Infection with Helicobacter pylori can cause chronic gastritis and lead to peptic ulcer disease. The infection is usually acquired during childhood and, if eradicated, is believed to rarely recur during adult life. Therefore, adequate therapy for patients with H. pylori is important in the treatment and prevention of peptic ulcers. Many treatments have been recommended for eradication of H. pylori, and the situation has been complicated by differences in study methodology and the emergence of antibiotic resistance. A review by de Boer and Tytgat clarifies and updates recommendations for treatment of patients with H. pylori infection.
Eradication of H. pylori is indicated in patients with proven peptic ulcers. The benefits to other H. pylori–positive, dyspeptic patients are currently unclear. In populations with a high incidence of ulcer disease, the authors recommend antibiotic treatment for all H. pylori-positive, dyspeptic patients. The two main antibiotics used are metronidazole and clarithromycin. Antibiotic resistance against these two medications is clinically important; both appear to be equally effective.
Good clinical evidence of efficacy has been provided for several triple or quadruple antibiotic therapies. These therapies are associated with cure rates of 80 to 90 percent based on intention to treat or completion of therapy, respectively. Therapies combining only a proton pump inhibitor and amoxicillin or clarithromycin are no longer regarded as effective. Several treatment regimens have been shown to be effective, but no single treatment regimen is considered the final treatment of choice (see the accompanying table).
Triple regimens consist of metronidazole, tetracycline or amoxicillin, and a bismuth compound. These regimens are cost effective but may cause side effects. In metronidazole-sensitive strains, high cure rates are obtained after seven days, but 14 days of therapy are recommended to optimize eradication. Although side effects are common, they are not generally severe and have not led to noncompliance in clinical trials. More recent triple therapies have replaced bismuth with a proton pump inhibitor and reduced the treatment period to seven days. The optimal regimen for sensitive strains may be a twice-daily dosage of 20 mg of omeprazole (or equivalent), 1,000 mg of amoxicillin and 500 mg of clarithromycin. Some regimens substitute metronidazole for clarithromycin. In areas with a high prevalence of resistant strains, therapy should continue for 10 to 14 days. An alternative triple therapy replaces the proton pump inhibitor with ranitidine bismuth citrate. Although providing less acid suppression, these regimens add the antimicrobial action of bismuth (see the accompanying figure).
FIGURE. Treatment Strategy
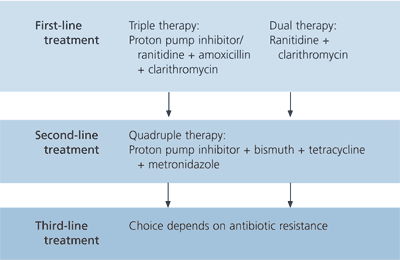
Recommended treatment strategy in areas with low primary prevalence of clarithromycin resistance.
Reprinted with permission from de Boer WA, Tytgat GN. Treatment of Helicobacter pylori infection. BMJ 2000;320:31–4.
Quadruple regimens add proton pump inhibitors to bismuth triple regimens. The most effective quadruple regimens include tetracycline and metronidazole and are the most complicated to follow. In metronidazole-sensitive strains, cure rates may be high after four days, but at least seven days of treatment are recommended.
No ideal second-line treatment has been established if the initial therapy fails to eradicate the organism. Quadruple therapy has been successful after failure of regimens containing clarithromycin; results after regimens containing metronidazole were disappointing.

