Clinical Scenario
A 36-year-old man presents with a productive cough of two days' duration with no evidence of sinusitis or pneumonia.
Clinical Question
Should clinicians treat this patient, who has classic symptoms of acute bronchitis, with antibiotics?
Evidence-Based Answer
While there is evidence that antibiotics offer a slight benefit to patients with acute bronchitis, there is not a compelling reason to treat this patient with antibiotics.
Cochrane Critique
Acute bronchitis is the recent onset of a productive cough in a patient without chronic obstructive pulmonary disease, sinusitis or pneumonia. Becker and colleagues,1 in their Cochrane meta-analysis, came to the conclusion that antibiotic therapy minimally helps patients with acute bronchitis. The trials included male and female adults and some children eight years of age and older, as well as smokers and nonsmokers. While this meta-analysis looked at many outcomes, the mild benefit is best illustrated by this example: antibiotics decreased sputum production by one-half day (Figure 1*). Based on this systematic review, should clinicians recommend antibiotics to patients with acute bronchitis?
Cochrane Abstract
Objectives. People with acute bronchitis may show little evidence of bacterial infection. If effective, antibiotics could shorten the course of the disease. However, if they are not effective, the risk of antibiotic resistance may be increased. The objective of this review was to assess the effects of antibiotic treatment in patients with a clinical diagnosis of acute bronchitis.
Search Strategy. The authors searched MEDLINE, Embase, reference lists of articles, personal collections up to 1996 and Scisearch from 1989 to 1996.
Selection Criteria. Randomized trials comparing any antibiotic therapy with placebo in acute bronchitis.
Data Collection and Analysis. At least two reviewers extracted data and assessed trial quality.
Primary Results. The results of eight trials involving 750 patients from eight years of age to 65 and older and including smokers and nonsmokers were included. The quality of the trials was variable. A variety of outcome measures was assessed. In many cases, only outcomes that showed a statistically significant difference between groups were reported.
Overall, patients taking antibiotics had slightly better outcomes than those taking placebo. They were less likely to report feeling unwell at a follow-up visit (odds ratio, 0.42; 95 percent confidence interval [CI] 0.22 to 0.82), to show no improvement on physician assessment (odds ratio, 0.43; CI, 0.23 to 0.79) or to have abnormal lung findings (odds ratio, 0.33; CI, 0.13 to 0.86), and had a more rapid return to work or usual activities (weighted mean difference, 0.7 days earlier; CI, 0.2 to 1.3). Antibiotic-treated patients reported significantly more adverse effects (odds ratio, 1.64; CI, 1.05 to 2.57), such as nausea, vomiting, headache, skin rash or vaginitis.
Reviewers' Conclusions. Antibiotics appear to have a modest beneficial effect in the treatment of acute bronchitis, with a correspondingly small risk of adverse effects. The benefits of antibiotics may be overestimated in this analysis because of the tendency of published reports to include complete data only on outcomes found to be statistically significant.1 and older, as well as smokers and nonsmokers. While this meta-analysis looked at many outcomes, the mild benefit is best illustrated by this example: antibiotics decreased sputum production by one-half day (Figure 1 *). Based on this systematic review, should clinicians recommend antibiotics to patients with acute bronchitis1
These summaries have been derived from Cochrane reviews published in the Cochrane Database of Systematic Reviews in the Cochrane Library. Their content has, as far as possible, been checked with the authors of the original reviews, but the summaries should not be regarded as an official product of the Cochrane Collaboration; minor editing changes have been made to the text (http://www.cochrane.org)
Did the authors address a focused clinical question?
Yes.
Were the criteria used to select articles for inclusion appropriate?
Yes—randomized, placebo-controlled clinical trials.
Is it likely that important relevant articles were missed?
No—except unpublished data.
Was the validity of the individual articles appraised?
Yes—using standard criteria.
Were the assessments of studies reproducible?
Yes—measured kappa statistic of 0.71.
Were the results similar from study to study?
Yes.
To answer this question, clinicians need to evaluate the merits of the Cochrane review, place it in the context of other relevant literature and use their own clinical judgment. In a sound approach to this process, the following series of questions are answered2,3:
WHAT WERE THE OVERALL RESULTS OF THE REVIEW?
The benefit of antibiotics in treating acute bronchitis was quite small. It was, however, evident in several outcomes. To cause one patient to feel better at a seven- to 14-day follow-up visit, six patients had to be treated with antibiotics (Figure 2*). To have a physician assess one patient as improved at the same follow-up visit, 13 patients had to be treated.
FIGURE 1. Review: Antibiotics for acute bronchitis
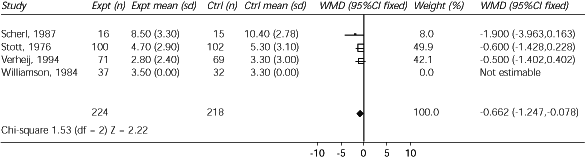
Comparison: Any antibiotic vs. placebo
Outcome: Days of sputum
Outcome in terms of days of sputum production in a comparison of antibiotics versus placebo in the treatment of acute bronchitis. (expt = experiment; n = number; sd = standard deviation; ctrl = control; WMD = weighted mean difference; CI = confidence interval; df = degrees of freedom; Z = standard deviation)
FIGURE 2. Review: Antibiotics for acute bronchitis
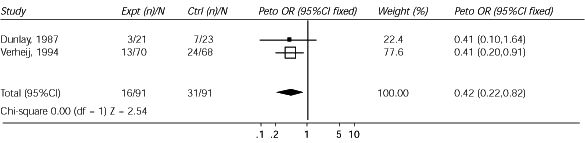
Comparison: Any antibiotic vs. placebo
Outcome: Feeling unwell at follow-up visit
Outcome in terms of feeling unwell at follow-up visit in a comparison of antibiotics versus placebo in the treatment of acute bronchitis. (expt = experiment; n = number; N = study population; ctrl = control; Peto OR = Peto odds ratio; CI = confidence interval; df = degrees of freedom; Z = standard deviation)
FIGURE 3. Review: Antibiotics for acute bronchitis
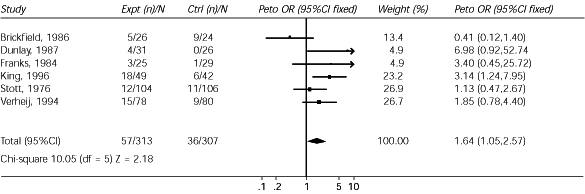
Comparison: Any antibiotic vs. placebo
Outcome: Adverse effects
Outcome in terms of adverse effects in a comparison of any antibiotic versus placebo in the treatment of acute bronchitis, (expt = experiment; n = number; N = study population; ctrl = control; Peto OR = Peto odds ratio; CI = confidence interval; df = degrees of freedom; Z = standard deviation)
Figures 1 through 3 reprinted with permission from Becker L, Glazier R, McIsaac W, Smucny J. Antibiotics for acute bronchitis (Cochrane Review). In: The Cochrane Library, Issue 3,1999. Oxford: Update Software.
Becker and colleagues1 found similarly small benefits in terms of decreasing daytime cough at a follow-up visit, days of sputum production (0.6 fewer days), less impairment of activities (0.7 fewer days), degree of chest congestion, taking cold or cough medicines, and abnormal lung examination results. Interestingly, there was no statistical difference in days of cough, days of daytime cough, days of nighttime cough, productive cough at a follow-up visit, amount of sputum production, limitation of work activities at a follow-up visit, days of fever, purulent sputum at follow-up, sore throat or lower respiratory infections in the next six months. Strangely, there was a small decrease in both upper and the combination of upper and lower respiratory tract infections in the next six months.
The only outcome that demonstrated a statistically significant detriment in the antibiotic-treated group was adverse medication side effects (Figure 3*). These adverse effects were mainly gastrointestinal (nausea and vomiting), and also included headache, rash and vaginitis. The number needed to harm, while not reported, can be calculated to be 15 (using data from Becker and colleagues1 and a standard formula). Thus, while the beneficial effect of antibiotics was small, the side effects were also small.
HOW PRECISE WERE THE RESULTS?
The results were reasonably, but not highly, precise. Some of the studies listed only outcomes with a statistically significance difference. Many of the outcomes analyzed were reported in only two or three of the eight included trials. This discrepancy limited the power of the meta-analysis. One solution to this problem that the authors did not select would have been to convert similar outcomes into an effect size and then perform the meta-analysis. Even with these limitations, the methodology of the analysis was strong and well constructed.
CAN THE RESULTS BE APPLIED TO PATIENT CARE?
Yes, if the patient is eight years of age or older and meets the definition of acute bronchitis in the first paragraph of this critique.
DO THE CONCLUSIONS MAKE BIOLOGIC AND CLINICAL SENSE?
It is certainly reasonable that a subset of patients with acute bronchitis would have a bacterial infection that is amenable to antibiotic therapy. In one of the trials, subgroup analysis correlated positive sputum Gram stains with a favorable response to antibiotics.4 Thus, it makes biologic sense. However, does it make clinical sense to treat patients who have acute bronchitis with antibiotics? To answer this question, clinicians must weigh the benefits and the cost of treatment.
ARE THE BENEFITS WORTH THE HARM AND THE COST?
It is not clear that the small benefit in patients treated with antibiotics outweighs a number of costs and harms. First, there is a similarly small risk of adverse effects associated with antibiotic use. Second, there is the direct cost of the medicine. Third, there is the indirect cost of reinforcing the need of patients to seek medical care for any productive cough. Finally, and most importantly, the use of antibiotics is associated with a significant risk of increased antibiotic drug resistance. This resistance is potentially dangerous to the person receiving the antibiotics and to the broader society.5
Reading the Numbers
| The number needed to treat (NNT) represents the number of patients a doctor would have to treat to benefit one patient over a specified length of time. It is calculated as one divided by the absolute risk reduction. |
| Ideally, every treatment would have an NNT of one; that would mean that every patient treated benefits from treatment. However, most treatments are not that effective. |
| A reasonable NNT depends on the risks and costs of the treatment and the degree of benefit. For example, we might accept a higher NNT if the benefit is saving a life than if the benefit is allowing someone to return to work 0.7 days sooner. This is especially true if the treatment has real risks, such as allergic reactions or side effects. Even if the treatment is shown to be effective, the adverse effects might not justify its use. |
Discussion
It is important to consider whether the results of this Cochrane meta-analysis are consistent with results in other related literature. The meta-analysis by Becker and colleagues1 is quite similar to two other recently published meta-analyses.6,7 The latter studies calculated an effect size and then converted back to a clinical measure. They showed that patients taking antibiotics for treatment of acute bronchitis reduced the duration of productive cough by about one-half day. Both studies had the benefit of including more trials in their calculations. These corroborating studies make more compelling the idea that antibiotic therapy makes a small difference in the course of acute bronchitis.
Given the consistency in results between the eight clinical trials, despite the use of three different antibiotics, it is not clear that the type of antibiotic is critical. Choosing an antibiotic with a spectrum similar to what doxycycline, trimethoprim-sulfamethoxazoleand erythromycin had in the 1970s and 1980s would be most consistent with the trial results.
Additional research in several areas may help to clarify some remaining questions. It is important to identify subsets of patients who are more likely to respond to antibiotic therapy.4,8 A cost-benefit analysis could also help provide quantitative data on the price of treating and not treating acute bronchitis. New modalities in the treatment of acute bronchitis, such as bronchodilators, should be compared with antibiotic therapy.9–11
Employment of antibiotics for the treatment of acute bronchitis is another area where clinicians should use their own judgment and involve the patient in an informed discussion. While there is evidence showing a small benefit from treating acute bronchitis with antibiotics, the need to do so is not compelling when the disadvantages of treatment are considered.

