A 43-year-old man presented to the emergency department after a fall backward onto his wrist, with complaints of pain in his right wrist. Radiographs showed no fracture of the wrist, metacarpals or other bones. There were no dislocations or subluxations noted. The entire wrist and thumb were markedly swollen and diffusely tender, with no localization to the pain. A diagnosis of soft tissue injury was made. The patient's wrist was placed in a customized fiberglass thumb spica/wrist splint, and follow-up was scheduled.
One week later, when the splint was removed, there was still noticeable swelling to the thenar eminence (Figure 1), with significant yellowing to the bruise (which usually occurs after the bruise is more than one to five days old),1,2 but the wrist was relatively non-tender. There was tenderness on abduction and extension of the thumb, and there was pain on flexing the thumb and on pinch grip. Photographs were taken one week after the injury, which revealed an unusual pattern of bruising in the wrist flexor creases (Figure 2).
FIGURE 1.*
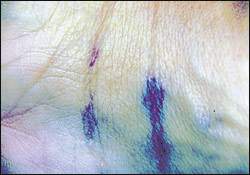
FIGURE 2.*
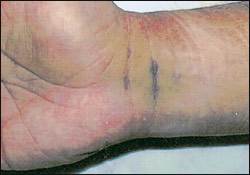
*— These images were taken with an electronic digital camera at 1.4 megapixel resolution.
Question
Which one of the following conditions does this type of bruising signify?
A. Occult fracture of the scaphoid bone.
B. Migration of deep hematoma fluid along fascial planes from a thumb sprain.
C. Subluxation of the lunate bone.
D. Tear of superficial palmar branch of the radial artery.
E. Rupture of flexor carpi radialis tendon.
Discussion
The correct answer is B: Migration of deep hematoma fluid from a thumb sprain. In a soft tissue injury, there is bleeding from the torn muscles and ligaments, but this blood is usually confined by the fascia and does not appear as surface bruising. As the hematoma resolves, the swelling and edema of the injured soft tissues go down. As fibrolysis of the clot occurs, liquefied blood and clot can track along the fascial planes. The migrating hematoma can emerge where the fascial planes are reflected superficially, because they form attachments to the skin. In this case, blood from the thenar eminence has migrated proximally and appears superficially at the proximal and distal palmar creases, where the fascia comes through the carpal tunnel.3
The tears are most likely to the thenar muscles (i.e., opponens pollicis, abductor pollicis brevis and possibly the adductor pollicis). The yellow color of the bruise is caused by hemoglobin breakdown products within the hematoma, whereas the deep purple bands in the flexor creases are from old fibrinolysed blood.1,2
Rupture of the superficial palmar branch artery would lead to much larger hematoma formation, and because this artery is superficial to the flexor retinaculum, it would not be confined in the carpal tunnel; the hematoma would not appear in the palmar creases. A ruptured flexor tendon would also not produce a large hematoma, and it would be confined within the flexor tendon sheath. An occult scaphoid fracture would likewise not be expected to produce bruising that migrates out to the creases, for it would be intra-articular hematoma within the carpal joint capsule. Although scaphoid fractures may easily be missed on initial radiographs, they would not typically cause the thenar swelling and unusual bruising seen here. Subluxation of the lunate would be seen on the radiographs.

