal can be achieved with moderate to vigorous exercise, but it can also be accomplished by engaging in leisure activities that involve lower levels of exercise. Figure 1 illustrates ways to vary the intensity, duration and frequency of activity and still attain an exercise training goal.
FIGURE 1.
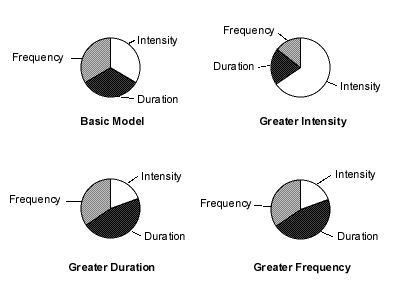
Exercise training protocols. The circles illustrate variations in intensity, duration and frequency of exercise. The circle at the upper left displays the basic model, with equal frequency, intensity and duration of exercise. The upper right circle displays a protocol of greater intensity, with shorter duration and less frequency of exercise; the lower left circle shows a protocol with greater duration and less frequency and intensity; and the lower right circle shows a protocol with greater frequency, shorter duration and less intensity.
Some data21 suggest that more vigorous exercise is beneficial, but it should be done carefully, particularly by those who are at moderate to high risk. Walking at the rate of 15 to 16 minutes per mile is a vigorous level of exercise for most persons, especially those with cardiovascular disease. When engaging in vigorous exercise, elderly patients in particular must be careful to avoid musculoskeletal injury. Precautions include performing proper warm-up and cool down, and limiting the exercise to low-impact activity. Guidelines for the specifics of writing an exercise prescription are listed in Table 3.
TABLE 3 Basic Principles of Writing an Exercise Prescription
| Obtain maximum heart rate from exercise test. |
| Designate a target heart rate at 60 to 80 percent of the maximum rate achieved with testing. |
| Begin at low level (60 to 70 percent) and progress over four to six weeks to 75 to 80 percent level. |
| Prescription should be employed for 30 to 60 minutes, four to six times weekly. |
| Sessions of exercise should incorporate aerobic activity such as walking/jogging, stationary cycling or water aerobics. Sessions should also incorporate warm-up and cool-down periods. |
| In addition to aerobic activity, resistance exercises (using light weights) may be added on an individual basis. |
Future Challenges
Because of the need for a long-term commitment to cardiac rehabilitation, behavior modification and compliance continue to be major concerns.1 A strategy for maintaining compliance has yet to be developed. Newer technology to address these concerns includes devices with “interactive audio” (voice synthesizer) to remind patients when it is time to exercise and to specify the number of calories to be expended in an exercise session. It is hoped that this and other types of technologic advances will make patients more compliant when they are away from the influence of health care professionals.
The future of cardiac rehabilitation will include greater emphasis on primary prevention measures in the families of patients with established cardiovascular disease.24 This effort will involve implementing many of the priorities of the AHA, such as controlling atherosclerotic risk factors in family members and providing incentives for increased physical activity from early childhood on. Such measures as encouraging dietary modifications for families may lead to healthier food choices for children at school as well as at home.

