Sleep problems are common in childhood. A distinction is made between problems in which polysomnography is abnormal (i.e., the parasomnias, sleep apnea and narcolepsy) and problems that are behavioral in origin and have normal polysomnography. The parasomnias—sleep terrors, somnambulism and enuresis—appear to be related to central nervous system immaturity and are often outgrown. Obstructive sleep apnea syndrome (OSAS) is frequently missed in children and can often be cured through surgery. Behavioral sleep problems may be overcome after parents make interventions. Physicians can be of great assistance to these families by recommending techniques to parents that have been shown to be effective.
Sleep behaviors are among the most common concerns that parents of young children bring to their physicians. A child who goes to bed unwillingly or wakes frequently during the night can be highly disruptive to a family. Sleep disorders in children, if confirmed by reproducible findings in a sleep laboratory, are not appreciably different from those occurring in adults. However, sleep problems, defined as a sleep pattern that is unsatisfactory to the parents, child or physician, are far more common.
Defining disordered sleep behavior is difficult because of important differences in sleep patterns that occur at different developmental stages. Thus, it is not considered abnormal when a two-month-old infant wakes frequently in the night, but it is considered abnormal in a two-year-old child. To make the definition of sleep problems even more difficult, families vary greatly in their tolerance of their children's sleeping habits; what one family finds problematic, another family takes as a matter of course.
Helping a family resolve a child's sleep problem is satisfying for a family physician and worth the time spent taking a careful history.
Normal Sleep in Children
Early-infant sleep is quite different from the sleep of adults. Infants younger than six months spend 50 percent of their sleep time in active rapid-eye-movement (REM) sleep, compared with 20 percent in adults. Infants enter sleep through an initial active REM stage, in contrast to adults, who don't commonly enter REM sleep until 90 minutes into the sleep cycle. Active REM emerges more often during a sleep cycle in infants, resulting in shorter sleep cycles. Until six months of age, quiet REM (also known as quiet or indeterminate sleep) cannot be subdivided into the four electroencephalographic (EEG) stages known in the mature sleep pattern.
By six months, the infant's sleep architecture closely resembles that of an adult's. After an initial “settling” period that typically takes 10 to 20 minutes, the infant drifts from stage 1 non-REM (NREM) sleep into stage 3 or 4. The infant may return to stage 1 and cycle again. After one to two cycles of NREM sleep, REM is entered at about 60 to 90 minutes. The first one third of the night is mostly deep sleep (NREM stages 3 and 4). The last one half of the night is predominately stage 2 NREM and REM.
In newborns, the amount of sleep is divided fairly equally between night and day. Nighttime sleep gradually becomes consolidated over the first year into a single uninterrupted block of time, and daytime sleep gradually decreases over the first three years (Figure 1).1 By the age of four, most children no longer require a daytime nap. Nighttime sleep requirements also gradually decrease, so that by adolescence they are similar to the sleep needs of an adult.
FIGURE 1. Change in Hours of Daytime and Nighttime Sleep with Increasing Age
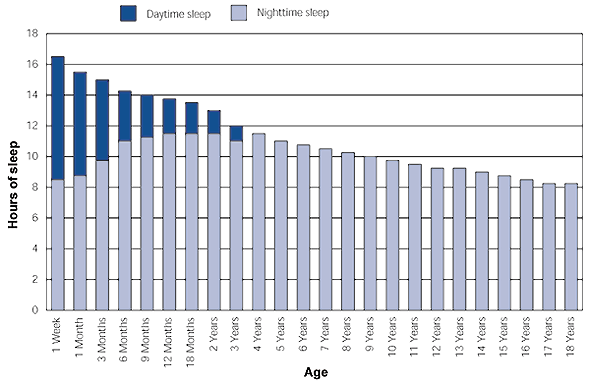
In newborns, the amount of sleep is divided fairly equally between night and day. In the normal infant, nighttime sleep gradually becomes consolidated over the first year into a single uninterrupted block of time, and daytime sleep gradually decreases over the first three years.
Adapted with permission from Ferber R. Solve your child's sleep problems. New York: Simon and Schuster, 1985.
Scope of the Problem
Parents of young children are eager to know when they can expect their child to sleep through the night. Research has provided divergent answers because different populations have been examined, different definitions used for “waking” and different techniques used to obtain results. As a rule, the frequency of night waking starts at 100 percent in newborns and tails off to approximately 20 to 30 percent in six-month-olds. Sleeping through the night is a milestone that is not always maintained once it has been reached. Children who previously slept through the night can sometimes resume night awakening, usually because of social factors rather than maturational ones.
Cross-sectional studies2,3 show that night awakenings are common throughout early childhood. Approximately one child in three up to four years of age will continue to awaken during the night and require intervention by a parent to return to sleep.
Parasomnias
Parasomnias are sleep disorders characterized by abnormal polysomnography. They are episodic in nature and are a reflection of central nervous system (CNS) immaturity. Thus, they are more common in children than in adults and are generally outgrown with time. There is often a family history positive for these parasomnias.
As a group, these disorders are paroxysmal, predictable in their appearance in the sleep cycle, nonresponsive to environmental manipulation and characterized by retrograde amnesia. The diagnosis is often made by means of a thorough history. An extensive work-up is seldom necessary.
‘Pavor Nocturnus’ or Night Terrors
Pavor nocturnus (night terrors) occur approximately 90 minutes into sleep during stage 3 or 4 NREM sleep. The child suddenly sits bolt upright and screams, and is inconsolable for up to 30 minutes before relaxing and falling back to sleep. Tachycardia, tachypnea and other signs of full-fledged autonomic arousal are apparent.
Night terrors usually occur in children three to eight years of age. They need to be distinguished from nightmares (Table 1). They are more likely to occur during times of stress or fatigue. As frightening as they are, parents and children usually only need to be reassured that they are generally self-limiting. Attempts should be made to alleviate whatever stress may be going on in the child's environment and to ensure that the child is getting adequate rest. In children for whom night terrors are not self-limiting or are especially disruptive, diazepam (Valium) has been used with some success.
TABLE 1 Comparison of Night Terrors and Nightmares
| Factor | Sleep Terrors | Nightmares |
|---|---|---|
| Age | 3 to 8 years | Any age |
| Gender | Male predominance | Either |
| Occurrence in sleep cycle | NREM | REM |
| Arousable? | No | Yes |
| Memory for event | None | Yes |
| Exacerbated by stress | Yes | Yes |
REM = rapid eye movement; NREM = non-rapid eye movement.
Somnambulism and Somniloquy
In somnambulism (sleepwalking) and somniloquy (sleeptalking), a child sits up in bed with eyes open but is “unseeing.” Activity may range from a purposeless restlessness in bed to actual walking through the house. Speech is mumbled and slurred, and is rarely intelligible.
These disorders occur in the school-aged child, more often in boys than in girls, and are often associated with enuresis. Sleepwalkers have the potential for physical harm, and parents must take steps to avoid unsafe situations, such as falling from balconies or down stairs. Bedrooms for sleepwalkers should be on the first floor of the home, and windows and doors must be firmly secured. When confronting a sleepwalking child, parents should keep interventions to a minimum and refrain from shaking, slapping or shouting at the child. These sleep behaviors are usually outgrown by adolescence and generally do not require any intervention other than those mentioned above.
Another intervention that proved effective in one study4 was scheduled awakenings. Parents kept a diary of the time of sleepwalking over several nights and then began to waken the child 15 minutes before the sleepwalking had been occurring, making sure the child was fully awake for at least five minutes. With the use of this technique, sleepwalking was quickly extinguished in more than 80 percent of children.
Nocturnal Enuresis
Nocturnal enuresis, or bed-wetting, is one of the most prevalent and persistent sleep problems in children. Enuresis is classed as primary when the child has never been persistently dry through the night and as secondary when the child starts wetting the bed after one year of continence. Primary enuresis is much more common and less likely to have a pathologic cause.
The etiology of primary enuresis is likely to be multifactorial. A strong family history of enuresis is often present. Achieving continence is also maturational, and children who lag developmentally at one and three years of age are more likely to be enuretic at age six. Enuretic children have been found to have a lower functional bladder capacity (the volume of urine a bladder can hold before starting to empty) than children without enuresis, although their true bladder capacity is no different.
Lastly, enuresis is widely regarded as a parasomnia by most sleep researchers because it occurs only during NREM sleep. However, despite parental beliefs, enuretic children are not more difficult to waken than their peers without enuresis.
Other than a thorough history and physical examination with attention to abdominal and neurologic examinations and a urinalysis, an in-depth diagnostic work-up is not indicated in the absence of significant signs and symptoms that suggest anything other than simple, sleep-related enuresis.
Behavioral interventions, such as limiting intake of fluids in the evening and waking the child to use the bathroom before the parent goes to bed have often been tried before the family comes to the physician. Although physicians have sometimes turned to medications, such as imipramine (Tofranil) and desmopressin (DDAVP) as a next step, multiple studies5 have demonstrated the superiority of bed-wetting alarms in terms of cure rates, lack of side effects and low relapse rates. These devices are available through medical supply stores or can be ordered over the Internet.
“Continence training” entails several techniques that are beyond the scope of this article. Readers are referred to the excellent chapter on nocturnal enuresis by Sheldon.6
Obstructive Sleep Apnea Syndrome
Obstructive sleep apnea syndrome (OSAS) is thought to affect 1 to 3 percent of children. Symptoms include snoring, difficulty breathing during sleep or mouth breathing during sleep. Parents of infants with significant OSAS may report difficulty with feeding. OSAS in children is frequently caused by adenotonsillar hypertrophy. Other causes include craniofacial abnormalities, obesity and neuromuscular disease. A high prevalence of allergic disease among children with snoring and OSAS has been reported.7
In adults with sleep apnea, the airway obstruction is intermittent and often profound. In children, because the etiology is adenotonsillar hypertrophy, the obstruction is persistent and, usually, less profound. Children do not often experience the hypersomnolence that occurs in adults but more often present with enuresis, excessive sweating or developmental delay. Emerging evidence links OSAS with a subset of older children who have learning or behavior difficulties, including attention-deficit/hyperactivity disorder.8,9
The diagnosis of OSAS is made in a pediatric sleep laboratory using nocturnal oximetry and polysomnography. Most of these children will experience significant relief from their symptoms following tonsillectomy and adenoidectomy.10 Children whose OSAS has an etiology other than adenotonsillar hypertrophy (e.g., obesity, craniofacial abnormalities, neuromuscular weakness) will not benefit from tonsillectomy and adenoidectomy. Those who experience only partial relief from tonsillectomy and adenoidectomy and those who have other etiologies may benefit from nasal continuous positive airway pressure (CPAP), which has been found to be safe and effective in children.11
Narcolepsy
Narcolepsy is uncommon in children but may sometimes occur in adolescence. The predominant symptom, as in adults, is excessive daytime sleepiness. Understandably, this can be disabling for children who have academic demands. Children do not experience cataplexy or hypnagogic hallucination as frequently as adults do.12
Initially, children with narcolepsy have great difficulty getting up in the mornings. When awakened, the child may appear to be confused or may be aggressive or verbally abusive. The diagnosis may be elusive; the initial polysomnographic study may be normal. Serial evaluations are required if the diagnosis is strongly suspected. These children benefit from regularly scheduled naps. Often, stimulant medication will be required. Because this is a lifetime disease with a potential for significant morbidity, children with narcolepsy should be followed by a sleep specialist.
Secondary Sleep Disturbances
These sleep disturbances are much more common than primary disorders and are characterized by normal polysomnography. The disrupted sleep pattern is often transient, but there is potential for much distress in the family when it persists. The most frequently encountered secondary sleep disturbances are night awakenings and bedtime resistance, which occur most commonly in toddlers and preschool-aged children.
Although 95 percent of newborns cry after a nighttime awakening and require parental response before returning to sleep, by one year of age, 60 to 70 percent of infants will be able to self-soothe if given the chance.13 The concept of sleep-onset associations is an important one. A child who is put to bed still awake and learns to fall asleep using self-comforting measures is often able to calm herself and return to sleep when she rouses in the middle of the night as most children and adults do.
On the other hand, a child who falls asleep accompanied by some parental behavior, such as rocking or being physically present, may sometimes have difficulty going back to sleep when he or she wakes up alone in the middle of the night. For this reason, parents may want to consider a trial of discontinuing rocking the child to sleep, or stop allowing a child to fall asleep somewhere other than his or her crib (such as a swing, a car seat or the parent's bed). They can try waiting a short while before responding to a child who stirs or cries in the night to help train the child to self-soothe back to sleep. Given the opportunity, many children will learn to settle themselves back to sleep without intervention by their parents.
‘COLIC’ AND NIGHT AWAKENINGS
Colic is often the bane of a new parent's existence. While colic is not a sleep problem per se, colicky infants appear to have a shorter duration of total sleep. Sleep problems may sometimes persist after the child has outgrown colic because the strategies that parents developed to decrease the crying spells (i.e., frequent holding, car rides) interfere with the adoption of normal sleep patterns.14
An infant older than four months who continues to wake during the night is considered a trained night crier. These infants calm quickly when picked up. Some people believe that this pattern develops because parents provide secondary gain for continued awakening. One approach that can be taken is to support parents in ignoring the child's cries for progressively longer intervals; they may also choose to stop responding to the crying child “cold turkey.” Either strategy can make for a few difficult nights but may succeed in “training” the child to return to sleep on his or her own. Ferber is best known for the progressive ignoring approach.1
Another technique that has been found to be effective and is more acceptable for some parents is scheduled awakenings. Parents waken the child at scheduled times, shortly before anticipated awakenings. As the frequency of spontaneous awakenings decreases, the length of intervals between scheduled awakenings can be increased. Eventually, the spontaneous awakenings subside, and the scheduled awakening can be discontinued.
DISORDERS OF INITIATING AND MAINTAINING SLEEP (DIMS)
Toddlers and preschoolers begin to have more problems with disorders of initiating and maintaining sleep (DIMS). These children are dealing with significant development issues of autonomy, separation and object permanence. Sometimes parents have trouble setting firm limits and accede to the child's demands for one more drink of water or one more story.
The author recommends that parents deal with attempts to delay bedtime by calmly, but firmly, ignoring the child's protests. Further confrontation is avoided by telling the child that, as long as he or she lies in bed, the door to the bedroom can be kept open, but whenever he or she gets out of bed, the door will be closed (but not locked).
Initially, parents will need to stand by the door, perhaps even holding it closed, but be available to open it as soon as the child gets back in bed.
A recent article15 described a technique that uses a “bedtime pass,” a file card with the child's name printed at the top. The pass can be exchanged without penalty for one short visit outside the bedroom per evening and then is surrendered to the parent for the remainder of the evening.
For children who have difficulty falling asleep, developing a predictable bedtime routine (e.g., three to four components lasting 20 to 30 minutes, such as a story, a song, a drink and a back rub) and using it consistently is helpful. The onset of the routine can be gradually moved earlier and earlier in the evening until the child is going to bed at the desired time. The use of transitional objects such as blankets or stuffed animals may also be helpful.16
SLEEP PROBLEMS IN OLDER CHILDREN
In pre-adolescents and adolescents, sleep problems again become more common. As parental control wanes and academic and social demands increase, sleep may become more and more erratic. There is sometimes a delay in sleep onset, a reduction in sleep hours and excessive daytime sleepiness.
In excessive cases, these children may develop delayed sleep phase syndrome. This means they are unable to sleep at night or to stay awake during the day. This condition may represent a form of school avoidance. Treatment involves holding the child to a firm bedtime, which is gradually moved back in the evening.
A summary of sleep problems and suggested interventions is presented in Table 2.
TABLE 2 Sleep Disorders by Age and Suggested Interventions
| Age | Disorder | Intervention |
|---|---|---|
| 0 to 4 months | Night waking and feeding are developmentally appropriate | |
| 4 to 12 months | Night waking | Systematic ignoring, scheduled awakenings |
| Demand for nighttime feeding | Lengthened interval before feeding, decreased volume/duration of feeding and dilute feeding | |
| 2 to 4 years | DIMS | Predictable bedtime routine, transitional objects, reward system, setting firm limits, bedtime pass |
| 3 to 8 years | Pavor nocturnus | None beyond reassurance, scheduled awakenings; diazepam (Valium) in extreme cases |
| 6 to 12 years | Nocturnal enuresis | Bed-wetting alarm, continence training, medication |
| 8 to 12 years | Sleepwalking, sleeptalking | Safety precautions |
| Adolescence | Delayed sleep phase syndrome | Setting firm limits, gradual movement of bedtime forward |
| Narcolepsy | Referral | |
| Any age | OSAS | Referral for possible T & A |
DIMS = disorders of initiating and maintaining sleep; OSAS = obstructive sleep apnea syndrome; T & A = tonsillectomy and adenoidectomy.
‘CO-SLEEPING’
Co-sleeping is the term given to parents and children sharing the same bed. Many experts have frowned on this practice because of concerns about possible sexual abuse or interference with developing normal independence. No studies have supported these concerns.
Some contemporary writers actually support co-sleeping, maintaining that this is the predominant pattern in many other cultures and leads to children who feel secure and loved.17,18
No matter how one views this issue, co-sleeping is most likely under-reported by parents, perhaps out of concern that physicians will disapprove of the practice.
Studies have shown that co-sleeping is common. From 35 to 55 percent of preschoolers and 10 to 23 percent of school-aged children sleep with their parents.19 It is a common practice among many ethnic groups; 90 percent of Hispanic homes and 70 percent of African-American homes report co-sleeping. It is an accepted practice among Pacific and Asian cultures as well.20
The U.S. Consumer Product Safety Commission recently published the results of a review of hazards associated with children placed in adult beds. The eight-year survey period contained 515 deaths in children younger than two years. Approximately one fourth of the deaths were due to overlying of the child by someone else sleeping in the bed. Three fourths of the deaths were caused by entrapment in the bed structure leading to suffocation or strangulation.21
Anticipatory Guidance to Facilitate Normal Sleep Patterns
Because of the prevalence of disordered sleep behavior among families with young children, questions about sleep should be incorporated into every well-child visit (Table 3). Physicians should use these moments as a time to let parents know that the development of healthy sleep patterns is as important as good nutritional and dental habits.
TABLE 3 Suggested Questions to Ask Parents About Their Child's Sleeping Pattern
| To bring up the topic as part of a well-child visit: |
| How has your child been sleeping recently? |
| If the parent indicates a problem, with reluctance to go to bed, frequent wakings, early arisings, etc.: |
| What time do you put your child to bed? |
| What is the usual routine in your household between dinner and bedtime? |
| What is your routine in the 30 to 60 minutes before bedtime? |
| What happens when the lights are turned off? |
| When your child cries, how do you respond? How quickly? |
| Does your child get a bottle or get nursed at bedtime? |
| Does your child get a bottle or get nursed in the middle of the night? |
| How many times a night does your child awaken? |
| How do you or your partner respond? |
| How long does it take your child to go back to sleep? |
| What time does your child get out of bed to start the day? |
| Will your child play quietly in bed if he or she is awake before others come to get him or her? |
| Does your child sleep in a crib or a bed? |
| Is the environment in your child's room conducive to sleep (e.g., dark, quiet)? |
| Does your child ever sleep in your bed with you? |
| Does your child sleep with a toy, stuffed animal or favorite blanket? |
| Does your child nap during the day? How often? How long? |
When parents acknowledge a problem, physicians should take a thorough history and determine which strategies the parents have adopted to deal with the problem. Medical causes such as chronic illness, respiratory problems, seizures, recurrent ear infections and the role of medications should be explored. Asking the parents to keep a sleep diary for a week can be helpful.
Parents should be guided to develop clear goals for creating consistent bedtime rituals and patterns of nighttime intervention. They must be given the opportunity to express their misgivings so that they are not sent out with a treatment plan they are unwilling to follow. The physician should offer his or her support or that of the office staff by telephone or through subsequent follow-up office visits.

