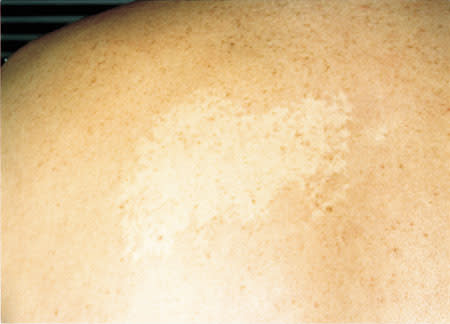
A 42-year-old man presented with a life-long history of an asymptomatic white patch on the left side of his back (see the accompanying figure). He stated that the patch was more prominent after exercise. On physical examination, a large, nonscaly, pale patch on his back was apparent. When a glass slide was applied to the border of the lesion, the border became inapparent.
Question
Given the patient's history and results of a physical examination, which one of the following is the correct diagnosis for the disorder shown above?
A. Hansen's disease.
B. Nevus anemicus.
C. Nevus depigmentosus.
D. Tinea versicolor.
E. Vitiligo.
Discussion
The answer is B: nevus anemicus. Nevus anemicus is a congenital patch manifested by skin pallor. It most commonly occurs as a single patch on the trunk. Several studies have shown that nevus anemicus is caused by a localized vascular hypersensitivity to catecholamines. This catecholamine sensitivity produces increased vasoconstriction and skin pallor. When pressure is applied to the border of the patch with a clear glass slide (i.e., diascopy), the border between lesion and normal skin disappears, because the normal skin becomes blanched. Since the histopathology of nevus anemicus is normal, nevus anemicus is a pharmacologic nevus and not an anatomic one.1,2 No treatment is available.
The differential diagnosis of nevus anemicus includes Hansen's disease, nevus depigmentosus, tinea versicolor and vitiligo. Hansen's disease is a skin infection that is caused by Mycobacterium leprae. It can manifest as hypopigmented patches and plaques. Involvement of the nerves usually causes anesthesia or hypesthesia. Histopathology would help differentiate Hansen's disease from the other hypomelanotic dermatoses. Nevus depigmentosus is an uncommon, congenital dermatosis that manifests as unilateral, hypopigmented patches in a somewhat dermatomal pattern. It appears to be caused by a block of transfer of melanosomes from melanocytes to keratinocytes. Because this is an anatomic nevus, diascopy would not obliterate the border between lesion and normal skin. Tinea versicolor, a superficial mycotic skin infection caused by Pityrosporum orbiculare, manifests as finely scaling, hypopigmented-to-erythematous patches, usually on the trunk. A potassium hydroxide preparation would reveal spores and hyphae. Persistent hypopigmentation, even after treatment with antifungal agents, is often present. This hypopigmentation is thought to result from the inhibition of tyrosinase by azelaic acid, a dicarboxylic acid, which is formed by Pityrosporum orbiculare.3 Vitiligo manifests as depigmented patches. It is a relatively common skin disease with an incidence of 1 to 2 percent. About one third of patients have a family history positive for vitiligo. Thyroid disease is the most common systemic association, occurring in 30 to 40 percent of patients with vitiligo.3 Histology shows absence of melanocytes in the epidermis. The treatment of choice is psoralens and ultraviolet A (PUVA). For localized disease, topical glucocorticoids may be useful.

