
Am Fam Physician. 2002;65(11):2307-2315
The body’s ability to regulate core temperature depends on both host (internal) and environmental (external) factors. Although athletes are commonly thought to be most at risk for heat illnesses, children and the elderly are particularly vulnerable. Heat cramps, which are caused by fluid and electrolyte imbalances, are treated with massage, and fluid and electrolyte replacement. Heat exhaustion occurs both as water- and sodium-depleted types, with associated symptoms such as malaise, vomiting, and confusion. Treatment involves taking the affected person to a cool environment and replacing fluids and electrolytes if needed. In more serious cases, intravenous hydration may be necessary, although monitoring of serum sodium levels is important to prevent cerebral edema. If not treated promptly, heat exhaustion may evolve into heatstroke, a deadly form of heat illness. Heatstroke occurs in classic and exertional forms and is present when the core body temperature exceeds 40 C (104 F). The patient may experience cardiac arrhythmias, rhabdomyolysis, serum chemistry abnormalities, disseminated intravascular coagulation, and death. Heatstroke is a medical emergency that should be treated immediately with temperature-lowering techniques such as immersion in an ice bath or evaporative cooling. Fluid resuscitation is important but should be closely monitored, and renal function may need to be protected with mannitol and diuretics. It is important to be vigilant for heat illnesses because they occur insidiously but progress rapidly.
The ability of the body to regulate core temperature depends on a host of factors, including ambient temperature, acclimatization, humidity, wind, clothing, pre-existing medical conditions, and medication use. An estimated 6 million workers in the United States are exposed to occupational heat stress,1 with fatalities most commonly reported in the fields of construction, agriculture/forestry/fishing, and manufacturing.1 Children and the elderly are particularly vulnerable,2 while athletes and recreational sports enthusiasts are also at risk.
Physiology
The normal core body temperature for humans, measured rectally, depends on the environmental climate and internal metabolic function. When the core temperature rises, the basal metabolic rate can increase significantly. For every 0.6°C increase in core temperature, there is a 10 percent elevation in the basal metabolic rate.3 Core temperature can increase as a result of elevated ambient temperature or through work-related activities and athletic performance that increase metabolic rate. For example, marathon runners have developed temperature elevations up to 41°C (105.8°F) while running in 25°C (77°F) weather.4
Thermoregulation is controlled by the hypothalamus. The parasympathetic system controls sweating, with the sympathetic nervous system regulating increases in skin blood flow and vasodilatation for heat dissipation. Normally, thermoregulation is highly efficient, with a mere 1°C change in core temperature for every 25°C to 30°C change in ambient temperature.5 Chronic disease, some medications, and poor physical conditioning can impair the body’s normal mechanisms of dissipating heat, which may result in a dangerously high core temperature.
The basic mechanism behind heat-related illness is the body’s inability to dissipate heat produced by metabolic activity, often as a result of increased ambient temperature. Environmental influences, clothing, preexisting illness (Table 1),1,6–8 and certain medications (Table 2)1,7,8 can contribute to this problem.
| Alcoholism |
| Anorexia |
| Cardiac disease |
| Cystic fibrosis |
| Dehydration |
| Diabetes insipidus |
| Eating disorders |
| Extremes of age |
| Febrile illness |
| Gastroenteritis |
| History of heatstroke |
| Hypokalemia |
| Obesity |
| Poor acclimatization |
| Sleep deprivation |
| Sunburn |
| Sweat gland dysfunction |
| Uncontrolled diabetes |
| Uncontrolled hypertension/thyroid disorder |
| Upper respiratory tract infection |
| Alcohol |
| Alpha adrenergics |
| Anticholinergics |
| Antihistamines |
| Benzodiazepines |
| Beta blockers |
| Calcium channel blockers |
| Neuroleptics |
| Phenothiazine diuretics |
| Tricyclic antidepressants |
There are four processes by which the body rids itself of excess heat: conduction, convection, radiation, and evaporation. Conduction occurs when the body comes in contact with something cold, allowing heat to be transferred to the cooler object, such as when one applies cold packs to the body. Convection takes place when air passes over the body, lifting heat away, as occurs on a windy day or through the use of fans. Infrared dissipation, heat released by the body into the environment, is radiation. Finally, the evaporation of sweat from the skin plays a major role in heat dissipation during exercise and is the primary thermoregulatory mechanism when the ambient temperature is above 20°C (68°F).6
Children deserve special mention in the consideration of heat-related illness. Compared with adults, children produce proportionately more metabolic heat, have a core temperature that rises faster during dehydration, and have smaller organ systems, allowing for less efficient heat dissipation.6 Thus, caution should be exercised with children when conditions are right for heat illness. Close observation of an active child is important, because a fatal event can occur within 20 minutes if normal heat loss mechanisms are overwhelmed.6 This fact emphasizes the danger of leaving children unattended in a car during hot weather.
HEAT CRAMPS
Muscle cramps, which commonly occur in athletes and other physically fit persons, are caused by excessive heat exposure. Any activity that results in profuse sweating followed by too little or too much fluid intake can result in these painful muscle spasms, usually affecting the calf or abdominal wall muscles. Cramping is probably secondary to sodium depletion.3
During exercise, a poorly conditioned athlete may lose 1 to 2 L of fluid and 65 mEq per L of sodium per hour, whereas a highly conditioned, well-acclimatized athlete loses 3 to 4 L of fluid per hour with a sodium loss of only 5 mEq per L.9 Although more conditioned athletes lose less salt, they may take in excessive amounts of water, thus diluting their electrolyte concentrations and precipitating cramps.7 In addition, during more intense activity, a “slow” loss of sodium may occur over several hours to days, leading to cramps and progressing to other heat illnesses.10
Stretching the affected muscles and maintaining good hydration are important. Liberal intake of water is recommended, but this may induce hyponatremia if lost salt is not replaced. Commercial electrolyte solutions may help to prevent excessive salt loss, and a homemade formula of 1 tsp salt in 500 mL of water may also be used.11 Increased intake of dietary salt may be preventive. The signs and symptoms of heat cramps are listed in Table 3.7,8,12,13
| Heat cramps |
|---|
| Elevated body temperature |
| Thirst |
| Muscle cramps |
| Sweating |
| Tachycardia |
| Heat exhaustion |
| Same as heat cramps, plus: |
| Nausea/vomiting |
| Headache |
| Malaise/myalgias |
| Hypotension |
| Lightheadedness/syncope |
| Oliguria |
| Uncoordination |
| Confusion |
| Irritability |
| Heatstroke |
| Same as heat exhaustion, plus: |
| Anhydrosis |
| Delirium/seizure/coma |
| Renal failure |
| Hepatocellular necrosis |
| Hyperventilation |
| Pulmonary edema |
| Arrhythmia |
| Rhabdomyolysis |
| Shock |
| DIC |
HEAT EXHAUSTION
Heat exhaustion occurs as two types, water depleted and sodium depleted, although in reality they often overlap. Signs and symptoms of heat exhaustion (Table 3)7,8,12,13 include fatigue and malaise, anorexia, nausea, vomiting, anxiety, and confusion. Potentially dangerous clinical manifestations include circulatory collapse and excessive temperature.14 Core body temperature is usually higher than 38°C (100.4°F) but below the cutoff for heat-stroke, which is 40°C (104°F).12
Heat exhaustion from water depletion tends to occur in the elderly, who are more likely to have pre-existing conditions or take medications that predispose them to dehydration, especially during the summer months, and in active persons who do not drink enough fluids. Signs of dehydration include increased thirst, fatigue, dry oral mucosa, and decreased urinary output.
Heat exhaustion from sodium depletion occurs most often in unacclimated persons who maintain volume status with water, but fail to replace sodium lost in sweat. These persons may actually be “hyperhydrated,” and most will have a history of high fluid intake.15 Symptoms such as weakness, fatigue, and headache appear acutely, but the onset tends to occur over a period of several days.7
For “mild” cases of heat exhaustion, in which the person is fluid depleted but not dehydrated, has normal vital signs, and is not vomiting, the treatment is rest in a cool environment along with oral fluid replacement and salt replacement, if needed. In more seriously impaired persons—those with mental status changes or cardiac arrhythmia (especially ventricular tachycardia), or those who fail to improve with conservative measures—treatment in the emergency department with intravenous (IV) fluids and careful monitoring of blood chemistries is appropriate. IV administration of 1 L of 5.5 percent dextrose in normal saline over 30 to 60 minutes while monitoring serum sodium and potassium levels is recommended.7 Metabolic abnormalities such as phosphate, calcium, and magnesium imbalances should also be monitored and corrected.
When a person with water-depleted heat exhaustion is hypernatremic, it is necessary to hydrate slowly at a rate sufficient to reduce serum sodium by about 2 mEq per L per hour to prevent iatrogenic cerebral edema.3,10 In the hypernatremic state, a condition of hyperosmolality exists. To maintain osmotic equilibrium, there is intracellular volume contraction. In hypertonic syndromes the brain compensates by increasing osmoles in the brain cells. A sudden decrease in serum osmolality may be hypotonic relative to the brain cells, causing an increase of intracellular fluid into the brain cells and, thus, resulting in brain edema.3
Treatment for heat exhaustion should begin as soon as symptoms occur. If there is any question about outpatient or inpatient treatment, the patient should be transported to the emergency department. Failure to arrest the process during heat exhaustion could lead to the more deadly condition of heatstroke.
HEATSTROKE
Heatstroke, the deadliest of heat illnesses, occurs in two forms—classic and exertional—and is defined by a core body temperature above 40°C (104°F).12 Treatment must begin immediately to ensure survival. With prompt recognition and appropriate treatment, the survival rate is 90 to 100 percent16; however, in specific occupations the mortality rate is high. In firefighters, for example, mortality from heatstroke may approach 80 percent, heightening clinical concern in these persons.13
Classic heatstroke occurs during summer months and predominantly affects those with advanced age or chronic medical conditions. The triad of classic heatstroke is hyperpyrexia, anhidrosis, and mental status changes.8,17 One half of all heat-related deaths occur in persons older than 65 years.18 In addition to the elderly, persons with cardiovascular and cerebrovascular disease, diabetes, and nervous system disorders are at increased risk for hospitalization from heatstroke.2 Complications from heatstroke, such as acute renal failure, are common.19
Exertional heatstroke most often occurs in the summer, and primarily affects laborers or athletes. Symptoms are similar to those of classic heatstroke but with one major difference: many persons with exertional heatstroke continue to sweat.3,12,20 This difference is important because in someone who continues to perspire, heatstroke may be overlooked, thus delaying treatment. In addition, rhabdomyolysis and its complications (hyperkalemia, hyperphosphatemia, hypocalcemia, and myoglobinuria) often occur in persons with exertional heatstroke.3
Heatstroke is a medical emergency. Multiple organ systems can be affected. Prompt recognition and treatment are necessary to increase survival and decrease sequelae. It is important to remember that heat exhaustion, if not promptly treated, can lead to heatstroke, and that the two conditions may overlap, making vigilance of the utmost importance. Signs and symptoms of heatstroke are listed in Table 3.7,8,12,13
“The penguin effect” is an interesting concept.5 The name is derived from the “huddling,” heat-conserving method used by Antarctic penguins. This concept applies to the physiologic changes that occur in humans in overcrowded environments. In a crowd situation, the persons in the middle are surrounded by heat-producing bodies. They tend to absorb the heat given off by the latter and are unable to dissipate heat effectively, leading to overheating and the possibility of heatstroke. This effect may occur even if the ambient temperature does not seem hot enough.
Treatment of Heatstroke
Treatment of heatstroke begins with monitoring airway, breathing, and circulation (Table 4).1,6,8,12,13,21 Affected persons may seize, aspirate, or become hypotensive, and maintenance of the airway and circulatory function is critical. Patients initially seen in the community setting should be moved to a shady, cooler environment and have clothing removed, while an ambulance is called. Ice packs should be applied to the neck, axillae, and groin.6,8 The patient should be doused with water and fanned, if possible, to promote evaporative heat loss. Monitoring of the patient’s airway, breathing, and circulation should continue until the ambulance arrives.
| Prevention | Treatment | ||
|---|---|---|---|
| Prehydrate liberally with fluids Drink fluids before becoming thirsty Exercise in early morning/evening Treat pre-existing conditions Wear clothing appropriate for environment Check Heat Index Chart Acclimate over a two-week period to get conditioned to exercising in the heat | Check airway, breathing, and circulation | ||
| External cooling techniques | |||
| Prehospital: | |||
| Transfer to a cool, shady area | |||
| Remove insulating clothing | |||
| Apply ice packs to neck, axillae, and groin | |||
| Douse with water | |||
| In emergency department: | |||
| Ice bath immersion | |||
| Evaporative cooling | |||
| Neuroleptics for seizures | |||
| Mannitol/diuretics if needed to maintain urine output at 50 to 100 mL per hour | |||
| Stop cooling at a rectal temperature of 38°C (100.4°F) | |||
In the emergency department, medical staff should obtain and monitor the patient’s blood chemistries (electrolytes, phosphate, magnesium, calcium, creatine phosphokinase, and liver enzyme levels), initiate intravenous hydration if not completed en route, and begin rapid cooling as soon as possible.
The techniques most commonly used for rapid cooling are cold water immersion and evaporative cooling. In “traditional” cold water immersion, the patient is immersed in an ice bath and core body temperature and vital signs are monitored. Evaporative cooling combines spraying the patient with water at 15°C (59°F) while air warmed to 45°C (113°F) is passed over the body. This technique has been well outlined.22 Some studies report that the evaporative technique is superior to cold water immersion, with one study21 achieving a cooling rate of 0.31°C per minute.
A complete blood count may reveal leukocytosis or thrombocytopenia. A coagulation profile should be obtained to rule out disseminated intravascular coagulation. Urine should be evaluated for ketones, protein, and myoglobin.
Because renal compromise may occur in patients with hypotension, physicians should consider using mannitol and diuretics to maintain urine output at 50 to 100 mL per hour.12 Resistant hyperkalemia may require the use of potassium-lowering resins.
Dantrolene (Dantrium) is a muscle relaxant that alters muscle contractility. It is the drug of choice for the treatment of malignant hyperthermia, and it has been studied for possible use in the treatment of heatstroke. Study results have been mixed. One study23 reported that dantrolene use reduced cooling times, a pivotal step in the treatment of heatstroke. However, there was no statistically significant difference in recovery time between the group treated with dantrolene and the control group. Conversely, another study24 found that dantrolene does not alter cooling time.
Once the patient is stable, and rectal temperature is 38.3°C (101°F) or less, cooling can be discontinued. This helps prevent the inducement of hypothermia.8 If the patient starts to shiver because the temperature is decreased too rapidly or temperature reduction is overshot, muscle relaxants or neuroleptics such as chlorpromazine (Thorazine) may be used to inhibit shivering and prevent a concomitant increase in temperature.12 However, it is best to monitor the patient carefully to avoid shivering in the first place.
Preventing heatstroke is the first step in treating heatstroke (Table 4).1,6,8,12,13,21 Although it sounds deceptively simple, the best prevention is to avoid hot environments. To assess the environmental danger, a Heat Index Chart (Figure 1)25 produced by the National Weather Service may help to determine when outside activity should be avoided.
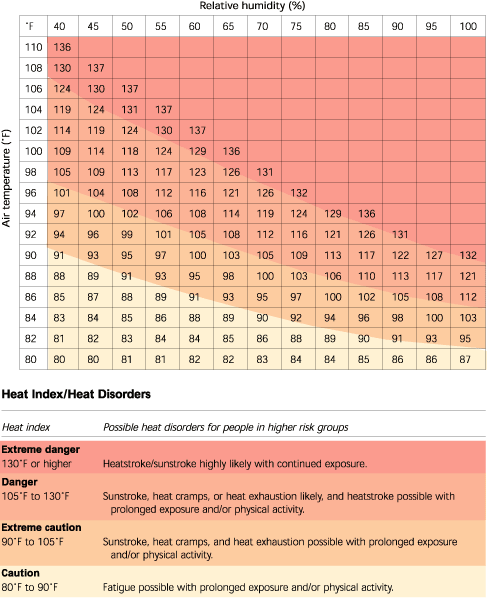
The Heat Index combines humidity and temperature measurements to construct a scale that describes how warm the air feels when humidity is high. However, if activity is unavoidable in unfavorable conditions, precautions can help minimize health risks. For an athletic event, pre-training to provide acclimatization should occur for at least two weeks before the event.6,12 In addition, liberal intake of fluids before thirst begins and attire appropriate for the climate and the activity are recommended. If possible, shading from the sun by a hat or other clothing may be helpful.