Herpes zoster (commonly referred to as “shingles”) and postherpetic neuralgia result from reactivation of the varicella-zoster virus acquired during the primary varicella infection, or chickenpox. Whereas varicella is generally a disease of childhood, herpes zoster and post-herpetic neuralgia become more common with increasing age. Factors that decrease immune function, such as human immunodeficiency virus infection, chemotherapy, malignancies and chronic corticosteroid use, may also increase the risk of developing herpes zoster. Reactivation of latent varicella-zoster virus from dorsal root ganglia is responsible for the classic dermatomal rash and pain that occur with herpes zoster. Burning pain typically precedes the rash by several days and can persist for several months after the rash resolves. With postherpetic neuralgia, a complication of herpes zoster, pain may persist well after resolution of the rash and can be highly debilitating. Herpes zoster is usually treated with orally administered acyclovir. Other antiviral medications include famciclovir and valacyclovir. The antiviral medications are most effective when started within 72 hours after the onset of the rash. The addition of an orally administered corticosteroid can provide modest benefits in reducing the pain of herpes zoster and the incidence of postherpetic neuralgia. Ocular involvement in herpes zoster can lead to rare but serious complications and generally merits referral to an ophthalmologist. Patients with postherpetic neuralgia may require narcotics for adequate pain control. Tricyclic antidepressants or anticonvulsants, often given in low dosages, may help to control neuropathic pain. Capsaicin, lidocaine patches and nerve blocks can also be used in selected patients.
Herpes zoster results from reactivation of the varicella-zoster virus. Unlike varicella (chickenpox), herpes zoster is a sporadic disease with an estimated lifetime incidence of 10 to 20 percent. The incidence of herpes zoster increases sharply with advancing age, roughly doubling in each decade past the age of 50 years. Herpes zoster is uncommon in persons less than 15 years old. In a recent study,1 patients more than 55 years of age accounted for more than 30 percent of herpes zoster cases despite representing only 8 percent of the study population. In this same study, children less than 14 years old represented only 5 percent of herpes zoster cases.
The normal age-related decrease in cell-mediated immunity is thought to account for the increased incidence of varicella-zoster virus reactivation. Patients with disease states that affect cell-mediated immunity, such as human immunodeficiency virus (HIV) infection and certain malignancies, are also at increased risk. Chronic corticosteroid use, chemotherapy and radiation therapy may increase the risk of developing herpes zoster.
The incidence of herpes zoster is up to 15 times higher in HIV-infected patients than in uninfected persons, and as many as 25 percent of patients with Hodgkin's lymphoma develop herpes zoster.2,3 The occurrence of herpes zoster in HIV-infected patients does not appear to increase the risk of acquired immunodeficiency syndrome (AIDS) and is less dependent on the CD4 count than AIDS-related opportunistic infections.2 There is no evidence that herpes zoster heralds the onset of an underlying malignancy.3
Race may influence susceptibility to herpes zoster. Blacks are one fourth as likely as whites to develop this condition.4 Although herpes zoster is not as contagious as the primary varicella infection, persons with reactivated infection can transmit varicella-zoster virus to nonimmune contacts. Household transmission rates have been noted to be approximately 15 percent.5
About 20 percent of patients with herpes zoster develop postherpetic neuralgia. The most established risk factor is age; this complication occurs nearly 15 times more often in patients more than 50 years of age. Other possible risk factors for the development of post-herpetic neuralgia are ophthalmic zoster, a history of prodromal pain before the appearance of skin lesions and an immunocompromised state.6
Pathophysiology
Varicella-zoster virus is a highly contagious DNA virus. Varicella represents the primary infection in the nonimmune or incompletely immune person. During the primary infection, the virus gains entry into the sensory dorsal root ganglia. How the virus enters the sensory dorsal root ganglia and whether it resides in neurons or supporting cells are not completely understood. The varicella-zoster virus genome has been identified in the trigeminal ganglia of nearly all seropositive patients.7
The virus remains latent for decades because of varicella-zoster virus–specific cell-mediated immunity acquired during the primary infection, as well as endogenous and exogenous boosting of the immune system periodically throughout life.8 Reactivation of the virus occurs following a decrease in virus-specific cell-mediated immunity. The reactivated virus travels down the sensory nerve and is the cause for the dermatomal distribution of pain and skin lesions.
The pathophysiology of postherpetic neuralgia remains unclear. However, pathologic studies have demonstrated damage to the sensory nerves, the sensory dorsal root ganglia and the dorsal horns of the spinal cord in patients with this condition.9
Clinical Presentation
Herpes zoster typically presents with a prodrome consisting of hyperesthesia, paresthesias, burning dysesthesias or pruritus along the affected dermatome(s). The prodrome generally lasts one to two days but may precede the appearance of skin lesions by up to three weeks.
During the prodromal phase, herpes zoster may be misdiagnosed as cardiac disease, pleurisy, a herniated nucleus pulposus or various gastrointestinal or gynecologic disorders. Some patients may have prodromal symptoms without developing the characteristic rash. This situation, known as “zoster sine herpete,” may further complicate the eventual diagnosis.
The prodromal phase is followed by development of the characteristic skin lesions of herpes zoster. The skin lesions begin as a maculopapular rash that follows a dermatomal distribution, commonly referred to as a “belt-like pattern.” The maculopapular rash evolves into vesicles with an erythematous base (Figure 1). The vesicles are generally painful, and their development is often associated with the occurrence of anxiety and flu-like symptoms.
FIGURE 1.
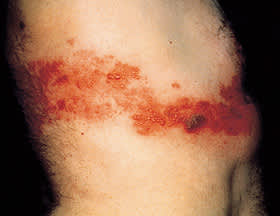
Typical dermatomal rash with hemorrhagic vesicles on the trunk of a patient with herpes zoster.
Pain is the most common complaint for which patients with herpes zoster seek medical care. The pain may be described as “burning” or “stinging” and is generally unrelenting. Indeed, patients may have insomnia because of the pain.10 Although any vertebral dermatome may be involved, T5 and T6 are most commonly affected. The most frequently involved cranial nerve dermatome is the ophthalmic division of the trigeminal nerve. Twenty or more lesions outside the affected dermatome reflect generalized viremia. Of these patients, approximately one half manifest other neurologic or visceral involvement, and as many as one in seven with viremia may die.
The vesicles eventually become hemorrhagic or turbid and crust over within seven to 10 days. As the crusts fall off, patients are generally left with scarring and pigmentary changes.
Ocular complications occur in approximately one half of patients with involvement of the ophthalmic division of the trigeminal nerve. These complications include mucopurulent conjunctivitis, episcleritis, keratitis and anterior uveitis. Cranial nerve palsies of the third, fourth and sixth cranial nerves may occur, affecting extraocular motility.
The most common chronic complication of herpes zoster is postherpetic neuralgia. Pain that persists for longer than one to three months after resolution of the rash is generally accepted as the sign of postherpetic neuralgia.11 Affected patients usually report constant burning, lancinating pain that may be radicular in nature. Patients may also complain of pain in response to non-noxious stimuli. Even the slightest pressure from clothing, bedsheets or wind may elicit pain.
Postherpetic neuralgia is generally a self-limited disease. Symptoms tend to abate over time. Less than one quarter of patients still experience pain at six months after the herpes zoster eruption, and fewer than one in 20 has pain at one year.
Treatment of Herpes Zoster
The treatment of herpes zoster has three major objectives: (1) treatment of the acute viral infection, (2) treatment of the acute pain associated with herpes zoster and (3) prevention of postherpetic neuralgia. Antiviral agents, oral corticosteroids and adjunctive individualized pain-management modalities are used to achieve these objectives.
ANTIVIRAL AGENTS
Antiviral agents have been shown to decrease the duration of herpes zoster rash and the severity of pain associated with the rash.12 However, these benefits have only been demonstrated in patients who received antiviral agents within 72 hours after the onset of rash. Antiviral agents may be beneficial as long as new lesions are actively being formed, but they are unlikely to be helpful after lesions have crusted.
The effectiveness of antiviral agents in preventing postherpetic neuralgia is more controversial. Numerous studies evaluating this issue have been conducted, but the results have been variable. Based on the findings of multiple studies, acylovir (Zovirax) therapy appears to produce a moderate reduction in the development of postherpetic neuralgia.13 Other antiviral agents, specifically valacyclovir (Valtrex) and famciclovir (Famvir), appear to be at least as effective as acyclovir.
Acyclovir, the prototype antiviral drug, is a DNA polymerase inhibitor. Acyclovir may be given orally or intravenously. Major drawbacks of orally administered acyclovir include its lower bioavailability compared with other agents and its dosing frequency (five times daily). Intravenously administered acyclovir is generally used only in patients who are severely immunocompromised or who are unable to take medications orally.
Valacyclovir, a prodrug of acyclovir, is administered three times daily. Compared with acyclovir, valacyclovir may be slightly better at decreasing the severity of pain associated with herpes zoster, as well as the duration of postherpetic neuralgia.14 Valacyclovir is also more bioavailable than acyclovir, and oral administration produces blood drug levels comparable to the intravenous administration of acyclovir.
Famciclovir is also a DNA polymerase inhibitor. The advantages of famciclovir are its dosing schedule (three times daily), its longer intracellular half-life compared with acyclovir and its better bioavailability compared with acyclovir and valacyclovir.
The choice of which antiviral agent to use is individualized. Dosing schedule and cost may be considerations. The recommended dosages for acyclovir, famciclovir and valacyclovir are provided in Table 1. All three antiviral agents are generally well tolerated. The most common adverse effects are nausea, headache, vomiting, dizziness and abdominal pain.
TABLE 1 Treatment Options for Herpes Zoster
| Medication | Dosage | Average cost (generic)* |
|---|---|---|
| Acyclovir (Zovirax)† | 800 mg orally five times daily for 7 to 10 days 10 mg per kg IV every 8 hours for 7 to 10 days‡ | $174 to 248 (129 to 200) |
| Famciclovir (Famvir)† | 500 mg orally three times daily for 7 days | 140 |
| Valacyclovir (Valtrex)† | 1,000 mg orally three times daily for 7 days | 84 |
| Prednisone (Deltasone) | 30 mg orally twice daily on days 1 through 7; then 15 mg twice daily on days 8 through 14; then 7.5 mg twice daily on days 15 through 21 | 2 (2 to 4) for days 1 through 7 2 (1 to 3) for days 8 through 14 1 (1 to 2) for days 15 to 21 |
IV = intravenously.
*—Estimated cost to the pharmacist based on average wholesale prices (rounded to the nearest dollar), for seven days of therapy, in Red book. Montvale, N.J.: Medical Economics Data, 2000. Cost to the patient will be higher, depending on prescription filling fee.
†—Antiviral therapy has been shown to be beneficial only when patients are treated within 72 hours of onset of the herpes zoster rash. Antiviral agents are not used in combination, and selection of an agent is based on dosage schedule and cost.
‡—Acyclovir can be administered IV to severely immunocompromised patients or patients who are unable to take medications orally.
CORTICOSTEROIDS
Orally administered corticosteroids are commonly used in the treatment of herpes zoster, even though clinical trials have shown variable results. Prednisone used in conjunction with acyclovir has been shown to reduce the pain associated with herpes zoster.15 The likely mechanism involves decreasing the degree of neuritis caused by active infection and, possibly, decreasing residual damage to affected nerves.
Some studies designed to evaluate the effectiveness of prednisone therapy in preventing postherpetic neuralgia have shown decreased pain at three and 12 months.16,17 Other studies have demonstrated no benefit.15,18
If the use of orally administered prednisone is not contraindicated, adjunctive treatment with this agent is justified on the basis of its effects in reducing pain, despite questionable evidence for its benefits in decreasing the incidence of postherpetic neuralgia. Given the theoretic risk of immunosuppression with corticosteroids, some investigators believe that these agents should be used only in patients more than 50 years of age because they are at greater risk of developing postherpetic neuralgia.15 The recommended dosage for prednisone is given in Table 1.
ANALGESICS
The pain associated with herpes zoster ranges from mild to excruciating. Patients with mild to moderate pain may respond to over-the-counter analgesics. Patients with more severe pain may require the addition of a narcotic medication. When analgesics are used, with or without a narcotic, a regular dosing schedule results in better pain control and less anxiety than “as-needed” dosing.
Lotions containing calamine (e.g., Caladryl) may be used on open lesions to reduce pain and pruritus. Once the lesions have crusted over, capsaicin cream (Zostrix) may be applied. Topically administered lidocaine (Xylocaine) and nerve blocks have also been reported to be effective in reducing pain.
OCULAR INVOLVEMENT
Ocular herpes zoster is treated with orally administered antiviral agents and corticosteroids, the same as involvement elsewhere. Although most patients with ocular herpes zoster improve without lasting sequelae, some may develop severe complications, including loss of vision. When herpes zoster involves the eyes, ophthalmologic consultation is usually recommended.
PREVENTIVE TREATMENT
The morbidity and mortality of herpes zoster could be reduced if a safe and effective preventive treatment were available. It is unusual for a patient to develop herpes zoster more than once, suggesting that the first reactivation of varicella-zoster virus usually provides future immunologic protection. Studies are currently being conducted to evaluate the efficacy of the varicella-zoster vaccine in preventing or modifying herpes zoster in the elderly.
Treatment of Postherpetic Neuralgia
Although postherpetic neuralgia is generally a self-limited condition, it can last indefinitely. Treatment is directed at pain control while waiting for the condition to resolve. Pain therapy may include multiple interventions, such as topical medications, over-the-counter analgesics, tricyclic antidepressants, anticonvulsants and a number of nonmedical modalities. Occasionally, narcotics may be required. Dosage recommendations are provided in Table 2.
TABLE 2 Treatment Options for Postherpetic Neuralgia*
| Medication | Dosage |
|---|---|
| Topical agents | |
| Capsaicin cream (Zostrix) | Apply to affected area three to five times daily. |
| Lidocaine (Xylocaine) patch | Apply to affected area every 4 to 12 hours as needed. |
| Tricyclic antidepressants | |
| Amitriptyline (Elavil) | 10 to 25 mg orally at bedtime; increase dosage by 25 mg every 2 to 4 weeks until response is adequate, or to maximum dosage of 150 mg per day. |
| Nortriptyline (Pamelor) | 10 to 25 mg orally at bedtime; increase dosage by 25 mg every 2 to 4 weeks until response is adequate, or to maximum dosage of 125 mg per day. |
| Imipramine (Tofranil) | 25 mg orally at bedtime; increase dosage by 25 mg every 2 to 4 weeks until response is adequate, or to maximum dosage of 150 mg per day. |
| Desipramine (Norpramin) | 25 mg orally at bedtime; increase dosage by 25 mg every 2 to 4 weeks until response is adequate, or to maximum dosage of 150 mg per day. |
| Anticonvulsants | |
| Phenytoin (Dilantin) | 100 to 300 mg orally at bedtime; increase dosage until response is adequate or blood drug level is 10 to 20 μg per mL (40 to 80 μmol per L). |
| Carbamazepine (Tegretol) | 100 mg orally at bedtime; increase dosage by 100 mg every 3 days until dosage is 200 mg three times daily, response is adequate or blood drug level is 6 to12 μg per mL (25.4 to 50.8 μmol per L). |
| Gabapentin (Neurontin) | 100 to 300 mg orally at bedtime; increase dosage by 100 to 300 mg every 3 days until dosage is 300 to 900 mg three times daily or response is adequate. (Drug levels for clinical use are not available.) |
*—Additional modalities include transcutaneous electric nerve stimulation (TENS), biofeedback and nerve blocks.
ANALGESICS
Capsaicin, an extract from hot chili peppers, is currently the only drug labeled by the U.S. Food and Drug Administration for the treatment of postherpetic neuralgia.19 Trials have shown this drug to be more efficacious than placebo but not necessarily more so than other conventional treatments.20
Substance P, a neuropeptide released from pain fibers in response to trauma, is also released when capsaicin is applied to the skin, producing a burning sensation. Analgesia occurs when substance P is depleted from the nerve fibers. To achieve this response, capsaicin cream must be applied to the affected area three to five times daily. Patients must be counseled about the need to apply capsaicin regularly for continued benefit. They also need to be counseled that their pain will likely increase during the first few days to a week after capsaicin therapy is initiated. Patients should wash their hands thoroughly after applying capsaicin cream in order to prevent inadvertent contact with other areas.
Patches containing lidocaine have also been used to treat postherpetic neuralgia. One study found that compared with no treatment, lidocaine patches reduced pain intensity, with minimal systemic absorption. Although lidocaine was efficacious in relieving pain, the effect was temporary, lasting only four to 12 hours with each application.21
Over-the-counter analgesics such as acetaminophen (e.g., Tylenol) and nonsteroidal anti-inflammatory drugs have not been shown to be highly effective in the treatment of post-herpetic neuralgia. However, these agents are often useful for potentiating the pain-relieving effects of narcotics in patients with severe pain. Because of the addictive properties of narcotics, their chronic use is discouraged except in the rare patient who does not adequately respond to other modalities.
TRICYCLIC ANTIDEPRESSANTS
Tricyclic antidepressants can be effective adjuncts in reducing the neuropathic pain of postherpetic neuralgia. These agents most likely lessen pain by inhibiting the reuptake of serotonin and norepinephrine neurotransmitters.22
Tricyclic antidepressants commonly used in the treatment of postherpetic neuralgia include amitriptyline (Elavil), nortriptyline (Pamelor), imipramine (Tofranil) and desipramine (Norpramin). These drugs are best tolerated when they are started in a low dosage and given at bedtime. The dosage is increased every two to four weeks to achieve an effective dose.
The tricyclic antidepressants share common side effects, such as sedation, dry mouth, postural hypotension, blurred vision and urinary retention. Nortriptyline and amitriptyline appear to have equal efficacy; however, nortriptyline tends to produce fewer anticholinergic effects and is therefore better tolerated. Treatment with tricyclic antidepressants can occasionally lead to cardiac conduction abnormalities or liver toxicity. The potential for these problems should be considered in elderly patients and patients with cardiac or liver disease.
Because tricyclic antidepressants do not act quickly, a clinical trial of at least three months is required to judge a patient's response. The onset of pain relief using tricyclic antidepressants may be enhanced by beginning treatment early in the course of herpes zoster infection in conjunction with antiviral medications.20
ANTICONVULSANTS
Phenytoin (Dilantin), carbamazepine (Tegretol) and gabapentin (Neurontin) are often used to control neuropathic pain. A recent double-blind, placebo-controlled study showed gabapentin to be effective in treating the pain of postherpetic neuralgia, as well as the often associated sleep disturbance.23
The anticonvulsants appear to be equally effective, and drug selection often involves trial and error. Lack of response to one of these medications does not necessarily portend a poor response to another. The dosages required for analgesia are often lower than those used in the treatment of epilepsy.
Anticonvulsants are associated with a variety of side effects, including sedation, memory disturbances, electrolyte abnormalities, liver toxicity and thrombocytopenia. Side effects may be reduced or eliminated by initiating treatment in a low dosage, which can then be slowly titrated upward.
There are no specific contraindications to using anticonvulsants in combination with antidepressants or analgesics. However, the risk of side effects increases when multiple medications are used.
Effective treatment of postherpetic neuralgia often requires multiple treatment approaches. In addition to medications, modalities to consider include transcutaneous electric nerve stimulation (TENS), biofeedback and nerve blocks.
Final Comment
Herpes zoster and postherpetic neuralgia are relatively common conditions, primarily in elderly and immunocompromised patients. Although the diagnosis of the conditions is generally straightforward, treatment can be frustrating for the patient and physician. Approaches to management include treatment of the herpes zoster infection and associated pain, prevention of postherpetic neuralgia, and control of the neuropathic pain until the condition resolves. Primary treatment modalities include antiviral agents, corticosteroids, tricyclic antidepressants and anticonvulsants.

