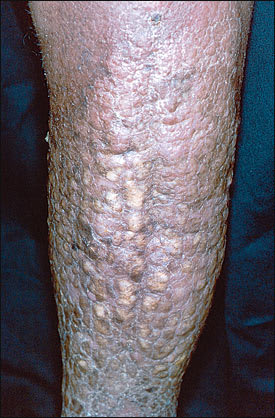
A 69-year-old man presented with severe bilateral lower extremity woody edema, pebbly hyperkeratotic plaques, and a fetid odor (see accompanying figure). Crusts were easily dislodged and left weeping erosions. This condition had progressed over many years of chronic lymphedema and recurrent skin infections.
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Venous stasis dermatitis.
B. Elephantiasis nostras.
C. Pretibial myxedema.
D. Filariasis (elephantiasis tropica).
E. Ichthyosis.
Discussion
The answer is B: elephantiasis nostras. It is a disorder in which chronic lymphedema and recurrent skin infection result in severely deformed fibrotic enlargement of the affected extremity.1–4 The epidermis becomes cobblestoned with a loosely adherent crust, which is often foul smelling and may be colonized with multiple bacteria and fungi.2–4
The differential diagnosis includes venous stasis dermatitis, pretibial myxedema, filariasis, and ichthyosis. Venous stasis dermatitis, caused by chronic venous insufficiency, is characterized by pitting edema and hemosiderin-stained, tight skin in which minor trauma causes ulceration. Pretibial myxedema, associated with Graves' disease, is caused by intradermal mucin accumulation. The usual manifestation is bilateral pretibial flesh-colored nodules or plaques. Filariasis can cause localized lymphedema. Blockage of lymph channels by filarial worms leads to edema most commonly affecting the legs and genital area. If filariasis is suspected on the basis of a travel history to an endemic tropical area, it can be diagnosed by serologic studies or by finding filarial worms in body fluids. Ichthyosis is a general term for a variety of genetic and acquired disorders that lead to development of thickened hyperkeratotic scales on the skin. Unlike elephantiasis nostras, there is no history of recurrent infection or chronic edema leading to the formation of the hyperkeratotic skin changes.
Lymphedema, regardless of etiology, is a predisposition for the development of elephantiasis nostras. However, it is the recurrent infections that cause the most damage. Repeated episodes of inflammation lead to fibrosis of the dermis and lymph channels that ultimately results in elephantiasis nostras.5–7
Treatment of elephantiasis nostras aims at prevention of recurrent infection and edema. Compressive stockings are used to decrease edema. In severe cases, pneumatic compression devices may be useful.6 Prolonged courses of antibiotics may be needed to clear deep-seated infections. Topical keratolytics and oral retinoids have been used to treat hyperkeratotic plaques, but chronic use is sometimes required to maintain the results and is not risk free.7 Recalcitrant cases may benefit from surgical intervention such as lymphovenous anastomosis but ultimately may require amputation. Early treatment of infection to eradicate bacteria and preserve the lymphatic drainage of dependent extremities is essential.

