A 52-year-old house painter with a history of hypertension, chronic obstructive pulmonary disorder (70-pack-per-year smoking history) and alcoholism presented for his annual physical examination complaining of a three-month history of bilateral knee pain, which was exacerbated when climbing and descending stairs. On examination, the knees were found to be diffusely tender to palpation, swollen and warm to the touch. Crepitus with movement was noted, but the knees had full range of motion. A bilateral clubbing of the fingers was also noted, which the patient said had been present for about one year. The patient had no other symptoms. Bilateral knee radiographs were obtained and read as “bilateral periosteal reactions along the distal shaft of the femoral and proximal tibia.”
FIGURE 1.
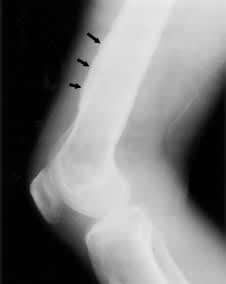
Knee radiograph showing periosteal reaction with new bone formation at distal femur (arrows).
Question
Which one of the following steps is indicated to diagnose this condition, given the unusual finding of the knee radiograph (see Figure 1), the patient's history and the results of the physical examination?
A. Aspirate joint fluid and send for culture.
B. No need to culture fluid; initiate empiric antibiotics effective against staphylococci, streptococci and gram-negative organisms.
C. Refer the patient for physical therapy.
D. Obtain a chest radiograph.
E. Obtain blood specimen to determine rheumatoid factor.
Discussion
The answer is D: obtain a chest radiograph (Figure 2). The clinical findings suggest hypertrophic osteoarthropathy, which is a syndrome characterized by digital clubbing, abnormal deposition of periosteal bone, arthralgias and synovitis. In adults, hypertrophic osteoarthropathy is typically seen in patients with a pulmonary neoplasm. It is occasionally seen with other lung diseases and in familial cases.
FIGURE 2.
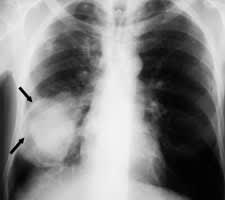
Chest radiograph showing large tumor mass in right lower lung field (arrows).
Clubbing is commonly found in a secondary form in adult patients. Although the pathogenesis is unknown, it is associated with pulmonary conditions, cyanotic cardiac diseases and disorders of the gastrointestinal tract, such as cirrhosis, hepatic carcinoma and inflammatory bowel disease.1 Clubbing is almost always present in hypertrophic osteoarthropathy and is typically asymptomatic. It generally evolves over months and often is first noted by the physician. Clubbing is characterized by paronychial soft tissue swelling associated with the loss of the normal angle between the nail and the soft tissue of the nail bed. Softening of the nail bed leads to a rocking sensation on palpation. Increased convexity of the nail and widening of the fingertips are also present. In most cases of hypertrophic osteoarthropathy, clubbing is the only external manifestation.2
Abnormal deposition of periosteal bone is first noted as subperiosteal edema with resultant periosteal elevation. Later, subperiosteal new bone forms along the long bone shafts primarily at the distal ends. Progression is symmetric and proximal. Periostosis most commonly occurs near the metacarpophalangeal, metatarsophalangeal, wrist, ankle and knee joints. It can be asymptomatic, but more commonly patients complain of a deep-seated burning or aching pain, particularly incapacitating in the lower extremities. The pain is aggravated by recumbency and generally relieved by elevation of the affected extremity. In the areas of new bone formation, tenderness on palpation is usually noted. On the radiograph, periosteal thickening is seen and periosteal elevation appears as a continuous, thin, sclerotic line of new bone along the long bone shaft.2
When hypertrophic osteoarthropathy is suspected, a search for an underlying pulmonary neoplasm must be initiated. This process should begin with a chest radiograph. Hypertrophic osteoarthropathy occurs in 5 to 10 percent of patients with intrathoracic malignancies; of these, bronchogenic carcinoma is the most common.2 It is the presenting symptom in 1 percent of non-small–cell lung cancers.1
In this patient, the chest radiograph revealed a mass measuring 8 cm × 10 cm in the right lung. Computed tomographic (CT)-guided transthoracic biopsy was performed the next day, and pathologic evaluation revealed non-small–cell carcinoma. CT scan of the head and abdomen was also performed and revealed metastases to the brain (parietal region) and the adrenals. Palliative radiation therapy was initiated.

