Pain is one of the most common symptoms in patients with advanced cancer. Approximately 70 to 90 percent of patients with advanced cancer report some component of pain. There are two types of pain patterns: continuous baseline and transitory exacerbations. The transitory exacerbation of pain is known by several different names, including episodic pain, breakthrough pain, end-of-dose failure, exacerbation of pain, incident pain, pain flare, transient pain, and transitory pain. Zeppetella and Ribeiro reviewed the treatment of this pain in patients with advanced cancer and labeled it episodic pain.
When providing pain control in any setting, an assessment of the characteristics of the pain is vital in establishing treatment strategies. This assessment includes pain location, severity, temporal characteristics such as frequency, onset, course and duration, relationship to analgesia, precipitating events, predictability, pathophysiology, etiology, and palliative factors. This assessment can be assisted with the use of an episodic pain document form (see accompanying figure). The authors point out that episodic pain will be unique and different for each patient, and there may also be more than one pain syndrome present.
FIGURE.
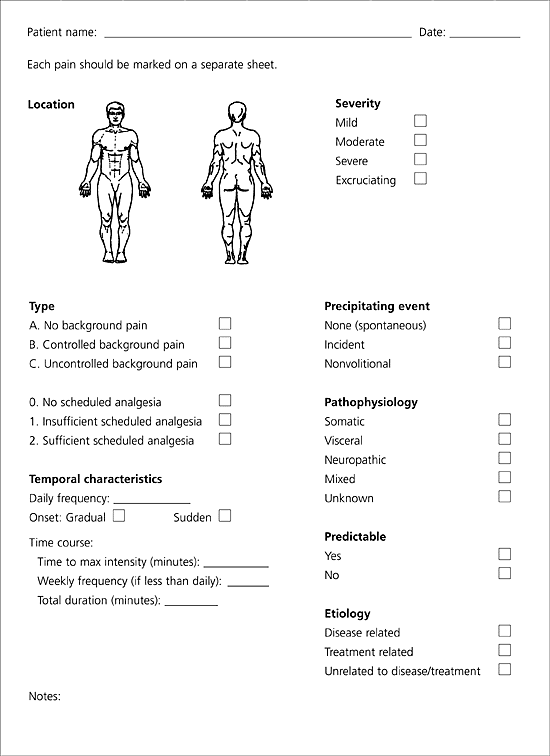
Episodic pain document form.
Adapted with permission from Zeppetella G, Ribeiro MD. Episodic pain in patients with advanced cancer. Am J Hosp Palliative Care 2002;19:271.
The authors state that there are three principles for the management of episodic pain, including (1) implementation of primary therapies for the underlying etiology of pain, (2) optimizing the scheduled analgesic regimen, and (3) using pharmacologic and non-pharmacologic interventions specifically for the episodic pain. Primary therapies include chemotherapy, radiotherapy, and biologic or hormone therapy when tumors are likely to respond to these agents. Optimizing analgesia includes using the World Health Organization's three-step analgesia ladder with nonopi-oids for step-one mild pain, weak opioids for step-two moderate pain and those in step one who do not respond to nonopioids, and strong opioids for step-three severe pain and those who fail to respond to step-two strategies. In addition, adjuvant medications can be used to treat certain pain types and reduce the dosage of opioids. An example of this is using anticonvulsants to treat neuropathic pain.
Nonpharmacologic modalities also can be used to treat episodic pain. These include transcutaneous electrical nerve stimulation units, acupuncture, relaxation techniques, and physiotherapy.
Specific analgesia medications can be used for episodic pain. The first is oral opioids, which can be used when episodic pain develops; in the case of morphine, the rescue dose should be 10 to 15 percent of the daily dose. Parenteral opioids also can be used and are best reserved for occasions when rapid pain relief or rapid dose adjustment is needed. Subcutaneous injection is the preferred route, but this choice requires a health care professional to insert the needle. Sublingual opioids also are available. Rectal opioids are another option, but they tend to have unreliable absorption. Oral transmucosal fentanyl citrate, which is a fentanyl-impregnated lozenge, can be used for episodic pain because it has a rapid onset of action and short duration.
Episodic pain is unique for each patient and is often unpredictable. The authors conclude that the successful management of episodic pain in patients with advanced cancer depends on comprehensive assessment and management strategies that combine pharmacologic and nonpharmacologic modalities.

