Several effective and inexpensive over-the-counter treatments are available for minor but troubling foot problems. In most cases, one week of therapy with topical terbinafine is effective for interdigital tinea pedis. Treatment of plantar warts with 17 percent salicylic acid with lactic acid in a collodion base is as effective as cryotherapy, but treatment must be sustained for several months. Toe sleeves and toe spacers can relieve pain from hard or soft corns. Metatarsal pads can relieve the pressure associated with plantar keratoses. Heel cups often can relieve pain caused by age-related thinning of the heel fat pad. Plantar fasciitis is a common cause of anteromedial heel pain caused by repetitive strain on the plantar fascia. Although the mainstay of therapy is stretching exercises, ready-made arch supports and insoles can be helpful adjuncts.
Minor but troubling foot problems are common complaints in primary care. In one series,1 71 percent of elderly patients reported foot problems that impaired their function, and 39 percent had consulted their physician about the problems. A variety of products are available over-the-counter for the treatment of common foot problems, such as athlete's foot, onychomycosis, foot pain, corns, warts and bunions. Several of these products are cost-effective alternatives to office-based or prescription treatments, but others have yet to be proven beneficial. This article reviews the efficacy of several widely available over-the-counter foot remedies for minor foot problems. Foot care for patients with severe orthopedic or systemic disease, including the care of the diabetic or vascularly compromised foot, is beyond the scope of this article.
Properly Fitted Shoes
Ill-fitting shoes can contribute to abnormal foot mechanics and areas of excessive pressure. When a patient presents with foot pain, bunions, corns or plantar warts, the physician should instruct them in how to choose properly fitting shoes. (Although papillomavirus is the etiologic factor in plantar warts, they tend to occur in areas where the foot is subjected to excess pressure.) An important component in the treatment of foot problems is finding properly-fitting shoes, because they contribute to symptom relief and help prevent recurrences. Table 1 lists instructions for proper shoe fitting.
Antifungal Agents
Tinea pedis, generally known as athlete's foot, is a fungal infection of the skin of the foot. Heat and dampness are predisposing factors. Diffuse involvement of the entire sole of the foot and dorsal surfaces of the foot is called moccasin-type tinea pedis and often requires systemic antifungal therapy (Table 22–11 ). However, interdigital tinea pedis, which presents as cracking and maceration in the interdigital spaces, responds well to topical antifungal agents (Table 22–11 ).
TABLE 1 Guidelines for Proper Shoe Fit
| Properly fitted shoes do not need to be broken in, but instead should be comfortable to wear right out of the box. |
| Shoes should be fitted on both feet during weight bearing, preferably at the end of the day when the feet are most swollen. |
| Allow a space of one-half inch between the end of the shoe and the longest toe. In athletic shoes, allow up to one inch. |
| Check the width. Adequate room should be allowed across the ball of the foot. The first metatarsophalangeal joint should be in the widest part of the shoe. |
| The heel should fit snugly. |
| The fit over the instep should be checked. A shoe that laces allows for adjustment of this area. |
| Orthotics and inserts will change the fit of shoes. A patient who plans to use an orthotic should fit the shoes while wearing the orthotic. |
Five antifungal antibiotics are widely available in cream form without a prescription: clotrimazole (Lotrimin), miconazole (Moni-stat-Derm), terbinafine (Lamisil AT), tolnaftate (Tinactin) and undecylenic acid (Desenex). Results of controlled studies2,3,12,13 have demonstrated that all of these agents have high rates of mycologic cure and symptom relief. All are used once or twice daily for four weeks, except terbinafine which is effective with one week of therapy in 88 to 97 percent of cases.
TABLE 2 Remedies for Common Foot Problems
| Problem | Remedy |
|---|---|
| Interdigital tinea pedis | Topical terbinafine (Lamisil AT, $16 for a 30-g tube)2,3 |
| Moccasin tinea pedis | Systemic antifungal therapy |
| Simple plantar warts | 17 percent salicylic acid in flexible collodion (Duofilm, Compound W,4,5 Wart-Off, $9 to $30 per oz) daily for six to 12 weeks. Relieve excess pressure with proper shoe fit and pads, if indicated. |
| Mosaic plantar warts4 | Difficult to cure. Salicylic acid paint is as effective as other treatments. |
| Corns | Properly fitting shoes Paring and curettage by physician or podiatrist Cushions, toe sleeves ($3 to $5) Lamb's wool padding ($5 per 3/8 oz) |
| Heel pain | Heel cups6 ($3 to $10 per pair) |
| Plantar fasciitis | Stretching exercises7–9 Closed-cell foam shoe insert10,11 with arch support is often helpful ($8 to $20 per pair). |
Although a 30-g tube of terbinafine cream costs considerably more than any of the other agents mentioned, a single tube is sufficient for the recommended treatment duration. The other agents mentioned often require the use of multiple tubes, resulting in higher overall cost. Topical terbinafine is a logical first-line choice for the treatment of tinea pedis. Although no direct comparative studies have been performed, terbinafine has a similar mycologic cure rate to prescription-only topical butenafine 1 percent cream (Mentax).
Foot hygiene is an important part of the treatment of tinea pedis. All studies show cure rates of 30 to 40 percent in patients using a placebo, which is most likely caused by hygiene measures (study protocols usually include twice-daily washing and drying of the feet) and the mild antifungal activity in the cream vehicle used for the placebo.
The antifungals tolnaftate and miconazole are also marketed in spray form for the prevention of athlete's foot. In a 12-week study14 in a prison population, 88 percent of the subjects treated with tolnaftate spray prophylaxis were free of tinea pedis compared with 69 percent of subjects treated with unmedicated talc and 50 percent of untreated control subjects. In a primary care population, there is no evidence that daily prophylaxis with antifungals is cost-effective compared with treating tinea pedis as it occurs.
Tea tree oil (an essential oil derived from the Australian Melaleuca alternifolia) is also marketed for the treatment of athlete's foot. Results of a study15 found that tea tree oil was comparable with tolnaftate in reducing the symptoms of tinea pedis, but no more effective than placebo at achieving mycologic cure.
Several over-the-counter topical products are marketed for the treatment of onychomycosis. However, we were unable to find any studies concerning the effectiveness of topical agents for this purpose.
Wart Treatments
Several brands of 17 percent salicylic acid combined with lactic acid in a base of flexible collodion are available (e.g., Duofilm, Compound W, Wart-Off) for the treatment of warts (Table 22–11 ). Results of one study4 showed no significant difference in cure rate of hand warts between the 17 percent salicylate paint and cryotherapy with liquid nitrogen alone or combined. In the treatment of simple plantar warts, 17 percent salicylic acid paint cured 84 percent of patients in a referral population4 and 76 percent of patients in a small primary care case series.5 Patients should be informed that daily application of acid paint is required for two to three months for complete eradication of warts.
Mosaic plantar warts are clusters of small plantar warts that are resistant to treatment. Salicylic acid paint has a similar cure rate for mosaic plantar warts (45 percent), compared with more expensive treatments such as 10 percent glutaraldehyde, 40 percent benzalkonium chloride dibromide and 5 percent fluorouracil (Table 22–11 ).4 No studies were found that directly compared acid paint with cryotherapy in the treatment of mosaic plantar warts. Salicylic acid is also available in a 40 percent plaster for the treatment of plantar warts (Sal-Acid, Mediplast), but we were unable to locate any studies concerning the efficacy of this form of treatment.
Corn Plasters, Corn Cushions and Metatarsal Pads
A corn is a hyperkeratotic nodule that is caused by excessive pressure on the foot. Soft corns are keratin nodules between the toes (most often the fourth and fifth toes) that have become macerated by perspiration and are extremely tender. Soft corns can be difficult to distinguish from interdigital tinea pedis. When hyperkeratotic nodules occur on the sole of the foot, they are called plantar keratoses or clavi (Figure 1). Corns frequently are tender and have a clear, hard keratin center when shaved. These features help differentiate corns from warts, which are not very tender and bleed from multiple capillary loops when shaved.
Treatment of corns involves the removal of excess keratin and the relief of pressure. A physician or podiatrist may remove hard corns by paring with a sterile blade, followed by curettage of the keratin core (Table 22–11 ).
Corn plasters are felt pads that contain 40 percent salicylic acid. Although salicylate is keratolytic and may be an effective treatment for corns, no studies of the effectiveness of plasters for the treatment of corns are available for review.
FIGURE 1.
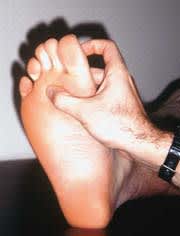
The area over the third metatarsal head (indicated by the examiner's thumb) is a common site for plantar keratoses. A grease pencil or lipstick mark on this area of the foot can help locate the exact spot in the shoe to place a metatarsal pad.
Placing a metatarsal pad (Figure 2) in the shoe16 will relieve pressure on the plantar metatarsal heads and may help prevent recurrence of plantar keratoses. After marking the nodule with lipstick or a grease pencil, have the patient step barefoot into the shoe. The pad should be placed proximal to the mark made on the insole of the shoe. Metatarsal pads can also be used to change the alignment of the toes to relieve pressure on soft corns.
FIGURE 2.

Two types of commonly available self-adhesive metatarsal pads are shown. Pads should be placed proximal to the point of contact between the plantar keratosis and the shoe.
Shoes with wide, deep toe boxes help prevent recurrence of hard corns on the dorsal surfaces of the toes, and wide toe boxes help relieve soft corns. Pressure on toes may be relieved with Silipos toe sleeves, polymer gel (e.g., Cushlin Gel), or with padding of foam or lamb's wool. Lamb's wool is preferred over cotton padding because it does not retain moisture and does not compress (Table 22–11 ).
FIGURE 3.
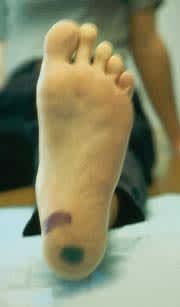
The blue mark indicates the location of tenderness in heel pain caused by thinning of the heel fat pad. The red mark indicates the typical point of maximal tenderness in plantar fasciitis.
Insoles, Orthotics and Arch Supports
Ready-made insoles are marketed for relief of heel pain, foot pain and back pain. In a small crossover study,17 73 percent of subjects reported decreases in back, leg and foot pain caused by prolonged standing on the job with the use of viscoelastic polyurethane insoles. There is some evidence that metatarsal pads18 and closed-cell foam insoles19 are useful in the relief of metatarsalgia.
Elderly patients may suffer from heel pain caused by age-related thinning of the heel fat pad. In contrast to plantar fasciitis, age-related heel pain is greatest in the center of the heel, and is usually not present on arising in the morning (Figure 3). Heel pads or heel cups (Table 22–11 ) may help relieve acute symptoms in patients with heel pain (Figure 4). Heel pads may also benefit patients who stand on hard surfaces for extended periods of time.7 Hard and soft heel cups have been used with success. Hard cups contain the heel pad beneath the calcaneus and help to restore some of its compressibility, while soft cups add cushioning in addition to containing the fat pad.6
Patients with plantar fasciitis present with heel pain, but on examination the anterome-dial aspect of the heel at the origin of the plantar fascia on the calcaneus will be more tender than the central area (Figure 3). Plantar fasciitis is not limited to the elderly and it frequently occurs in athletes. Patients may report the greatest pain with standing in the morning, after the plantar fascia has contracted during the night's rest.
Although stretching of the plantar fascia and Achilles tendon is the mainstay of treatment in plantar fasciitis, inserting cushioning insoles may be helpful adjuncts. Because flattening of the foot during walking triggers pain by overstretching the planter fascia, orthoses designed to maintain the medial longitudinal arch during ambulation are preferred.8
FIGURE 4.
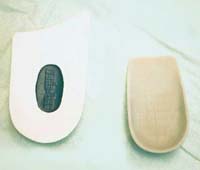
Either a hard or soft heel cup may be helpful in age-related heel pain.
Orthoses made of cork, viscoelastic polymer or closed-cell foam provide cushioning by reducing shock during walking by as much as 42 percent (Figure 5).9 Results of a survey10 of runners using orthotics for plantar fasciitis showed that 74 percent reported a significant improvement of symptoms with the use of orthotics and 90 percent continued to use orthotics even after resolution of symptoms.
FIGURE 5.

Viscoelastic polymer or closed-cell foam insoles, which have molded support for the plantar arch.
In a prospective, randomized trial11 of patients with plantar fasciitis, rates of pain relief were higher for patients who used ready-made heel cups and insoles combined with a stretching program than for patients who used rigid custom orthotics combined with stretching or stretching alone. Over-the-counter foam insoles and arch supports generally cost $8 to $20 per pair, while custom-molded orthotics cost $100 to $300. A trial of the inexpensive alternative certainly seems justified before referring patients to a podiatrist or a pedorthist.
Orthotic shoe inserts may be effective for pain relief in patients with pes planus, hyperpronation or a cavus foot.20 Rigid, semi-rigid and flexible shoe inserts all can be used. It may also be possible to obtain adequate arch support by changing the brand of shoe. Well-fitting shoes are an essential component of any treatment plan for patients with foot problems. Patients who do not respond to simple interventions, or those who have orthopedic or systemic diseases complicating their foot care may require a referral to a podiatrist, foot clinic or orthopedist.

