Paronychia is one of the most common infections of the hand. Clinically, paronychia presents as an acute or a chronic condition. It is a localized, superficial infection or abscess of the paronychial tissues of the hands or, less commonly, the feet. Any disruption of the seal between the proximal nail fold and the nail plate can cause acute infections of the eponychial space by providing a portal of entry for bacteria. Treatment options for acute paronychias include warm-water soaks, oral antibiotic therapy and surgical drainage. In cases of chronic paronychia, it is important that the patient avoid possible irritants. Treatment options include the use of topical antifungal agents and steroids, and surgical intervention. Patients with chronic paronychias that are unresponsive to therapy should be checked for unusual causes, such as malignancy.
Paronychia is one of the most common infections of the hand. Paronychias are localized, superficial infections or abscesses of the perionychium (epidermis bordering the nails). Paronychial infections develop when a disruption occurs between the seal of the proximal nail fold and the nail plate that allows a portal of entry for invading organisms.
Noninfectious causes of paronychia include contact irritants and excessive moisture. Clinically, paronychia presents as an acute or chronic (longer than six weeks' duration) condition. People with occupations such as baker, bartender and dishwasher seem predisposed to developing chronic paronychia. Treatment may consist of warm-water soaks, antimicrobial therapy or surgical intervention.
Nail Anatomy
Components of the nail complex include the nail bed (matrix), the nail plate and the perionychium. The nail bed lies beneath the nail plate and contains the blood vessels and nerves. Within the nail bed is the germinal matrix, which is responsible for the production of most of the nail volume, and the sterile matrix. This matrix is the “root” of the nail, and its distal portion is visible on some nails as the half-moon–shaped structure called the lunula.1 The nail plate is hard and translucent, and is composed of dead keratin.2 The plate is surrounded by the perionychium, which consists of proximal and lateral nail folds, and the hyponychium, the area beneath the free edge of the nail1 (Figure 1).
FIGURE 1.
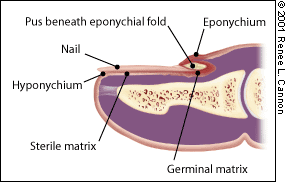
Anatomy of a nail
Acute Paronychia
Acute paronychia most commonly results from nail biting, finger sucking, aggressive manicuring, a hang nail or penetrating trauma, with or without retained foreign body3 (Figure 2). Sculptured fingernail (artificial nail) placement has also been shown to be associated with the development of paronychia.4 The most common infecting organism is Staphylococcus aureus, followed by streptococci and pseudomonas organisms. Gram-negative organisms, herpes simplex virus, dermatophytes and yeasts have also been reported as causative agents. Children are prone to acute paronychia through direct inoculation of fingers with flora from the mouth secondary to finger sucking and nail biting. This scenario is similar to the acquisition of infectious organisms following human bites or clenched-fist injuries.5
FIGURE 2.
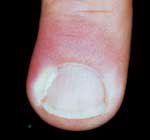
Acute paronychia.
CLINICAL PRESENTATION
Patients with acute paronychia may report localized pain and tenderness of the perionychium. Symptoms may arise spontaneously, or following trauma or manipulation of the nail bed. The perionychial area usually appears erythematous and inflamed, and the nail may appear discolored and even distorted. If left untreated, a collection of pus may develop as an abscess around the perionychium. Fluctuance and local purulence at the nail margin may occur, and infection may extend beneath the nail margin to involve the nail bed. Such an accumulation of pus can produce elevation of the nail plate (Table 1).6
TABLE 1 Comparison of Acute and Chronic Paronychia
| Features | Acute | Chronic |
|---|---|---|
| Clinical appearance | Red, hot, tender nail folds, with or without abscess | Swollen, tender, red (not as red as acute), boggy nail fold; fluctuance rare |
| People at high risk | People who bite nails, suck fingers, experience nail trauma (manicures) | People repeatedly exposed to water or irritants (e.g., bartenders, housekeepers, dishwashers) |
| Pathogens | Staphylococcal aureus, streptococci, Pseudomonas, anaerobes | Candida albicans (95 percent), atypical mycobacteria, gram-negative rods |
| Treatment | Warm soaks, oral antibiotics (clindamycin [Cleocin] or amoxicillin–clavulanate potassium [Augmentin]); spontaneous drainage, if possible; surgical incision and drainage | Avoidance of water and irritating substances; use of topical steroids and antifungal agents; surgery as last resort |
Information from Jebson PJ. Infections of the fingertip. Paronychias and felons. Hand Clin 1998;14:547–55.
TREATMENT
Conservative treatment, such as warm-water soaks three to four times a day, may be effective early in the course if an abscess has not formed.3 If infection persists, warm soaks in addition to an oral antistaphylococcal agent and splint protection of the affected part are indicated. Children who suck their fingers and patients who bite their nails should be treated against anaerobes with antibiotic therapy. Penicillin and ampicillin are the most effective agents against oral bacteria. However, S. aureus and Bacteroides can be resistant to these antibiotics. Clindamycin (Cleocin) and the combination of amoxicillin–clavulanate potassium (Augmentin) are effective against most pathogens isolated from these infections.5,7 First-generation cephalosporins are not as effective because of resistance of some anaerobic bacteria and Escherichia coli.5 Some authorities recommend that aerobic and anaerobic cultures be obtained from serious paronychial infections before antimicrobial therapy is initiated.5
When abscess or fluctuance is present, efforts to induce spontaneous drainage or surgical drainage become necessary. If the paronychia is neglected, pus may spread under the nail sulcus to the opposite side, resulting in what is known as a “run-around abscess.”8 Pus may also accumulate beneath the nail itself and lift the plate off the underlying matrix. These advanced cases may require more complex treatment, including removal of the nail to allow adequate drainage.
SURGICAL TREATMENT
As in the treatment of any abscess, drainage is necessary. It should be performed under digital block anesthesia unless the skin overlying the abscess becomes yellow or white, indicating that the nerves have become infarcted, making the use of a local anesthetic unnecessary.9 The nail fold containing pus should be incised with a no. 11 or no. 15 scalpel with the blade directed away from the nail bed to avoid injury and subsequent growth abnormality6 (Figure 3). After the pus is expressed, the abscess should be irrigated and packed with a small piece of plain gauze. An oral antibiotic agent should be prescribed. The dressing should be removed in 48 hours, followed by the initiation of warm soaks four times a day for 15 minutes.
FIGURE 3
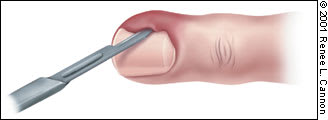
Incision of a paronychia with blade directed away from the nail.
If the nerves have infarcted, anesthesia may not be required for surgical intervention.8 In this case, the flat portion of a no. 11 scalpel should be gently placed on top of the nail with the point of the blade directed toward the center of the abscess. The blade should be guided slowly and gently between the nail and the eponychial (cuticle) fold so that the tip of the blade reaches the center of the most raised portion of the abscess. Without further advancement, the scalpel should be rotated 90 degrees, with the sharp side toward the nail, gently lifting the eponychium from its attachment to the nail. At this point, pus should slowly extrude from the abscessed cavity. Because the skin is not cut, no bleeding should occur. Drains are not necessary. Warm-water soaks four times a day for 15 minutes should be performed to keep the wound open. Between soakings, an adhesive bandage can protect the nail area. Antibiotic therapy is usually not necessary.9 Recurrent acute paronychia may lead to the development of chronic paronychia.
Chronic Paronychia
Chronic paronychia resembles acute paronychia clinically, but the cause is multi-factorial. Chronic paronychia is usually non-suppurative and is more difficult to treat. People at risk of developing chronic paronychia include those who are repeatedly exposed to water containing irritants or alkali, and those who are repeatedly exposed to moist environments. Persons at high risk include bartenders, housekeepers, homemakers, dishwashers and swimmers, as well as diabetic and immunosuppressed persons. In addition, metastatic cancer, subungual melanoma and squamous cell carcinoma may present as chronic paronychia. Breast cancer metastasized to the lateral nail fold of the great toe has been reported.3 Therefore, benign and malignant neoplasms should always be ruled out when chronic paronychias do not respond to conventional treatment.3,8,10
CLINICAL PRESENTATION
Chronic paronychia usually causes swollen, red, tender and boggy nail folds (Figure 4). Symptoms are classically present for six weeks or longer.11 Fluctuance is rare, and there is less erythema than is present in acute paronychia. Inflammation, pain and swelling may occur episodically, often after exposure to water or a moist environment. Eventually, the nail plates become thickened and discolored, with pronounced transverse ridges.6,8 The cuticles and nail folds may separate from the nail plate, forming a space for various microbes, especially Candida albicans, to invade.8 A wet mount with potassium hydroxide from a scraping may show hyphae, or a culture of the purulent discharge may show hyphae for bacteria and fungal elements. C. albicans may be cultured from 95 percent of cases of chronic paronychia.6 Other pathogens, including atypical mycobacteria, gram-negative rods and gram-negative cocci, have also been implicated in chronic paronychia (Table 1).6
FIGURE 4.
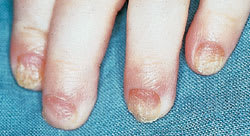
Chronic paronychia.
TREATMENT
Treatment of chronic paronychia primarily involves avoiding predisposing factors such as exposure to irritating substances, prolonged exposure to water, manicures, nail trauma and finger sucking. When it is necessary to wear vinyl gloves, cotton gloves should be worn underneath.3,10 Treatment with a combination of topical steroids and an antifungal agent has been shown to be successful.3,7 Oral antifungal therapy is rarely necesssary.3 Treatment of potential secondary bacterial infections with antibacterial solutions or ointments, acetic acid soaks (1:1 ratio of vinegar to water) or oral antibiotics may be necessary. Surgical intervention is indicated when medical treatment fails. Excellent results have been reported with the use of an eponychial marsupialization technique, as well as removal of the entire nail and application of an antifungal-steroid ointment to the nail bed.3,6,8

