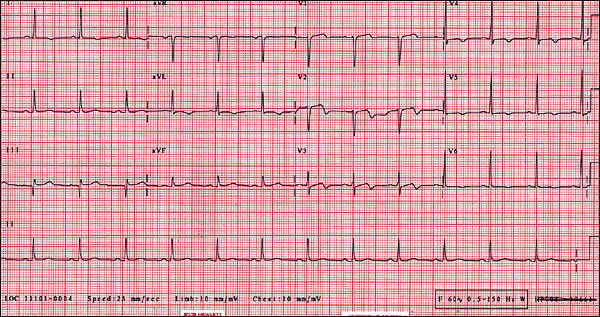
A 63-year-old man complained of pain in his substernal and epigastric region for the past three weeks. The pain occurred after walking a great distance or after he ate, and it resolved with rest. He experienced no radiation of the pain, and no shortness of breath, nausea, or diaphoresis. The patient reported no cardiac history or family history of coronary artery disease. His medical history was notable for type 2 diabetes mellitus for which he took metformin (Glucophage). Other medications included an antacid and omeprazole (Prilo-sec). He stopped smoking 10 years ago, but he did have a 20 pack-year history. He was pain-free at the time of the interview. Physical examination was unremarkable. An electrocardiogram was obtained (see accompanying figure).
Question
Based on the history and electrocardiographic findings, this patient most likely has which one of the following conditions?
A. Early repolarization changes.
B. Transmural anterior wall myocardial infarction.
C. Hyperkalemia.
D. Hypokalemia.
E. Proximal left anterior descending lesion.
Discussion
The answer is E: proximal left anterior descending (LAD) lesion. The electrocardiogram (ECG) shows Wellens' sign in leads V2 and There are also nonspecific T-wave V3. abnormalities in the lateral and precordial leads (flipped T waves in I, avL, V4-V6) and a nonpathologic Q wave in lead III.
Dr. Hein J.J. Wellens and colleagues first described this ECG finding in 1982.1 They identified a subgroup of patients with angina who showed a characteristic biphasic T-wave appearance. Patients in this subgroup had a critical proximal LAD lesion. Seventy-five percent of these patients who did not have surgery progressed to have extensive anterior wall myocardial infarctions.1 The patient described in this case had a severe LAD lesion diagnosed by angiography.
Early repolarization changes often lead to abnormal appearing ST-T-wave complexes in the precordial leads. They usually occur in young adults and are characterized by an elevated initial portion of the ST segment (J-point elevation), not a biphasic T wave.
There is no evidence of transmural anterior wall myocardial infarction; however, the natural history of Wellens' syndrome is eventual development of this injury.
There is no evidence for hyperkalemia, which presents with peaked T waves in each lead. The Wellens' sign can be mistaken for the U wave often seen with hypokalemia. The important difference is the biphasic nature of the Wellens' T wave. A U wave is concave upward in concordance with the T wave it follows.
Biphasic T waves in leads V2 and V3 comprise Wellens' sign. This finding is part of the Wellens' syndrome, which includes a history of chest pain, normal or minimally elevated cardiac enzymes, absence of precordial Q waves, no pathologic ST elevation, and no loss of R waves in the precordium.2 An alternate, and actually more common, T-wave abnormality with proximal LAD lesions is deep inversion in leads V2 and V3.3
It is important to recognize the biphasic T wave, despite its subtle nature, because it helps identify a high-risk patient who will not do well with conservative management.1,4 Wellens' sign is unlikely to be diagnosed accurately by computer interpretation.2 Furthermore, the sign tends to appear during pain-free intervals.5
The approach to a patient with nonspecific T-wave abnormalities on ECG often involves cardiac stress testing. If the T-wave abnormality is actually Wellens' sign, stress testing is contraindicated and may provoke a fatal outcome.2 Prompt cardiology consultation and angiography comprise the appropriate work-up of this important finding.

