Refreshing sleep requires both sufficient total sleep time as well as sleep that is in synchrony with the individual's circadian rhythm. Problems with sleep organization in elderly patients typically include difficulty falling asleep, less time spent in the deeper stages of sleep, early-morning awakening and less total sleep time. Poor sleep habits such as irregular sleep-wake times and daytime napping may contribute to insomnia. Caffeine, alcohol and some medications can also interfere with sleep. Primary sleep disorders are more common in the elderly than in younger persons. Restless legs syndrome and periodic limb movement disorder can disrupt sleep and may respond to low doses of antiparkinsonian agents as well as other drugs. Sleep apnea can lead to excessive daytime sleepiness. Evaluation of sleep problems in the elderly includes careful screening for poor sleep habits and other factors that may be contributing to the sleep problem. Formal sleep studies may be needed when a primary sleep disorder is suspected or marked daytime dysfunction is noted. Therapy with a benzodiazepine receptor agonist may be indicated after careful evaluation.
Complaints of sleep difficulty are common among the elderly. In a National Institute on Aging study of over 9,000 persons aged 65 years and older, over one half of the men and women reported at least one chronic sleep complaint.1 Typical symptoms of sleep problems in the elderly include difficulty falling asleep and maintaining sleep, early-morning awakening and excessive daytime sleepiness.
A variety of processes may interfere with sleep and wakefulness in the elderly.2,3 Among them are acute and chronic medical illnesses, medication effects, psychiatric disorders, primary sleep disorders, social changes, poor sleep habits and circadian rhythm shifts. Sleep-wake problems may be compounded further by inappropriate treatment initiated by the patient, family members, physicians or other care providers.
The consequences of chronic sleep problems can be considerable. Loss of sleep or chronic use of sedating medications may lead to falls and accidents.4,5 Sleep-disordered breathing may have serious cardiovascular, pulmonary and central nervous system effects. Evidence supports a strong association between sleep apnea and hypertension.6–8 In persons with dementia, severe sleep disruption often leads to nursing home placement. For all of these reasons, sleep problems in elderly patients should be properly evaluated and treated.
Normal Sleep
Two primary factors control the physiologic need for sleep: the total quantity of sleep and the daily circadian rhythm of sleepiness and alertness. For optimal daytime alertness, humans require an average of about eight hours of sleep for a 24-hour period. Sleep deprivation causes increased sleepiness and may cause cognitive impairment.
Under normal conditions, the circadian rhythm promotes a daily cycle of nighttime sleep and daytime alertness. Also commonly experienced is the physiologic mid-afternoon dip in alertness, which can be conducive to napping. It is now well established that a person's circadian rhythm is strongly influenced by exposure to light.
Normal sleep progresses through a number of stages during each sleep period. Rapid-eye movement (REM) sleep encompasses 15 to 25 percent of the total amount of sleep and is associated with dreaming, as well as increased lability of heart rate, blood pressure and respiration. Non-REM sleep is subdivided into four stages of increasing depth. The deepest non-REM sleep generally occurs in the early part of the night. Episodes of REM sleep occur at approximately 90-minute cycles, with the duration of each episode tending to increase throughout the night. As can be seen in Figure 1, elderly persons have more fragmented sleep and a shorter duration of stage 3 and stage 4 sleep than that occurring in young adults.
FIGURE 1. Comparison of Sleep Cycles in Young Adults and the Elderly
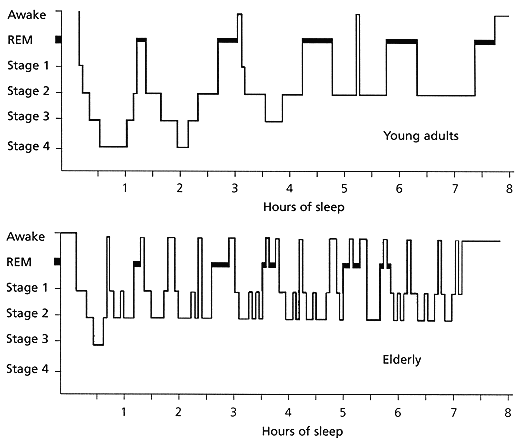
Hypnograms demonstrating typical sleep characteristics in young adults and elderly persons. Compared with young adults, the elderly tend to have delayed sleep onset, fragmented sleep, early-morning awakening and decreased time in sleep stages 3 and 4. (REM = rapid eye movement)
Sleep and Aging
Several generalizations can be made regarding aging and sleep characteristics. Compared with younger persons, elderly persons tend to achieve less total nighttime sleep. However, it cannot be assumed that elderly persons require less sleep. Elderly persons have more nighttime arousals and awakenings. Increased daytime sleepiness may be the effect of such a pattern. Overall, the sleep-wake cycle in the elderly may be fragmented, with interrupted nighttime sleep and daytime wakefulness interrupted by naps. The deepest stages of non-REM sleep are frequently reduced or nonexistent in elderly persons; however, REM sleep tends to be preserved. Although a mild deterioration in sleep quality may be normal in the aging process, an elderly patient's complaint of significantly disrupted nighttime sleep or impaired daytime functioning because of excessive sleepiness must be evaluated.
Another common age-associated sleep change relates to the circadian rhythm of the typical sleep period. Although exceptions exist, elderly persons tend to go to sleep earlier in the evening and to awaken earlier in the morning. Early-morning awakening is a common complaint in the elderly. Some people find it annoying to awaken spontaneously at 4:30 a.m. instead of at 6:30 a.m. In these persons, if the onset of evening sleep is not correspondingly earlier, sleep deprivation and excessive daytime sleepiness may result.
Daytime napping may compound the problem by reducing the drive for sleep at the usual bedtime hour, resulting in delayed sleep onset and a further decrease in the duration of nighttime sleep.
Less common in elderly persons, but sometimes dramatic, is the development of a “night owl” pattern, with bedtime delayed until the early-morning hours. This sleep-wake cycle may have been tolerated in the younger years during employment, when the cues of early-morning bright light were stronger and the regularity of sleep-wake hours was greater. On retirement, however, these cues weaken, and the sleep-wake cycle may become delayed by several hours. These patients may complain of day-night reversal, where sleep does not begin until dawn and then continues until mid-afternoon.
Factors That May Disrupt Sleep
It is important to keep multiple factors in mind when evaluating sleep complaints in elderly patients because a number of problems may contribute to poor sleep (Table 1). Nighttime insomnia and excessive daytime sleepiness should not be viewed as isolated symptoms. It is important to obtain a complete sleep history that includes the entire 24-hour day to examine all of the factors that may influence sleep and wakefulness (Table 2). Asking the patient to keep a sleep log that covers all sleep over a period of several weeks may be helpful in establishing the patient's sleep patterns. In addition to an assessment of the timing and regularity of bedtime, sleep onset, nighttime awakenings and daytime naps, other important features in the evaluation include the usual total sleep time during a 24-hour period and the predictability of the longest uninterrupted sleep periods.
TABLE 1 Factors Contributing to Sleep Problems in the Elderly
| Primary sleep disorders | |
| Circadian rhythm disorder | |
| Sleep apnea (obstructive, central or mixed) | |
| Restless legs syndrome | |
| Periodic limb movement disorder (nocturnal myoclonus) | |
| REM–behavior disorder | |
| Pain from any source | |
| Neurologic disease (e.g., Parkinson's disease, Alzheimer's disease) | |
| Cardiovascular disease | |
| Gastrointestinal disease | |
| Pulmonary disease | |
| Psychiatric disorders (e.g., anxiety, depression, psychosis, dementia, delirium) | |
| Medications and other substances | |
| Alcohol | |
| Anticholinergics | |
| Antidepressants | |
| Antihypertensive agents | |
| Caffeine | |
| Corticosteroids | |
| Diuretics | |
| Herbal remedies | |
| Histamine H2 blockers | |
| Levodopa | |
| Nicotine | |
| Sympathomimetics | |
| Poor sleep habits | |
REM = rapid eye movement.
TABLE 2 Factors to Consider When Evaluating Sleep Problems in the Elderly
| Is the patient's complaint predominantly excessive sleepiness, inability to go to sleep at a desired time, early-morning awakening or a combination of these features? |
| Is total sleep insufficient and is sleep attempted at times that are not synchronous with the patient's circadian rhythm? |
| Are stressors or environmental factors influencing the sleep-wake cycle, such as a barking dog, ringing telephone, too much light or uncomfortable temperature in the bedroom? |
| Is an underlying medical or psychiatric illness contributing to the sleep disturbance? |
| Are stimulating or sedating effects of substances such as caffeine, alcohol and over-the-counter or prescription drugs playing a role in the patient's sleep problems? |
| Does the patient have a primary sleep disorder, such as sleep apnea, restless legs syndrome or periodic limb movements? |
| Are poor sleep habits, such as activity other than sleep in bed, irregular sleep-wake times or daytime napping, perpetuating the patient's symptoms? |
Treatment directed at correcting inappropriate sleep-wake timing or increasing the total sleep time if it is insufficient may produce considerable improvement of the patient's sleep problem or even completely resolve it. A full investigation of a complaint of insufficient sleep or excessive daytime sleepiness includes consideration of other potential problems that contribute to disrupted sleep, such as poor sleep habits, medical illness, medications and psychiatric disorders.
POOR SLEEP HABITS
Poor sleep habits are a very common cause of sleep disruption. Irregular sleep-wake patterns related to lifestyle or work requirements can undermine the ability of the circadian system to effectively provide sleepiness and wakefulness at appropriate times. Caffeine intake can continue to have alerting effects for many hours. Consumption of caffeine-containing beverages in the afternoon can impair nighttime sleep. Alcohol consumption in the evening, while initially sedating, prevents deeper sleep and increases arousals during the latter part of the night. Excessive wakeful time in bed may cause the patient to develop increased arousal that is reinforced nightly.
MEDICAL ILLNESS
Acute and chronic medical illnesses, such as arthritis, prostatic hypertrophy and cardiovascular, gastrointestinal and pulmonary diseases, may precipitate sleep disruption. Pain and discomfort may delay sleep onset and shorten the duration of sleep. Deterioration of the sleep-wake cycle can accompany neurodegenerative disorders, particularly Alzheimer's disease.
MEDICATIONS
Many medications can have stimulating effects and thereby cause sleep disruption. Included among them are some antidepressants (particularly selective serotonin reuptake inhibitors), decongestants, bronchodilators, some antihypertensives and corticosteroids. Predictably, nighttime use of diuretics can promote repeated awakening to go to the bathroom. The potential sedating effects of medications (especially long-acting sedatives that are inappropriately used as sleep aids) should also be a consideration in patients who report excessive daytime sleepiness.
PSYCHIATRIC DISORDERS
Distress from acute symptoms of a psychiatric disorder may promote disturbed sleep. A classic example is insomnia in association with major depression. The tendency toward increased arousals and early-morning awakening in an elderly person may be severely exacerbated in the presence of depression. Also contributing to a deterioration in the quality of sleep are the psychologic manifestations of the assorted life changes that elderly persons often experience. Significant factors include physical limitations, loss of loved ones and leaving a familiar home to live in a more supervised setting.
Primary Sleep Disorders
Several primary sleep disorders are associated with aging. Primary sleep disorders may delay sleep onset, cause multiple arousals and awakenings, and promote excessive daytime sleepiness (Table 3). Wandering behavior and confusional arousals may occur, especially in patients with dementing disorders. In rare instances, behaviors emanating from sleep may result in serious injury to the patient or bed partner.
TABLE 3 Characteristics of Primary Sleep Disorders
| Sleep disorder | Clinical features | Method of diagnosis | Treatment | Comments |
|---|---|---|---|---|
| Sleep apnea | Loud snoring, obesity, daytime sleepiness | History and physical examination; polysomnogram | CPAP during sleep, weight loss; surgery (?) | Intermittent airway closure; affects men more than women; use of sedatives at night can worsen condition |
| Restless legs syndrome | Motor restlessness and pacing in the evening | History | Dopaminergic agents, benzodizepines, opiates | More common with iron deficiency; may develop in association with renal failure; periodic limb movement disorder often present |
| Periodic limb movement disorder | Kicking of legs during sleep, frequent arousals from sleep, daytime sleepiness | Polysomnogram | Dopaminergic agents | Contractions may extend to other muscle groups; may occur during waking periods |
| REM–behavior disorder | Thrashing or seemingly purposeful behaviors during sleep | History, polysomnogram | Clonazepam (Klonopin) | Mostly idiopathic; injury to patient or bed partner is possible |
CPAP = continuous positive airway pressure; REM = rapid eye movement.
RESTLESS LEGS SYNDROME AND PERIODIC LIMB MOVEMENT DISORDER
Restless legs syndrome is characterized by an intense discomfort, mostly in the legs, during the evening when the person is at rest.9 It is an akathisia, often described as a “creepy-crawly” sensation. The patient notes a strong urge to keep moving the legs or to get up and walk around to relieve the discomfort. Restless legs syndrome may significantly interfere with the onset of sleep.
Periodic limb movement disorder, another primary sleep disorder, may accompany restless legs syndrome or occur independently. This idiopathic condition is characterized by episodes of stereotypic rhythmic movement, usually of the legs, although other muscle groups, including the arms, may be involved in severe cases. The patient's bed partner typically perceives these episodes as kicks that occur in cycles of 20 to 40 seconds. Hundreds of limb movements may occur during a single night, but most of the time they do not awaken the affected person. They may, however, produce many brief arousals that disrupt sleep organization and decrease the amount of time in the deeper stages of sleep. The delayed sleep onset related to restless legs syndrome and the sleep disruption from periodic limb movements cause daytime sleepiness. Restless legs syndrome is primarily a clinical diagnosis. Periodic limb movement disorder may be suspected based on information obtained from a bed partner. If necessary, the diagnosis can be confirmed by electromyography of limb muscle activity during nighttime monitoring in a sleep laboratory.9 Risk factors for these two disorders include increasing age, renal failure and iron deficiency (serum ferritin level less than 50 ng per mL). Up to one third of elderly persons have measurable periodic leg movements during sleep; however, only relatively high rates of events and high percentages of associated arousal should be regarded as clinically significant. The degree of distress reported by the patient should influence the treatment decision.
Soaking the legs and feet in a warm bath or engaging in regular exercise provides relief of restless legs syndrome in some patients. The most appropriate initial pharmacologic treatment for both restless legs syndrome and periodic limb movement disorder is carbidopa-levodopa (Sinemet) and other dopaminergic agents. Comorbid conditions such as a low iron level also may need to be corrected for an adequate response. Carbidopa-levodopa (in the 25- to 100-mg formulation) may be started in a dosage of one half tablet at bedtime. The dosage can be increased in increments of one half tablet every three or four days, to a maximum of two tablets per day. As with the use of carbidopa-levodopa in the treatment of Parkinson's disease, the development of so-called augmentation, where the motor restlessness begins earlier in the evening or in the afternoon, is a potential problem with this agent.
Pergolide (Permax), starting at a very low dosage, such as 0.05 mg two hours before bedtime, and gradually increasing up to 0.5 mg, also has been used successfully in the treatment of restless legs syndrome and periodic limb movement disorder. In some cases, a bedtime dose of a benzodiazepine or a low-potency opiate, such as codeine or oxycodone (Roxicodone), may be beneficial. Other drugs tried in the treatment of restless legs syndrome include bromocriptine (Parlodel), carbamazepine (Tegretol), clonidine (Catapres) and clonazepam (Klonopin). Patients may appreciate the information and support that are available from organizations such as the Restless Legs Syndrome Foundation (Web site: http://www.rls.org).
SLEEP APNEA
Sleep apnea commonly causes repeated episodes of brief arousal, of which the patient often is not aware, and may promote extended awakenings from sleep.10,11 The patient may report insomnia but more commonly notes excessive daytime sleepiness. Hundreds of apneic events may occur during a night. The frequent sleep interruptions, coupled with repeated drops in the blood oxygen saturation, may cause a marked decline in daytime alertness and performance. Sleep may intrude on daytime activities such as driving, with dangerous consequences. Patients suspected of having sleep apnea are evaluated in a sleep laboratory, where monitoring of the electroencephalogram, blood oxygen saturation, airflow, and chest and abdomen ventilatory efforts can be performed to confirm the diagnosis.
The apneic events usually result from complete or partial occlusion of the airway (obstructive sleep apnea) or, less commonly, from a decrease in the respiratory drive (central sleep apnea). Risk factors for sleep apnea include male sex and obesity (especially a heavy neck). Sleep apnea may be associated with hypothyroidism, neurodegenerative disorders and cardiovascular disorders. The major clinical clue to sleep apnea is a history of loud, excessive snoring, punctuated by pauses that are followed by stuttered gasps for breath. Observations by the patient's bed partner or another family member can provide the physician with crucial information. Weight loss is frequently beneficial in overweight patients with sleep apnea. However, the mainstay of therapy is continuous positive airway pressure during sleep, which is accomplished by having the patient wear a tight-fitting nasal mask. Surgical intervention often eliminates snoring but may not eliminate the apnea. Effective control of sleep apnea can produce more consolidated nighttime sleep and a dramatic improvement in daytime alertness and functioning.
REM-BEHAVIOR DISORDER
The rare REM-behavior disorder occurs most commonly in elderly persons. Underlying this disorder is disinhibition of the process that normally prevents transmission of muscle activity during dreaming. The patient may thrash about in bed, sometimes falling or leaping from the bed and incurring significant injury. Treatment with bedtime doses of a long-acting benzodiazepine such as clonazepam often provides effective control of this disorder.
General Treatment Considerations
Because many factors influence the sleep-wake cycle, treatment must be individualized according to the patient's specific symptoms and findings from the patient's evaluation.12 Several generalizations are possible, however. Implementation of good sleep habits and daily physical activity should help create an environment conducive to restorative sleep (Table 4). Even if poor sleep habits are not responsible for insomnia, elimination of such habits can minimize their perpetuating influence.
TABLE 4 Proper Sleep Habits
| Regularity of sleep and wake times |
| Avoidance of excessive time in bed |
| Relaxing bedtime routine |
| Daily activity and exercise |
| Avoidance of caffeine, alcohol and nicotine in the afternoon and evening |
| Elimination of loud noise, excessive light and uncomfortable room temperature |
Daily exercise and exposure to daylight can help reinforce the circadian cycle. These measures have the greatest potential for improving the quality of sleep in elderly persons. Exposure to bright light for 30 to 60 minutes in the evening may benefit patients with early bedtimes who complain of early-morning awakening.13 Minimizing the amount of exposure to dawn light in the bedroom also may help. In persons with a late sleep onset and problems with late awakening in the morning, regular exposure to bright light at an early-morning hour may help shift the sleep-wake rhythm to an earlier time for sleep at night and awakening in the morning. Melatonin appears to help shift the phase of sleep, but further study is needed to clarify its use for treatment of insomnia, as well as jet lag.
Many patients with insomnia have excessive anxiety deriving from their failed attempts to sleep and respond well to a behavioral approach. If hyperarousal at bedtime has evolved, it might be useful for the patient to spend less time in bed trying to go to sleep. This may help decrease the patient's anxiety over not being able to fall asleep. Patients may be advised to avoid going to bed until they feel as though they can easily fall asleep. An extended wakeful time in bed (e.g., more than 30 minutes) should be avoided to minimize further reinforcement of hyperarousal. In addition, patients should plan relaxing nighttime activities before bedtime.
Selected patients may benefit from temporary use of sleep-promoting medications.14,15 Over-the-counter antihistamines should be used with caution in the elderly because of their relatively long duration of action and their anticholinergic effects, which may cause confusion, constipation and urinary retention. Low dosages of sedating antidepressants are especially helpful in patients with depressive symptoms. Consideration must be given to the duration of the sedation and other potential side effects.
If hypnotic medications are considered, the first choice would be a short-acting benzodiazepine receptor agonist. Generally, a low dosage and short-term use are recommended. Intermittent dosing has advantages. Occasional use minimizes potential withdrawal effects. Patients may be given guidelines, such as the recommendation that a hypnotic agent be used no more than two nights a week. The availability of a sleep medication may be reassuring to the patient on particularly difficult nights. That reassurance will likely decrease the patient's distress on nights when no medication is used.
While potentially valuable in offering relief of insomnia, hypnotic agents should not be regarded as the ultimate solution to a sleep problem. They should be used under limited circumstances, following evaluation of the patient's symptoms and in the context of good sleep habits.
Consultation with a sleep disorders specialist should be considered in patients with marked daytime sleepiness, because this symptom can be dangerous. Guidance regarding the management of chronic insomnia and sleep-related behavioral problems also may be obtained from a sleep disorders specialist. Formal sleep studies are appropriate when a primary sleep disorder is suspected.
Final Comment
A wealth of information on sleep and sleep disorders is available from various national organizations through the Internet. Useful Web sites include the American Sleep Disorders Association (http://www.asda.org), the National Sleep Foundation (http://www.sleepfoundation.org) and Sleep Home Pages (http://bisleep.medsch.ucla.edu).

