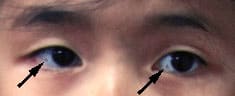
An 11-year-old girl of average build presented to the office with a history of grayish discolorations in both eyes (see the accompanying photograph). Her parents said that the pigmentation had been present since birth. On physical examination, a grayish pigmentation was noted in the lateral aspect of the right eye and the medial aspect of the left eye, but the patient had no diminution of vision. The physical examination was normal in other respects.
Question
Which one of the following is the correct diagnosis, given the patient's history and the physical appearance of the eyes?
A. Scleral melanocytosis.
B. Nevus of Ota.
C. Nevus of Ito.
D. Mongolian spot.
E. Blue nevus.
Discussion
The answer is A: scleral melanocytosis. Scleral melanocytosis is a congenital melanocytic hyperpigmentation of the sclera that is more commonly seen in the Asian population. Scleral melanocytosis often presents as bilateral spots of black or gray-blue pigmentation in the sclerae; the conjunctivae can be moved over the pigmented spots. Histologically, bipolar or multipolar dendritic melanocytes are found in the sclera and episclera, rather than in the conjunctival substantia propria.1
Nevus of Ota (oculodermal melanocytosis) is characterized by benign melanosis involving the skin of the face about the eye, which is supplied by ophthalmic and maxillary divisions of the trigeminal nerve.2 The color of the affected skin varies from light brown to dark brown, blue-black or slate. The skin pigmentation is usually unilateral. Ocular melanosis is a common finding in patients with nevus of Ota, especially in moderate or severe cases; ocular involvement ranges from a black or gray-blue discoloration of the sclera alone in two thirds of cases to hyperpigmentation of the entire uveal tract, conjunctiva and optic nerve. Nevus of Ota is most commonly found among the Japanese and other people of Asian descent. It is much less common among blacks and is least common among whites. An incidence of 0.4 to 0.8 percent has been noted among the Japanese; 80 percent of affected persons are female.3 Approximately one half of the lesions are noted at birth, while most appear by the second decade of life.
Nevus of Ito is a variant of nevus of Ota. However, in patients with nevus of Ito, the skin pigmentation occurs in the acromioclavicular region and is more diffuse and less mottled.
A Mongolian spot is a congenital hyperpigmented spot of varying size and shape that is usually grayish in color. It is caused by the abnormal occurrence of melanocytes in the lower half of the dermis of human skin. It is found most frequently in the sacrococcygeal region and usually regresses and disappears during childhood. The spot is found in almost all newborn Chinese, Japanese and Mongolian children, as well as some white and black children.
A blue nevus is characterized by a small, smooth, dome-shaped, hairless, firm, blue papule or nodule. The lesion may be present at birth or may develop during childhood. Histologically these nevi are composed of intensely pigmented, spindle-shaped melanocytes and are found in the dermis and around appendicular structures.

