Nonretentive encopresis refers to inappropriate soiling without evidence of fecal constipation and retention. This form of encopresis accounts for up to 20 percent of all cases. Characteristics include soiling accompanied by daily bowel movements that are normal in size and consistency. An organic cause for nonretentive encopresis is rarely identified. The medical assessment is usually normal, and signs of constipation are noticeably absent. A full developmental and behavioral assessment should be made to establish that the child is ready for intervention to correct encopresis and to identify any barriers to success, particularly disruptive behavior problems. Successful interventions depend on the presence of soft, comfortable bowel movements and addressing toilet refusal behavior. Daily scheduled positive toilet sits are recommended. Incentives may be used to reinforce successful defecation during these sits. A plan for management of stool withholding should be agreed on by the parents/caretakers and the family physician before intervention.
Encopresis affects 1 to 3 percent of children, with higher rates in boys than in girls.1,2 However, encopresis may go undetected unless health professionals directly inquire about toileting habits.3
From 80 to 95 percent of encopresis cases involve fecal constipation and retention.4 Although several excellent reviews cover retentive encopresis,5–7 encopresis in which fecal retention is not a primary etiologic component is under-represented in the literature. Typically, children with the latter condition soil on a daily basis, with bowel movements of normal size and consistency. Various terms have been used to describe this problem, including functional encopresis, primary nonretentive encopresis and stool toileting refusal. These children may be further divided into at least four subgroups: (1) those who fail to obtain initial bowel training, (2) those who exhibit toilet “phobia,” (3) those who use soiling to “manipulate” their environment and (4) those who have irritable bowel syndrome. Although the toileting dynamics and behavioral characteristics of children with nonretentive encopresis are well described,8–10 few specific treatment guidelines are available for family physicians.
While the treatment of retentive encopresis has progressed substantially in the past 20 years, less attention has been paid to the 5 to 20 percent of cases in which constipation is not contributory, or where a child “refuses” the toilet-training process. The family physician is likely to be the first to identify this problem and to provide “front line” intervention. Occasionally, a child presents who is not physically, cognitively or emotionally prepared for toilet training. In these cases, waiting until the child matures is the sensible choice. However, many times the reason is not a lack of readiness skills, but a child who is behaviorally resistant or parents who need information on effective behavior management or toilet-training strategies.11
Once the reason for a child's resistance is identified, specific interventions can be initiated. If the problem is related to a skill deficit (e.g., opening the bathroom door, disrobing, seating self on the toilet, wiping), then modeling, teaching and reinforcement are preferred to passive waiting. In similar fashion, if the child is oppositional or noncompliant with adult instructions, the physician may choose to refer the family to a pediatric psychologist who is familiar with compliance training protocols. In either case, without active intervention, the “strong-willed” child may resist toilet training, create unnecessary stress on the parent-child relationship and increase the risk of abuse.12
This article provides treatment guidelines for children with primary nonretentive encopresis or stool toileting refusal. The guidelines were developed from the literature on toilet training and encopresis, with a special emphasis on practicality and ease of implementation by the family physician. The illustrative case presented on page 2176 shows the efficacy and simplicity of these treatment guidelines.
Guideline 1: Identify Potential Medical, Developmental or Behavioral Pathology
MEDICAL
First, a complete physical examination is indicated when a child presents with a history of soiling. The history and physical examination may be the only diagnostic tools necessary to identify retentive encopresis and related organic factors. Few cases of retentive encopresis and even fewer cases of nonretentive encopresis have an organic etiology.13,14 Table 1 summarizes pertinent aspects of the history and physical examination. The principal differential diagnoses of encopresis are listed in Table 2.13–15
TABLE 1 History and Physical Examination in Children with Toileting Refusal and Soiling
| History | |
| Stool pattern | |
| Size | |
| Consistency | |
| Interval | |
| History of constipation | |
| Age of onset | |
| History of soiling | |
| Age of onset | |
| Type and amount of material | |
| Diet history | |
| Type and amount of food | |
| Changes in diet | |
| Decrease in appetite | |
| Abdominal pain | |
| Medications | |
| Urinary symptoms | |
| Day or night enuresis | |
| Urinary tract infection | |
| Family history of constipation | |
| Family or personal stressors | |
| Physical examination | |
| Height | |
| Weight | |
| Abdominal examination | |
| Distention | |
| Mass, especially suprapubic | |
| Rectal examination | |
| Sacral dimple | |
| Position of anus | |
| Anal fissures | |
| Anal wink | |
| Sphincter tone | |
| Rectal vault size | |
| Presence or absence of stool in rectum | |
| Pelvic mass | |
| Neurologic examination | |
TABLE 2 Differential Diagnosis of Encopresis
| Retentive | |
| Functional constipation (95 percent) | |
| Organic (5 percent) | |
| Anal causes | |
| Fissures | |
| Stenosis/atresia with fistula | |
| Anterior displacement of anus | |
| Trauma | |
| Postsurgical repair | |
| Neurogenic causes | |
| Hirschsprung's disease | |
| Chronic intestinal psuedo-obstruction | |
| Spinal cord disorders | |
| Cerebral palsy/hypotonia | |
| Pelvic mass | |
| Neuromuscular disease | |
| Endocrine/metabolic causes | |
| Hypothyroidism | |
| Hypercalcemia | |
| Lead intoxication | |
| Drugs | |
| Codeine | |
| Antacids | |
| Others | |
| Nonretentive | |
| Nonorganic (99 percent) | |
| Organic (1 percent) | |
| Severe ulcerative colitis | |
| Acquired spinal cord disease (i.e., sacral lipoma, spinal cord tumor) | |
| Rectoperineal fistula with imperforate anus | |
| Postsurgical damage to anal sphincter | |
Children with retentive encopresis often soil small quantities of loose fecal matter several times a day but periodically pass very large bowel movements. They may present with urinary complaints and abdominal pain or distention. The physical examination is usually suggestive of constipation.
A consistent soiling pattern characterized by stools that are normal in size and consistency and the absence of constipation usually suggests nonretentive encopresis. If the physician is unable to confirm the presence of constipation or impaction following the history and physical examination, a flat plate radiograph of the abdomen will aid in diagnosis. Further diagnostic investigation using laboratory tests, barium enemas, rectal manometry or biopsy is reserved for use in children who fail conservative therapy or whose history and physical examination suggest an organic etiology. Finally, Hirschsprung's disease is frequently mentioned in the differential diagnosis of encopresis; however, children with Hirschsprung's disease do not typically pass large bowel movements and rarely soil.13
DEVELOPMENTAL
Unrealistic expectations or family priorities (particularly the birth of another child) may prompt parents to begin toilet training before the child is developmentally prepared.16 Physicians can use the 15- or 18-month well baby visit to inquire about plans for toilet training and to ensure that both the child and the family are ready for the process. Initiating training when parents are under time constraints or during periods of family adaptation and stress will be difficult.
Child readiness is determined by the presence of the prerequisite physiologic, developmental and cognitive/psychologic skills to master the complexities of independent toileting. Physiologic readiness is demonstrated by sphincter control, which is usually present by the time the child crawls or walks,17 and by bladder and bowel readiness, shown by the ability to remain dry for several hours at a time and to fully empty the bladder on voiding.
Some children make facial expressions, assume certain body postures (e.g., squatting) or go to a specific location to urinate or defecate. Developmental criteria include attainment of major motor skills such as being able to walk to the bathroom, sit on the toilet, lower and raise pants and flush the toilet. Cognitive/psychologic readiness criteria involve both receptive language adequate to understand toileting-related words such as “wet,” “dry,” “pants” and “bathroom,” and instructional readiness, as indicated by a child who desires to imitate and please parents and to follow simple instructions. Most children meet the above criteria and are ready to be toilet trained between 24 and 30 months of age.16,18
BEHAVIORAL
The most important areas of behavioral assessment of toileting include ruling out the presence of disruptive behavior problems such as aggression, oppositional behavior, noncompliance and temper tantrums, establishing the child's compliance with adult instructions and obtaining a daily diary of toileting habits.
Coexisting behavior problems are a predictor of poor outcome in toilet-training protocols.19 Disruptive behavior and childhood noncompliance across multiple settings (e.g., dressing, bath time, bedtime) require direct attention before toilet training is attempted. It is critical that the child be cooperative and compliant with adult instructions; the child should be able to consistently follow at least seven of 10 parental instructions in a timely manner.
Rather than relying on a parental report, the physician can simply observe the child during an office visit to see if the child complies with parental instructions. Although protocols are available for helping parents decrease a child's oppositional behavior and increase compliance with instructions,20,21 many physicians choose to refer the child to a behavioral psychologist with experience in this area.
Finally, an important component of the behavioral assessment is pretreatment information on daily toileting patterns. A daily toileting diary provides a wealth of information that can be incorporated into the treatment plan (see accompanying patient information handout). For example, the diary may help identify times to schedule toilet sits. Continued use of the diary may provide clues regarding treatment compliance and the effectiveness of the intervention.
Guideline 2: Address Toilet Refusal Behavior
Many children with fecal soiling have a history of painful defecation, toilet “phobia” or toilet refusal behavior.22 Positive toilet sits are one strategy to help children overcome negative associations regarding the bathroom. The goal of positive toilet sits is to associate the bathroom and the toilet with enjoyable activities and parent-child interactions. Initially, sits can be scheduled three to five times daily at the family's convenience. The strategy starts with very short sits (e.g., 30 seconds) that gradually increase to a maximum of five minutes each, using a portable timer to signal completion. The child can remain in underpants or diapers because there is no expectation of producing a bowel movement. While the child is sitting on the toilet, proper foot support, access to enjoyable (relaxing and noncompetitive) activities and individual parental attention should be ensured.
If a child is extremely resistant to approaching the toilet or potty chair, the parent may employ a gradual shaping procedure. For example, a parent begins by modeling appropriate toileting behavior for a few weeks; after this, the parent starts playing games or reading books with the child in or near the bathroom. The parent and child gradually progress to engaging in these activities while the child is sitting on the potty chair for longer periods of time. During the modeling process, we recommend that fathers and male caretakers sit during urination. Boys should be encouraged to sit while urinating until they are fully bowel trained.
Guideline 3: Ensure Soft, Well-Formed Stools
It is critical to ensure that the child is having relatively frequent, soft and well-formed bowel movements before engaging in any intervention for soiling. Dietary changes or short-term use of supplements such as flavored fiber drinks or bran sprinkles may be needed to increase the number of bowel movements and to maximize daily toileting opportunities.
If obtaining frequent, soft and well-formed bowel movements continues to be a problem, the addition of stool softeners or laxatives may be considered. Suitable daily regimens include Milk of Magnesia, in a dosage of 1 to 3 mL per kg per day; mineral oil, in a dosage of 1 to 5 mL per kg per day; or sorbitol, in a dosage of 1 to 3 mL per kg per day. These agents can be given in one or two doses per day. Mineral oil is not indicated in children who are at risk for aspiration.13–15
Any of these supplements may make it more difficult for the child to withhold bowel movements, resulting in more soiling accidents. Consequently, it is a good idea for parents to develop a standard clean-up procedure that can be carried out in a matter-of-fact, emotionally neutral manner. The appropriate reaction is for parents to use a neutral tone of voice while directing the child through developmentally appropriate clean-up activities. Parents should avoid blaming, criticizing or name-calling during this time.
Guideline 4: Schedule Prompted Toilet Sits
When the child is no longer resistant to sitting on the toilet and is having normal bowel movements, it is time to begin prompted toilet sits during times when the child is likely to defecate. These sits can be scheduled up to five times daily for three to five minutes each. The portable timer, which previously signaled the end of positive sits, now terminates the end of each prompted sit. The best time to schedule prompted sits is five to 20 minutes after each meal—to take advantage of the gastrocolic reflex. Additional sits can be scheduled during high-frequency opportunities as indicated by the daily toileting diary. From the child's perspective, these prompted sits will appear to be no different than the earlier positive sits, as foot support, toys, activities and individual attention are still available. The child's behavior has simply been shaped to the point where he or she can now sit on the toilet without pants or diapers, in a pleasant and relaxed atmosphere, during a time when he or she is likely to defecate.
Once this guideline is satisfied, the family is ready to hold a “graduation ceremony.” This ceremony involves having a small party and informing the child that he or she is now a “big boy” (or girl) and that diapers will no longer be used. It is important that parents do not use diapers occasionally during the day (e.g., on a shopping trip) because that sends a mixed message to the child about toileting expectations.
Guideline 5: Provide Incentives for Appropriate Bowel Movements and Self-Initiation
Although some authors recommend using incentives to target clean pants or diapers,23,24 this practice may encourage fecal withholding and increase the risk of constipation. Incentives can instead be tied to the passage of fecal material in the toilet. Incentives will be most effective if they are age-appropriate, given immediately after the desired behavior is displayed and provided after every occurrence of the behavior during the early phases of teaching.
Many types of incentive programs can be developed, depending on the age of the child, including access to candy, star charts, dot-to-dot pictures, grab bags and special privileges or activities with parents and peers. Selected incentives should be made available only after appropriate toileting, and access to these incentives should be restricted at other times.
When the child is eliminating in the toilet and no longer having daily soiling accidents, self-initiation skills can be targeted. Parents will want to gradually reduce verbal prompts to use the toilet, train the child to recognize the need to urinate or defecate and teach the child to request to use the bathroom each time. Incentives are now provided any time the child requests access to the bathroom and produces a bowel movement. Young children should inform the parent or caregiver before using the bathroom to ensure proper monitoring and hygiene.
Guideline 6: Arrange for Physician Contact in Case of Stool Withholding
Although ensuring frequent, soft and well-formed bowel movements should reduce the likelihood of a child withholding fecal material, a back-up plan is necessary. For example, the family could be asked to contact the physician if the child withholds for four consecutive days. A daily regimen of dietary supplements or stool softeners, as outlined in Guideline 3, may be all that is needed. If stool withholding leads to impaction, the physician may suggest hypertonic phosphate enemas (one to two per day, for up to three days) or suppositories, both of which work efficiently.14 If parents prefer an oral plan, the physician may use electrolyte solutions or high-dose mineral oil, in a dosage of 15 to 30 mL per year of age per day (maximum: 8 oz). Electrolyte solutions often require inpatient admission and nasogastric tubes to administer the volume and rate needed for effective evacuation. Mineral oil usually takes longer to work than enemas and may result in increased soiling, cramping and abdominal pain until the fecal mass is passed.25 Once the child is no longer impacted, the physician can return to the daily regimen.
The following illustrative case demonstrates the efficacy of these treatment guidelines in a child with nonretentive encopresis and toileting refusal.
Illustrative Case
A healthy four-year-old boy whose developmental and behavioral histories were unremarkable was brought to the physician because of a 16-month resistance to bowel training. He was generally cooperative with adult requests, exhibited age-appropriate social skills and rarely engaged in temper tantrums or aggressive behavior.
His foster mother reported that he had accomplished daytime bladder training by three years of age, when he began wearing ordinary underpants. He used an adult-sized toilet and stood during urination; however, he had never produced a bowel movement in the toilet. When he needed to defecate, he brought a diaper to his foster mother, stood in front of her and said, “I go poop.” Within one-half hour of being diapered, he would usually walk behind the living room couch to defecate into the diaper. Immediately after defecation, he would return to his foster mother, who would remove the diaper, clean him and put him back into ordinary underpants. The child would defecate only while at home in the living room and only when diapered. In the event of a family outing, arrangements were made to return home to provide him the opportunity to defecate. On occasions when he was refused a diaper, he repeatedly requested a diaper and withheld defecation for up to three days.
A complete history and physical examination revealed no significant medical findings or evidence of fecal impaction. Behavioral assessment included a brief clinical interview, behavior rating scales and a toileting diary that the foster mother maintained throughout assessment and intervention.
The child was placed on a daily fiber supplement to ensure frequent bowel movements and to reduce the likelihood of fecal withholding. The foster mother agreed to contact the physician if the child had not defecated for four days. A program of positive toilet sits was begun, using preferred toys while the foster mother actively engaged him in play and conversation. A kitchen timer was used to signal the end of his “bathroom fun.”
It was reported that he “accidentally” produced his first bowel movement in the toilet during a positive sit. Although he appeared fearful at first, his foster mother reassured him through physical affection, verbal praise and a small reward. By the seventh day, the boy willingly sat on the toilet and was enjoying bathroom activities. During the second week, family and adult friends held a “graduation ceremony,” during which his diapers were symbolically thrown away.
For several days after his graduation, the child repeatedly asked for a diaper. These requests were ignored and the fiber supplements and prompted toilet sits were continued; however, the child did not defecate for three consecutive days. The physician encouraged waiting one more day before beginning oral mineral therapy. The next day, the child defecated during one of his prompted toilet sits.
Over the next few weeks, he continued with the scheduled sits, fiber supplements and incentives for appropriate toileting while his foster mother monitored his toileting habits. By the third week he was no longer soiling his pants and had begun to independently request to use the bathroom. Consequently, the fiber supplements, prompted sits and incentives were gradually discontinued. During a six-month follow-up telephone contact, it was reported that he continued to toilet independently with no soiling accidents (Figure 1).
FIGURE 1. Illustrative Case
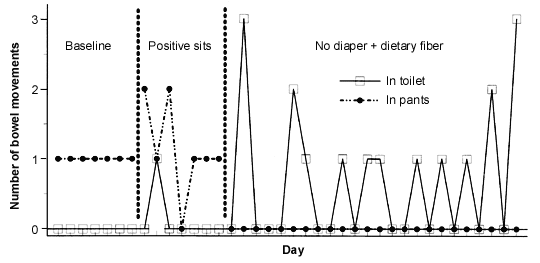
Frequency of soiling accidents and bowel movements in toilet and pants across baseline and intervention in the patient in the illustrative case.

