
Am Fam Physician. 2002;65(11):2327-2328
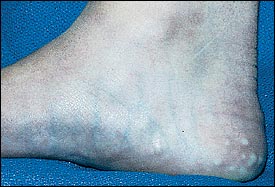
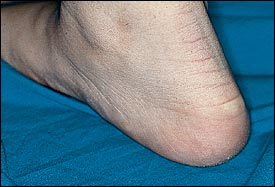
An otherwise healthy 14-year-old girl presented to her family physician with visible growths on the plantar and lateral aspect of both feet (Figure 1). She was especially puzzled because the lesions disappeared in a non–weight-bearing state (Figure 2). Comments from family and classmates, who spoke of the prominence of the lesions, heightened her concern and prompted her visit. The condition was otherwise asymptomatic and she acknowledged that they had been present for several years.
Question
Discussion
The answer is D: Ehlers-Danlos syndrome. Piezogenic pedal papules usually reflect a benign condition consisting of normal fat tissue that has extruded through the dermis. The papules usually appear on the plantar aspect of the foot and heel and are more marked on the medial aspect; they may also occur near the wrist and lateral borders of the hand. They are visible only when the patient is weight bearing and immediately disappear in a non–weight-bearing posture. Occasionally, the papules will be painful. This has been attributed to ischemia of the herniated fatty tissue caused by compressive compromise of its blood supply.
Piezogenic papules are most commonly diagnosed in otherwise healthy patients.1 Usually, they are not suggestive of systemic diseases. Because they are typically painless, they may go unrecognized. They only impair musculoskeletal function if they cause pain from focal ischemic effects, but ulceration does not occur.
Sometimes the papules may be familial.2 Rarely, they may be associated with Ehlers-Danlos syndrome. This patient, however, did not demonstrate hyperlaxity of joints, hyperelasticity of skin, easy bruising, or atrophic skin changes typically seen in Ehlers-Danlos patients. Additionally, no family members reported a history of the syndrome.
Treatment of the papules is usually unnecessary unless they cause pain. Therapeutic measures include use of heel pads and avoidance of prolonged standing. If these interventions fail, excision of the papules can be performed, but this is rarely necessary.
Obesity, per se, is not associated with piezogenic pedal papules, and most patients with piezogenic papules are otherwise healthy.
Piezogenic papules are not seen in Marfan syndrome, in which superficial cutaneous findings are minimal. Striae may be observed over the shoulders and buttocks. Otherwise, the skin is grossly normal. Skeletal abnormalities, including long extremities, are observed. Classically, the hands and fingers are described as spider-like.
Xanthomas can occur in disorders of lipid metabolism, such as familial hyperlipidemia. High triglyceride values exceeding 1,000 mg per dL may result in eruptive xanthomas. These are red-yellow, painless lesions that are most prominent on the buttocks. Their appearance does not change in the weight-bearing state.
Tophi are collections of solid urate that deposit in connective tissues in patients with gout. Common locations include the external ear, foot, hand, prepatellar bursa, and olecranon region. Their appearance also remains unchanged in the non–weight-bearing state.