
Am Fam Physician. 2000;62(10):2267-2274
Recent studies have shown that beta blocker therapy improves survival and reduces hospitalizations in patients who have chronic heart failure and left ventricular systolic dysfunction, the majority of whom are under the management of primary care physicians. Appropriate patient selection is essential to the successful initiation of beta blocker therapy. Candidates should be stable in New York Heart Association functional class II or III. Patients with severe heart failure, especially inotrope-dependent and hospitalized patients, and those with hypotension, bradycardia or higher than first-degree heart block are not considered appropriate candidates for beta blocker therapy. Optimal diuresis is essential for maximal tolerability. Beta blockers should be started at the lowest dose, with the dose increased every two to four weeks until the target dose or highest tolerated dose is reached. Close monitoring allows for the detection and appropriate management of side effects, such as hypotension, bradycardia and increased congestion. The treatment goal is long-term improvement of prognosis, rather than immediate improvement of symptoms.
Recent large clinical trials have shown that long-term beta blocker therapy reduces morbidity and mortality in patients with chronic heart failure.1–8 The unequivocal evidence creates a mandate for the extension of beta blocker therapy to the large and growing population of patients with chronic heart failure, a population managed mostly by primary care physicians. There is persistent concern, however, among medical practitioners regarding this seemingly counterintuitive therapy. This concern might lead to underutilization and deprive patients and the health care system of a tremendous benefit.
To succeed with this challenge, physicians should adopt the improvement of survival and the reduction of morbidity as the main long-term therapeutic goals in the management of patients with chronic heart failure. They should also identify appropriate patients and initiate therapy in a manner similar to that employed in the clinical trials. This article reviews evidence for the use of beta blocker therapy in patients with chronic heart failure and discusses its practical aspects.
Evidence
The first compelling survival evidence supporting the use of beta blockers in patients with chronic heart failure came from the carvedilol research program, which was conducted in patients with left ventricular systolic dysfunction and predominantly mild to moderate impairment of exercise tolerance.1–5 In these studies, carvedilol, which is a nonselective beta blocker with alpha1-blocker vasodilating properties, reduced mortality by 65 percent and hospitalizations by 29 percent. Carvedilol therapy also resulted in significant improvement in left ventricular ejection fraction and sense of well-being.
In the Cardiac Insufficiency Bisoprolol Study II (CIBIS-II),6 treatment with bisoprolol, a beta1-selective blocker, resulted in a 34 percent reduction of mortality in patients with mild or moderate chronic heart failure and systolic dysfunction. The reduction in all-cause hospitalizations was approximately 20 percent.
Most recently, the Metoprolol CR/XL Randomised Intervention Trial in Heart Failure (MERIT-HF)7 demonstrated that treatment with sustained-release metoprolol (i.e., metoprolol succinate), also a beta1-selective blocker, reduced mortality by 34 percent in patients with predominantly mild or moderate chronic heart failure.
These three trials (Table 1),1,6,7 along with a series of smaller controlled studies, enrolled more than 10,000 patients and conclusively demonstrated a remarkable reduction in the risk of death and the combined risk of death or hospitalization in patients with chronic heart failure who were treated with one of several beta-adrenergic blockers.8 The reduction in mortality risk applied to both sudden death and death from progressive heart failure, and the benefit was demonstrated in patients with ischemic and nonischemic cardiomyopathy. The studies also demonstrated a consistent significant improvement in ventricular function. However, no consistent improvement in maximal exercise capacity was shown.
| Study | Number of patients (functional class*) | Drug and mean dose | Follow-up period | Relative reduction in all-cause mortality |
|---|---|---|---|---|
| U.S. Carvedilol Heart Failure program1 | 1,094 (mostly class II or III) | Carvedilol, 45 mg per day | 7 months (median) | 65 percent (P < 0.001) |
| Cardiac Insufficiency Bisoprolol Study II6 | 2,647 patients (mostly class II or III) | Bisoprolol, 7.5 mg per day | 16 months (mean) | 34 percent (P < 0.0001) |
| Metoprolol CR/XL Randomised Intervention Trial in Congestive Heart Failure7 | 3,991 patients (mostly class II or III) | Metoprolol, 159 mg per day | 12 months (mean) | 34 percent (P < 0.0001) |
Why Beta Blockers Work
Left ventricular systolic dysfunction is associated with activation of a host of interconnected neurohormonal “adaptive” mechanisms, most notably the sympathetic and renin-angiotensin-aldosterone systems. Chronic activation of these mechanisms exerts deleterious hemodynamic and direct cardiotoxic effects and contributes to the progressive deterioration of ventricular function. Attenuation of these mechanisms is associated with improvement in survival. This has been demonstrated for angiotensin-converting enzyme (ACE) inhibitors,9–12 beta blockers1–8 and spironolactone,13 and is suggested for other classes of drugs under evaluation.
Selection of Patients
Proper selection of patients is essential to the successful initiation of beta blocker therapy.
APPROPRIATE PATIENTS
Based on current evidence, consideration of beta blocker therapy is appropriate in patients with chronic heart failure who meet the following criteria (Table 2):
Systolic left ventricular dysfunction (left ventricular ejection fraction of 40 percent or less).
Stable circulation (neither progressive fluid accumulation nor worsening cardiac output).
Mild or moderate impairment of functional capacity. Appropriate candidates are those in functional class II or III (New York Heart Association [NYHA] classification), regardless of the extent of ventricular dysfunction.
Generally meet the enrollment criteria of the clinical trials,1,6,7 including no symptomatic hypotension (systolic blood pressure should be greater than 90 mm Hg), no bradycardia (heart rate should be greater than 60 beats per minutes) and no higher degree (second- or third-degree) heart block.
No contraindications to the use of beta blockers.
| Left ventricular systolic dysfunction (left ventricular ejection fraction ≤ 40 percent) |
| Mild or moderate impairment in functional capacity (functional class II or III*) |
| Optimal and stable circulation |
| No contraindications to the use of beta blockers |
INAPPROPRIATE PATIENTS
Beta blockers are not appropriate for use in some patients with chronic heart failure because evidence of benefit is lacking or because experience suggests that treatment may have deleterious effects (Table 3). At this time, patients inappropriate for beta blocker therapy include those who have severe heart failure (functional class IV), those who require intravenous inotropic support, those who are hospitalized for decompensated heart failure and those who do not have systolic dysfunction.
| Heart failure without left ventricular systolic dysfunction |
| Severe impairment of functional capacity (functional class IV*) |
| Decompensated circulation (fluid overload and/or low cardiac output) |
| Circulation requiring intravenous inotropic support (e.g., dobutamine [Dobutrex]) |
Patients with Severe Heart Failure. The role of beta blockers in patients with severe heart failure is still under evaluation. At present, beta blocker therapy is not indicated in these patients.
Many patients with functional class IV heart failure are symptomatic because of inadequate diuresis. These patients often improve markedly with appropriate diuresis, and they are likely to tolerate and benefit from beta blockers once they are optimally diuresed.
It is also important to note that the criterion for the severity of heart failure is not the extent of left ventricular systolic dysfunction but the impairment of functional capacity on optimal medical therapy.
Inotrope-Dependent Patients. Patients with chronic heart failure whose circulation requires intravenous inotropic support (e.g., dobutamine [Dobutrex]) should not be treated with beta blockers. These patients are unlikely to tolerate withdrawal of their endogenous inotropic support.
Patients Hospitalized for Heart Failure. In general, it is advisable to avoid initiating beta blocker therapy during or immediately after hospitalization for decompensated heart failure. Beta blocker therapy should be started in patients with stable “compensated” circulation. Hospitalized patients often have fluid overload or low cardiac output. Although their condition may be improved at the time of hospital discharge, their long-term stability has not been ascertained, and their medical regimen often requires further adjustment. If beta blocker therapy were to be started too early, it might be difficult to determine whether subsequent deterioration is due to the beta blocker, the inadequacy of background therapy or the patient's lack of circulatory reserve.
Patients Without Systolic Dysfunction. Beta blockers have not been shown to reduce morbidity and mortality in patients with chronic heart failure but normal systolic function (i.e., normal left ventricular ejection fraction). These patients, who probably account for more than 30 percent of all patients with chronic heart failure, are often elderly and have hypertension, coronary artery disease or diabetes. Although these patients often tolerate beta blockers and might benefit from their anti-ischemic and blood pressure–lowering effects, they should not receive beta blocker therapy for the primary treatment of heart failure.
Background Medical Therapy
Before beta blocker therapy is initiated, patients should be receiving appropriate background therapy.
DIURETICS
Optimal diuresis is essential to the successful initiation of beta blocker therapy. Overdiuresis and underdiuresis can result in inappropriate ventricular loading and low cardiac output, which can lead to further activation of the sympathetic nervous system and increased reliance on it for circulatory support.
Intravascular volume depletion can also potentiate the hypotensive effect of beta blockade. Underdiuresis, on the other hand, results in congestion, which might make it difficult to tolerate the negative inotropic effects of beta blockers.
ACE INHIBITORS
The survival benefit of beta blockers was demonstrated in patients who were given ACE inhibitors. Before beta blocker therapy is initiated, candidates should be receiving standard doses of ACE inhibitors. In view of the higher benefit derived from beta blockers, it is argued that priority should be given to the initiation and up-titration of beta blockers before further increase in the dose of ACE inhibitors.14
DIGOXIN
The Digitalis Investigation Group (DIG) study15 found that digoxin therapy did not reduce mortality in patients with mild to moderate chronic heart failure, the same patients in whom beta blockade is appropriate. Therefore, beta blockers should take precedence over digoxin (Lanoxin), especially when bradycardia is a concern or a patient is at high risk for dysrhythmia.
SPIRONOLACTONE
Initiation of Beta Blocker Therapy
Appropriate candidates for beta blocker therapy should be evaluated thoroughly before treatment is initiated. The evaluation should include a comprehensive history and physical examination, with special emphasis on the assessment of functional capacity and the appropriateness of diuretic therapy. An electrocardiogram should be obtained to exclude the presence of high-degree heart block. An approach to the evaluation and treatment of patients with chronic heart failure is presented in Figure 1.14
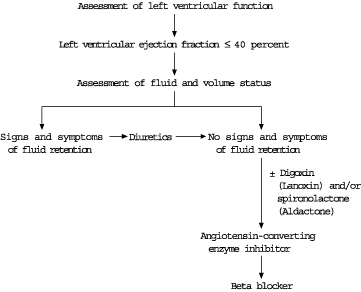
CIRCULATORY STATE AND DIURESIS
Optimal management of intravascular volume results in maximal resting cardiac output and minimal congestion, thereby minimizing sympathetic activation. Patients with evident extravascular fluid retention should be diuresed until the disappearance of excess fluid and the normalization of jugular venous pressure (unless tricuspid regurgitation is present). The diuresis is usually associated with improvement in perfusion. Before beta blocker therapy is initiated, patients should be stable on a maintenance diuretic regimen.
CHOICE OF BETA BLOCKER
Carvedilol (Coreg), bisoprolol (Zebeta) and metoprolol succinate (Toprol XL) have all been shown to be beneficial in patients with chronic heart failure. At present, the U.S. Food and Drug Administration has labeled only carvedilol for use in slowing the progression of chronic heart failure. Carvedilol is also the only beta blocker that is available in the requisite low starting dose. No studies to date have compared the effects of carvedilol, bisoprolol and metoprolol succinate on clinical outcomes.
Not all beta blockers are equally tolerated by patients with chronic heart failure. Other beta blockers, such as labetalol (Normodyne), atenolol (Tenormin) and propranolol (Inderal), have not been studied adequately in this patient population.8
DOSING
Abrupt withdrawal of sympathetic circulatory support is not well tolerated. Patients should therefore be started on a low dose: carvedilol, 3.125 mg twice daily; metoprolol succinate, 12.5 mg per day; or bisoprolol, 1.25 mg per day.
Rapid advancement of the dose may not be tolerated, especially in sicker patients who are more dependent on neurohormonal compensatory mechanisms. Adequate attempts should be made to increase the dose gradually to the highest level tolerated, because higher doses are associated with increased benefit.4
A reasonable timetable is to double the dose every two to four weeks as tolerated, until the target dose (or highest tolerated dose) is attained. The target doses for carvedilol are 25 mg twice daily for patients weighing less than 84 kg (185 lb) and 50 mg twice daily for patients weighing more than 84 kg. For bisoprolol, the target dose is 10 mg per day, and for metoprolol succinate, the target dose is 200 mg per day.
MONITORING SIDE EFFECTS
With appropriate patient selection and preparation, clinic-based monitoring for side effects may be unnecessary in most patients once the physician has adequate experience in treating chronic heart failure with beta blockers. The majority of patients with functional class II chronic heart failure tolerate the small initial doses well.
Up to 15 percent of patients might not tolerate beta blocker therapy. The intolerance might only become apparent when symptoms are reported several days later or signs are detected at the next visit. Therefore, patients should be informed of possible side effects and instructed to call if any occur.
Patients should be monitored closely for signs and symptoms of increased congestion or hypoperfusion. This can be done effectively through telephone contact, visiting nurses or frequent office visits. Patients should be evaluated in the office before any dose increase, depending on clinical status, and an electrocardiogram should be obtained to exclude advanced heart block.
Neither patient nor physician should expect immediate improvement of symptoms but should aim for long-term improvement of prognosis. Patients should be informed of the goals of therapy and that this treatment might continue in the absence of immediate improvement of symptoms.
Management of Side Effects and Concomitant Therapy
HYPOTENSION
Symptomatic hypotension or hypoperfusion might occur at the starting doses of beta blockers. Intravascular volume depletion should first be excluded. In less serious situations, hypotension might be prevented by the administration of a once-daily ACE inhibitor taken at a different time than the beta blocker.
At times, a temporary decrease in the dose of ACE inhibitor might be necessary. Often, the dose can be increased to the original level after a few months of stability on the maximal dose of beta blocker.
If hypoperfusion or symptomatic hypotension (other than fleeting orthostatic symptoms) persists, the dose of the beta blocker must be reduced, or the drug must be discontinued (Table 4).
| Possible problem | Step 1 | Step 2 | Step 3 |
|---|---|---|---|
| Symptoms of vasodilation | Decrease diuretic dose. | Decrease vasodilator dose. | Decrease beta blocker dose. |
| Symptoms of fluid retention | Increase diuretic dose. | Decrease beta blocker dose. | |
| Symptomatic bradycardia | Check digoxin (Lanoxin) level; adjust dose if necessary. | Decrease beta blocker dose. |
BRADYCARDIA
beta blocker therapy is associated with a dose-dependent decrease in heart rate. Often, this decrease is neither severe nor symptomatic. The beta blocker dose should be reduced if the decrease in heart rate is symptomatic or is associated with hypoperfusion or higher than first-degree atrioventricular block.
If patients are also taking digoxin, consideration should be given to reducing the digoxin dose or discontinuing the drug, especially in patients with mild heart failure.
INCREASED VASCULAR CONGESTION
Increased congestion might occur because of the negative inotropic effect of beta blockers. Congestion often resolves with transient intensification of diuresis. Rarely, it might necessitate dose reduction or discontinuation of the beta blocker.
Management of Decompensation
The management of patients with chronic heart failure who deteriorate after a period of stability on beta blocker therapy requires thoughtful evaluation. Often, the “decompensation” occurs because of fluid retention, which may be the consequence of an inadequate diuretic regimen, poor absorption of diuretic or loop-diuretic resistance. In this situation, diuresis should be intensified, by increasing the diuretic dose, adding a thiazide-like diuretic or administering a diuretic intravenously, while the beta blocker therapy is continued.
On the other hand, if the decompensation is in the form of low cardiac output in the setting of optimal fluid management, an attempt should be made to restore stable circulation with short-term intravenous infusion of a phosphodiesterase inhibitor (e.g., milrinone [Primacor]) while beta blocker therapy is maintained. If this approach fails, the beta blocker dose should be decreased, or the drug should be discontinued.
Discontinuation of Beta Blockers
Stable patients with chronic heart failure who are taken off beta blockers are at risk for circulatory deterioration and electrophysiologic instability.16 Unless necessary, beta blockers should not be discontinued. If discontinuation is necessary, the dose should be decreased slowly whenever possible.