
Am Fam Physician. 2000;61(2):391-393
See related patient information handout on diaper rash, written by the author of this article.
Perianal streptococcal dermatitis is a bright red, sharply demarcated rash that is caused by group A beta-hemolytic streptococci. Symptoms include perianal rash, itching and rectal pain; blood-streaked stools may also be seen in one third of patients. It primarily occurs in children between six months and 10 years of age and is often misdiagnosed and treated inappropriately. A rapid streptococcal test of suspicious areas can confirm the diagnosis. Routine skin culture is an alternative diagnostic aid. Treatment with amoxicillin or penicillin is effective. Follow-up is necessary, because recurrences are common.
Perianal streptococcal cellulitis in children was first described in 1966.1 Symptoms may last from three weeks to six months. Patients are frequently misdiagnosed.2 Initial treatment regimens that delay effective treatment include topical antifungal agents, topical steroids and oral preparations for pinworms. This case report is written to remind family physicians about the existence of this disorder. Early recognition, diagnosis and treatment will greatly decrease patient discomfort and parental distress. Early antibiotic treatment results in dramatic and rapid improvement in symptoms.
Illustrative Case
A four-year-old boy presented with a complaint of rectal itching and pain. The patient was potty trained but still wore a diaper overnight. Physical examination revealed a bright red, moist rash that extended approximately 3 cm circumferentially around the perianal area. Several papules located on the peripheral area were observed, and the rash had spread onto the ventral surface of the penis. A scant mucoid discharge was present. The patient was treated for one week with a topical ointment (i.e., A&D Ointment) and baby powder, with no improvement of symptoms. A topical antifungal agent was then added to the regimen. The patient showed no improvement in symptoms after two weeks and was referred to a pediatrician for a second opinion. A clinical diagnosis of perianal streptococcal dermatitis was reached and confirmed with a rapid streptococcal (strep) screen of the perianal region. A subsequent culture grew group A beta-hemolytic streptococcus. The patient was given oral amoxicillin, and a dramatic improvement was noted within 24 hours.
Several days later, two siblings (two months and 30 months of age) of the four-year-old boy in the illustrative case developed similar symptoms. They experienced a similar, ineffective course of treatment. After physical examination and positive strep tests were performed, treatment with antibiotic therapy was initiated. Clinical improvement again was noted after 24 hours.
At the same time, a four-year-old neighbor of the three children also had diaper rash. She had been treated for several weeks by her pediatrician, who had recommended a topical antifungal agent. The rash was similar to that of the other children, and it had spread to her vulva. After hearing about the diagnosis of the neighbor children, these parents took their daughter back to their pediatrician, where a strep test revealed group A beta-hemolytic streptococcus. A similar, rapid improvement was seen following treatment with amoxicillin.
Etiology and Epidemiology
Perianal streptococcal dermatitis is caused by group A beta-hemolytic streptococci and occurs mainly in children between six months and 10 years of age.3 In one study, the incidence was reported to range from one in 218 to one in 2,000 pediatric outpatient visits.4 Signs and symptoms in this study included perianal dermatitis (90 percent), perianal itching (78 percent), rectal pain (52 percent) and blood-streaked stools (35 percent).4 Intrafamily spread was reported in 50 percent of possible cases. Communal bathing is thought to facilitate familial spread; however, the incidence of communal bathing did not reach statistical significance in this study.4
Prior therapy with topical antifungal agents, topical corticosteroids and oral preparations for pinworms fails to improve or worsens patients' symptoms.2 This type of therapy frequently leads to a delay in definitive diagnosis and treatment.
Children with streptococcal pharyngitis have a 6 percent anal carriage rate.5 It is thought that gastric acid in a healthy host eliminates most of the swallowed pharyngeal bacteria; therefore, other sources of transmission are likely. Digital contamination from an infected oropharynx or other sites of streptococcal infection (i.e., impetigo) may be the source.
Clinical Presentation
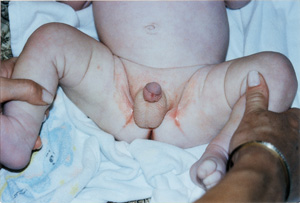
Physical examination reveals a bright red, sharply demarcated, perianal rash. Subcutaneous involvement suggestive of cellulitis is normally absent. The absence of fever and systemic signs and symptoms also supports the superficial localization of this rash.4 Spread to the penis or vulva may occur6 (Figure 1). Fissures, a mucoid discharge and yellow crusting are sometimes present.
Differential Diagnosis and Treatment
The differential diagnosis of perianal streptococcus dermatitis includes diaper dermatitis, candidiasis, psoriasis, seborrheic dermatitis, sexual abuse, pinworm infestation, local trauma from heavy wiping and inflammatory bowel disease. A rapid strep test or a culture of the perianal area may elucidate the diagnosis. Relapses have been noted in up to 39 percent of cases; thus, close follow-up is indicated.4 Repeat treatment is usually successful.
Treatment consists of amoxicillin, 40 mg per kg per day, divided into three doses, and/or topical applications of mupirocin (Bactroban) 2 percent three times per day for 10 days.3,7 Penicillin, clindamycin phosphate (Cleocin Phosphate) and erythromycin have also been used.8 Although penicillin is generally recommended for treatment of group A beta-hemolytic streptococci infection, amoxicillin is often better tolerated in the pediatric population because of its better-tasting suspension.9 Early antibiotic treatment causes a dramatic and rapid improvement of symptoms.