What is GER?
Gastroesophageal (say: gas-tro-ee-sof-ah-gee-all) refers to the stomach. Reflux means to flow backward. So, gastroesophageal reflux (GER) is when liquids or foods in the stomach flow “back up” into the esophagus (the tube where food passes from your mouth to your stomach). GER is a disorder that affects the muscle that connects your esophagus to your stomach (see picture below).
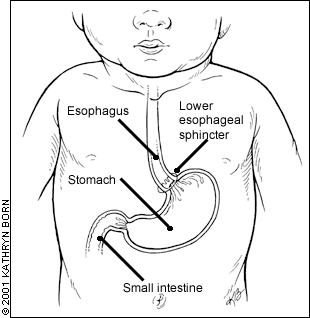
GER is a common cause of “spitting up” formula or breast milk during the first year of life. Spitting up has been noted in 40 to 65 percent of healthy babies. By one year of age, only 1 percent of infants will spit up milk or solid foods.
Children and adolescents may have heartburn and discomfort after heavy meals. GER is made worse by drinking caffeinated and citrus beverages. In teenagers, drinking alcohol and smoking cigarettes can make GER worse.
When should I be concerned about my infant or child with GER?
Most cases of GER will go away on their own. However, regular spitting up or vomiting in infants associated with any of the following symptoms may be a sign of a more serious problem:
- Weight loss or poor weight gain
- Frequent breathing problems such as not breathing for longer than 20 seconds, turning blue, choking, or unexplained wheezing, cough, or pneumonia
- Unexplained severe fussiness, crying, and discomfort with feedings
You should be concerned if a child older than one year has pain in the lower chest or upper abdomen that occurs regularly. If it bothers your child during activities or sleep, call your doctor.
Older children who have severe abdominal discomfort, bloody vomit, or unexplained anemia (low iron count) should see their doctor. This may be a sign of GER disease or another disorder.
How is GER evaluated?
Because GER often goes away on its own, most cases do not need special tests. If needed, your doctor may order a test called an upper gastrointestinal (GI) study. It is a special x-ray of the esophagus, stomach, and part of the small intestine that is done after your child drinks a special liquid.
Other tests may require a visit to a children's GI doctor. Endoscopy is a test that checks the lining of the stomach and upper GI tract. Pictures are taken of the lining and tissue samples can be studied. Endoscopy is best used to study pain in the upper abdomen that does not go away.
The 24-hour pH probe can be used to measure acid in GER disease. This study requires an overnight hospital stay. Probe equipment is inserted near your child's stomach to check for episodes of acid reflux.
How is GER treated?
Lifestyle/dietary
Most cases of GER will go away without medicines. You should thicken your baby's food. Add 1 tablespoon of dry rice cereal to each ounce of formula or breast milk. You can buy pre-thickened formulas. Hold your baby upright after feedings instead of lying your baby down right away.
For children, you can try more frequent, smaller meals. Your child should drink fewer caffeinated drinks and citrus juices and eat fewer heavy meals.
Medical
When GER does not go away after you make these changes, your doctor may want to give your child a medicine. A visit to a children's GI doctor may be needed.
Medicines that lower stomach acid include cimetidine (brand name: Tagamet), ranitidine (brand name: Zantac), omeprazole (brand name: Prilosec), and lansoprazole (brand name: Prevacid).
Other medicines include metoclopramide (brand name: Reglan) and cisapride (brand name: Propulsid). These help prevent return of food from the stomach to the mouth. You should know that extreme caution should be used if your child is given cisapride. Electrocardiogram (ECG) tests should be done. Certain medicines should not be taken while taking metoclopramide and cisapride. You should carefully check to make sure you are giving the proper dosage. Your doctor can help if you have any questions.
Surgical
Surgery may be needed if your child has severe GER disease and still has problems after treatment with medicine. Talk to your doctor about the surgical options.

