What is sickle cell disease?
Sickle cell disease is a blood disease that children inherit from their parents. The disease causes the red blood cells to make abnormal hemoglobin. Hemoglobin is the part of blood that carries oxygen in the body.
There are different kinds of sickle cell disease. Some kinds are mild, but others cause serious illness.
Who gets sickle cell disease, and how?
Sickle cell disease is most common in people whose ancestors came from Africa, Central America (especially Panama), South America, Caribbean nations, Mediterranean countries, India or Near Eastern countries.
To get sickle cell disease, a child has to inherit the sickle hemoglobin gene from one parent and a sickle gene or another abnormal hemoglobin gene from the other parent.
People with one normal gene and one sickle gene are carriers of the abnormal gene. They have sickle cell trait, but they do not have sickle cell disease. If both parents have sickle cell trait, their child has a 25 percent chance of getting sickle cell disease.
Sometimes one parent has sickle cell trait and the other parent has a gene for another kind of abnormal hemoglobin. This means that their child has a chance of getting a variant kind of sickle cell disease.
Genes are tiny pieces of DNA; they are like pieces of a jigsaw puzzle. When all your genes are put together, they make you.
What happens to red blood cells in sickle cell disease, and what problems can this cause?
When the red blood cells of people with sickle cell disease don't get enough oxygen, shape. They become longer and curved. Some people think they look like the blade of a cutting tool called a “sickle.” Picture 1 shows normal red blood cells, and picture 2 shows sickle cells.
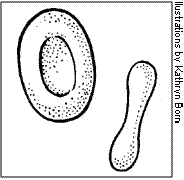
PICTURE 1. Normal red blood cells.

PICTURE 2. Sickle cells.
Sickle cells can get stuck in blood vessels and keep blood from reaching parts of the body. This causes pain and can damage the body's internal organs. Blocked blood vessels in the arms, legs, chest or abdomen can cause strong pain. Children with sickle cell disease might get more infections because their spleen is damaged by sickle cells. One of the spleen's main jobs is to protect against infection. When sickle cells block blood flow to organs and cause pain and other problems, this is called a “sickle cell crisis,” or a “pain crisis.”
How can my doctor tell if my baby has sickle cell disease?
If you are in a risk group, you should ask your doctor to check you and your sexual partner for sickle cell trait or disease before you get pregnant. Then you will know if you might have a child with sickle cell disease. Your doctor might want you to get genetic testing. If you are already pregnant, you might get testing for your fetus.
Most states test all newborn babies for sickle cell disease. If your state does not do this testing, your doctor can get a special blood test for your baby. This test will show if your baby has sickle cell disease.
How is sickle cell disease treated?
If your child has sickle cell disease, he or she is at risk for some infections, lung problems and pain.
Your child will need to take an antibiotic (usually penicillin) to prevent bad infections. Also, certain vitamins, like folic acid, can help your child's body replace damaged blood cells.
Your child needs to have all of the recommended shots for children. Your child will also need a few special shots.
Your child will need to see your family doctor often for blood tests and to be checked for damage to internal organs. If your child has pain, fever, weakness or trouble breathing, he or she may need intravenous fluids (liquids given through a needle placed in your child's vein) and antibiotics. Your child may also need oxygen, blood transfusions and strong pain medicines. Special treatments will be needed if your child has organ damage.
When should I call my child's doctor?
You should call your doctor right away if your child has any of these signs:
- Swollen hands or feet
- Sudden paleness of the skin or nail beds
- Yellow color of the skin or eyes
- Fever or signs of infection
- Swelling in the abdomen (tummy)
- Sudden tiredness with no interest in what is going on
- Erection of the penis that won't go away
- Trouble hearing or seeing
- Weakness on one side of the body or a sudden change in speech
- Headache
- Trouble breathing
- Joint, stomach, chest or muscle pain, or limping
Can sickle cell disease be cured?
Generally, not. But with good care, people with sickle cell disease can live a mostly normal life. Bone marrow transplants can cure the disease in a small number of people.
Where can I get more information about sickle cell disease?
For more information, you can contact:
- Sickle Cell Disease Association of America
- 200 Corporate Pointe, Suite 495
- Culver City, CA 90230-8727
- Telephone: 1-800-421-8453
- Web site: http://www.sicklecelldisease.org

