Digital mucous cysts are solitary, clear, or flesh-colored nodules that develop on the dorsal digits between the distal interphalangeal joint and the proximal nail fold. There are two types of digital mucous cysts: one type is associated with degenerative changes in the distal interphalangeal joint, and the second type is independent of the joint and arises from metabolic derangement of fibroblasts that produce large quantities of hyaluronic acid. The two types are clinically indistinguishable. The cysts can be asymptomatic, or they can cause pain, tenderness, or deformity of the nail. Aggressive surgical techniques to remove osteophytes from the joint can produce low recurrence rates. Other procedures to eliminate cysts, such as a simple surgical technique, cryosurgical destruction, or repeated needling, can be performed in an office setting.
Digital mucous, or myxoid cysts, are clear or flesh-colored nodules that develop on the dorsal digits between the distal interphalangeal joint and the proximal nail fold (Figure 1).1–4 The lesions, which are usually solitary and appear lateral to the midline,3 are more common on dominant hands.5 The cysts can be from a few millimeters to one centimeter or larger in diameter.3,6 The lesions develop more commonly in middle-aged and elderly persons,3,7 and women are affected more than twice as often as men.3,5 Mucous cysts are uncommonly encountered on toes.2,3,6,8
There are two types of digital mucous cysts.1,4,9 One type is associated with degenerative changes in the distal interphalangeal joint and looks similar to ganglia and synovial cysts.1,2,4,9 These cysts can have a stalk that tracks back to the joint.4,9,10 The second type of cyst seems to be independent of the joint and is thought to arise from the metabolic derangement of fibroblasts that produce large amounts of hyaluronic acid.1,4,9 This type of cyst typically involves the proximal nail fold.9 Neither type has a true epithelial lining, which makes them “pseudocysts.”1,2,11
Digital mucous cysts are frequently asymptomatic.1,6 Patients may experience decreased range of motion in the nearby joint along with pain, tenderness, and nail deformity.1–3,8 Nail ridging, which is caused by pressure on the nail matrix, may be present in one third of cases.5 Damage to the nail matrix during treatment can cause permanent nail deformity. The cysts are usually chronic, and it has been suggested that the cysts rarely resolve spontaneously. However, results from one longitudinal study suggest that some cysts gradually regress.3 A preceding history of trauma may be present, especially in patients younger than 40 years.12 Transillumination may aid in correctly identifying cysts.3,11
FIGURE 1.
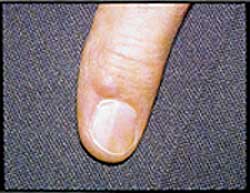
Digital mucous cyst.
Various therapies have been proposed to treat digital mucous cysts. Observation may be appropriate for asymptomatic patients. Most surgical approaches attempt to remove the cyst and any underlying stalk connected to the joint.4,13 Aggressive surgery to remove underlying osteophytes at the joint results in few recurrences.3,12–17 However, this procedure may slightly increase the risk of surgical complications such as joint stiffness and loss of motion.1,7,8 Nail deformities often resolve following osteophyte removal.16 Osteophyte removal alone (without removal of the cyst) has been reported to be effective.15,16
While osteophyte removal or open joint procedures are usually performed in the hospital setting, other management techniques can be performed in the office by family physicians.13
Techniques
REPEATED NEEDLING
Cure rates of up to 70 percent have been reported following repeated puncture and expression of cyst contents.2,7 Clear, jelly-like content squeezed from the cyst confirms the diagnosis.7,9 Puncture can be repeated with a sterile 25-gauge needle when the cyst becomes noticeable. Typically, a minimum of two to five punctures are needed for resolution of the cyst to occur.2,7
EXPRESSION AND STEROID INJECTION
Expression of the cyst contents can also be performed using a 21-gauge needle. An equal mixture of 0.2 mL of 1 percent lidocaine (Xylocaine) and 0.2 mL of triamcinolone acetonide (Kenalog, 10 mg per mL) can be injected into the site. This intervention is limited by high rates of recurrence.2,3,8 While many authors no longer recommend this intervention, it has been reported that a few patients have achieved long-term resolution following aspiration and injection.5
CRYOSURGERY
Cryosurgical destruction is an effective therapy for digital mucous cysts.8,18 The cyst is unroofed and drained (Figure 2a), followed by sufficient cryosurgical application to produce an ice ball with at least a 2 mm margin surrounding the edges of the cyst (Figure 2b). Freeze time is about 15 to 30 seconds and thaw time is about 60 to 90 seconds.2,6,10 Because of the possible cyst stalk to the joint, the treated area should include the cyst base and as far proximal as the transverse groove overlying the distal interphalangeal joint.10 A freeze-thaw-freeze technique appears superior to a single freeze.2,10
FIGURE 2.
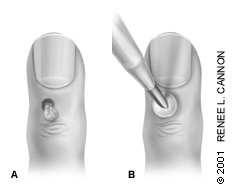
(A) The cyst is unroofed, and the characteristic jelly-like substance is expressed. (B) Freeze-thaw-freeze cryosurgical treatment is applied.
FIGURE 3A.
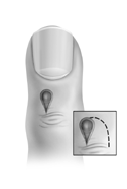
Once the entire lesion is removed, a small rotation flap is created.
FIGURE 3B.
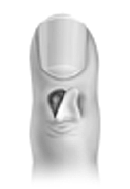
The flap is rotated over the defect.
Notching of the proximal nail fold can occur follow cryosurgery for digital mucous cysts.2 About 10 to 15 percent of patients experience a recurrence following cryosurgery.17 Carbon dioxide lasers also are being used to ablate the cyst base.
SIMPLE SURGICAL EXCISION
Simple excision of cysts is associated with high recurrence rates.3 A simple surgical technique, described below, has been shown to result in good cosmetic and functional outcomes for patients.18 Following digital block, the skin over the cyst is incised and the lesion is carefully dissected from the surrounding connective tissue and the extensor tendon below it (Figure 3a).18 A small, U-shaped rotation flap is created next to the circular defect created by the removal of the cyst.6,18 The flap is moved to cover the defect and, preferably, is not sutured, but left to heal by secondary intention (Figure 3b). It is possible that the extra scarring created by not suturing the wound may result in more widespread scar formation and, consequently, a decreased chance of recurrence of the cyst. If the small rotation flap does not stay centered over the surgical defect, a single suture may be used to hold the flap in place (Figure 3c). The flap technique is often used when an open, draining cyst is encountered.13
Antibiotic cream and light gauze compression dressing are applied following surgery.13 Some authors believe immobilization is unnecessary in most cases,13 but an aluminum splint may reduce discomfort when applied for two to 10 days following the procedure.
FIGURE 3C.
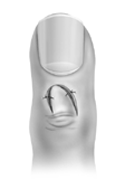
One or two sutures may be used to stabilize the flap in a central position over the defect, or the flap may be left to heal by secondary intention.

