The shoulder is the site of multiple injuries and inflammatory conditions that lend themselves to diagnostic and therapeutic injection. Joint injection should be considered after other therapeutic interventions such as nonsteroidal anti-inflammatory drugs, physical therapy, and activity-modification have been tried. Indications for glenohumeral joint injection include osteoarthritis, adhesive capsulitis, and rheumatoid arthritis. For the acromioclavicular joint, injection may be used for diagnosis and treatment of osteoarthritis and distal clavicular osteolysis. Subacromial injections are useful for a range of conditions including adhesive capsulitis, sub-deltoid bursitis, impingement syndrome, and rotator cuff tendinosis. Scapulothoracic injections are reserved for inflammation of the involved bursa. Persistent pain related to inflammatory conditions of the long head of the biceps responds well to injection in the region. The proper technique, choice and quantity of pharmaceuticals, and appropriate follow-up are essential for effective outcomes.
This article, the third in a series on diagnostic and therapeutic injections, covers the shoulder region. The rationale, indications, contraindications and general approach to this technique are covered in the first article1 in this series published in the July 15, 2002 issue. The shoulder is the site of multiple injuries and inflammatory conditions that lend themselves to diagnostic and therapeutic injection.2–4 This article covers the anatomy, pathology, diagnosis, and injection technique of common sites in which this skill is applicable.
Glenohumeral Joint
The glenohumeral joint represents the articulation of the humerus with the glenoid fossa, and it is the most mobile joint in the body. The glenohumeral joint is not a true ball and socket joint. The articulation is stabilized by the soft tissue configurations of a number of ligaments and muscles, including the four muscles of the rotator cuff (supraspinatus, infraspinatus, teres minor, and subscapularis) that serve as dynamic stabilizers of the joint. Static stabilizers include the joint capsule, the glenoid labrum, and the glenohumeral ligaments.
INDICATIONS AND DIAGNOSIS
Joint injection in this area should be considered only after other appropriate therapeutic interventions have been tried. These include the use of nonsteroidal anti-inflammatory drugs (NSAIDs), physical therapy, and other disease-modifying agents for rheumatoid arthritis. There are three major indications for a glenohumeral joint injection: osteoarthritis, adhesive capsulitis (frozen shoulder),5–14 and rheumatoid arthritis.11
Osteoarthritis of the shoulder typically occurs in older persons or following traumatic injury in younger persons. Patients usually present with chronic pain, decreased range of motion, and accompanying weakness. Although radiographs can assist in the diagnosis, findings do not always correlate with clinical symptoms or functioning. Adhesive capsulitis is a condition typically occurring in middle-aged and older adults, and it is usually associated with a traumatic injury or nonuse of the shoulder secondary to pain, discomfort, or prolonged immobilization. The condition is more common in women and persons with diabetes.12 There is often accompanying tendinosis or bursitis. Rheumatoid arthritis is a systemic inflammatory disease of autoimmune nature that involves inflammation of the synovium of the shoulder joint.
Diagnosis of glenohumeral joint pathology is suspected clinically, and on physical examination, the physician may find painful and decreased range of motion, generalized weakness, and palpable crepitus with shoulder movement.15 Radiographs may be helpful in confirming the diagnosis. Historical factors also cue the diagnosis, with osteoarthritis being more insidious in onset, and rheumatoid arthritis, while chronic in nature, being punctuated by periodic exacerbations secondary to inflammation. In adhesive capsulitis, progressive worsening of pain occurs with loss of motion and a firm, painful end point in the range of motion during physical examination.
TECHNIQUE
The glenohumeral joint can be injected from an anterior, posterior, or superior approach. The anterior and posterior approaches, which are used more often, are described here. In each case, the joint is most easily accessible with the patient sitting, the patient's arm resting comfortably at the side, and the shoulder externally rotated. Essential landmarks to palpate before performing this injection include the head of the humerus, the coracoid process, and the acromion.
TABLE 1 Equipment and Pharmaceuticals
| Site | Syringe | Needle | Anesthetic | Corticosteroid* | Hydrocortisone equivalents/injection (mg) | ||
|---|---|---|---|---|---|---|---|
| Glenohumeral joint | 10 mL | 25 gauge, 1.5 inches | 5 to 7 mL of 1% lidocaine (Xylocaine) | 1 to 2mL betamethasone sodium phosphate and acetate (Celestone Soluspan) | 150 to 300 | ||
| or | or | ||||||
| 0.25% or 0.5% bupivacaine (Marcaine) | 1 to 2 mL methylprednisolone (Depo-Medrol), 40 mg/mL | 200 to 400 | |||||
| Acromioclavicular joint | 3 to 5 mL | 25 gauge, 1 to 1.5 inches | 0.5 mL of 1% lidocaine | 0.25 to 0.5 mL betamethasone sodium phosphate and acetate | 37.5 to 75 | ||
| or | or | ||||||
| 0.25% or 0.5% bupivacaine | 0.25 to 0.5 mL methylprednisolone, 40 mg/mL | 50 to 100 | |||||
| Subacromial space | 10 mL | 25 gauge, 1.5 inches | 5 to 7 mL of 1% lidocaine | 1 to 2 mL betamethasone sodium phosphate and acetate | 150 to 300 | ||
| or | or | ||||||
| 0.25% or 0.5% bupivacaine | 1 to 2 mL methylprednisolone, 40 mg/mL | 200 to 400 | |||||
| Scapulothoracic articulation | 3 to 5 mL | 25 gauge, 1.5 inches | 1 to 2 mL of 1% lidocaine | 0.5 to 1 mL betamethasone sodium phosphate and acetate | 75 to 150 | ||
| or | or | ||||||
| 0.25% or 0.5% bupivacaine | 0.5 to 1 mL methylprednisolone, 40 mg/mL | 100 to 200 | |||||
| Area of biceps tendon | 3 to 5 mL | 25 gauge, 1 to 1.5 inches | 0.5 mL of 1% lidocaine | 0.25 mL betamethasone sodium phosphate and acetate | 37.5 | ||
| or | or | ||||||
| 0.25% or 0.5% bupivacaine | 0.25 mL methylprednisolone, 40 mg/mL | 50 | |||||
*— Other preparations such as triamcinolone or dexamethasone may be used.
Anterior Approach
The needle (Figure 1) should be placed just medial to the head of the humerus and 1 cm lateral to the coracoid process. The needle is directed posteriorly and slightly superiorly and laterally. If the needle hits against bone, it should be pulled back and redirected at a slightly different angle.
FIGURE 1.
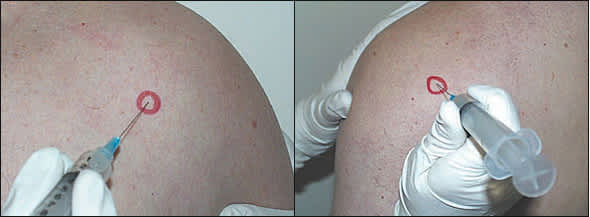
(Left) Anterior approach to the glenohumeral joint. (Right) Posterior approach to the glenohumeral joint.
Posterior Approach
The needle (Figure 1) should be inserted 2 to 3 cm inferior to the posterolateral corner of the acromion and directed anteriorly in the direction of the coracoid process. As with any injection, aspiration should be done to ensure that there has not been needle placement in the blood vessel. The injection should be performed slowly, but with consistent pressure.
Follow-up care should include the following recommendations. Patients should remain seated or placed in supine position for several minutes after the injection. To ascertain whether the pharmaceuticals have been delivered to the appropriate location, the joint or area may be put through passive range of motion. The patient should remain in the office to be monitored for 30 minutes after the injection, and the patient should avoid strenuous activity involving the injected region for at least 48 hours. Patients should be cautioned that they might experience worsening symptoms during the first 24 to 48 hours, related to a possible steroid flare, which can be treated with ice and NSAIDs. A follow-up examination should be arranged within three weeks.
Acromioclavicular Joint
The acromioclavicular (AC) joint is a diarthrodial joint that connects the acromion to the distal clavicle. The AC ligament is weak and provides little joint stability. Rather, the coracoclavicular ligament (trapezoid and conoid ligaments) provides the major structural support for the joint and is the primary ligament injured in an AC sprain, otherwise known as a separated shoulder.
INDICATIONS AND DIAGNOSIS
Therapeutic injection of the AC joint should be performed only after a trial of other therapeutic modalities such as relative rest, activity modification, and NSAIDs. Indications for injection of the AC joint include osteolysis of the distal clavicle and osteoarthritis.17 Osteolysis of the distal clavicle is a degenerative process that results in chronic pain, particularly with adduction movements of the shoulder. Osteolysis of the distal clavicle is typically seen secondary to traumatic injury or in persons who perform repetitive weight training involving the shoulder. Osteoarthritis also may develop in the AC joint and typically develops secondary to previous trauma or injury.
History and physical examination are important in making the diagnosis of osteolysis of the distal clavicle or osteoarthritis. In each condition, patients usually have insidious onset of pain. On physical examination, there is tenderness to palpation of the AC joint, and pain with active or passive adduction (reaching the arm across the body) of the shoulder. Pain can be exacerbated by having the patient hold the opposite shoulder and pushing the elbow toward the ceiling against resistance. Radiographs of the AC joint will confirm the diagnosis of osteolysis or osteoarthritis.
In some cases, it may be difficult to differentiate pain from AC joint pathology from other shoulder pathology, particularly rotator cuff impingement syndrome. Injecting 5 mL of 1 percent lidocaine (Xylocaine) into the subacromial space to eliminate this as the source of pain is a useful test. If pain is still present, the test localizes the AC joint as the probable source of pain. Patients with osteolysis or arthritis of the AC joint will not have temporary relief of symptoms following the injection.
TECHNIQUE
Patients are placed in the supine or seated position with the affected arm resting comfortably at their side. To identify the AC joint, palpate the clavicle distally to its termination at which point a slight depression will be felt at the joint articulation. Aseptic technique is followed. Pharmaceuticals and equipment are listed in Tables 1 and 2.16 The needle is inserted from the superior and anterior approach into the AC joint and directed inferiorly (Figure 2). The pharmaceutical solution is injected evenly and slowly. Follow-up care is the same as described for the glenohumeral joint.
FIGURE 2.
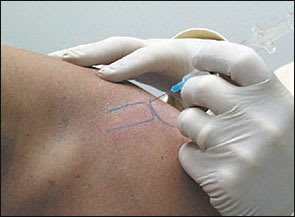
Acromioclavicular joint.
Subacromial Space
Important structures defining the subacromial space include the acromion, subdeltoid bursa, coracoacromial ligament, and supra-spinatus tendon, which inserts into the greater tuberosity of the humerus. The shape of the acromion affects the subacromial space and is a contributor to impingement syndrome. The susceptibility to impingement syndrome increases as the degree of curve in the acromion increases.
INDICATIONS AND DIAGNOSIS
Typically, a subacromial injection is performed after a trial of more conservative therapy.18 For the patient who presents with severe pain and acute onset of symptoms consistent with subdeltoid bursitis, the best treatment plan may be injection at the initial visit. Persistent pain unresponsive to therapy, including injection therapy, should prompt the physician to consider other causes, such as Parsonage-Turner syndrome, a rare disorder of unknown cause that involves chronic shoulder pain.
Four common indications for therapeutic injection in this area are subdeltoid bursitis, rotator cuff impingement, rotator cuff tendinosis, and adhesive capsulitis.19 Subdeltoid bursitis (or subacromial bursitis) can be the result of traumatic injury or chronic overuse, and it frequently accompanies other shoulder problems. A history of pain in the lateral shoulder and tenderness to palpation along the acromial border indicates a diagnosis of subdeltoid bursitis.
Tendonitis, more properly termed tendinosis, results from acute or chronic stress of the rotator cuff tendons. Rotator cuff impingement results from repeated irritation of the rotator cuff beneath the acromial arch.20 Repetitive overhead reaching and weight training are frequent precipitants of rotator cuff tendinosis and impingement. Rotator cuff tendinosis is diagnosed by eliciting pain or weakness with stress testing of the rotator cuff muscles. There are two common tests used for diagnosis of impingement. The Hawkins' test elicits pain with the shoulder passively flexed to 90 degrees and internally rotated.21 The Neer's test elicits pain with passive abduction of the shoulder to 180 degrees.22 Radiographs, if obtained, may show calcific deposits in the subacromial space or at the insertion of the supraspinatus tendon to the greater tuberosity. In cases of impingement, curvature of the acromion process may be seen.
Adhesive capsulitis can also be treated with a subacromial injection. The subacromial bursa is involved in most cases of adhesive capsulitis.23 For adhesive capsulitis, the use of a subacromial corticosteroid injection should be combined with other treatment modalities, including physical therapy.
At times, it may be difficult to differentiate the diagnosis of shoulder pain. Subacromial injection can be used for diagnostic purposes. Injecting 5 mL of 1 percent lidocaine into the subacromial space can help differentiate rotator cuff tendinosis or impingement from other shoulder disorders, such as osteoarthritis of the glenohumeral or acromioclavicular joints and labral or rotator cuff tears. Patients with tendinosis or impingement will have temporary relief of symptoms and will have increased range of motion and strength following the injection.
TECHNIQUE
The distal, lateral, and posterior edges of the acromion are palpated. Pharmaceuticals and equipment are listed in Tables 1 and 2.16 Using aseptic technique, the needle is inserted just inferior to the posterolateral edge of the acromion (Figure 3). The needle is directed toward the opposite nipple. The pharmaceutical material should flow freely into the space without any resistance or significant discomfort to the patient. Follow-up care is the same as previously described.
FIGURE 3.
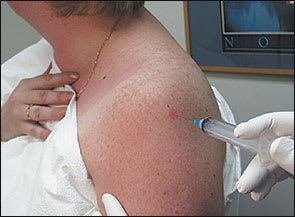
Subacromial space.
Scapulothoracic Articulation
This is not a true joint, but rather represents the position of the scapula on the posterior thoracic cage on which it freely moves. Lateral to the inferior medial border of the scapula is a bursa that can become inflamed.
INDICATIONS AND DIAGNOSIS
Injection is performed after a trial of other modalities, including NSAIDs, strengthening of the rotator cuff, and the scapular stabilizer muscles. This area is the site of inflammation associated with various activities, including throwing, weight lifting, and activities, of daily living involving pushing or pulling.24 Diagnosis is assisted by obtaining a history of pain with any of the above activities, which frequently will cause the sensation of popping or catching with the offending motion. Palpation of the area may reveal tenderness on the inferior medial border of the scapula, as well as crepitus with movement or compression of the scapula against the chest wall.
TECHNIQUE
The patient is placed in the prone position with the ipsilateral hand placed on the buttock to open up the scapulothoracic space. The inferior medial border of the scapula is then palpated. Aseptic technique is used. Pharmaceuticals and equipment are listed in Tables 1 and 2.16 The needle is inserted along the inferior medial border of the scapula and directed parallel to the plane of the undersurface of the scapula, not toward the chest wall (Figure 4). Follow-up care is the same as previously described.
FIGURE 4.
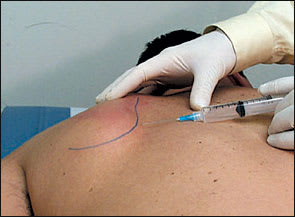
Scapulothoracic articulation.
Long Head of the Biceps Tendon
The long head of the biceps tendon travels through the bicipital groove to insert on the head of the humerus.25 This is a site for inflammation with any repetitive motion involving flexion of the shoulder. Weight lifters, masons, and rock climbers are at particular risk. Pain and tenderness of the long head of the biceps tendon commonly occur in the presence of rotator cuff tendinosis.
INDICATIONS AND DIAGNOSIS
This injection should be performed only after the patient has failed all conservative treatments, including NSAIDs, avoidance of precipitating activities, and a course of physical therapy. Repeat injections should be avoided because of the possibility of tendon rupture. Underlying rotator cuff pathologies should be treated before injection.
Persistent pain secondary to inflammation of the bicipital tendon is an indication for therapeutic injection. Diagnosis is usually made by eliciting pain with palpation of the tendon along the bicipital groove to its origin. A positive Speed's test is the elicitation of pain with the patient's shoulder flexed to 60 degrees, elbow extended to 150 to 160 degrees, palm supinated, and pushing up against resistance.
TECHNIQUE
The patient should be sitting or in a supine position, the bicipital tendon is identified in the groove, and the point of insertion noted. Pharmaceuticals and equipment are listed in Tables 1 and 2.16 To inject into the area of the long head of the biceps tendon, the needle is inserted directly into the most tender area over the bicipital groove. The needle should enter the skin at 30 degrees and be directed parallel to the groove (Figure 5). The objective is to infiltrate the area in and around the groove and not into the tendon. Intratendinous injection has been associated with rupture. Intratendinous needle placement can be appreciated by increased resistance to flow of the pharmaceutical. Follow-up care is the same as previously described.
FIGURE 5.
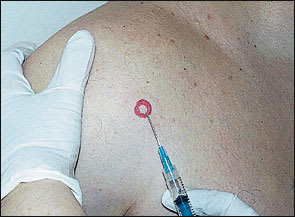
Biceps tendon region.

