
This is a corrected version of the article that appeared in print.
Am Fam Physician. 2002;65(7):1367-1375
Venomous snakebites, although uncommon, are a potentially deadly emergency in the United States. Rattlesnakes cause most snakebites and related fatalities. Venomous snakes in the United States can be classified as having hemotoxic or neurotoxic venom. Patients with venomous snakebites present with signs and symptoms ranging from fang marks, with or without local pain and swelling, to life-threatening coagulopathy, renal failure, and shock. First-aid techniques such as arterial tourniquets, application of ice, and wound incisions are ineffective and can be harmful; however, suction with a venom extractor within the first five minutes after the bite may be useful. Conservative measures, such as immobilization and lymphatic constriction bands, are now advocated until emergency care can be administered. Patients with snakebites should undergo a comprehensive work-up to look for possible hematologic, neurologic, renal, and cardiovascular abnormalities. Equine-derived antivenin is considered the standard of care; however, a promising new treatment is sheep-derived antigen binding fragment ovine (CroFab), which is much less allergenic. Although there is no universal grading system for snakebites, a I through IV grading scale is clinically useful as a guide to antivenin administration. Surgical intervention with fasciotomy is now reserved for rare cases. Snakebite prevention should be taught to patients.
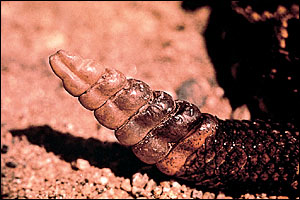
In the United States, 99 percent of snakebites are caused by the Crotalidae (pitviper) family of snakes6 (Table 1). The Crotalidae family includes the following snakes: rattlesnakes, genera Crotalus and Sistrurus (Figure 1); copperheads, Agkistrodon contortrix (Figure 2); and cottonmouths, or water moccasins, Agkistrodon piscivorous (Figure 3). These snakes are referred to as pit vipers because of small, heat-sensitive pits between the eye and the nostril that allow them to sense their prey.
| Rattlesnakes |
| Banded rock |
| Black-tailed |
| Canebrake |
| Diamondback (eastern and western) |
| Massasauga (eastern and western) |
| Mojave |
| Mottled rock |
| Pacific (northern and southern) |
| Pigmy (southeastern and western) |
| Prairie |
| Red diamond |
| Ridge-nosed |
| Sidewinder |
| Speckled |
| Tiger |
| Timber |
| Twin-spotted |
| Copperheads |
| Broad-banded |
| Northern |
| Osage |
| Southern |
| Trans-Pecos |
| Cottonmouths |
| Eastern |
| Florida |
| Western |
| Coral snakes |
| Arizona |
| Eastern |
| Texas |
| Western |


Because of their widespread distribution and relatively potent venom, rattlesnakes are responsible for the majority of fatalities from snakebites; eastern and western varieties of diamondback rattlesnakes (Figure 4) account for almost 95 percent of these deaths.3 Bites from copperhead snakes, which are common in the eastern United States, seldom require antivenin therapy because they have the least potent venom and a negligible fatality rate.
Cottonmouths, or water moccasins, are aggressive semi-aquatic snakes native to the southeast; they have an intermediate-potency venom. Coral snakes of the Micrurus genus in the family elapidae (Figure 5) are responsible for a minority of snakebites in the United States. Native to the deep South, their territory extends west to Arizona. Coral snakes are secretive and nonaggressive; they seldom bite unless provoked. Their venom is transferred by chewing rather than by injecting. Coral snake bites, although rare, are easy to miss, and often present as painless, tiny puncture wounds with negligible surrounding tissue change.

Although exotic snakes account for only a small percentage of venomous snakebites,7 the prevalence of these bites is increasing as the popularity of keeping exotic snakes as house pets continues to rise.
Snake Envenomation
Snake venoms can be classified as hemotoxic (attacking tissue and blood) and neurotoxic (damaging or destroying nerve tissue). Pit viper snake venoms are hemotoxic, except for some Mojave rattlers. Contrary to public perception, pit viper bites are not immediately fatal unless the venom enters a vein directly. The venom consists of proteins, polypeptides, and enzymes that cause necrosis and hemolysis. Most crotalid venoms damage capillary endothelial cells, resulting in third spacing of plasma and extravasation of erythrocytes.8
Pit viper bites classically appear as two fang punctures (one or three puncture wounds occur, but rarely) with local swelling and necrosis. Extremity bites are rarely complicated by infection and compartment syndrome, and prophylactic fasciotomies often do more harm than good.
Clinical effects of snakebites range from mild local reactions to life-threatening systemic reactions, depending on the species and size of the snake involved; the location of the bite(s); the volume of venom injected; and the age, size, and health of the victim. Children are more likely to suffer significant morbidity and mortality because they receive a larger envenomation relative to body size.9
| Hemotoxic symptoms | Neurotoxic symptoms |
| Intense pain | Minimal pain |
| Edema | Ptosis |
| Weakness | Weakness |
| Swelling | Paresthesia (often numb at bite site) |
| Numbness or tingling | |
| Rapid pulse | Diplopia |
| Ecchymoses | Dysphagia |
| Muscle fasciculation | Sweating |
| Paresthesia (oral) | Salivation |
| Unusual metallic taste | Diaphoresis |
| Vomiting | Hyporeflexia |
| Confusion | Respiratory depression |
| Bleeding disorders | Paralysis |
Systemic reactions include a syndrome similar to disseminated intravascular coagulation, acute renal failure, hypovolemic shock, and death. Renal failure is a common cause of delayed mortality from untreated snakebites in developing parts of the world. Immediately life-threatening conditions such as hypotension or shock occur in only about 7 percent of envenomations.7
The venoms of coral snakes, exotic elapids and some Mojave rattlesnakes are neurotoxic and usually cause local numbness instead of pain and swelling, with the risk of cranial nerve palsies, respiratory paralysis, and death. Symptoms of neurotoxic envenomations are listed in Table 2. Systemic reactions are difficult to reverse once they develop.
Snakebite First Aid
In recent years, first aid measures for snakebites have been radically revised to exclude methods that were found to worsen a patient's condition, such as tight (arterial) tourniquets, aggressive wound incisions, and ice. Initial treatment measures should include avoiding excessive activity, immobilizing the bitten extremity, and quickly transporting the victim to the nearest hospital.11
A wide, flat constriction band may be applied proximal to the bite to block only superficial venous and lymphatic flow (typically, with about 20 mm Hg pressure) and should be left in place until antivenin therapy, if indicated, is begun. One or two fingers should easily slide beneath this band, since any impairment of arterial blood flow could increase tissue death. Upper extremities should be splinted as close to a gravity-neutral position as possible, preferably at heart level.
No study has shown any benefit in survival or outcome from incision and suction.11–13 However, a venom extractor can be beneficial if applied within five minutes of the bite and left in place for 30 minutes.5 Although electric shock (often with a stun gun) has been a popular treatment for snakebite in developing countries, it should be avoided as it is a potentially hazardous intervention that has never been shown to be effective.14
An attempt should be made to identify the type of snake from a safe distance; however, no attempt should be made to capture or kill the snake. Even if the snake is dead, it should not be picked up with the hands because envenomation by reflex biting after death of the snake has been reported.15
Equine-derived antivenin to snake venom is not recommended for the formularies of standard emergency medical services because of the potential for life-threatening allergic reactions from the antivenin and the length of time required for reconstitution (up to 60 minutes).16 As safer products, such as Crotalidae Polyvalent Immune Fab (Ovine; Cro-Fab), become more commonplace, antivenin administration in the field may become more feasible, especially in remote areas.
Treatment
Patients with snakebite must be admitted to an emergency department, where a poison control center should be contacted immediately. Wounds should be cleaned, and administration of tetanus toxoid or tetanus immune globulin should be considered for under-immunized or nonimmunized patients. Patients should be given intravenous fluid, and blood should be drawn from an unaffected extremity. Complete recommendations for laboratory evaluations of snakebite are summarized in Table 3. At least 25 percent of snakebites do not result in envenomation. Patients with asymptomatic pit viper bites should be observed for at least 12 hours before discharge.8 When envenomation does occur, the leading edge of the swelling should be marked, the time of observation recorded, and the circumference of the extremity measured every 30 minutes.17 If there is no proximal progression of local signs on the extremity and no coagulopathy after 12 hours of clinical observation and serial laboratory examinations, a reliable patient can be sent home.
| Complete blood count with platelets and differential* | Platelet count |
| Prothrombin time* | Liver function tests |
| Partial thromboplastin time* | Bilirubin |
| Fibrinogen* | Creatine kinase |
| Fibrin degradation products* | Creatinine |
| Blood type and cross match | Urinalysis† |
| Serum electrolytes | Stool hemoccult |
| Glucose | Electrocardiography‡ |
| Blood urea nitrogen | Arterial blood gas§ |
The patient should be given strict instructions to return to the hospital immediately if any of the following occurs: increase in pain or onset of redness or swelling; fever; epistaxis; bloody or dark urine; nausea or vomiting; faintness; shortness of breath; diaphoresis; or other symptoms except mild pain at the bite site.8 Prophylactic antibiotics are usually not recommended, as the occurrence of wound infection following crotalid envenomation is low (3 percent).18,19
Patients with bites from snakes with neurotoxic venom should be observed for at least 24 hours. A patient with suspected envenomation by the eastern coral snake needs immediate treatment with an appropriate antivenin, and necessary resuscitation measures should be implemented.
Antivenin Indications and Administration
Equine-derived antivenin to snake venom has been the mainstay of hospital treatment for venomous snakebite for 35 years.20 It is used to treat approximately 75 percent of the venomous snakebites inflicted annually in the United States.5 The majority of snakebite victims in the United States reach a medical facility within 30 minutes to two hours of being bitten and can be given antivenin at an early stage.3
For rattlesnake, cottonmouth, and copperhead bites, Antivenin (Crotalidae) Polyvalent (ACP) has been the standard available treatment; however, ACP is known to be highly allergenic because of its equine origin and may pose a greater risk to the patient than the snakebite.21 In retrospective studies,20 rates for acute allergic reactions (including hypotension and anaphylaxis) after ACP administration range from 23 to 56 percent, with even higher rates for delayed serum sickness.
The ovine (sheep-derived) antivenin, CroFab, received approval by the U.S. Food and Drug Administration for treatment of snakebites in October 2000; its use is still limited because of availability and expense, but it is likely to soon replace the equine crotalid antivenin. A prospective trial using CroFab reports only a 14.3 percent incidence of acute reaction, and nearly all events were mild to moderate.20 Experience with CroFab is still too limited to support the conclusion that serious allergic reactions like anaphylaxis will never occur with its administration.
Eastern coral snakebites require Antivenin (Micrurus fulvius). The specific antivenin for exotic snakebites may be acquired from the Arizona Poison and Drug Information Center (520-626-6016). An antivenin index is available from the American Zoo and Aquarium Association (301-562-0777) and the American Association of Poison Control Centers (800-222-1222).22 A prescription is required to obtain U.S. antivenin, and a permit is needed to import antivenin not held domestically.23
Ideally, antivenin is administered within four hours of the snakebite, but it is effective for at least the first 24 hours. Physicians should be present for antivenin administration, and epinephrine and antihistamines (both histamine H1 and H2 receptor blockers) should be at the bedside.
Performing a skin test with horse serum is a matter of controversy because it delays therapy, has itself caused anaphylaxis and serum sickness,24,25 and has been demonstrated to have a 10 to 36 percent false-negative rate21,26 and a 33 percent false-positive rate.21 Some physicians believe that medicolegal issues mandate that this test be performed before antivenin administration except in extreme emergencies.27 Other physicians bypass skin testing altogether, relying instead on premedication with antihistamines and a trial dose of 5 mL of antivenin administered intravenously.
In the event of a significant skin-test reaction, antivenin would be reserved for use in only the most severe cases and should only be given with careful monitoring, hydration, and premedication with antihistamines. An alternative to skin testing is to premedicate all patients who will receive equine antivenin.28 Suggested intravenous antihistamine pretreatment is diphenhydramine (Benadryl), in a dosage of 1 mg per kg, and cimetidine (Tagamet), in a dosage of 6 mg per kg.8 If signs or symptoms of anaphylaxis develop, the patient should be immediately treated with epinephrine and steroids.8 Unstable patients (i.e., those with hypotension, severe coagulopathy respiratory distress) must receive antivenin because no other treatment can reverse the venom's effect.
The unpredictable nature of snakebites often makes assessment and management difficult. Progressive local injury (swelling, ecchymosis), a clinically evident coagulation abnormality, or systemic effects (hypotension, altered mental status) are strong indications for antivenin treatment. Withholding antivenin is recommended in patients with milder envenomations.21 The decision to use antivenin requires a careful analysis of the risks and benefits.
ADMINISTRATION OF ANTIVENIN
Both ACP and CroFab are provided as dry powders and require reconstitution before administration. Reconstitution can take up to 60 minutes and should be initiated immediately when the patient arrives in the emergency department. ACP can be reconstituted by injecting 10 mL of supplied sterile water diluent into each vial and swirling (not shaking) to mix, or by diluting 10 vials of antivenin in 1 L of normal saline. The reconstituted antivenin (amount will vary, depending on amount required) is then diluted in 500 mL of normal saline or 5 percent dextrose in water, and a trial dose of 5 to 10 mL is administered intravenously over five minutes. If no reaction occurs, the rate should be adjusted to give up to 10 vials in the first hour. Additional infusions should be given every two hours until signs and symptoms are resolving.
In contrast, the safer CroFab is given as a large initial dose to control the envenomation, and smaller subsequent doses are given as needed. In one study,20 a total of three to 12 vials of CroFab were given for initial control, and additional two-vial doses were given at six, 12, and 18 hours.
For any eastern coral snake bite with possible envenomation, three to five vials of Antivenin (Micrurus fulvius) should be administered immediately. If systemic manifestations are present, at least six to 10 vials should be administered. One exception is the Arizona coral snake (Micruroides), which is not associated with human fatality and for which no antivenin exists.
Immediate hypersensitivity reactions to any antivenin should be managed with epinephrine, antihistamines and supportive care to protect the respiratory and cardiovascular systems. Serum sickness, which commonly occurs one to four weeks after administration of antivenin, presents with pruritus, urticaria, fever, and arthralgias. Serum sickness can be successfully treated with systemic steroids.
GRADING THE SEVERITY OF THE BITE
A popular scale for grading the severity of pit viper bites and estimating the antivenin dose is presented in Table 4. It is important to remember that a patient must have serial evaluations, because an envenomation that appears to be mild on presentation can soon exhibit the hallmarks of a severe envenomation. Doses of antivenin must not be reduced for children or small persons, since the amount of venom that needs to be neutralized is the same.
| Degree of envenomation | Presentation | Treatment |
|---|---|---|
| 0. None | Punctures or abrasions; some pain or tenderness at the bite | Local wound care, no antivenin |
| I. Mild | Pain, tenderness, edema at the bite; perioral paresthesias may be present. | If antivenin is necessary, administer about five vials.* |
| II. Moderate | Pain, tenderness, erythema, edema beyond the area adjacent to the bite; often, systemic manifestations and mild coagulopathy | Administration of five to 15 vials of antivenin may be necessary. |
| III. Severe | Intense pain and swelling of entire extremity, often with severe systemic signs and symptoms; Coagulopathy | Administer at least 15 to 20 vials of antivenin. |
| IV. Life-threatening | Marked abnormal signs and symptoms; severe coagulopathy | Administer at least 25 vials of antivenin. |
Surgical Management
Although once popular, surgical intervention with fasciotomy for venomous snakebite is now reserved for selected rare cases and should never be performed prophylactically. The local and systemic effects of crotaline venom closely resemble the signs and symptoms of compartment syndrome15 and cannot be reliably diagnosed in an envenomated patient without directly measuring the compartment pressure.
Fasciotomy should only be performed in patients with clinical signs and symptoms of compartment syndrome (i.e., pain on passive stretch, hypoesthesia, tenseness of compartment, and weakness) and hourly, serially measured compartment pressures exceeding 30 mm Hg. These criteria should be present despite elevation of the affected limb and administration of 20 vials of antivenin.8 In an animal study,29 the best outcome in subjects with compartment syndrome was achieved with the administration of antivenin alone. In a series of 1,257 cases of extremity bites, only two fasciotomies were necessary.12
Prevention
Physicians should educate their patients on ways to prevent snakebites, as prevention is far preferable to treatment. Many bites can be easily prevented by using common sense. For some precautions against snakebites, see the accompanying patient information handout on page 1377.