
Am Fam Physician. 1999;60(2):649-651
What is insulin, and why do I need it?
Insulin is a hormone that controls the level of blood sugar (also called glucose) in your body. People with diabetes may not have enough insulin or may not be able to use it properly. The sugar builds up in the blood and overflows into the urine, passing out of your body unused. Over time, high blood sugar levels can cause serious health problems.
All people with type 1 diabetes, and some people with type 2 diabetes, need to take insulin to help control their blood sugar levels. (The box below lists the different types of insulin.) The goal in treating diabetes is to keep the blood sugar level within a normal range.
Do I need to monitor my blood sugar level?
Yes. You need to check your blood sugar level regularly using a blood glucose monitor. Your doctor or the office staff can teach you how to use the monitor. You'll need to write down each measurement and show this record to your doctor, so your doctor can tell you how much insulin to take.
How often will I need to take insulin?
Your doctor will give you a schedule. Most people with diabetes need at least 2 insulin shots a day. Some people need 3 or 4 shots for good blood sugar control.
When should I take insulin?
If you take Regular insulin or a longer-acting insulin, you should generally take it 15 to 30 minutes before a meal. If you take insulin lispro (brand name: Humalog), which works very quickly, you should generally take it less than 15 minutes before you eat.
What is different about insulin lispro?
Insulin lispro is a new type of insulin. It starts working sooner than other insulin types. It also reaches peak activity faster and goes away sooner. Insulin lispro helps keep your blood sugar level from going too high after you eat. To keep your blood sugar level steady, your doctor will probably prescribe either a longer-acting insulin or another drug for you to take each day in addition to the insulin lispro.
If you need to mix insulin lispro with a longer-acting insulin, it's best that you mix insulin lispro only with Humulin U or Humulin N, which are brand names for certain longer-acting insulins. Insulin lispro should always be drawn into the syringe first. This will keep the longer-acting insulin from getting into the insulin lispro bottle.
Types of insulin
Each type of insulin works at a different speed and lasts for a different length of time.
Quick-acting, such as insulin lispro (Humalog), begins to work very quickly (5 to 15 minutes) and lasts for 3 to 4 hours.
Short-acting, such as Regular (R) insulin, starts working within 30 minutes and lasts about 5 to 8 hours.
Intermediate-acting, such as NPH (N) or Lente (L) insulin, starts working in 1 to 3 hours and lasts 16 to 24 hours.
Long-acting, such as Ultralente (U) insulin, doesn't start to work for 4 to 6 hours, but lasts 24 to 28 hours.
NPH and Regular insulin mixture, two types of insulin mixed together in 1 bottle, starts working in 30 minutes and lasts 16 to 24 hours.
Source: Medicine for People with Diabetes. National Diabetes Information Clearinghouse, NIH Publication No. 98-4222, November 1997.
How do I take insulin?
Insulin is normally injected under the skin with a very small needle. It can also be taken with an insulin pen. Your doctor will teach you exactly how to inject insulin, but here are the basics:
Wash your hands.
Take the plastic cover off the insulin bottle and wipe the top of the bottle with a cotton swab dipped in alcohol.
Pull back the plunger of the syringe, drawing air into the syringe equal to the dose of insulin that you are taking (measured in units). Put the syringe needle through the rubber top of the insulin bottle. Inject air into the bottle by pushing the syringe plunger forward. Turn the bottle upside down.
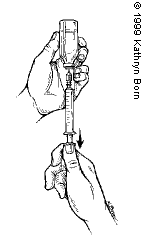
Make sure that the tip of the needle is in the insulin. Pull back on the syringe plunger to draw the correct dose of insulin into the syringe (see picture 1).
Make sure there are no air bubbles in the syringe before you take the needle out of the insulin bottle. If there are air bubbles, hold the syringe and the bottle straight up, tap the syringe with your finger and let the air bubbles float to the top. Push on the plunger of the syringe to move the air bubbles back into the insulin bottle. Then withdraw the correct insulin dose by pulling back on the plunger.
Clean your skin with cotton dipped in alcohol (see picture 2, top). Grab a fold of skin and inject the insulin under the skin at a 90-degree angle (see picture 3).
Clean the injection area using cotton and alcohol (top). Pinch an area of skin (bottom).
Inject the insulin with the needle at an angle of about 90 degrees.
If you're thin, you may need to pinch the skin and inject the insulin at a 45-degree angle (see picture 4).Thin people may find it easier to inject at an angle of 45 degrees.
Where on my body should I inject the insulin?
Ask your doctor which place you should use. Insulin injected near the stomach works fastest. Insulin injected into the thigh works slowest. Insulin injected into the arm works at medium speed.
What happens if I take too much insulin?
If you take too much insulin it will lower your blood sugar level too much, and you may get hypoglycemia (also called an insulin reaction). When you have hypoglycemia, you may feel cranky, more tired than usual, confused and shaky, and you may sweat more. You may get a headache, have a rapid heartbeat, or feel more hungry. In serious cases, you can pass out or have a seizure.
Most people who take insulin have an insulin reaction at some time. Talk to your doctor about what to do if you have hypoglycemia. Your doctor may suggest that you always have on hand a snack that has sugar in it, such as candy, fruit juice or regular (not diet) soda, to counteract hypoglycemia.