Fractures of the proximal portion of the fifth metatarsal may be classified as avulsions of the tuberosity or fractures of the shaft within 1.5 cm of the tuberosity. Tuberosity avulsion fractures cause pain and tenderness at the base of the fifth metatarsal and follow forced inversion during plantar flexion of the foot and ankle. Local bruising, swelling and other injuries may be present. Nondisplaced tuberosity fractures are usually treated conservatively, but orthopedic referral is indicated for fractures that are comminuted or displaced, fractures that involve more than 30 percent of the cubo-metatarsal articulation surface and fractures with delayed union. Management and prognosis of both acute (Jones fracture) and stress fracture of the fifth metatarsal within 1.5 cm of the tuberosity depend on the type of fracture, based on Torg's classification. Type I fractures are generally treated conservatively with a nonweight-bearing short leg cast for six to eight weeks. Type II fractures may also be treated conservatively or may be managed surgically, depending on patient preference and other factors. All displaced fractures and type III fractures should be managed surgically. Although most fractures of the proximal portion of the fifth metatarsal respond well to appropriate management, delayed union, muscle atrophy and chronic pain may be long-term complications.
Patients with fractures of the proximal portion of the fifth metatarsal commonly present to family physicians. The two basic fracture types are tuberosity avulsion fractures and fractures of the metatarsal shaft within 1.5 cm of the tuberosity (Table 1). When acute, the latter type is commonly referred to as a Jones fracture. Stress fractures also occur.
TABLE 1 Classification System for Fractures of the Proximal Fifth Metatarsal
| A. Tuberosity avulsion fracture | ||
| B. Fractures of the proximal metatarsal within 1.5 cm of the tuberosity | ||
| Acute Jones fracture | ||
| Type I: early | ||
| Type II: delayed union | ||
| Type III: nonunion | ||
| Stress fractures | ||
| Type I: early | ||
| Type II: delayed union | ||
| Type III: nonunion | ||
Anatomy and Initial Evaluation
The fifth metatarsal consists of a base, the tuberosity, the shaft (diaphysis), the neck and the head (Figure 1). The tuberosity (styloid process) is a bony prominence that protrudes laterally and plantarward from the base of the fifth metatarsal.1 The distal metaphysis tapers to the tubular diaphysis (shaft) of the fifth metatarsal. Acute and stress fractures of the metatarsal shaft, within 1.5 cm of the tuberosity, occur in this area. Associated soft tissue structures include the lateral band of the plantar fascia, the peroneus brevis tendon and the peroneus tertius tendon. The peroneus brevis tendon inserts in a fan-like pattern across the proximal fifth metatarsal. In contrast, the static lateral band of the plantar fascia has a focused insertion on the proximal tip of the fifth metatarsal. Both structures have been implicated in avulsion-type fractures.2–5
FIGURE 1.
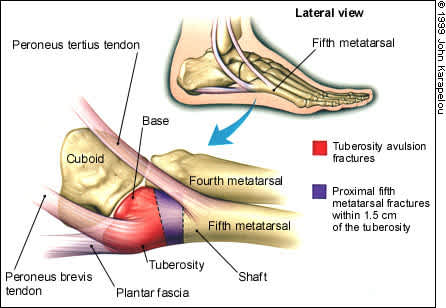
Anatomy and regional structures of the proximal fifth metatarsal.
Diagnosis of fractures of the proximal fifth metatarsal relies on the basic principles of evaluating musculoskeletal injuries. The history should focus on the mechanism of injury. In addition, any previous injury in the area or prodromal symptoms should be noted. Physical examination should elicit the point of maximal tenderness with careful neurovascular and soft tissue assessment. Radiographs should include three views of the foot—anteroposterior, lateral and oblique.
Tuberosity Avulsion Fractures
Avulsion fractures of the tuberosity are the most common fractures involving the proximal fifth metatarsal. If not displaced or comminuted, these fractures uniformly heal well with conservative treatment. It is imperative that the clinician differentiate this fracture from fractures of the metatarsal shaft within 1.5 cm of the tuberosity.
HISTORY AND PHYSICAL EXAMINATION
The patient with an avulsion fracture experiences the sudden onset of pain at the base of the fifth metatarsal. These fractures occur after forced inversion with the foot and ankle in plantar flexion. Physical examination reveals tenderness at the base of the fifth metatarsal, often with ecchymosis and swelling at the site. Full evaluation of the distal fibula and lateral ligamentous structures must be included in the assessment.
RADIOGRAPHS
Radiographs show radiolucency located proximal to the metaphyseal-diaphyseal junction (Figure 2). These fractures are usually perpendicular to the long axis of the fifth metatarsal. Although the avulsion fracture is often extra-articular, involvement of the metatarsal-cuboid joint is not uncommon.
FIGURE 2.
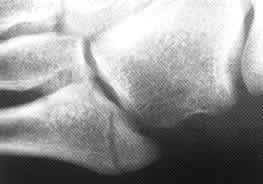
Tuberosity avulsion fracture. Note that the radiolucency is perpendicular to the long axis of the fifth metatarsal. Intra-articular involvement is not present in this example.
DIFFERENTIAL DIAGNOSIS
Apophysis. The development of a secondary center of ossification (apophysis) at the proximal end of the fifth metatarsal can be mistaken radiographically as a fracture site (Figure 3). In girls nine to 11 years of age and boys 11 to 14 years of age, the apophysis becomes visible on plain radiographs as a fleck of calcification adjacent to the fifth metatarsal shaft.1 The apophysis has an oblique orientation, with the radiolucency aligned parallel to the fifth metatarsal diaphysis. No treatment is necessary.
FIGURE 3.
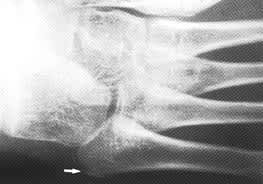
Apophysis (arrow) of the base of the fifth metatarsal, common in girls nine to 11 years of age and in boys 11 to 14 years of age. Note the oblique orientation with the radiolucency aligned in parallel to the fifth metatarsal diaphysis.
Apophysitis (Iselin's Disease). Apophysitis of the fifth metatarsal base (Iselin's disease) is a self-limiting disorder of active children that spontaneously resolves with completion of growth. The child complains of localized pain on activity that resolves with rest. Physical examination reveals tenderness at the fifth metatarsal base. Rarely, the clinician finds associated ecchymosis and edema. Radiographic findings include irregular apophyseal density and shape. Treatment is primarily limitation of activity.6
Accessory Ossicles. Accessory ossicles may also be confused with avulsion fractures. The os vesalianum is quite rare and may be found next to the peroneus brevis insertion. The more common os peroneum can be located at the lateral border of the cuboid within the substance of the peroneus brevis tendon. Each ossicle can be radiographically differentiated by its smooth appearance; in contrast, avulsion fractures appear to have “scalloped” edges. Symptomatic accessory ossicles may be definitively treated with surgical excision.
TREATMENT
Treatment of nondisplaced tuberosity avulsion fractures is conservative. Options include elastic wrapping, ankle splints and low-profile walking boots or casts. Weight bearing is allowed as tolerated. Treatment should be continued until symptoms abate—usually within three to six weeks.7–9 Plain film evidence of union varies widely but is generally evident within eight weeks.1 Rarely, the fracture may heal by asymptomatic fibrous union.
INDICATIONS FOR ORTHOPEDIC REFERRAL
Displaced fractures of the tuberosity are best managed by either open reduction and internal fixation or closed reduction and pinning. Comminuted fractures and avulsion fractures involving more than 30 percent of the cubo-metatarsal articulation surface should also be considered for orthopedic referral5 (Figure 4).
FIGURE 4.
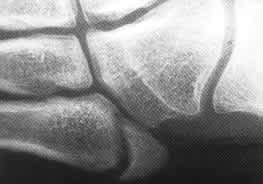
Tuberosity avulsion fracture with intra-articular involvement. This example involves greater than 30 percent of the cubo-metatarsal articulation with displacement. These characteristics help define indications for surgical consultation.
Proximal Fifth Metatarsal Fractures
Sir Robert Jones described his own fracture of the fifth metatarsal in 1902, when he injured himself while dancing around a Maypole at a military garden party. The mechanism of injury was described as treading on the outer side of his foot with his “heel at the moment being off the ground.” He described the location of the fracture as occurring in the 3/4-in (1.5-cm) segment of the shaft on the fifth metatarsal distal to the styloid.10
CLASSIFICATION/RADIOGRAPHIC APPEARANCE
The classification system based on historical and radiographic criteria developed by Torg and colleagues11–13 has been used to classify these fractures and to identify those suitable for nonoperative treatment (Table 2). Type I fractures are described as having “no intramedullary sclerosis, a sharp, well-delineated fracture line and minimal cortical hypertrophy”12 (Figure 5). Type II fractures (delayed unions) have “a fracture line that involves both cortices with associated periosteal new bone, a widened fracture line with adjacent radiolucency related to bone resorption and evidence of intramedullary sclerosis”12 (Figure 6). Type III fractures (nonunions) have “a wide fracture line with periosteal new bone and radiolucency, and complete obliteration of the medullary canal at the fracture site by sclerotic bone.”12
TABLE 2 Torg's Classification System for Fractures of the Proximal Fifth Metatarsal Within 1.5 cm of the Tuberosity
| Torg classification | Radiographic appearance |
|---|---|
| Type I (Figure 5) | No intramedullary sclerosis |
| Fracture line with sharp margins and no widening | |
| Minimal cortical hypertrophy | |
| Minimal evidence of periosteal reaction to chronic stress | |
| Type II, delayed | Fracture line that involves both cortices with associated periosteal bone union (Figure 6) |
| Widened fracture line with adjacent radiolucency related to bone resorption | |
| Evidence of intramedullary sclerosis | |
| Type III, nonunion | Wide fracture line |
| Periosteal new bone and radiolucency | |
| Complete obliteration of the medullary canal at the fracture site by sclerotic bone |
FIGURE 5.
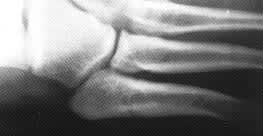
Fracture of the metatarsal shaft within 1.5 cm of the tuberosity, type I. This example is an acute Jones fracture. Type I fractures have no intramedullary sclerosis, a sharp fracture line and no widening. Cortical hypertrophy is not present in this example.
FIGURE 6.
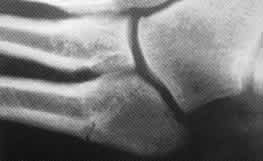
Fracture of the fifth metatarsal shaft within 1.5 cm of the tuberosity, type II. This type II fracture includes intramedullary sclerosis, widening of the fracture line and cortical hypertrophy. The history is critical in distinguishing acute type II fractures (delayed unions) from stress-type fractures (see Table 1).
Acute Fractures (Jones Fractures)
HISTORY AND PHYSICAL EXAMINATION
Patients describe sudden pain at the base of the fifth metatarsal, with difficulty bearing weight on the foot. Often, ecchymosis and/or edema will be present at the site. The mechanism of injury is described as a laterally directed force on the forefoot during plantar flexion of the ankle. Examples include pivot-shifting in football or basketball, with the heel off the ground.
TREATMENT
Before the development of Torg's classification system, high rates of nonunion were reported in patients with Jones fracture. It has been postulated that these nonunions were due to disruption of the vascular supply, which enters the bone in the metaphyseal-diaphyseal region.14,15 However, if the fracture is properly classified as type I or type II, treatment is initially conservative in all but elite athletes, advanced amateur athletes, or patients who prefer surgical treatment.
Type I fractures are treated with a non-weight-bearing, short leg cast for six to eight weeks, with progressive ambulation after cast removal. Type II fractures may also be treated with a nonweight-bearing cast, but a prolonged period may be required until union is achieved. In competitive athletes, these fractures are usually treated operatively, either with medullary curettage and inlay bone grafting or intramedullary screw fixation. Type III fractures should be treated operatively (Table 3). Complications associated with surgical fixation include persistent pain at the base of the fifth metatarsal and may require screw removal and shoe modifications.5 In addition, surgical treatment of acute Jones fractures may result in delayed union, nonunion or refracture.16
TABLE 3 Fractures of the Proximal Fifth Metatarsal: Mechanism, Treatment, Chronicity and Prognosis
| Fracture type | Mechanism | Initial treatment | History | Prognosis |
|---|---|---|---|---|
| Acute fracture of the proximal metatarsal within 1.5 cm of tuberosity (Jones fracture) | Laterally directed force on forefoot with ankle in plantar flexion | Type I: nonweight-bearing immobilization for six to eight weeks | Acute incident | Type I: good healing potential |
| Type II: nonweight-bearing immobilization vs. surgical fixation for active athletes or patients preferring surgical therapy | Types II, III: variable healing potential | |||
| Type III: surgical fixation | ||||
| Stress fracture of the proximal metatarsal within 1.5 cm of tuberosity | Repetitive microtrauma | Type I: nonweight-bearing immobilization for six to eight weeks (may require up to 20 weeks) | Variable prodrome (weeks to months) | Variable healing potential |
| Type II: nonweight-bearing immobilization vs. surgical fixation for active athletes or patients preferring surgical therapy | ||||
| Type III: surgical fixation | ||||
| Tuberosity avulsion fracture | Forced inversion with ankle in plantar flexion | Elastic wrapping, ankle splints, low-profile walking boot or cast with weight bearing as tolerated (approximately three to six weeks) | Acute incident | Excellent healing potential |
INDICATIONS FOR ORTHOPEDIC REFERRAL
Based on the treatment guidelines listed above, any patient with a type III fracture should be referred to an orthopedic surgeon. In a type II fracture, referral should be considered if the patient is an active athlete, requires an accelerated healing time or prefers surgical treatment. Most type I fractures can initially be treated nonoperatively; however, a referral should be made if the patient is an active athlete or prefers surgical treatment.17 Patients with displaced fractures should always be referred for surgical consultation.
Stress Fractures
It is important to differentiate the stress fracture from the more acute Jones fracture, as treatment and prognoses differ (Table 3). Differentiation is based on history. A history of prodromal pain suggests the likelihood of a stress fracture. Patient history is the most critical determinant, since radiographic appearance may be nearly impossible to distinguish. While some authors have postulated that stress fracture occurs in a different anatomic region than the acute fracture,5,7 no conclusive evidence supports this postulation.
HISTORY AND PHYSICAL EXAMINATION
Stress fracture occurs predominantly in younger patients and athletes. Athletes often present early in the training season. Patients complain of pain at the base of the fifth metatarsal and may have ecchymosis and edema at the site. They usually report a prodromal period of aches and pain at the base of the fifth metatarsal while exercising or weight bearing. The prodromal period can vary from weeks to months before initial presentation.
TREATMENT
Stress fractures are treated as acute fractures of the proximal metatarsal within 1.5 cm of the tuberosity. It is important to note that nonweight-bearing immobilization for up to 20 weeks may be needed and that nonunions may still occur, necessitating surgical intervention. Treatment options, as well as potential complications of prolonged immobilization, such as reflex sympathetic dystrophy and muscle atrophy, should be fully discussed with the patient at the time of presentation. Treatment of type II and type III stress fractures parallels that described for acute fractures (Table 3).
INDICATIONS FOR ORTHOPEDIC REFERRAL
Criteria for referral of stress fracture are the same as for acute fractures. Elite athletes, active athletes or patients who are reluctant to undergo conservative treatment with possible prolonged immobilization should be considered for surgical intervention. Type III fractures require surgical fixation, and type II fractures may require surgery, depending on the patient's activity level and preference.

