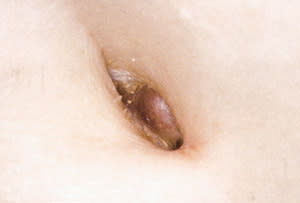
An 84-year-old woman presented for evaluation of various benign skin lesions and was incidentally noted to have an 8-mm violaceous nodule in the umbilicus (Figure 1). The patient's medical history was significant only for prior cholecystectomy, total hysterectomy and oophorectomy.
FIGURE 1.
Question
Given the results of the physical examination and the history, which one of the following is the most appropriate management of the lesion pictured?
A. Cryotherapy with liquid nitrogen.
B. Testing for human immunodeficiency virus.
C. Reassurance that this represents a benign lesion.
D. Fine-needle aspiration or tissue biopsy.
E. Incision and drainage of lesion.
Discussion
The answer is D: fine-needle aspiration or tissue biopsy. Sister Joseph's nodule is a lymphatic metastasis to the umbilical region. The differential diagnosis of an umbilical nodule includes, but is not limited to, granuloma (pyogenic, foreign body), urachal duct cyst, endometrioma, keloid, hernia and epithelial inclusion cyst.
Given the patient's age, a malignancy was the primary concern. The physical examination was nonfocal for a source of metastatic disease. A punch biopsy of the lesion was performed and revealed a poorly differentiated adenocarcinoma in the superficial and deep dermis. Computed tomography (CT) of the chest, abdomen and pelvis (Figure 2) showed diffuse caking of the omentum with tumor metastases and extension of the tumor into the periumbilical region. Additionally, the CT scan revealed two hypodense areas in the liver and a 15-mm nodule in the lower lobe of the right lung, suspicious for metastatic disease. The patient had no history of breast cancer, and mammography showed no evidence of breast carcinoma as a primary site for her metastatic disease. Upper endoscopy and colonoscopy were negative, and the patient's carcinoembryonic antigen level was measured as 1.1 ng per mL (normal range, 1 to 3 ng per mL). Further testing with immunohistochemical and receptor stains was inconclusive. No primary tumor was ever identified.
FIGURE 2.
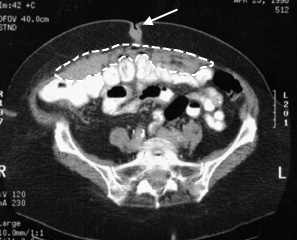
Computed tomographic scan. Note the caking of the omentum (dashed outline) and tumor metastases and extension into the periumbilical region (arrow).
Sister Joseph (1856–1939), superintendent of St. Mary's Hospital, was credited with making the observation of lymphatic metastases to the umbilical region in metastatic tumors of intra-abdominal origin, hence the name “Sister Joseph's nodule.”1 Indeed, the primary tumor in most cases of Sister Joseph's nodule is intra-abdominal: stomach, large and small intestine, pancreas, kidney, uterus, ovary or gallbladder.2–4 Additionally, there are rare reports of primary tumors outside the abdominal cavity with metastasis to the umbilicus, including breast, lung and penis.2 In an estimated 9 to 17 percent of cases, the primary tumor is never found.2,4 In summary, Sister Joseph's nodule is a rare but important clinical finding. Although generally a poor prognostic sign, long-term survival may be possible if the nodule represents a solitary metastasis.2,4,5

