Acute abdominal pain in children presents a diagnostic dilemma. Although many cases of acute abdominal pain are benign, some require rapid diagnosis and treatment to minimize morbidity. Numerous disorders can cause abdominal pain. The most common medical cause is gastroenteritis, and the most common surgical cause is appendicitis. In most instances, abdominal pain can be diagnosed through the history and physical examination. Age is a key factor in evaluating the cause; the incidence and symptoms of different conditions vary greatly over the pediatric age spectrum. In the acute surgical abdomen, pain generally precedes vomiting, while the reverse is true in medical conditions. Diarrhea often is associated with gastroenteritis or food poisoning. Appendicitis should be suspected in any child with pain in the right lower quadrant. Signs that suggest an acute surgical abdomen include involuntary guarding or rigidity, marked abdominal distention, marked abdominal tenderness, and rebound abdominal tenderness. If the diagnosis is not clear after the initial evaluation, repeated physical examination by the same physician often is useful. Selected imaging studies also might be helpful. Surgical consultation is necessary if a surgical cause is suspected or the cause is not obvious after a thorough evaluation.
Abdominal pain is a common problem in children. Although most children with acute abdominal pain have self-limited conditions, the pain may herald a surgical or medical emergency. The most difficult challenge is making a timely diagnosis so that treatment can be initiated and morbidity prevented. This article provides a comprehensive clinical guideline for the evaluation of the child with acute abdominal pain.
Pathophysiology
Clinically, abdominal pain falls into three categories: visceral (splanchnic) pain, parietal (somatic) pain, and referred pain.
Visceral pain occurs when noxious stimuli affect a viscus, such as the stomach or intestines. Tension, stretching, and ischemia stimulate visceral pain fibers. Tissue congestion and inflammation tend to sensitize nerve endings and lower the threshold for stimuli. Because visceral pain fibers are bilateral and unmyelinated and enter the spinal cord at multiple levels, visceral pain usually is dull, poorly localized, and felt in the midline. Pain from foregut structures (e.g., lower esophagus, stomach) generally is felt in the epigastrium. Midgut structures (e.g., small intestine) cause periumbilical pain, and hindgut structures (e.g., large intestine) cause lower abdominal pain.
Parietal pain arises from noxious stimulation of the parietal peritoneum. Pain resulting from ischemia, inflammation, or stretching of the parietal peritoneum is transmitted through myelinated afferent fibers to specific dorsal root ganglia on the same side and at the same dermatomal level as the origin of the pain. Parietal pain usually is sharp, intense, discrete, and localized, and coughing or movement can aggravate it.
Referred pain has many of the characteristics of parietal pain but is felt in remote areas supplied by the same dermatome as the diseased organ. It results from shared central pathways for afferent neurons from different sites. A classic example is a patient with pneumonia who presents with abdominal pain because the T9 dermatome distribution is shared by the lung and the abdomen.1
TABLE 1 Causes of Acute Abdominal Pain in Children
| Gastrointestinal | Genitourinary causes | Drugs and toxins |
| causes | Urinary tract infection | Erythromycin |
| Gastroenteritis | Urinary calculi | Salicylates |
| Appendicitis | Dysmenorrhea | Lead poisoning |
| Mesenteric lymphadenitis | Mittelschmerz | Venoms |
| Constipation | Pelvic inflammatory disease | Pulmonary causes |
| Abdominal trauma | Threatened abortion | Pneumonia |
| Intestinal obstruction | Ectopic pregnancy | Diaphragmatic |
| Peritonitis | Ovarian/testicular torsion | Pleurisy |
| Food poisoning | Endometriosis | Miscellaneous |
| Peptic ulcer | Hematocolpos | Infantile colic |
| Meckel’s diverticulum | Metabolic disorders | Functional pain |
| Inflammatory bowel disease | Diabetic ketoacidosis | Pharyngitis |
| Lactose intolerance | Hypoglycemia | Angioneurotic edema |
| Liver, spleen, and biliary tract disorders | Porphyria | Familial |
| Hepatitis | Acute adrenal insufficiency | Mediterranean fever |
| Cholecystitis | Hematologic disorders | |
| Cholelithiasis | Sickle cell anemia | |
| Splenic infarction | Henoch-Schönlein purpura | |
| Rupture of the spleen | Hemolytic uremic syndrome | |
| Pancreatitis |
Etiology
Table 1 lists many causes of acute abdominal pain in children. Information on rare entities can be found in a standard pediatric surgery textbook.2
INFANTILE COLIC
Infantile colic affects 10 to 20 percent of infants during the first three to four weeks of life. Typically, infants with colic scream, draw their knees up against their abdomen, and appear to be in severe pain.3
GASTROENTERITIS
Gastroenteritis is the most common cause of abdominal pain in children.4 Viruses such as rotavirus, Norwalk virus, adenovirus, and enterovirus are the most frequent causes.4,5 The most common bacterial agents include Escherichia coli, Yersinia, Campylobacter, Salmonella, and Shigella.
APPENDICITIS
Appendicitis is the most common surgical condition in children who present with abdominal pain.2,6 Approximately one in 15 persons develop appendicitis.7 Lymphoid tissue or a fecalith obstructs the appendiceal lumen, the appendix becomes distended, and ischemia and necrosis may develop. Patients with appendicitis classically present with visceral, vague, poorly localized, periumbilical pain. Within six to 48 hours, the pain becomes parietal as the overlying peritoneum becomes inflamed; the pain then becomes well localized and constant in the right iliac fossa.
MESENTERIC LYMPHADENITIS
Mesenteric lymphadenitis often is associated with adenoviral infection. The condition mimics appendicitis, except the pain is more diffuse, signs of peritonitis often are absent, and generalized lymphadenopathy may be present.
CONSTIPATION
Acute constipation usually has an organic cause (e.g., gastroenteritis, appendicitis), while chronic constipation usually has a functional cause (e.g., low-residue diet). Abdominal pain resulting from constipation is most often left-sided or suprapubic.
ABDOMINAL TRAUMA
Abdominal trauma can be accidental or intentional. Blunt abdominal trauma is more common than penetrating injury. Abdominal trauma may cause musculocutaneous injury, bowel perforation, intramural hematoma, laceration or hematoma of the liver or spleen, and avulsion of intra-abdominal organs or vascular pedicles.
INTESTINAL OBSTRUCTION
Intestinal obstruction produces a characteristic cramping. Causes of intestinal obstruction include volvulus, intussusception, incarcerated hernia, and postoperative adhesions.
PELVIC INFLAMMATORY DISEASE
Pelvic inflammatory disease (PID) usually is caused by Chlamydia trachomatis or Neisseria gonorrhoeae.7 Risk factors include multiple sexual partners, use of an intrauterine device (IUD), and a history of PID.
Clinical Evaluation
In evaluating children with abdominal pain, a thorough history is required to identify the most likely cause. An initial evaluation of the history is followed by a physical examination and a reassessment of certain points of the history. An algorithm is presented in Figure 1.8
HISTORY
Age of Onset
Pain History
Children who do not verbalize typically present with late symptoms of disease. Children up to the teenage years have a poor sense of onset or location of pain. The classic sequence of shifting pain usually occurs with appendicitis. In children who cannot verbalize, the initial 24-hour history of vague nausea or periumbilical pain may be unreported or go unnoticed, so these children more often present at the second stage of more visceral pain. However, any child with pain that localizes to the right lower quadrant should be suspected of having appendicitis. Thus, inquiry into the location, timing of onset, character, severity, duration, and radiation of pain are all important points but must be viewed in the context of the child's age.
Recent Trauma
A history of recent trauma may indicate the cause of pain.
Precipitating or Relieving Factors
Parietal pain is aggravated by movement. Relief of pain after a bowel movement suggests a colonic source, and relief after vomiting suggests a source in the more proximal bowel.
FIGURE 1. Evaluation of Acute Abdominal Pain in Children
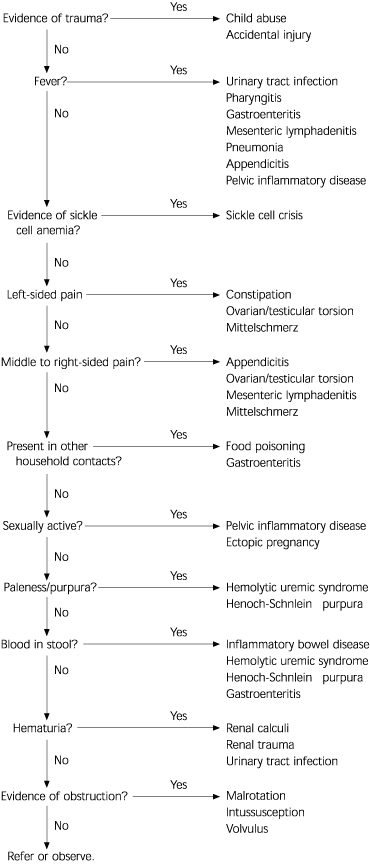
Algorithm for evaluating acute abdominal pain in children.
Adapted with permission from King BR. Acute abdominal pain. In: Hoekelman RA. Primary pediatric care. 3d ed. St. Louis: Mosby, 1997:188.
Associated Symptoms
In the acute surgical abdomen, pain generally precedes vomiting, and the reverse is true in medical conditions. Any child presenting with bilious vomiting should be presumed to have a bowel obstruction. Diarrhea often is associated with gastroenteritis or food poisoning, but it also can occur with other conditions. Bloody diarrhea is much more suggestive of inflammatory bowel disease or infectious enterocolitis. The classic “currant-jelly stool” often is seen in patients with intussusception. Failure to pass flatus or feces suggests intestinal obstruction.
TABLE 2 Differential Diagnosis of Acute Abdominal Pain by Predominant Age
| Birth to one year | Two to five years | Six to 11 years | 12 to 18 years |
| Infantile colic Gastroenteritis Constipation Urinary tract infection Intussusception Volvulus Incarcerated hernia Hirschsprung's disease | Gastroenteritis Appendicitis Constipation Urinary tract infection Intussusception Volvulus Trauma Pharyngitis Sickle cell crisis Henoch-Schönlein purpura Mesenteric lymphadenitis | Gastroenteritis Appendicitis Constipation Functional pain Urinary tract infection Trauma Pharyngitis Pneumonia Sickle cell crisis Henoch-Schönlein purpura Mesenteric lymphadenitis | Appendicitis Gastroenteritis Constipation Dysmenorrhea Mittelschmerz Pelvic inflammatory disease Threatened abortion Ectopic pregnancy Ovarian/testicular torsion |
Urinary frequency, dysuria, urgency, and malodorous urine suggest a urinary tract infection.12 Purulent vaginal discharge suggests salpingitis. Cough, shortness of breath, and chest pain point to a thoracic source. Polyuria and polydipsia suggest diabetes mellitus. Joint pain, rash, and smoke-colored urine suggest Henoch-Schönlein purpura.13
Gynecologic History
In girls, a thorough gynecologic history, including a menstrual history and a history of sexual activity and contraception, is essential. Amenorrhea may indicate pregnancy. A history of multiple sexual partners and the use of an IUD suggest PID. Use of an IUD and a history of PID or tubal ligation increase the risk of ectopic pregnancy. Sudden onset of midcycle pain of short duration suggests mittelschmerz.
Past Health
All previous hospitalizations or significant illnesses such as sickle cell anemia and porphyria should be noted. A history of surgery not only can eliminate certain diagnoses but also can increase the risk of others, such as intestinal obstruction from adhesions. A history of similar pain may suggest a recurrent problem.
Drug Use
A detailed drug history is important, because certain drugs (Table 1) may cause abdominal pain.
Family History
A family history of sickle cell anemia or cystic fibrosis may indicate the diagnosis. The patient's ethnic background is important because sickle cell anemia is most common in blacks of African origin.
PHYSICAL EXAMINATION
General Appearance
In general, children with visceral pain tend to writhe during waves of peristalsis, while children with peritonitis remain quite still and resist movement. The hydration status of the child should be assessed.
Vital Signs
Fever indicates an underlying infection or inflammation. High fever with chills is typical of pyelonephritis and pneumonia.12 Tachycardia and hypotension suggest hypovolemia. If a postmenarcheal girl is in shock, ectopic pregnancy should be suspected. Hypertension may be associated with Henoch-Schönlein purpura or hemolytic uremic syndrome.13,14 Kussmaul's respiration indicates diabetic ketoacidosis.
Abdominal Examination
The breathing pattern should be observed, and the patient should be asked to distend the abdomen and then flatten it. After the child is asked to indicate, with one finger, the area of maximal tenderness, the abdomen should be gently palpated, moving toward (but not palpating) that area. The physician should examine for Rovsing's sign (when pressure on the left lower quadrant distends the column of colonic gas, causing pain in the right lower quadrant at the site of appendiceal inflammation), then gently assess muscle rigidity. Gentle percussion best elicits rebound tenderness. Deeper palpation is necessary to discover masses and organomegaly.
Rectal and Pelvic Examination
These examinations should be used when significant information is sought or expected.2,10,15 A rectal examination may provide useful information about tenderness, sphincter tone, and presence of masses, stool, and melena. In boys, examination of the external genitalia may reveal penile and scrotal abnormalities. In girls, it may reveal vaginal discharge, vaginal atresia, or imperforate hymen. A bimanual pelvic examination may provide useful information about uterine or adnexal masses or tenderness. Purulent cervical discharge, cervical motion tenderness, and adnexal mass are signs of PID.
Associated Signs
Jaundice suggests hemolysis or liver disease. Pallor and jaundice point to sickle cell crisis. A positive iliopsoas test (passive extension of the right hip and flexion of the right thigh against resistance) or obturator test (rotation of the right flexed hip) suggests an inflamed retrocecal appendix, a ruptured appendix, or an iliopsoas abscess. A positive Murphy's sign (interruption of deep inspiration by pain when the physician's fingers are pressed beneath the right costal margin) suggests acute cholecystitis. Cullen's sign (bluish umbilicus) and Grey Turner's sign (discoloration in the flank) are unusual signs of internal hemorrhage. Purpura and arthritis suggest Henoch-Schönlein purpura.13
Investigations
Laboratory studies should be tailored to the patient's symptoms and clinical findings. Initial laboratory studies may include a complete blood cell count and urinalysis. A low hemoglobin level suggests blood loss or underlying hematologic abnormalities, such as sickle cell disease. However, a normal hemoglobin level does not exclude an acute massive hemorrhage for which the body has not yet compensated. Leukocytosis, especially in the presence of a shift to the left and toxic granulations in the peripheral smear, indicates an infection. Urinalysis can help identify urinary tract pathology, such as infection or stones. A pregnancy test should be considered in post-menarcheal girls.16
Plain-film abdominal radiographs are most useful when intestinal obstruction or perforation of a viscus in the abdomen is a concern. Chest radiographs may help rule out pneumonia. The most contentious issue in emergency medicine may be the usefulness of ultrasonography and computed tomography (CT) in patients with abdominal pain.17–20 CT likely is more accurate than ultrasonography.18 However, the experience of the operator and interpreter significantly affect the accuracy of both modes.19 In the emergency department, ultra-sonography probably is most useful in diagnosing gynecologic pathology such as ovarian cysts, ovarian torsion, or advanced periappendiceal inflammation.17,20 CT involves radiation exposure and may require the use of contrast agents. CT may be necessary if excessive bowel gas precludes ultrasonographic examination.
TABLE 3 Indications for Surgical Consultations in Children with Acute Abdominal Pain
| Severe or increasing abdominal pain with progressive signs of deterioration |
| Bile-stained or feculent vomitus |
| Involuntary abdominal guarding/rigidity |
| Rebound abdominal tenderness |
| Marked abdominal distension with diffuse tympany |
| Signs of acute fluid or blood loss into the abdomen |
| Significant abdominal trauma |
| Suspected surgical cause for the pain |
| Abdominal pain without an obvious etiology |
Management
Treatment should be directed at the underlying cause. In many patients, the key to diagnosis is repeated physical examination by the same physician over an extended time.21 Indications for surgical consultations are listed in Table 3. Traditionally, the use of analgesics is discouraged in patients with abdominal pain for fear of interfering with accurate evaluation and diagnosis. However, several prospective, randomized studies have shown that judicious use of analgesics actually may enhance diagnostic accuracy by permitting detailed examination of a more cooperative patient.22–24 [References 22 and 23—Evidence level A, randomized controlled trials]

