to the editor: A 76-year-old woman presented to the dermatology office because of a large mass on her left upper back (Figure 1). Although the lesion was present for many years, she was only prompted to remove it when it began to “poke her in the back.” On examination, the mass was a large cutaneous horn measuring 6 cm in length and varying from 4 cm in diameter near the skin surface to 1.5 cm in diameter near the tip of the horny growth. The differential diagnosis of cutaneous horn can be found in the accompanying table. Further examination revealed a brownish-yellow excrescence made up of dense hyperkeratotic tissue with longitudinal ridges on an erythematous base (Figure 2).
FIGURE 1.

Patient presented with large mass on left upper back.
The horn, with its base, was surgically excised under local anesthesia. Results of a biopsy are shown in Figure 3. Microscopically, the superficial portion shows a papillated surface with hyperkeratosis, parakeratosis, and marked epithelial hyperplasia. The deep margin is well defined with large bulky downward proliferations composed of well-differentiated keratinocytes with glassy, eosinophilic cytoplasm consistent with verrucous carcinoma.
FIGURE 2.
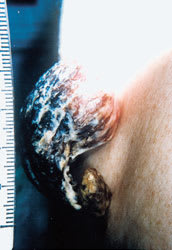
Close-up view of cutaneous horn, measuring 6 cm in length.
FIGURE 3.
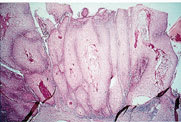
Microscopic evaluation reveals a papillated surface with hyperkeratosis, parakeratosis, and marked epithelial hyperplasia.
A verrucous carcinoma is a well-differentiated variant of a low-grade squamous cell carcinoma. It usually appears in the oral cavity, anogenital region, or plantar surface of the foot, but can arise anywhere on the skin Keratoacanthoma surface. Although rare, verrucous carcinoma has been reported to arise on the buttocks,1 maxillary antrum,2 and face3.
Differential Diagnosis of a Cutaneous Horn
| Hypertrophic actinic keratosis | Squamous cell carcinoma |
| Seborrheic keratoses | Acrochordon |
| Filiform wart |
Although the pathogenesis of verrucous carcinoma is unknown, many possible causes have been proposed. The use of chewing tobacco has been considered in the development of oral verrucous carcinomas4. Many types of human papillomaviruses have been linked to verrucous carcinomas. More recent studies are looking at tumor suppressors such as p53 and Rb genes; monoclonal antibodies suggest that a high percentage of verrucous carcinomas have an overexpression of the p53 protein5. Other reports using immunochemistry not only show p53 expression but also note an overexpression of cyclin D1 without alterations of Rb staining. This suggests that Rb may become inactive by the overexpres-sion of cyclin D1 or from the human papillo-mavirus infection6.
Cutaneous verrucous carcinomas are slow growing and exophytic with little metastatic potential. As the tumor extends, it tends to compress contiguous structures rather than invading them. Although rare, metastases to regional lymph nodes and distant sites can occur. Furthermore, the tumor can be locally aggressive, causing bone destruction and nerve involvement.
Surgical excision is the treatment of choice for cutaneous carcinomas. Care must be taken to remove all aspects of abnormal skin or mucosa because recurrences are common. Radiotherapy remains controversial because anaplastic transformation has been reported7. The verrucous carcinoma here was surgically excised under local anesthetic with clear margins.
The case presented demonstrates that verrucous carcinoma can occur in multiple sites and as a cutaneous horn. It underscores the need to adequately remove such lesions and biopsy them to rule out an underlying malignancy.

