Atrial fibrillation is the arrhythmia most commonly encountered in family practice. Serious complications can include congestive heart failure, myocardial infarction, and thromboembolism. Initial treatment is directed at controlling the ventricular rate, most often with a calcium channel blocker, a beta blocker, or digoxin. Medical or electrical cardioversion to restore sinus rhythm is the next step in patients who remain in atrial fibrillation. Heparin should be administered to hospitalized patients undergoing medical or electrical cardioversion. Anticoagulation with warfarin should be used for three weeks before elective cardioversion and continued for four weeks after cardioversion. The recommendations provided in this two-part article are consistent with guidelines published by the American Heart Association and the Agency for Healthcare Research and Quality.
In recent years, management strategies for atrial fibrillation have expanded significantly, and new drugs for ventricular rate control and rhythm conversion have been introduced.1–3 Family physicians have the challenge of keeping current with recommendations on heart rate control, antiarrhythmic drug therapy, cardioversion, and antithrombotic therapy.
Atrial fibrillation is the most common sustained arrhythmia encountered in the primary care setting. Approximately 4 percent of persons in the general U.S. population have permanent or intermittent atrial fibrillation, and the prevalence of the arrhythmia increases to 9 percent in persons older than 60 years.2 Atrial fibrillation can result in serious complications, including congestive heart failure, myocardial infarction, and thromboembolism. Recognition and acute management of atrial fibrillation in the physician's office or emergency department are important in preventing adverse consequences.
Diagnosis
The diagnosis of atrial fibrillation should be considered in elderly patients who present with complaints of shortness of breath, dizziness, or palpitations. The arrhythmia should also be suspected in patients with acute fatigue or exacerbation of congestive heart failure.3 In some patients, atrial fibrillation may be identified on the basis of an irregularly irregular pulse or an electrocardiogram (ECG) obtained for the evaluation of another condition.
Cardiac conditions commonly associated with the development of atrial fibrillation include rheumatic mitral valve disease, coronary artery disease, congestive heart failure, and hypertension. Noncardiac conditions that can predispose patients to develop atrial fibrillation include hyperthyroidism, hypoxia, alcohol intoxication, and surgery.4
The ECG is the mainstay for diagnosis of atrial fibrillation (Figure 1). An irregularly irregular rhythm, inconsistent R-R interval, and absence of P waves are usually noted on the cardiac monitor or ECG. Atrial fibrillation waves (f waves), which are small, irregular waves seen as a rapid-cycle baseline fluctuation, indicate rapid atrial activity (usually between 150 and 300 beats per minute) and are the hallmark of the arrhythmia.
FIGURE 1.
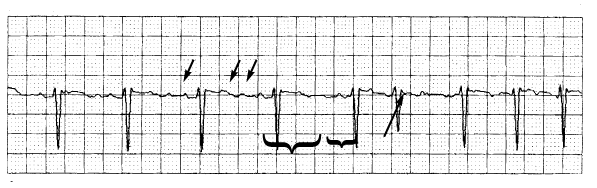
Atrial fibrillation. The tracing demonstrates the absence of P waves (long arrow), as well as the presence of the fine f waves of atrial fibrillation (short arrows). Note the irregularity of the ventricular response, as seen from the variable R-R interval (brackets).
When the fibrillation waves reach 300 beats per minute, they may be difficult to see (fine versus coarse fibrillation).5 These waves may be even harder to detect on a cardiac monitor in a busy emergency department because of interference from other electrical equipment. The f waves may be easier to identify on a printed rhythm strip. In addition, when the ventricular response to atrial fibrillation is very rapid (more than 200 beats per minute), variability of the R-R interval can frequently be seen more easily using calipers on a paper tracing.
Atrial flutter is included in the spectrum of supraventricular arrhythmia. This rhythm disturbance is usually distinguishable by its more prominent saw-tooth wave configuration and slower atrial rates (Figure 2). Atrial fibrillation should also be distinguished from atrial tachycardia with variable atrioventricular block, which usually presents with an atrial rate of approximately 150 beats per minute. In this condition, the atrial rate is regular (unlike the irregular disorganized f waves of atrial fibrillation), but conduction to the ventricles is not regular. The resultant irregularly irregular rhythm may be difficult to differentiate from atrial fibrillation.3
FIGURE 2.
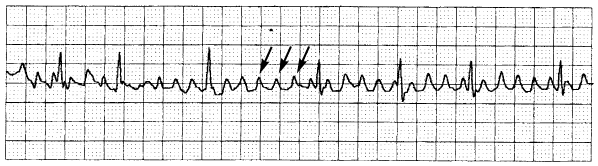
Atrial flutter. Note the saw-tooth wave configuration, or flutter waves (arrows).
Initial Management
Recent advances in treatment and the introduction of new drugs have not changed initial management goals in patients with atrial fibrillation. These goals are hemodynamic stabilization, ventricular rate control, and prevention of embolic complications.4,6–8 When atrial fibrillation does not terminate spontaneously, the ventricular rate should be treated to slow ventricular response and, if appropriate, efforts should be made to terminate atrial fibrillation and restore sinus rhythm4,7,9 (Figure 3).8
FIGURE 3. Initial Management of Atrial Fibrillation
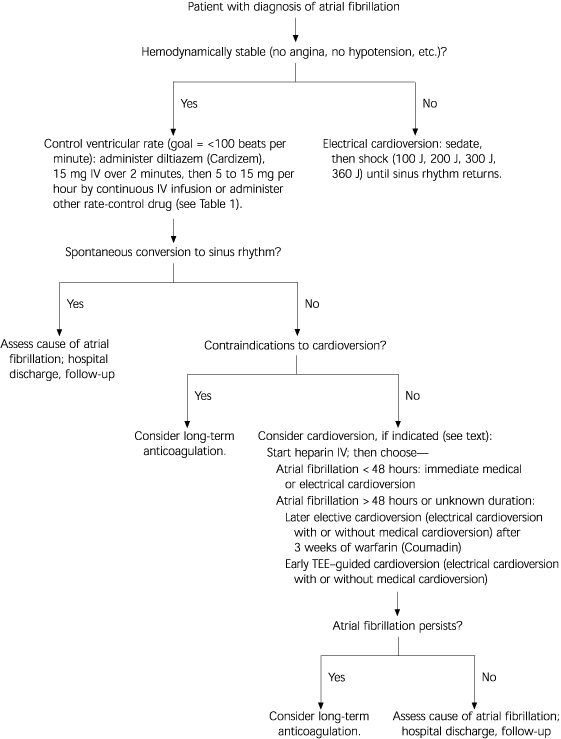
Initial approach to the patient with acute atrial fibrillation. (IV = intravenous; J = joule; TEE = transesophageal echocardiography)
Information from Falk RH. Atrial fibrillation. N Engl J Med 2001;344:1067–78.
VENTRICULAR RATE CONTROL
Ventricular rate control to achieve a rate of less than 100 beats per minute is generally the first step in managing atrial fibrillation. Beta blockers, calcium channel blockers, and digoxin (Lanoxin) are the drugs most commonly used for rate control3,4,7 (Table 1).3 These agents do not have proven efficacy in converting atrial fibrillation to sinus rhythm and should not be used for that purpose.4,7,10,11
TABLE 1 Drugs Commonly Used to Control Ventricular Rate in Patients with Atrial Fibrillation
| Drug | Initial dosing | Maintenance dosing | Comments | |
|---|---|---|---|---|
| Calcium channel blockers | ||||
| Diltiazem (Cardizem) | 15 to 20 mg IV over 2 minutes; may repeat in 15 minutes | 5 to 15 mg per hour by continuous IV infusion | Convenient; easy to titrate to heart rate goal | |
| Verapamil (Calan, Isoptin) | 5 to 10 mg IV over 2 minutes; may repeat in 30 minutes | Not standardized | More myocardial depression and hypotension than with diltiazem | |
| Beta blockers | ||||
| Esmolol (Brevibloc) | Bolus of 500 mcg per kg IV over 1 minute; may repeat in 5 minutes | 50 to 300 mcg per kg per minute by continuous IV infusion | Very short-acting; easy to titrate to heart rate goal | |
| Propranolol (Inderal) | 1 mg IV over 2 minutes; may repeat every 5 minutes to maximum of 5 mg | 1 to 3 mg IV every 4 hours | Short duration of action; hence, need for repeat dosing | |
| Digoxin (Lanoxin) | 0.25 to 0.5 mg IV; then 0.25 mg IV every 4 to 6 hours to maximum of 1 mg | 0.125 to 0.25 mg per day IV or orally | Adjunctive therapy; less effective for rate control than beta blockers or calcium channel blockers | |
IV = intravenous.
Adapted with permission from Li H, Easley A, Barrington W, Windle J. Evaluation and management of atrial fibrillation in the emergency department. Emerg Med Clin North Am 1998;16:389–403.
Beta blockers and calcium channel blockers are the drugs of choice because they provide rapid rate control.4,7,12 These drugs are effective in reducing the heart rate at rest and during exercise in patients with atrial fibrillation.4,7,12 Factors that should guide drug selection include the patient's medical condition, the presence of concomitant heart failure, the characteristics of the medication, and the physician's experience with specific drugs.
Compared with beta blockers and calcium channel blockers, digoxin is less effective for ventricular rate control, particularly during exercise. Digoxin is most often used as adjunctive therapy because of its slower onset of action (usually 60 minutes or more) and its weak potency as an atrioventricular node–blocking agent.3,13 It can be used when rate control during exercise is of less concern.4,7,12 Digoxin is a positive inotropic agent, which makes it especially useful in patients with systolic heart failure.7
The calcium channel blockers diltiazem (Cardizem) and verapamil (Calan, Isoptin) are effective for initial ventricular rate control in patients with atrial fibrillation. These agents are given intravenously in bolus doses until the ventricular rate becomes slower.7 Dihydropyridine calcium channel blockers (e.g., nifedipine [Procardia], amlodipine [Norvasc], felodipine [Plendil], isradipine [DynaCirc], nisoldipine [Sular]), are not effective for ventricular rate control.
Physicians can use the “rule of 15” in administering diltiazem to patients weighing 70 kg (154 lb): first, give 15 mg intravenously over two minutes, repeat the dose in 15 minutes if necessary, and then start an intravenous infusion of 15 mg per hour; titrate the dose to control the ventricular rate (5 to 15 mg per hour). Verapamil, in a dose of 5 to 10 mg administered intravenously over two minutes and repeated in 30 minutes if needed, can also be used for initial rate control. Although all calcium channel blockers can cause hypotension, verapamil should be used with particular caution because of the possibility of prolonged hypotension as a result of the drug's relatively long duration of action.
Beta blockers such as propranolol (Inderal) and esmolol (Brevibloc) may be preferable to calcium channel blockers in patients with myocardial infarction or angina, but they should not be used in patients with asthma. As initial treatment, 1 mg of propranolol is given intravenously over two minutes; this dose can be repeated every five minutes up to a maximum of 5 mg. Maintenance dosing of propranolol is 1 to 3 mg given intravenously every four hours. Esmolol has an extremely short half-life and may be given as a continuous intravenous infusion to maintain rate control (Table 1).3
Despite depressive effects on contractility (unless the ejection fraction is below 0.20), calcium channel blockers and beta blockers can be used for initial ventricular rate control in patients with heart failure. Oxygen delivery to the heart is usually much improved once the ventricular rate is controlled (less than 100 beats per minute). A slower ventricular response rate also allows more filling time for the heart and, thus, improved cardiac output.14 However, the benefits of long-term treatment with calcium channel blockers or beta blockers should be carefully weighed against the negative inotropic effects. Drugs for rate control can generally be stopped once sinus rhythm is restored.3
Limited data suggest that combination regimens provide better rate control than any agent alone.15
RESTORATION OF SINUS RHYTHM
Medical (Pharmacologic) Cardioversion
After patients with atrial fibrillation have been stabilized and the ventricular rate has been controlled, conversion to sinus rhythm is the next consideration. The decision to restore sinus rhythm should be individualized.
The many reasons for not attempting pharmacologic cardioversion include duration of atrial fibrillation for more than 48 hours, recurrence of atrial fibrillation despite multiple treatment attempts, poor tolerance of antiarrhythmic agents, advanced patient age and concomitant structural disease, large size of left atrium (greater than 6 cm), and the presence of sick sinus syndrome.2 However, continued atrial fibrillation is associated with long-term complications that can best be avoided by prompt return to sustained normal sinus rhythm and correction of underlying ischemic or structural abnormality. Early successful cardioversion may also reduce the incidence of recurrent atrial fibrillation.3
Medical cardioversion may be appropriate in certain situations, especially when adequate facilities and support for electrical cardioversion are not available or when patients have never been in atrial fibrillation before. Pharmacologic agents are effective in converting atrial fibrillation to sinus rhythm in about 40 percent of treated patients.2,3
Physicians should use medical cardioversion only after careful consideration of the possibility of proarrhythmic complications, particularly in patients with structural heart disease or congestive heart failure.7 Because cardioversion can lead to systemic emboli, heparin should be given before medical cardioversion is attempted7 (see part II for more information on this subject). Anticoagulation with warfarin (Coumadin) should be continued for four weeks after cardioversion.
After anticoagulation is initiated, quinidine sulfate (Quinidex), flecainide (Tambocor), or propafenone (Rythmol) may be used to attempt pharmacologic conversion. The following intravenously administered drugs may also be used: dofetilide (Tikosyn), ibutilide (Corvert), procainamide, or amiodarone (Cordarone).8,16
A recent review4 and a meta-analysis17 concluded that flecainide, ibutilide, and dofetilide were the most efficacious agents for medical conversion of atrial fibrillation, but that propafenone and quinidine were also effective. In the presence of Wolff-Parkinson-White syndrome, procainamide is the drug of choice for converting atrial fibrillation.7 Less evidence supports the use of disopyramide (Norpace) and amiodarone, and evidence supports a negative effect for sotalol (Betapace).4,17 However, some investigators consider amiodarone to be the most effective agent for converting to sinus rhythm in patients who do not respond to other agents.7
Quinidine, disopyramide, propafenone, and sotalol have been found to be effective in maintaining sinus rhythm. One study comparing amiodarone and disopyramide found moderate evidence of efficacy for amiodarone in the maintenance of sinus rhythm.17
Overall, antiarrhythmic drug selection should be individualized based on the patient's renal and hepatic function, concomitant illnesses, use of interacting medications, and underlying cardiovascular function. Because of intravenous-formulation availability and effectiveness, one drug may be used for conversion and another for maintenance therapy. Amiodarone is the recommended agent in patients with a low ejection fraction (below 0.35) or structural heart disease. Patients should be monitored closely because quinidine, propafenone, and amiodarone may increase the International Normalized Ratio when they are used with warfarin. These same drugs and verapamil raise digoxin levels, which may necessitate a decrease in the digoxin dosage.7
The question of whether rate control or rhythm control should take precedence is currently being investigated in a randomized trial (Atrial Fibrillation Follow-up Investigation of Rhythm Management).18 A recent small study19 examined rate control (using diltiazem) versus rhythm control (using amiodarone) plus anticoagulation. Overall, rate control was as good as rhythm control in reducing or eliminating symptoms and in reducing hospitalization rates, but the comparative effect on stroke risk was not studied.
Electrical Cardioversion
When patients with atrial fibrillation are hemodynamically unstable (e.g., angina, hypotension) and not responding to resuscitative measures, emergency electrical cardioversion is indicated. In stable patients, elective cardioversion is performed after three weeks of warfarin therapy.7,8 To prevent thrombus formation, warfarin is continued for four weeks after cardioversion. Although the success rate for electrical cardioversion is high (90 percent), proper equipment and expertise are necessary for safe performance.3
If there is time and patients are conscious, sedation should be achieved before cardioversion is attempted. Synchronized external direct-current cardioversion is performed with the pads placed anteriorly and posteriorly (over the sternum and between the scapulae) at 100 joules (J). If no response occurs, the current is applied again at 200 J; if there is still no response, the current is increased to 300 J, and then to a maximum of 360 J. If patients cannot be moved, the pads can be applied over the right sternal border and left lateral chest wall.3
Patients with atrial fibrillation at a ventricular rate of less than 150 beats per minute who are hemodynamically stable can be initially treated with drugs for ventricular rate control and intravenously administered heparin for anticoagulation (see part II for more information). Medical cardioversion or elective electrical cardioversion can then be considered as appropriate. Patients are usually monitored in the hospital while cardioversion is being attempted. However, one study20 documented positive results for emergency-department performance of cardioversion followed by direct discharge of hemodynamically stable patients without congestive heart failure.
An alternative approach for achieving earlier return to sinus rhythm is early electrical cardioversion and the use of transesophageal echocardiography according to American Heart Association guidelines.7 Transesophageal echocardiography is used to detect thrombi in the right atrium. If no thrombi are present, electrical cardioversion can be performed immediately; if thrombi are detected, cardioversion can be delayed until patients have undergone three weeks of oral anticoagulation using warfarin.21 One recent comparative study22 found no differences in thromboembolic complications between conventional treatment and early cardioversion following transesophageal echocardiography.
Because of the risk of complications such as heart failure and embolic stroke, restoration of sinus rhythm is thought to be preferable to allowing atrial fibrillation to continue. However, restoration of sinus rhythm is not always possible. In elderly patients with longstanding atrial fibrillation, repeated attempts at cardioversion may be counterproductive. The chances of reverting to and maintaining sinus rhythm are lower with longer duration of atrial fibrillation and decrease to particularly low levels when atrial fibrillation has been present for more than one year. When cardioversion is inappropriate or unsuccessful, medication should be used for ventricular rate control, and anticoagulation therapy should be considered.
General recommendations for the initial management of atrial fibrillation are summarized in Table 2.2,3,7,8,22
TABLE 2 General Recommendations for Initial Management of Atrial Fibrillation
| Acute control of the ventricular rate is best achieved with an intravenously administered calcium channel blocker (e.g., diltiazem [Cardizem]) or beta blocker (e.g., esmolol [Brevibloc]). |
| Immediate electrical cardioversion should be considered in hemodynamically unstable patients with atrial fibrillation. |
| Medical (pharmacologic) or electrical cardioversion following anticoagulation should be considered in hemodynamically stable patients with atrial fibrillation. |
| Elective electrical cardioversion should be used in patients with persistent or recurrent atrial fibrillation. The success rate for electrical cardioversion is 90%. |
| Medical cardioversion is a convenient and reasonable alternative in some patients, but it does not always terminate atrial fibrillation. The success rate for medical cardioversion is about 40%. |
| Early cardioversion after transesophageal echocardiography with intravenous anticoagulation is an increasingly used alternative strategy. |

