
Am Fam Physician. 2001;63(2):288-295
See patient information handout on kidney cysts, written by the authors of this article.
Incidental renal or adrenal masses are sometimes found during imaging for problems unrelated to the kidneys and adrenal glands. Knowledgeable family physicians can reliably diagnose these masses, thereby avoiding unnecessary worry and procedures for their patients. A practical and cost-efficient means of evaluating renal lesions combines ultrasonography and computed tomographic scanning, with close communication between the family physician and the radiologist. Asymptomatic patients with simple renal cysts require no further evaluation. Patients with minimally complicated renal cysts can be followed radiographically. Magnetic resonance imaging is indicated in patients with indeterminate renal masses, and referral is required in patients with symptoms or solid masses. The need for referral of patients with adrenal masses is determined by careful assessment of clinical signs and symptoms, as well as the results of screening laboratory studies and appropriate radiologic studies. Referral is indicated for patients with incidental adrenal masses more than 6 cm in greatest diameter. Appropriate laboratory screening tests include the following: a 24-hour urinary free cortisol measurement for patients with evidence of Cushing's syndrome; a 24-hour urinary metanephrine, vanillylmandelic acid or catecholamine measurement for patients with evidence of pheochromocytoma; and a serum potassium level for patients with evidence of hyperaldosteronism.
The widespread use of abdominal computed tomographic scanning (CT) and ultrasonography has increased the detection of incidental renal and adrenal masses that are found on imaging for problems unrelated to the kidneys or adrenal glands. Based on careful clinical assessment, imaging studies and selected screening laboratory tests, family physicians can diagnose most of these masses and determine the need for referral.
Incidental Renal Masses
Autopsy results have shown that approximately 50 percent of persons older than 50 years have one or more renal cysts.1 Other studies indicate that almost one third of persons in this age group have at least one renal cyst that is identifiable on a CT scan.2 Most of these lesions are benign simple cysts that require no further evaluation, intervention or urologic consultation.
The primary reason to investigate a renal mass is to exclude a malignant neoplasm. One screening study using ultrasound examinations found clinically or pathologically malignant renal tumors in 12 (0.2 percent) of 5,898 consecutive patients 50 to 79 years of age.3 The lifetime risk of renal cell carcinoma in a 40-year-old man is 1.34 percent, and the risk of death is slightly greater than 0.5 percent.4
Renal masses can be broadly categorized into cysts, tumors and inflammatory lesions (Table 1). Although simple cysts are usually asymptomatic, they occasionally cause flank or abdominal pain, a palpable abdominal mass or hematuria. Malignant masses may produce the same symptoms, or they may be associated with paraneoplastic syndromes. Inflammatory lesions are not usually incidental because there is almost always an associated clinical history when symptoms are present. A history of fever, chills or urinary tract infection suggests an infected cyst or an abscess.
| Cysts | Tumors | Inflammatory lesions | |
| Simple | Malignant masses | Infection | |
| Complex | Renal cell carcinoma | Infarction | |
| Multiple | Lymphomas | Trauma (hematoma) | |
| Sarcomas | |||
| Metastases | |||
| Benign masses | |||
| Renal adenomas | |||
| Angiomyolipomas | |||
| Oncocytomas | |||
| Others | |||
With the proper history and interpretation of the renal ultrasonogram and/or CT scan, family physicians can correctly identify the majority of renal masses, which are simple cysts. They can also identify complex cysts and solid masses, which require further evaluation. Probable benign cysts may undergo surveillance, whereas indeterminate or complex cysts should be referred for surgical evaluation.
ULTRASOUND EXAMINATION
Many incidental renal masses are discovered on abdominal ultrasound examinations. Ultrasound criteria for the diagnosis of a simple renal cyst include the following: (1) spherical or ovoid shape; (2) absence of internal echoes; (3) presence of a thin, smooth wall that is separate from the surrounding parenchyma; and (4) enhancement of the posterior wall, indicating ultrasound transmission through the water-filled cyst.5
When the ultrasound criteria for a simple cyst are met, the likelihood of malignancy is extremely small. Asymptomatic patients with incidental renal cysts that meet these criteria require no additional evaluation.
One study showed that ultrasound examination had a sensitivity of 79 percent for the detection of renal parenchymal masses.5 However, this imaging modality did not identify masses less than 5 mm in diameter.
When visualization is inadequate on ultrasound scanning or when the ultrasound examination shows evidence of calcifications, septa or multiple cysts that may obscure a potential malignancy, renal CT scanning with contrast medium should be performed. Symptomatic patients should also be evaluated with renal contrast CT scanning.
CT AND MRI
Incidental renal masses may also be detected on the standard abdominal CT scan. The current “gold standard” for evaluating renal masses requires capturing CT images (5 mm or less in thickness) before and after (no less than 100 seconds) contrast medium is administered. The density of a renal mass is reported in Hounsfield units (H).6,7 The Hounsfield measurements of the relative densities of various substances, including tissues, are presented in Table 2.
| Substance | Hounsfield units (H) |
|---|---|
| Air | −1,000 |
| Fat | −50 |
| Water | 0 |
| Soft tissue (i.e., muscle) | +40 |
| Calculus | +100 to +400 |
| Bone | +1,000 |
In one study, CT scanning had a sensitivity of 94 percent for the detection of renal parenchymal masses, but magnetic resonance imaging (MRI) was statistically superior to CT scanning (P < 0.001) in the correct characterization of benign lesions.5 Thus, MRI may be helpful for further evaluation of an equivocal lesion before an invasive procedure is performed. T2-weighted turbo-spin echo images are especially helpful in providing additional characterization of a lesion.
DIFFERENTIATING BENIGN FROM MALIGNANT LESIONS
| Class I | Simple benign cysts. These lesions are round or oval in shape, are unilocular with the uniform density of water, have no perceptible wall and exhibit no enhancement on radiographs taken after the administration of contrast medium. |
| Class II | Probable benign simple cystic lesions that are minimally complicated These lesions include septated cysts, minimally calcified cysts, infected cysts and high-density cysts. |
| Class III | More complicated cystic lesions. These lesions exhibit some findings seen in malignancy, such as thick, irregular calcifications, irregular borders, multilocular form, thickened or enhancing septa, uniform wall thickening or small nonenhancing nodules. |
| Class IV | Clearly malignant cystic masses. The appearance of these lesions results from necrosis and liquefaction of a solid tumor or a tumor growing in the wall. These lesions are heterogeneous, with a shaggy appearance, thickened walls or enhancing nodules. |
Class I lesions are simple benign cysts that require no further evaluation unless signs or symptoms develop. Class II lesions are also benign. These cysts, which are minimally complicated by previous infection or hemorrhage, can be followed radiographically. Class III lesions are “indeterminate” and have a malignancy rate of 50 percent9; hence, surgical exploration of these lesions is warranted in otherwise healthy patients. Class IV cystic lesions and solid renal masses that enhance with contrast medium are presumed to be malignant.
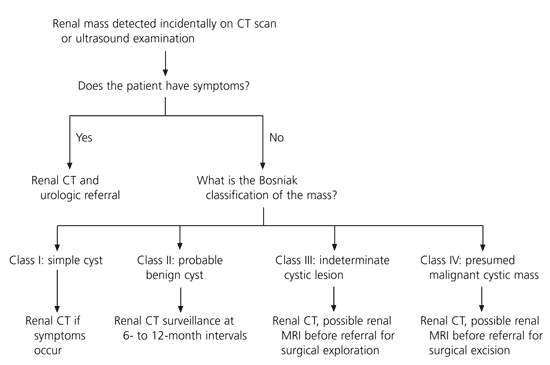
The CT criteria for a renal mass to be called a Bosniak class I cyst include the following: uniform density of no greater than 20 H (assigned density of water is 0 H, with a range of−20 to +20 H5), no enhancement of the mass on radiographs obtained after the administration of contrast medium (i.e., no increase in the Hounsfield units) and round or oval shape with no perceptible wall. Bosniak class I cysts constitute the majority of incidental renal masses and require no additional evaluation or treatment. Rarely, some patients with large simple cysts may become symptomatic. Patients with symptoms should be referred to a urologist for discussion of the risks, benefits and nature of possible interventions (Figure 1).
Class II cysts have three distinct features: one or two nonenhancing septa, calcifications in the wall or septum, and hyperdense contents (50 to 90 H) resulting from the presence of blood, protein or colloid. These lesions should not enhance with contrast medium. In addition, they should be smaller than 3 cm in greatest diameter and should otherwise have the appearance of benign simple cysts. Bosniak8 did not recommend follow-up for lesions that fulfill these criteria. However, care should be taken in evaluating probable benign simple cysts, and surveillance seems prudent because there is a small chance that these cysts will develop into renal cell carcinomas.
Class III lesions are cystic masses with any or all of the following features: thick, irregular borders, irregular calcifications, thickened or enhancing septa and multilocular form. These lesions are difficult to distinguish from a renal cell carcinoma, which may have a cystic appearance. In four reviews, 12 of 29 class III lesions proved to be malignant.9 MRI may help to better characterize these lesions before urologic referral for potential surgical exploration and close follow-up.
Class IV lesions are malignant-appearing heterogeneous cysts with shaggy, thickened walls or enhancing nodules. Their unequivocal malignant appearance results from solid tumor necrosis and liquefaction. The diagnosis of these lesions is usually straightforward, and surgical excision is indicated.
Incidental Adrenal Masses
Incidental adrenal masses are also being discovered more frequently on CT scanning and ultrasound examinations. Most adrenal masses are detected first on abdominal CT scans, with an incidence of 0.6 to 1.3 percent on such scans.11 The vast majority of asymptomatic adrenal masses are benign, and patients with these lesions do not require subspecialist referral or treatment.12 The differential diagnosis of incidental adrenal masses, summarized from studies in the literature, is provided in Table 4.13
| Mass | Number (%) |
|---|---|
| Adenoma | 107 (51) |
| Metastatic cancer | 64 (31) |
| Adrenal cancer | 9 (4) |
| Cyst | 9 (4) |
| Pheochromocytoma | 9 (4) |
| Hyperplasia | 4 (2) |
| Lipoma | 3 (2) |
| Myelolipoma | 3 (2) |
The two most important factors in the diagnostic work-up are the lesion's size and “functioning.” The size of an adrenal mass is important: lesions larger than 6 cm in greatest diameter are more likely to be malignant.14 Even at a threshold size of 6 cm, it has been estimated that more than 60 adrenalectomies would have to be performed to remove one adrenal carcinoma.15
To determine whether an adrenal mass is functioning, the patient should be assessed for signs and symptoms of Cushing's syndrome, pheochromocytoma or hyperaldosteronism. Cushing's syndrome is characterized by hypertension, moon-shaped face, proximal muscle weakness, truncal obesity, buffalo hump, thin skin, abdominal striae and easy bruising. Classic features of pheochromocytoma include paroxysmal hypertension, headache, sweating and palpitations. Hypertension, hypokalemia and hypernatremia characterize hyperaldosteronism.
In 1990, a team of investigators16 proposed a screening endocrine laboratory evaluation of adrenal masses that is sensitive and cost-effective (Figure 2 and Table 5). The serum potassium level is used to screen for hyperaldosteronism in patients with hypertension. Measurement of 24-hour urinary metanephrine, vanillylmandelic acid or catecholamines is used to screen for pheochromocytoma. Because urinary catecholamine measurements have a higher false-negative rate for pheochromocytoma, some investigators have proposed the addition of plasma catecholamine measurements. It seems reasonable to add plasma catecholamine measurements to the screening endocrine evaluation because even though pheochromocytoma is rare, it can be a potentially life-threatening problem.

| Cause | Signs or symptoms | Screening test |
|---|---|---|
| Cushing's syndrome | Hypertension, moon-shaped face, buffalo hump, striae, proximal muscle weakness, truncal obesity, thin skin, easy bruising | 24-hour urinary free cortisol measurement or dexamethasone suppression test |
| Pheochromocytoma | Hypertension, headache, diaphoresis, palpitations | 24-hour urinary metanephrine, vanillyl mandelic acid or catecholamine measurement |
| Hyperaldosteronism | Hypertension, hypokalemia, hypernatremia | Serum potassium level |
The best initial screening test for Cushing's syndrome is the 24-hour urinary free cortisol measurement.17 Although some authors16 do not support screening for Cushing's syndrome in the absence of clinical signs or symptoms, other investigators recommend routine measurement of 24-hour urinary free cortisol levels in all patients with incidental adrenal masses. Additional evaluation with a dexamethasone suppression test is warranted if Cushing's syndrome is suspected, a patient has signs or symptoms of the syndrome or the results of the 24-hour urinary free cortisol measurement are equivocal.
Laboratory screening for adrenal carcinoma using urinary 17-ketosteroid measurements is not advised because the test lacks sensitivity and specificity. Furthermore, adrenal cancer is rare.
Patients with a mass larger than 3 cm in greatest diameter, normal screening laboratory tests and no clinical signs or symptoms of adrenal disease can be followed by their family physician. Reasonable surveillance includes a CT scan or ultrasound examination in three months, and then every six months for two years.18
REFERRAL OF PATIENTS WITH AN INCIDENTAL ADRENAL MASS
Referral is required for patients with an incidental adrenal mass larger than 3 cm if a change in the size of the lesion is noted on serial radiographic studies. Referral for surgical removal is required for all patients with adrenal masses larger than 6 cm because of the possibility of malignancy. Patients with masses between 3 and 6 cm in greatest diameter should undergo an MRI study and additional endocrine evaluation; referral may be advised.
Patients with abnormal screening laboratory results should be referred, regardless of the size of the mass, because hormone-producing tumors need to be surgically excised. Lastly, all patients with a history of a malignancy who are found to have an adrenal mass probably should undergo needle biopsy of the lesion because metastatic disease is the most likely pathology in this situation.19