The risk of ventricular arrhythmia and sudden cardiac death is increased in persons who regularly consume large amounts of alcohol (more than five drinks per day). However, the effect of light-to-moderate alcohol consumption on the risk of sudden cardiac death has not been defined. Prospective studies have found either no association or a positive association, while case-control studies have found an inverse linear association. Albert and colleagues addressed this issue by using data from the Physicians' Health Study to explore the relationship between consumption of light-to-moderate amounts of alcohol and the risk of sudden cardiac death.
In the Physicians' Health Study, 22,071 male physicians between 40 and 84 years of age with no history of myocardial infarction, stroke, transient ischemic attack or cancer were assigned to therapy with aspirin and/or beta-carotene in a randomized, double-blind, placebo-controlled trial. At the beginning of the study and 84 months later at its completion, the physicians completed a questionnaire that included, among other factors, a question concerning level of alcohol consumption. The 21,537 physicians who responded to this question were placed in seven categories based on the number of drinks consumed per unit of time, with the reference group being those who consumed less than one drink per month.
The alcohol intake of the 21,537 participants was fairly evenly distributed throughout the seven categories, with a somewhat smaller percentage of men in the category with the highest alcohol consumption. Over the 12 years of the study, 141 sudden cardiac deaths were documented in these groups. The relationship of alcohol intake and the risk of sudden cardiac death is demonstrated in the accompanying figure. A moderate alcohol intake correlated with a decrease in the incidence of sudden cardiac death, with the lowest risk in the group that reported an intake of five to six drinks per week.
FIGURE. Sudden Cardiac Death
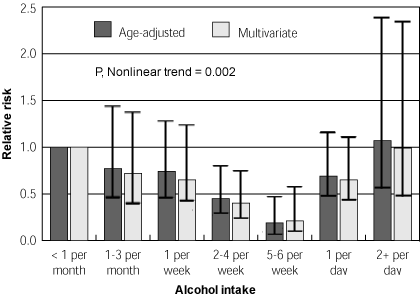
Age-adjusted, multivariate relative risk of sudden cardiac death according to level of alcohol intake. Vertical bars represent 95% CI.
*—RRs that are significantly less than 1.
Reprinted with permission from Albert CM, Manson JE, Cook NR, Ajani UA, Gaziano JM, Hennekens CH. Moderate alcohol consumption and the risk of sudden cardiac death among US male physicians. Circulation 1999;100:944–50.
This study demonstrated a significant reduction in the risk of sudden cardiac death in men who consumed a moderate amount of alcohol. However, these results are not completely in agreement with the results of earlier studies. Most prospective studies have shown no reduction in the risk of sudden cardiac death with moderate alcohol intake. The authors of this study attribute the difference in their study to the small number of sudden cardiac deaths in the other studies. Retrospective studies, on the other hand, are in agreement with the findings of these authors.
The authors postulate that the reduction in risk of sudden cardiac death in men with moderate alcohol consumption is due to the beneficial effects of alcohol on plaque rupture and thrombosis. However, in contrast to men with moderate alcohol intake, men with heavy alcohol intake (defined as more than two drinks per day) have an increased risk of sudden cardiac death. This increased risk is likely due to alcohol's arrhythmogenic properties, which at higher levels outweigh its beneficial properties.
The conclusions of this study are promising in terms of demonstrating that moderate alcohol intake decreases the risk of sudden cardiac death. Nevertheless, given the limitations of the population studied and the lack of understanding of the underlying mechanism by which alcohol may protect against sudden cardiac death, further research is necessary before any definitive recommendations about alcohol intake may be made.

