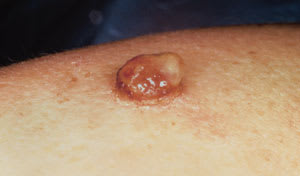
A 33-year-old woman presented with an enlarging lesion on her right arm that bled easily with any form of manipulation. She was five weeks postpartum and had initially noted the lesion three to four weeks before delivery. The patient had no previous injury to the area, no history of similar lesions and was otherwise healthy. Physical examination revealed an erythematous, friable, exophytic nodule on her right lateral arm that measured 1 cm by 1 cm (see the accompanying figure).
Question
Which one of the following is the correct diagnosis?
A. Angiokeratoma.
B. Pyogenic granuloma.
C. Bacillary angiomatosis.
D. Basal cell carcinoma.
E. Nodular melanoma.
Discussion
The correct answer is B: pyogenic granuloma. A pyogenic granuloma is a benign, usually solitary, vascular tumor that occurs most commonly in pregnant women and in children.1 Despite its name, it is neither infectious nor granulomatous.2 Some have suggested that a more appropriate term for this neoplasm would be lobular capillary hemangioma because histologically the lesion consists of lobular clusters of capillaries in a dense stroma, accompanied by an inflammatory infiltrate.3
Angiokeratomas are benign purple-red keratotic vascular papules that present in several forms. Angiokeratoma is included in the differential diagnosis of pyogenic granuloma, although these lesions are usually smaller (1 to 3 mm), slower-growing, and are often multiple.
Bacillary angiomatosis is a vascular proliferation associated with infection with Bartonella henselae, which is commonly seen in patients with acquired immunodeficiency syndrome. The lesions are often clinically indistinguishable from pyogenic granulomas, except that they more often appear in greater numbers.
Basal cell carcinoma is a tumor arising from the basal cell layer of the epidermis. It is associated with chronic sun exposure. The lesions classically have a pearly papular component. Lesions may become ulcerated but rarely grow as fast as a pyogenic granuloma.
Nodular melanomas are rare but deadly invasive melanocytic tumors. Nodular melanomas are more penetrating than superficial melanomas. The deeper the depth of penetration of malignant melanocytes, the worse the prognosis. Therefore, nodular amelanotic melanoma is the most important tumor to differentiate from pyogenic granuloma. Delay in diagnosis or lack of confirmation of the histopathologic diagnosis can be life-threatening.
The pathogenesis of pyogenic granuloma is not clear, but there is much speculation about the etiology. Local trauma or irritation has been noted in 7 to 50 percent of patients with the diagnosis.1 It has been reported as a complication of second-degree burns, with multiple pyogenic granulomas appearing in the affected area.4 A viral origin has also been hypothesized (warts and pyogenic granulomas share an affinity for the hands, forearms, soles of feet and oral cavity) but seems unlikely because the most common types of human papillomavirus have been ruled out as etiologic agents by polymerase chain reaction testing.5 Underlying arteriovenous anastomoses may be in some way related to the development of pyogenic granuloma because lesions often develop within port-wine stains.1,6
Hormonal influences (specifically progesterone) almost certainly play a role in the pathogenesis of pyogenic granuloma because these lesions commonly develop in pregnant women or in those taking oral contraceptives.1 Most frequently these “pregnancy tumors” (also called granuloma gravidarum or epulides gravidarum) appear on intraoral or perioral tissue during the second and third trimesters.1,7 Bleeding from these highly friable lesions can be a significant problem for patients, but it can usually be controlled with improved oral hygiene. Excision before delivery is not advised because the tumor is likely to recur, and some pyogenic granulomas regress spontaneously in the postpartum period.7,8
A pyogenic granuloma most often presents as a solitary, red, painless nodule or papule (with or without ulceration) on the hands or face. It usually grows rapidly over several weeks but is rarely greater than 1 cm in diameter.1 The solitary superficial type is most common, but subcutaneous, intravenous and multiple disseminated pyogenic granulomas have been reported.2,9 The diagnosis is made largely on clinical grounds, but biopsy for histopathologic confirmation before treatment of the lesion may be advisable in cases of atypical lesions without the usual rapid growth and disorganized, friable surface features. Treatment options include all of the common methods of removal or destruction (e.g., shave excision with electrodessication at base, cryotherapy, laser or electric ablation or complete surgical removal). Recurrence (or development of satellite lesions) has been reported with all therapeutic modalities but seems to be most rare with complete surgical excision.1,6,10

