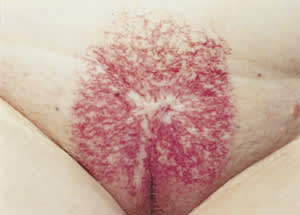
An elderly woman in her 80s was admitted for an acute myocardial infarction, from which she recovered relatively uneventfully. However, on admission it was noted that she had an unusual rash in her pubic area (see the accompanying figure). She admitted to having this discoloration for many years, but it had not caused her any other symptoms. On examination, she had a purple relatively sharply bordered rectangular “eruption” centered on the mons pubis and the vulvar cleft. Initially, the history was not revealing, but later she noted that she was treated approximately 50 years earlier for cervical cancer.
Question
Given the history and physical appearance of the rash, which one of the following conditions does this lesion represent?
A. Contact dermatitis from adult incontinence “diaper” pad.
B. Congenital hemangioma of the port-wine variety.
C. Radiation dermatitis.
D. Fixed drug eruption.
E. Atypical candidiasis.
Discussion
The answer is C: radiation dermatitis. This patient was treated many years ago with radiotherapy by external beam, possibly also by internal implantation, and subsequently developed a significant radiation dermatitis, which has healed with localized angiodysplasia and telangectasia, as well as some scarring. This condition has been relatively asymptomatic for many years and was only noted as an incidental finding. She declined any treatment for the skin discoloration.
Contact dermatitis is unlikely, because there are no vesicles and no scaling, and the skin in between the telangectasia is normal in color, not inflamed.
Congenital port-wine stain usually would be noticeable early after birth and may enlarge as the child ages. The scarring seen with this patient's lesion and its telangectatic nature differentiate it from the flat, fairly uniform appearance of port-wine stain hemangiomas.
Fixed drug eruptions can manifest as discrete purple lesions on the genitalia. These eruptions are usually uniform in color, however, and resolve shortly after removal of the causative drug.
Finally, candidiasis is less common in this age group, and one would expect more skin inflammation, perhaps fissuring, as well as satellite lesions that are round macules, not the lacey punctuation seen at the superior border of the radiation portal.
Although radiation may cause longstanding skin changes, more recently the use of multiple portals and improved equipment has made these sorts of changes uncommon. Scleroderma has been reported1 in radiation sites from breast cancer radiotherapy, and acute desquamative dermatitis with late vulvar fibrosis has been noted after radiotherapy for vulvar carcinoma.2

