
Am Fam Physician. 2000;62(12):2613-2620
See related patient information handout on coping tips for caregivers, written by the authors of this article.
Patients who provide care to family members or friends with dementia are likely to be in a family physician's practice. The caregiver role can be stressful, and identifying these patients can give the family physician opportunities to help patients cope with the challenges of the caregiver role. Family physicians have a systematic approach for assessing the degree of caregiver burden in these patients. Because caregivers are at increased risk for depression and anxiety, screening should be done to exclude the presence of either disorder. The caregiver's skill in managing behavioral problems in the family member with dementia should be assessed. If there are problems, family physicians should provide practical counseling about common caregiving stresses and about resources that benefit caregivers. Helping the caregiver learn strategies for coping with difficulties may help reduce some of the stress the caregiver is experiencing.
By the year 2030, an estimated 20 percent of the U.S. population will be 65 years or older.1 As the American population ages, a growing number of people will be serving as caregivers for family members affected by dementia and other types of functional impairment. Dementia is present in 10 percent of individuals older than 65 years and in 47 percent of those older than 85 years.2 As many as 80 percent of persons with dementia are cared for in their homes by family members.3 In day-to-day practice, family physicians are likely to see patients who serve as caregivers. In fact, one study of patients in a family practice demonstrated that 21 percent of the patients had caregiving responsibilities for persons with chronic medical conditions.4
Caring for someone with dementia is associated with a higher level of stress than caring for someone with functional impairment from another type of chronic illness.5 One survey revealed that persons with Alzheimer's disease required an average of 70 hours of care per week, with 62 of those hours provided by the primary caregiver. By 1990 dollar amounts, it was calculated that a caregiver provided $34,517 of care annually.6
While the issues faced by caregivers of patients with dementia are emphasized in this article, the basic principles apply to other illnesses as well. Knowledge of these principles can help family physicians teach their patients who are caregivers new coping strategies and make appropriate interventions for those caregivers who are overwhelmed.
Caregiver Burden
Caregiver burden is an all-encompassing term used to describe the physical, emotional and financial toll of providing care.7 Numerous questionnaires have been developed to quantify the largely subjective domain of caregiver burden, but the Zarit Burden Interview is the most widely referenced scale in studies of caregiver burden (Figure 1).8
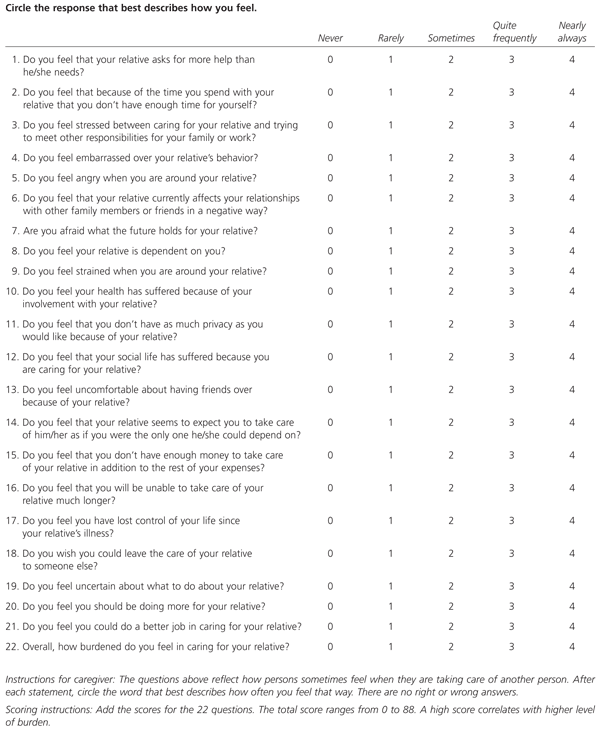
Surprisingly, research has shown that the level of burden perceived by the caregiver does not correlate with the duration of time spent as a caregiver or the progression of memory loss in the family member who is receiving care.9,10 Studies also suggest that the degree of functional impairment in the person receiving care does not correlate with caregiver burden.11 The degree of behavioral problems in patients with dementia, however, does contribute to caregiver burden.10 When patients with dementia have depression, their caregivers report higher levels of burden.12
Characteristics of the caregiver's skills are directly related to caregiver burden. For example, active coping skills and management strategies are associated with lower levels of caregiver burden. Active strategies include “constructing a larger sense of the illness” and being firm in directing a relative's behavior.13 According to Saad and colleagues,13 a caregiver may develop a larger sense of the illness by making sense of the illness, praying for strength to keep going and reminding himself or herself that this is something to expect with aging. Family support, specifically frequent visits by other family members, and the presence of a strong social network correspond with lower levels of caregiver burden.8,11
The consequences of a high caregiver burden include an increased risk of the need to place the family member in a long-term care facility as well as increased use of formal in-home services.14 The societal and economic benefits of reducing the amount of caregiver burden are evident. In addition, higher levels of burden may correlate with increased morbidity and mortality in caregivers.15 Multiple studies10,16–20 have shown that the incidence of depression in caregivers is high, ranging from 18 to 47 percent, and caregivers who are depressed experience higher degrees of burden.21
Health Problems of Caregivers
Most of the research on the health of caregivers has focused on psychologic well-being. Depression is the most heavily researched area in caregiver health. One study22 revealed that anxiety was present in 17.5 percent of caregivers, compared with 10.9 percent of subjects in a matched control group. An increased incidence of anxiety correlates with research that has documented a higher amount of psychotropic drug use among caregivers.23 The incidence of alcohol use among caregivers is uncertain. One study10 showed less alcohol use among caregivers than the general population, and another study24 showed no difference in the amount of alcohol use by caregivers and the general population.
When compared with persons who are not in a caregiving role, caregivers perceive their own health status to be lower.23 More than just perception, the immune function of caregivers may be reduced. Research24 has shown that viral illnesses last longer in caregivers than in control subjects. In addition, three measures of cellular immunity have been shown to be lower in caregivers than in control subjects.24
A landmark study15 of caregiver health revealed that elderly spousal caregivers who experienced caregiver strain had a mortality risk that was 63 percent higher than that in control subjects. The implications of this study make early identification of caregiver burden and appropriate intervention even more critical.
An Office-Based Approach
Caregivers have been described as “hidden patients.”4 Family physicians should identify their patients who are caregivers through a detailed family and social history. Caregivers should be assessed for their level of perceived burden and for the presence of affective disorders such as depression and anxiety. In addition, family physicians should assist caregivers with coping strategies, counseling them about ways to handle behavioral management issues that arise during the course of dementia.
The degree of caregiver burden should be assessed systematically. Questionnaires designed to quantify caregiver burden are not intended for use during routine office assessments. In the office setting, asking the patient a few questions can give a measure of the patient's caregiver burden (Table 1).
| Screening question | Area of concern |
|---|---|
| Do you feel that you are currently under a lot of stress? What aspects of your day are the most stressful? | Mental health |
| Have you been feeling down or blue lately? | Mental health |
| Have you been feeling more anxious and irritable lately? | Mental health |
| Do your family and friends visit often? Do they telephone often? | Social support |
| Do your friends and family watch your relative for you so that you have time for yourself? | Social support |
| Do you have any outside help? | Resources |
| Is your relative with dementia having any behaviors, such as wandering, that are difficult to manage? | Behavioral management |
| What do you do to relieve your stress and tension? | Coping |
Mental health issues are a significant area of concern. Because depression is the most common health problem in caregivers, it should be screened for routinely. Family and individual counseling may be considered for patients with affective disorders or a high level of caregiver burden.
Social support and resources should be explored if the patient's answers to screening questions suggest a need for outside help. The clinician should ask specifically about the number of visits each week by family members and friends. The patient also may be asked, “Have your family or friends offered to help?” or “Have you accepted the offer?”
RESPITE CARE
If the caregiver does not receive respite regularly, physicians should give them permission to ask for help and assist them in finding sources for assistance. Ways to suggest sources include stating something like “You might want to think about contacting your church/synagogue for some help with your mom. They often have sitting services available.” Another approach might be to say, “Getting outside help may be a way for you to get regular time outside the house. I'm going to give you a telephone number so you can contact your local office on aging. It is a good resource for you.”
Adult day services are an excellent source of respite for the caregiver and provide engaging activities for persons with dementia. The local Area Agency on Aging can provide the caregiver with a list of nearby facilities. In one study,25 caregivers gave respite services a rating of high overall satisfaction. Although formal and informal respite care has been shown to delay institutionalization, respite care has a varied impact on caregiver burden.25,26
Family issues often surface when discussing the specifics of respite care. Numerous and varied family stresses develop around providing care to the family member. The primary caregiver can have difficulty accepting other family members' support while at the same time resenting a perceived lack of support.
BEHAVIORAL ISSUES
The caregiver's skills in managing behavioral issues should be explored in more detail if the screening questions indicate problems in this area. When assessing the caregiver's skills in dealing with behavioral problems, the physician should give examples of situations, such as “How would you respond to your mother's asking the same question repeatedly, such as, ‘Where is John?’” Studies13 suggest that caregivers who are firm and directive tend to have less depression. Physicians should tell caregivers to be more directive, as opposed to passive, in their strategies for dealing with difficult behaviors. For example, a direct response would be, “Mom, John is not here right now, so let's start getting lunch ready.”
Physicians should also encourage the caregiver to engage the family member in activities. For example, the caregiver can be asked, “Does your husband help with household tasks?” In this case, the caregiver should be encouraged to involve her husband in simple tasks such as folding the laundry.
STRATEGIES FOR STRESS RELIEF
If the caregiver has trouble listing his or her strategies for stress relief, this is an area for further questioning. Coping strategies can be divided into emotion-focused and problem-focused. Examples of emotion-focused strategies are worrying and self-accusation. Caregivers who use problem-focused strategies, such as confronting issues and seeking information have less burnout.26 Physicians should explore these strategies with their patients. A sample question for caregivers would be, “When something goes wrong with your brother's care, for instance, if he loses control of his bladder, how would you react?” Emotion-focused responses are “I'd cry” or “I'd put him in a home.” A problem-focused response is, “I'd call the doctor and find out what's happening.” A tendency to use emotion-focused responses should alert the physician to an increased risk of burnout in the caregiver.
Active coping strategies, such as constructing a larger sense of the illness, are associated with a lower incidence of depression among caregivers.13 The caregiver can be guided toward seeing the bigger picture by stating, for example, “I know this time has been challenging for you. What do you see yourself doing when you are no longer a caregiver?”
Support groups are popular outlets for caregivers. One study3 revealed that educational support was most beneficial to caregivers when it was problem-focused, such as on behavioral management. In another study,28 combination intervention that included individual and family counseling sessions as well as mandatory participation in support groups was found to delay the need for nursing home placement. Institutionalization of dementia patients was delayed by 329 days in the intervention group of caregivers, compared with the group of caregivers who did not receive counseling and other forms of support.
For many caregivers, much of their burden is related to feelings of loneliness or isolation. Specific groups such as the Breakaway program26 are designed to supplement traditional support groups by providing informal recreational and social activities with a peer group of caregivers who are experiencing similar stresses. Table 2 summarizes some coping tips for caregivers.
| Educate yourself about the disease your family member is facing and how it may affect his or her behavior, pain level, etc. |
| Find sources of help for caregiver tasks. Contact family, friends, neighbors, church/synagogue, workplace, Area Agency on Aging or other organizations. Keep looking! |
| Protect your personal time for something you enjoy or something you need to get done. |
| Try to find time for exercise, eating well and sleeping enough. |
| Use your personal network of friends and family for support or find a support group for caregivers of dementia patients in your area. |
| Watch out for symptoms of depression (such as crying more, sleeping more or less than usual, increased or decreased appetite or lack of interest in usual activities). Notify your doctor if symptoms of depression are present. |
| Consider how you will feel and what you will do after the caregiving ends. |
ELDER ABUSE
After the caregiver's behavioral management and coping strategies are assessed, it is important to consider the issue of elder abuse. Although the incidence of abuse in the dyad of a dementia patient and a family caregiver is not very high, caregivers with a higher burden may have an increased potential for mistreating the family member.29 If abuse is suspected, physicians can contact the appropriate local authorities through the National Hotline for Physician Reporting of Elder Abuse or Neglect at 800-490-8505. Mandatory reporting laws vary by state.
PATIENT EDUCATION
Because a lack of understanding about the family member's disease process may worsen caregiver stress, the caregiver's knowledge about the dementing illness and available resources should be explored and additional information provided when needed. Caregivers may be given written educational materials regarding dementia. Resources such as those in Table 3 should also be made available to caregivers.
| Alzheimer's Association | |
| Telephone: 800-272-3900 | |
| Web address: http://www.alz.org | |
| National Information Center of the U.S. Administration on Aging | |
| Telephone: 202-619-7501 | |
| American Association of Retired Persons; a free caregiver resource kit is available (No. D15267) | |
| Telephone: 800-424-3410 | |
| National Counsel on the Aging | |
| Telephone: 202-479-1200 | |
| Children of Aging Parents | |
| Telephone: 800-227-7294 | |
| Telephone: 215-945-6900 | |
| Web address: http://www.caps4caregivers.org | |
| National Family Caregivers Association | |
| Telephone: 800-896-3650 | |
| Web address: http://www.nfcacares.org | |
| The Well Spouse Foundation | |
| Telephone: 800-838-0879 | |
| Telephone: 202-685-8815 | |
| Web address: http://www.wellspouse.org | |
| National Hotline for Physician Reporting of Elder Abuse and Neglect | |
| Telephone: 800-490-8505 | |
| Eldercare Locator (A nationwide service for locating area agencies on aging) | |
| Telephone: 800-677-1116 | |
| Administration on Aging | |
| Web address: http://www.aoa.gov | |
| Caregiving Online (Online support service through a caregiving newsletter) | |
| Web address: http://www.caregiving.com | |
| Alzheimer's Disease Education and Referral Center, National Institute on Aging (This Web site includes information about ongoing studies.) | |
| Web address: http://www.alzheimers.org | |
| CareGuide.com (A personal caregiving resource) | |
| Web address: http://www.careguide.net | |
| Caregiverzone.com (A Web site for family persons) | |
| Web address: http://www.caregiverzone.com | |
Anticipatory Guidance
The period following the death of the care recipient can be a difficult transition for some caregivers. One study30 suggests that caregivers who experience high levels of burden during the caregiving role tend to have more difficulty with the bereavement process. After identifying caregivers with higher levels of burden, family physicians should help prepare these patients for the emotional challenges ahead.
Final Comment
Family physicians can have a significant impact on the health and well-being of caregivers. By assessing the caregiver's level of burden, including the issue of depression, the physician can identify caregivers who are at high risk for physical and emotional problems. Family physicians can educate caregivers on behavioral management techniques and coping strategies. By providing the holistic approach to care for caregivers, family physicians can help prepare them for the many phases of this challenging role.