
A more recent article on fibromyalgia is available.
Am Fam Physician. 2000;62(7):1575-1582
See related patient information handout on fibromyalgia, written by the authors of this article.
Fibromyalgia is an extremely common chronic condition that can be challenging to manage. Although the etiology remains unclear, characteristic alterations in the pattern of sleep and changes in neuroendocrine transmitters such as serotonin, substance P, growth hormone and cortisol suggest that dysregulation of the autonomic and neuroendocrine system appears to be the basis of the syndrome. The diagnosis is clinical and is characterized by widespread pain, tender points and, commonly, comorbid conditions such as chronic fatigue, insomnia and depression. Treatment is largely empiric, although experience and small clinical studies have proved the efficacy of low-dose antidepressant therapy and exercise. Other less well-studied measures, such as acupuncture, also appear to be helpful. Management relies heavily on the physician's supportive counseling skills and willingness to try novel strategies in refractory cases.
Fibromyalgia is a rheumatologic condition characterized by spontaneous, widespread soft tissue pain, sleep disturbance, fatigue and extensively distributed areas of tenderness known as tender points. Estimates of prevalence are 3.4 percent for women and 0.5 percent for men.1
Fibromyalgia can be perplexing to patients and physicians because of the lack of associated abnormalities on readily available diagnostic tests. Despite this, recent findings about the pathogenesis and pathophysiology of fibromyalgia have dispelled the belief that the disorder is psychosomatic. While no laboratory test can confirm fibromyalgia, most patients present with a history of widespread pain, physical findings and comorbid conditions. With experience, the disorder may be diagnosed with confidence on initial presentation or after a period of observation and minimal diagnostic testing. The family physician is ideally suited to treat fibromyalgia because its management calls for a longitudinal relationship, a willingness to try different therapeutic modalities and an understanding of the interrelationship of the biopsychosocial aspects of health.
Pathophysiology
While the cause of fibromyalgia remains elusive, substantial findings implicate disturbances in the neuroendocrine axis as central to its etiology.2 This is particularly true of the relationship between the neuroendocrine axis and sleep. The sleep electroencephalogram of patients with fibromyalgia indicates disturbance of the non-REM sleep phase by intrusions of alpha waves with infrequent progression to stage 3 and stage 4 sleep.3 These findings correlate with patient reports of awakening repeatedly and being “unrefreshed by sleep.”4
The stages of sleep have concomitant hormone release activity. For example, release of growth hormone occurs primarily during stage 3 and stage 4 of non-REM sleep. One third of patients with fibromyalgia have low insulin growth factor (IGF) levels, an indication of low growth hormone secretion. Furthermore, symptoms of fibromyalgia may be created by disturbing non-REM sleep.5
Other endocrinologic and neurologic findings in patients with fibromyalgia include:
Elevation of cerebrospinal fluid substance P levels (a neurotransmitter associated with enhanced pain perception) to three times normal levels.6
Alteration in the hypopituitary-adrenal axis with low overall production of cortisol. This contrasts with the findings in depression, where a higher-than-normal cortisol level is found.7
Provocation of symptoms during tilt table testing and a significant prevalence of neurally mediated hypotension.8
These results suggest that disturbances in the autonomic and endocrine stress response systems may underlie the etiology of fibromyalgia. How these pathophysiologic processes are set in motion is not understood; however, the prevalence of premorbid physical and psychologic trauma is high in these patients.
Diagnosis
Fibromyalgia should be considered in any patient with musculoskeletal pain that is unrelated to a clearly defined anatomic lesion. Making the diagnosis of fibromyalgia depends on findings from the history and physical examination rather than on diagnostic testing.
In 1990, the American College of Rheumatology (ACR) established criteria for classifying patients with fibromyalgia.9 However, failure to meet these criteria does not absolutely exclude the possibility of fibromyalgia.
As with other rheumatologic disorders, fibromyalgia:
Is established on the basis of clinical observations.
Is a condition with signs and symptoms that exist on a continuum.
Often requires observation over time to firmly establish the diagnosis.
History
Widespread pain is characteristic of fibromyalgia. Although not all areas may be involved simultaneously, pain may occur in the occiput, neck, shoulders, thoracic and lumbar spine, paraspinous regions, buttocks, hips, elbows and knees. A careful history will uncover additional areas of pain when the chief complaint lies in one area. It is not unusual for the most significant area of pain to shift over time.
Physical Examination
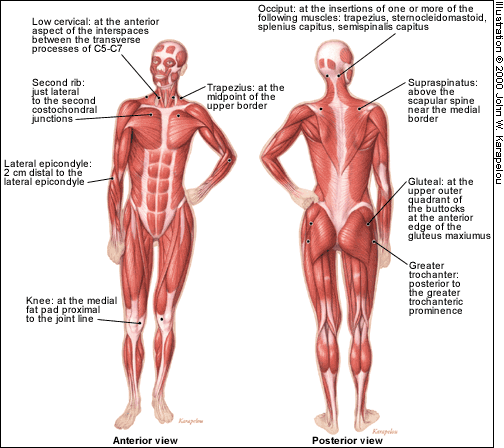
Examination will reveal areas of pain on palpation but without the classic inflammatory signs of redness, swelling and heat in the joints and soft tissue. Although tender points are found in many different locations, the ACR has selected 18 sites that are more characteristic for fibromyalgia (Figure 1). To be classified with a definitive diagnosis of fibromyalgia, the patient must have tenderness on palpation at 11 of the 18 sites and a history as defined in Table 1, although patients with fewer than 11 sites still may have fibromyalgia. The number of tender points may change over time.
| Widespread pain for at least three months, defined as the presence of all of the following: | |
| Pain on the right and left sides of the body | |
| Pain above and below the waist (including shoulder and buttock pain) | |
| Pain in the axial skeleton (cervical, thoracic or lumbar spine, or anterior chest) | |
| Pain on palpation with a 4-kg force in 11 of the following 18 sites (nine bilateral sites, for a total of 18 sites): | |
| Occiput: at the insertions of one or more of the following muscles: trapezius, sternocleidomastoid, splenius capitus, semispinalis capitus | |
| Low cervical: at the anterior aspect of the interspaces between the transverse processes of C5–C7 | |
| Trapezius: at the midpoint of the upper border | |
| Supraspinatus: above the scapular spine near the medial border | |
| Second rib: just lateral to the second costochondral junctions | |
| Lateral epicondyle: 2 cm distal to the lateral epicondyle | |
| Gluteal: at the upper outer quadrant of the buttocks at the anterior edge of the gluteus maximus muscle | |
| Greater trochanter: posterior to the greater trochanteric prominence | |
| Knee: at the medial fat pad proximal to the joint line | |
Skill in palpation of tender points is critical to establishing a diagnosis of fibromyalgia. Physical findings encountered during palpation of the soft tissues include tender points, changes in skin texture, increased resting muscle tension and changes in the texture of the subcutaneous tissue.
Differential Diagnosis
The diagnosis of fibromyalgia may be made based on the ACR criteria or based on the presence of the characteristic syndrome, or both. Clinicians familiar with fibromyalgia order a minimum of testing when cases appear straightforward. The thyroid-stimulating hormone level should be checked routinely because hypothyroidism can mimic the symptoms of fibromyalgia. Other diagnoses to consider include drug-induced myopathies (particularly those associated with the statin class of lipid-lowering agents), polymyalgia rheumatica and other rheumatologic syndromes.
Myofascial pain syndrome may be confused with fibromyalgia. To complicate the situation, myofascial pain syndrome may occur in patients with fibromyalgia. Similar to fibromyalgia, myofascial pain syndrome is a condition that is diagnosed clinically. With a careful history and physical examination, the physician should be able to determine whether a patient has fibromyalgia, myofascial pain syndrome, or both. While the pain of fibromyalgia is widespread with changing areas of emphasis, myofascial pain arises from trigger points in individual muscles. The diagnosis of myofascial pain syndrome should be considered when, by history, the patient's pain pattern is limited to a particular region over time.
The definitive differentiation between myofascial pain syndrome and fibromyalgia is made by physical examination. Myofascial pain syndrome is defined by the presence of trigger points. Unfortunately, location alone does not differentiate between trigger points and tender points because they often occur in similar locations. Distinguishing between trigger points and tender points depends on characteristic findings associated with trigger points that are found on physical examination. Trigger points are located within taut bands of muscle, whereas tender points are not. Palpation of trigger points often reproduces the pain radiation pattern experienced by the patient and can elicit a twitch in the muscle. The pain elicited on palpation of a tender point is localized to the area under palpation and does not elicit a jump or twitch. Lastly, trigger points often have a nodular texture described as similar to a pencil eraser, whereas tender points have no palpatory characteristics distinguishing them from surrounding tissue.10
Comorbid Conditions
Patients with fibromyalgia often have one or more comorbid conditions (Table 211). Along with myofascial pain syndrome, the most common of these are migraine headache, irritable bowel syndrome and a history of depression and chronic fatigue.11 Although treatment for fibromyalgia may help to alleviate the symptoms of comorbid conditions, specific treatment for these comorbidities may be indicated.
| Migraine headache |
| Chronic fatigue |
| Irritable bowel syndrome |
| Depression |
| Restless legs syndrome |
| Temporomandibular joint syndrome |
| Myofascial pain syndrome |
Treatment
Because the symptoms of fibromyalgia wax and wane, treatment (as with that of other chronic diseases) is an ongoing process rather than management of a single episode. Flare-ups often exacerbate the patient's underlying stress. Furthermore, stress can also precipitate flare-ups of fibromyalgia. Physicians should spend some time eliciting and hearing the ongoing narrative of the struggle of living with a chronic disease and attempt to ameliorate the effects of the symptoms on the patient's quality of life.
Treatment of fibromyalgia is largely empiric. Although some frequently used approaches, such as antidepressants and exercise, have evidence to support their use, others (such as acupuncture) are less well studied. None of the therapies used in fibromyalgia are based on evidence from larger randomized, double-blind, placebo-controlled trials. This void places a premium on the physician's therapeutic creativity and supportive counseling skills.
The therapeutic response to patients with relatively mild symptoms and no sleep disturbances may involve only identification of fibromyalgia to explain and legitimize their symptoms, along with encouragement to develop and maintain an active exercise program. Many patients will benefit from the use of low-dose antidepressants. Other patients may require more complicated regimens, which may include psychotherapy, medications, acupuncture, massage and physical therapy, to maintain function. Ideally, the practitioner will collaborate with the patient to construct a unique treatment plan consonant with the patient's circumstances.12 That plan will necessarily evolve within the context of the physician-patient relationship.
THERAPEUTIC MEASURES
Antidepressant Agents. Although antidepressants have a lengthy history in the treatment of chronic pain syndromes, they have received only limited study in the treatment of fibromyalgia. The tricyclic antidepressants, selective serotonin reuptake inhibitors (SSRIs), or combinations of both, produce mild to moderate improvement in symptoms. In controlled studies,1 approximately one third to one half of patients responded to pharmacologic treatment. One study13 found that while 25 mg of amitriptyline (Elavil) or 20 mg of fluoxetine (Prozac) reduced the symptoms of fibromyalgia, the combination of the two was twice as effective as either agent taken alone. The dosages used are somewhat lower than those needed to treat depression. The older agents (such as amitriptyline) can be started at a dosage of 10 mg taken daily two to three hours before bedtime. This allows the peak sedative effect to be realized while avoiding unwanted carry-over sedation on awakening. The time of administration can be adjusted depending on individual patient response.
The dosage of antidepressant must be individualized. This is particularly true of the tricyclic agents, given their variable absorption, metabolism and excretion. Dosages should be gradually increased, not to exceed the recommended maximum for the drug. Even patients who are able to tolerate very small amounts of these medications may derive benefit from them. In these instances, doxepin elixir (Sinequan) can be started at a low dose (one drop, or 0.67 mg) and slowly titrated upward.14 Fluoxetine, an SSRI, can be started at doses in the lower range and should generally be taken in the morning.
The use of cyclobenzaprine (Flexeril) is supported by evidence primarily from one randomized controlled trial that followed 120 patients.15 Clinically, its use has many adherents.
There is a note of caution when using anti-depressants to manage fibromyalgia: a significant portion of patients may find that their symptoms worsen while using these drugs. Symptoms must be monitored carefully as therapeutic blood levels are reached.16
Exercise. Aerobic and strength-training activities have been associated with significant improvements in pain, tender point counts and disturbed sleep in patients with fibromyalgia.17 Unfortunately, maintenance of exercise regimens tends to be poor in patients with fibromyalgia. Strategies for improving compliance, such as having the patient work out with a companion, can be discussed with the patient.
Acupuncture. A substantial meta-analysis of studies using acupuncture in the treatment of fibromyalgia confirms the empiric finding of medical acupuncturists that acupuncture is an extremely useful adjunctive treatment for many patients with fibromyalgia.18 While not curative, acupuncture can enhance the patient's quality of life. The frequency of acupuncture is individualized and may range from weekly visits to visits once every 10 to 12 weeks. Information about physician acupuncturists practicing in a particular area may be obtained by contacting the American Association of Medical Acupuncture, 5820 Wilshire Blvd., Ste. 500, Los Angeles, CA 90036. This information is also on their Web site at http://www.medicalacupuncture.org.
Chronic Opioid Analgesic Therapy (COAT). This intervention should be reserved for patients with moderate to severe pain or significant functional impairment and for those in whom other therapies are ineffective or contraindicated. Controlled clinical trials demonstrate COAT to be safe and effective in patients with pain that is not related to cancer.19 Patients requiring intermittent relief from pain may be given appropriate dosages of oral narcotic analgesics combined with acetaminophen. Those patients needing ongoing pain relief may be prescribed controlled-release oxycodone (Roxicodone) or morphine sulfate (Duramorph). Patients receiving COAT should be informed of the possibility of dependence and should be monitored regularly.20
Nonsteroidal Anti-Inflammatory Agents (NSAIDs). Although commonly prescribed in analgesic doses, NSAIDs have not been proved to be effective in the treatment of fibromyalgia.
BEHAVIOR THERAPIES
Patients with fibromyalgia may experience difficulty fulfilling work and social obligations because of poor symptom control. This difficulty can lead to social isolation and feelings of decreased self-efficacy. Collaborative care between family physicians and other health care professionals may provide optimal benefit for patients. Pain perception is an extremely complex phenomenon that may be modified by experience. Several behavior science approaches appear to hold benefit for fibromyalgia.
Cognitive Behavior Training. A program21 of 20 hours of relaxation response training and movement therapy found to be effective in treating patients with low back pain included 28 patients with fibromyalgia. Patients who completed the program reported reduced pain and other symptoms, as well as improved function and general health.21
One study22 reviewed two types of “formal self-management strategies” published from 1981 through 1996. The results tend to favor training in coping skills as being more effective than physical fitness training, but preliminary evidence suggests that combining both types of training may be more effective than either alone. As with all of the approaches to fibromyalgia, this article22(p.445) points out that “not all individuals show the same response to these programs.” A program23 combining cognitive behavior strategies, physical exercise, relaxation and information about chronic pain was compared with a control program of autogenic (self-hypnosis) training only. At the end of treatment and four months later, members of the study group reported less impairment in their daily lives.23
Hypnosis. In a controlled study of 40 patients, hypnosis improved functioning and reduced pain more than physical therapy.24
OTHER THERAPIES
Several therapies that are less well studied and less commonly used may be helpful in certain cases.
Growth Hormone Therapy. Treatment with recombinant growth hormone was highly effective in reducing symptoms and improving quality of life in a small, randomized study25 involving a subset of patients with fibromyalgia and low insulin-like growth factor I levels. No significant side effects were encountered. Unfortunately, the cost of growth hormone is prohibitive for most patients.25
Chiropractic Treatment. Following four weeks of treatment, 21 patients with fibromyalgia improved compared with control subjects receiving medication only.26
Support Groups and Online Chat Rooms. Many patients benefit from discussing their day-to-day lives with others who are also affected by fibromyalgia. Support groups may be located through a local chapter of the Arthritis Foundation (AF). The AF address is 1330 W. Peachtree St., Atlanta, GA 30309. Information on local chapters can be found on the AF Web site at http://www.arthritis.org.
INITIATING TREATMENT
The goals of treatment for fibromyalgia are to control pain and improve function. These goals can be met using a variety of techniques. A reasonable and cost-effective strategy may be initiated using antidepressants and exercise. If patients do not tolerate these measures or if additional symptomatic relief is needed to maintain function, the addition of hypnosis, behavior therapy, acupuncture and/or chiropractic treatment could then be considered. If pain control or function, or both, are still poor, COAT should then be considered.