A 37-year-old woman presented for evaluation of a scar on her philtrum (see accompanying figures). She had been referred by her primary care physician for excision of this cosmetically disturbing lesion. The patient explained that she thought the scar resulted from an outbreak of herpes simplex virus infection two years before. She was concerned because the scar appeared to be slowly increasing in size. She denied tobacco use or significant sun exposure. There was no family history of dermatologic conditions, and she had no other medical problems to suggest dermatologic pathology.
On examination, a 12 × 15-mm yellow-white, firm plaque with telangiectasias was noted above her lip. A punch biopsy was performed.
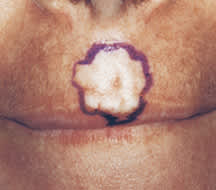
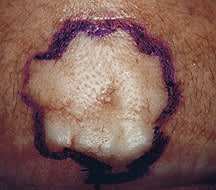
Question
Given the medical history and the physical appearance of the lesion, which one of the following is the correct diagnosis?
A. Dermatofibroma.
B. Hypertrophic scar.
C. Basal cell carcinoma.
D. Squamous cell carcinoma.
E. Sebaceous hyperplasia.
Discussion
The answer is C: basal cell carcinoma. To be more precise, histology results showed this lesion to be a morpheaform or sclerosing basal cell carcinoma.
Dermatofibromas represent a fibrous reaction to trauma. They are usually found on the lower extremities or trunk and present as pink-brown hard growths that tend to retract beneath the skin when compressed (the “dimple sign”).
A hypertrophic scar is a collection of excessively large fibrous tissue within the location of a previous wound.
Squamous cell carcinomas, like basal cell carcinomas, can be induced by ultraviolet radiation. The distribution of squamous cell carcinomas is different, however. They usually occur on the scalp, back of hands and upper pinna. Squamous cell carcinomas are generally scaly and have a red, irritated base or may present as well-circumscribed, firm, mobile indurated masses.1
Sebaceous hyperplasia can resemble basal cell carcinoma, with its yellow, umbilicated, papular appearance and occasional telangiectasias, but it differs from basal cell carcinoma on closer examination. While the vessels in basal cell carcinoma are irregularly distributed, those of sebaceous hyperplasia are usually found in a regular fashion between the yellow lobular lesions.1
Sebaceous hyperplasia presents as a smaller and more stable papule (1 to 2 mm in size), while a morpheaform basal cell carcinoma presents as a much firmer plaque that continues to grow.
Forty percent of all cancers in the United States are skin cancers, and the majority of these are basal cell and squamous cell carcinomas.2 Basal cell carcinoma is the most common cutaneous malignancy, with men having a higher incidence.1 Although basal cell carcinoma can occur anywhere, the most common areas of occurrence are the face, head and neck. Lesions typically occur with advancing age; persons less than 40 years of age are less commonly diagnosed with basal cell carcinoma. Additional risk factors include fair skin, a family history of basal cell carcinoma and a history of prolonged sun exposure. Exposures to chemical cocarcinogens, arsenic and ionizing radiation are also predisposing factors. Burn scars, chronic venous stasis dermatitis and ulcers are also sites that are at increased risk of developing basal cell carcinoma or squamous cell carcinoma.
The five major clinical varieties of basal cell carcinoma are noduloulcerative, pigmented, morpheaform, superficial, and fibroepithelioma of Pinkus. The most common variety, noduloulcerative, presents with central ulceration in a pearly nodule with telangiectasias. Pigmented basal cell carcinoma has a brown pigmentation within the lesion. Morpheaform basal cell carcinoma is usually seen as a firm yellow-white plaque that is flat or depressed. Telangiectasias are apparent but ulceration is not. Superficial basal cell carcinoma is found as multiple erythematous, scaly patches with pearly borders, crusting and superficial ulceration. Unlike the three previous types, this cancer primarily occurs on the trunk. Fibroepithelioma of Pinkus presents as sessile, flesh-colored lesions, which usually are found in the lumbosacral area.3
Morpheaform basal cell carcinoma often has a wide extension, and localization by inspection with the naked eye is unreliable; therefore, Mohs' micrographic surgery is the treatment of choice.1 Morpheaform basal cell carcinoma is associated with aggressive growth characteristics and a high percentage of recurrence.4 Although metastatic basal cell carcinoma is quite rare, it does occur. Deeply invasive tumors can metastasize, usually to the regional lymph nodes, but also to the lungs, bone and skin. Once metastasis has occurred, life expectancy is significantly reduced.5 Mohs' surgery has been the standard to eliminate aggressive basal cell carcinoma, such as the morpheaform variety. Because extensive tissue loss can occur, tissue-sparing treatment such as intralesional injection of interferon has been tried. Unfortunately, the majority of aggressive basal cell carcinomas have not been cured by interferon administration.6

