Am Fam Physician. 2002;66(4):643-646
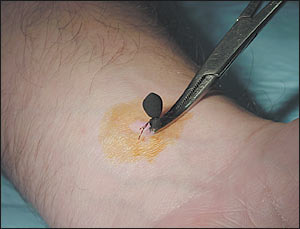
Many methods of tick removal that have been reported in the literature have proved to be unsatisfactory in controlled studies. Some methods may even cause harm by inducing the tick to salivate and regurgitate into the host. Ticks are best removed as soon as possible, because the risk of disease transmission increases significantly after 24 hours of attachment. The use of a blunt, medium-tipped, angled forceps offers the best results. Following tick removal, the bite area should be inspected carefully for any retained mouthparts, which should be excised. The area is then cleaned with antiseptic solution, and the patient is instructed to monitor for signs of local or systemic illness. Routine antibiotic prophylaxis following tick removal generally is not indicated but may be considered in pregnant patients or in areas endemic to tick-borne disease.
Because tick bites are nearly painless, a tick may not be noticed until after it is attached. It is important to remove the tick from the host as soon as possible after it is discovered. Animal and human studies have shown that the risk of Lyme disease transmission increases significantly after 24 hours of attachment and is even higher after more than 48 hours.1–6
In addition to timely removal, it is important to remove the tick completely, including the mouthpart and the cement the tick has secreted to secure attachment. Improper tick removal may cause mouthparts to break off in the skin, possibly leading to infection or granuloma formation.7 Twisting off the head should be avoided, because this may cause the tick's potentially infectious body fluids to escape.
Ticks should never be handled with bare hands and should be disposed of with hazardous waste or preserved in alcohol if identification is needed.
Few methods for tick removal that have been reported in the literature have scientific support. Some methods that are not recommended (Table 1) include applying a hot match or nail to the tick body; covering the tick with petroleum jelly, nail polish, alcohol or gasoline; using injected or topical lidocaine (Xylocaine); or passing a suture needle through the tick.8–15 Although there is conflicting evidence as to whether the removal technique influences infection rates,6,10,16 these methods may induce the tick to salivate and regurgitate into the attachment site, theoretically increasing the risk of infection.8,11
| Do not use sharp forceps. |
| Do not crush, puncture, or squeeze the tick's body. |
| Do not apply substances such as petroleum jelly, gasoline, lidocaine (Xylocaine), etc., to the tick. |
| Do not apply heat with a match or hot nail. |
| Do not use a twisting or jerking motion to remove the tick. |
| Do not handle the tick with bare hands. |
Commercially available tick-removal devices include the Sawyer Tick Pliers (B&A Products, Bunch, Okla.), Pro-Tick Remedy (SCS Limited, Stony Point, N.Y.) and Ticked Off (Ticked Off Inc., Dover, N.H.). Although one study17 found that the Pro-Tick Remedy and Ticked Off devices left mouthparts in the skin less often, all three devices listed above were recommended over tweezers for tick removal. Another study2 recommended the Ticked Off device but did not compare it with other devices. There are other commercially available tick-removal devices, but no studies have evaluated their usefulness.
After a tick is removed, an antiseptic solution is applied to the attachment site, and patients should be educated about the signs and symptoms of local and systemic illness. There is conflicting evidence as to the need for routine antibiotic prophylaxis.22–24 Although a discussion of evidence is beyond the scope of this article, most experts, including the Centers for Disease Control and Prevention and the Infectious Diseases Society of America, do not recommend routine antibiotic prophylaxis.25,26 [Reference 26—Evidence level C, expert opinion] However, antibiotic use may be considered in patients who are deemed high-risk, in pregnant patients, and in patients living in areas endemic to tick-borne disease.2,18