In this issue of American Family Physician, the treatment of sexually transmitted diseases (STDs) is concisely reviewed by Woodward and Fisher,1 who used for reference the “1998 Guidelines for Treatment of Sexually Transmitted Diseases,” published in January 1998 by the Centers for Disease Control and Prevention.2 The advice of both the review and the guidelines remain sound, and it will be another year before an update of the 1998 guidelines is published. Current therapies for STDs are good; what else about STDs might we consider?
It is useful to think about the relationships of reproductive tract infections (RTIs), STDs and sexually transmitted infections (STIs). All infections that occur in the genital tract are RTIs, but not all of them are sexually transmitted (see the accompanying figure). “Infection” means the presence of a microorganism in the body, while “disease” means the presence of an adverse bodily state. Although not all infections result in disease, STIs need to be identified and treated (either by medicine or counseling), because they are capable of ultimately causing disease, either in the person infected or in someone who might be infected by that person.
FIGURE:
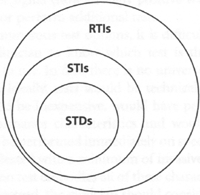
The relationship of reproductive tract infections (RTIs), sexually transmitted diseases (STDs) and sexually transmitted infections (STIs), with the size of circles representing the approximate number of each.
And, we increasingly realize that the majority of STIs (certainly in women and probably in men) are not accompanied by symptoms or signs. Thus, although persons who acquire an STI are generally prone to accuse their sex partner of knowingly “giving them something,” the transmitting partner is often “innocent,” because the infection was asymptomatic. To reach these asymptomatically infected persons, we have the following two choices: screening and partner notification.
The distinction between RTIs and STIs has important patient care implications. The term STI (my preference, over STD, and one increasingly being adopted) often has a profound social impact on patients. We can use the term, but we should be careful when we do. For example, candidiasis or bacterial vaginosis, or some cases of pelvic inflammatory disease (those caused, for instance, by the organisms characteristic of bacterial vaginosis), are RTIs but not STIs. Similarly, syndromes for which we have not tested patients for an etiology (for instance, a vaginal discharge) should be cautiously approached when counseling patients.
We should use diagnostic tests whenever possible. Some authorities believe that the use of syndromic management (e.g., not testing a man with urethritis for the causes of urethritis but, rather, simply treating with antimicrobials active against the major causes of urethritis) is acceptable in this country. I strongly disagree. By determining the etiology of a reproductive tract syndrome, we can (1) choose the most appropriate therapy, (2) avoid the use of “polypharmacy” and, thus, avoid excess cost and development of antimicrobial resistance, (3) give appropriate counseling, (4) better manage the patient if prescribed therapy fails and (5) determine the need for appropriate partner notification.
No diagnostic test has ideal performance characteristics (i.e., 100 percent sensitivity and specificity). While clinicians understand this, the social implications of STIs again argue for particular caution in the clinician's use of test results for counseling purposes. This is of particular concern in screening when we test patients who do not have symptoms or signs—for instance, testing young persons for chlamydial infection, pregnant women for many STIs, or even using the Papanicolaou smear to screen for infection (in cases in which the presence of an STI, such as Trichomonas vaginalis, might be detected). The lack of 100 percent specificity is particularly an issue because there will always be false-positive tests (and, thus, the concept of predictive values is vital to understand).
The proportion of all positive tests that are false-positive may be quite large if one is testing patient populations with a relatively low prevalence of infection. For example, if one is using a chlamydia test that has a 99 percent specificity (a specificity representative of nonamplification tests) to screen a population with a prevalence of infection of 2 percent (which might be representative of a population of married women), then only two thirds of all positive tests are truly positive. To tell all women with a positive test in this population that they have a chlamydial infection when, in fact, only 67 percent do, is wrong. When appropriate, we should make additional attempts to ensure the diagnosis is accurate—that is, ask the laboratory for the strength of signal (how strongly positive was the test?) or perform additional tests.
Given numerous test options, it is difficult for the clinician to know which test is the right one to use. In fact, there is no universal right test. Ideally, tests would be technically easy, would be inexpensive, would have perfect performance characteristics and would be able to be performed immediately on specimens collected with a minimum of invasiveness, but no test embodies all of these characteristics. Instead, the clinician should consider his or her needs and know the advantages and disadvantages of the test that is chosen, including the performance characteristics. Any test is only as good as the specimen that is tested; the technically best test will perform badly if specimens are poorly collected and handled.
The management of STIs includes not only choosing an antimicrobial agent but also appropriate counseling and partner notification. Many patient's lives have been dramatically altered by misinformation or good information misinterpreted (e.g., women with genital herpes who believe they can never have children, or men and women who believe that a diagnosis of human papillomavirus means never being able to have sex again). The guidelines offer valuable advice in a variety of patient management areas and should be on the desk of every family physician.2 Copies of the guidelines may be obtained on the CDC's Web site at http://www.cdc.gov, select CDC Prevention Guidelines; by calling 888-232-3228; or by writing the Office of Communications, CDC, 1600 Clifton Rd., Mailstop EO6, Atlanta, GA 30333.

