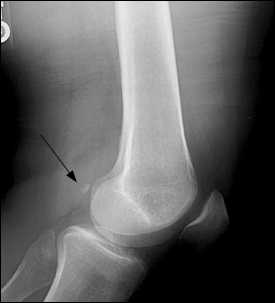
A 38-year-old woman presented with a two-month history of left lateral knee pain. The pain appeared after she had started an aerobic exercise program that combined martial arts and shadow boxing. Physical examination revealed tenderness over the lateral aspect of the popliteal fossa, directly behind the lateral femoral condyle. Further findings on examination were normal, without evidence of ligamentous laxity or effusions. Around object of bony density was apparent on the film adjacent to the lateral femoral condyle, corresponding to the area of tenderness (see accompanying figure).
Question
Based on findings of the patient's history, physical examination, and films, which one of the following conditions is causing the sore knee?
A. Osteochondral defect.
B. Osteochondritis dissecans.
C. Calcific tendonitis.
D. Fabella syndrome.
E. Foreign body.
Discussion
The answer is D: fabella syndrome. The fabella is a sesamoid bone of the lateral gastrocnemius muscle. It is directly posterior to the lateral femoral condyle. It is present in 10 to 20 per cent of the population. It serves as an attachment point for the popliteus and arcuate ten don complex and the fabellofibular ligament.1
Fabella syndrome is characterized by the slow onset of sharp, intermittent pain in the posterolateral aspect of the knee. On full extension, the knee will reveal localized ten derness over the fabella. The syndrome is most common in early adolescence2 and most likely is the result of repetitive friction of the fabella over the posterolateral femoral condyle. Treatment should follow the PRICE (protection, rest, ice, compression, and elevation) mnemonic. Nonsteroidal anti-inflammatory drugs can be used to control the pain. Some physicians have advocated the use of heel lifts to shorten the gastrocnemius muscle. If conservative measures fail after about six months, surgical excision may be considered.3
An osteochondral defect is complete or incomplete separation of the joint cartilage and subchondral bone. It is by definition intra-articular. One should not confuse osteochondral defect with osteochondritis dissecans. The former is a traumatic injury usually in skeletally mature people, while the latter is a condition of adolescents caused by an interaction between repetitive trauma and a genetic predisposition to the problem.4 The most common location for both conditions in the knee is the medial femoral condyle. The usual presentation is pain, swelling, and intermittent locking or catching.
Calcific tendonitis can occur at any tendon location in the body. It is usually caused by an overuse injury, resulting in anterior knee pain. In the knee, the most common lesion would be a patellar or supraspinatus ten donitis. The posterolateral location of pain in this cause would be atypical.
A foreign body usually presents with a history of trauma and an entrance wound that will not heal. The smooth contours of the object in these films and a radiodensity identical to adjacent bone suggest a sesamoid, not a foreign object.

